In recent years an association has been reported between number of prior episodes and response to cognitive therapy in depressed patients. Several subgroup analyses, based on stratified Reference Teasdale, Segal, Williams, Ridgeway, Soulsby and Lau1,Reference Ma and Teasdale2 and non-stratified Reference Bockting, Schene, Spinhoven, Koeter, Wouters, Huyser and Kamphuis3 subsamples, pointed out that preventive cognitive therapy is more effective than usual care in patients with three to five, or more, prior episodes, but not in patients who had experienced fewer previous episodes. Since depression is a major mental health problem and treatment capacity is limited, optimising treatment allocation could help to decrease the problem of unmet need for treatment. 4 The finding of differential treatment response depending on number of prior episodes may therefore be of importance.
Unfortunately, several issues remain unresolved. First, the studies mentioned concern preventive cognitive therapy, whereas cognitive therapy in daily practice consists almost exclusively of acute-phase treatment. Second, these studies used mixed samples of patients recruited from community healthcare facilities and by media announcements, whereas the vast majority of depressed patients are treated in primary care. Third, it is unclear through which particular depressive symptom(s) cognitive therapy exerts its effect in patients with multiple previous episodes.
Therefore, this study examines whether this differential treatment response can be replicated in depressed primary care patients, treated by acute-phase cognitive–behavioural therapy (CBT) v. usual care. In addition, we set out to examine whether the difference CBT may make is predominantly due to its impact on cognitive symptoms of depression. This may be expected, since rumination is seen as a source of recurrence, and treatment of dysfunctional thinking is central to CBT. Reference Teasdale, Scott, Moore, Hayhurst, Pope and Paykel5 Thus, we anticipate that in patients with multiple previous episodes, the effect of CBT will be particularly noticeable at the cognitive-symptoms level of depression.
Method
Patients participated in a randomised clinical trial in primary care evaluating the effects of experimental depression treatments. Reference Conradi, De Jonge, Kluiter, Smit, Van der Meer, Jenner, Van Os, Emmelkamp and Ormel6 We included patients, referred by general practitioners (GPs), who: had a diagnosis of depression; were 18–70 years old; had no life-threatening medical condition, psychotic disorder, bipolar disorder, dementia or primary alcohol or drug dependency; and were not already receiving psychotherapy. For the current analyses we selected patients who received usual care from their GP and, since CBT was followed by psychoeducation in the trial, patients who were randomised to psychoeducation alone or CBT plus psychoeducation. Analyses of the latter two groups enable us to disentangle effects of both treatment components.
Usual care, according to clinical guidelines, consists of brief supportive counselling, possible antidepressant prescription and/or referral.
The psychoeducational prevention programme is a protocolised low-intensity programme consisting of three face-to-face sessions and short 3-monthly telephone contacts thereafter. Psychoeducation alone had no effect on long-term outcomes of depression. Reference Conradi, De Jonge, Kluiter, Smit, Van der Meer, Jenner, Van Os, Emmelkamp and Ormel6
Cognitive–behavioural therapy plus psychoeducation consists of 10–12 protocolised CBT sessions with a psychotherapist and aims at promoting (social) reactivation and restructuring of dysfunctional cognitions. Subsequently patients followed the psychoeducational programme.
Two instruments were used to assess the course of depression. First, to determine severity of depression, the Beck Depression Inventory (BDI) was administered every 3 months during a 2-year follow-up. Second, an adapted version of the Composite International Diagnostic Interview (CIDI), a structured psychiatric interview which has shown good reliability and validity, was administered every 3 months: face-to-face at baseline and by telephone thereafter. With this we measured the presence of the individual DSM–IV 7 symptoms of depression per week over the previous 3 months. Thus, we could establish the percentage of time during the 2-year follow-up that patients had: depressed mood and/or diminished interest, eating problems, sleeping problems, psychomotor problems, fatigue, worthlessness or guilt, cognitive problems and death ideations. The number of previous depressive episodes was established with the baseline lifetime CIDI.
Linear mixed-model analysis was used to evaluate differential change over time in the eight repeated BDI measurements for usual care v. psychoeducation and usual care v. CBT plus psychoeducation. Baseline BDI score and timing of assessment were incorporated as covariates. This analysis was carried out for all patients and two subgroups, namely patients who had experienced three or fewer, or four or more depressive episodes before baseline. To evaluate the appropriateness of conducting subgroup analyses, we added an interaction term to the model, representing the interaction effect of CBT v. usual care×prior episodes. Alpha was set at 50.10.
Mann–Whitney non-parametric tests were used to examine per subgroup whether treatments differed regarding the percentage of time the discrete DSM–IV depressive symptom clusters, as measured by the CIDI, were present during follow-up. We set α<0.05.
Results
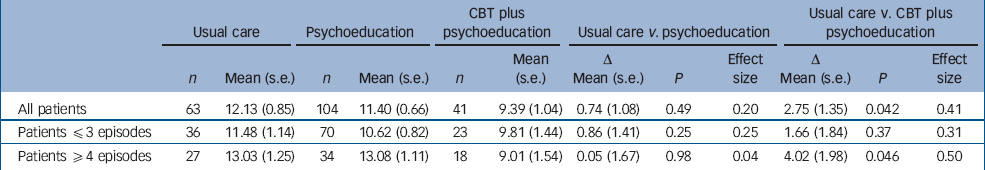
Overall, psychoeducation patients did not, but CBT plus psychoeducation patients did, report a significantly lower mean than usual care patients on the BDI from 3 to 24 months (Table 1). As the interaction term of CBT v. usual care×prior episodes approached significance (P<0.09), further subgroup analyses were considered to be justified. In the group of patients with three or fewer prior episodes we found no significant differences on the BDI during follow-up between treatment groups. However, in the group with four or more episodes, psychoeducation patients did not differ from usual care patients, whereas the mean BDI score of CBT plus psychoeducation patients was 4 points lower than that of usual care patients (effect size ≃0.5).
Table 1 Analyses of the eight repeated BDI measurements conducted during the 2-year follow-up, adjusted for baseline BDI
| Usual care | Psychoeducation | CBT plus psychoeducation | Usual care v. psychoeducation | Usual care v. CBT plus psychoeducation | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | Mean (s.e.) | n | Mean (s.e.) | n | Mean (s.e.) | Δ Mean (s.e.) | P | Effect size | Δ Mean (s.e.) | P | Effect size | |
| All patients | 63 | 12.13 (0.85) | 104 | 11.40 (0.66) | 41 | 9.39 (1.04) | 0.74 (1.08) | 0.49 | 0.20 | 2.75 (1.35) | 0.042 | 0.41 |
| Patients ≤3 episodes | 36 | 11.48 (1.14) | 70 | 10.62 (0.82) | 23 | 9.81 (1.44) | 0.86 (1.41) | 0.25 | 0.25 | 1.66 (1.84) | 0.37 | 0.31 |
| Patients ≥4 episodes | 27 | 13.03 (1.25) | 34 | 13.08 (1.11) | 18 | 9.01 (1.54) | 0.05 (1.67) | 0.98 | 0.04 | 4.02 (1.98) | 0.046 | 0.50 |
Finally, we compared per subgroup whether the treatments differed on each of the DSM–IV depressive symptom clusters (CIDI) during the 2-year follow-up. Only one significant difference emerged. In the group with four or more previous episodes, the median percentage of follow-up time during which usual care patients reported having cognitive problems was 47% (interquartile range 25–88; representing 11.3 months) compared with 15% for CBT plus psychoeducation patients (interquartile range 8–64; representing 3.6 months), which was significantly better (Z=–2.328, P=0.020).
Discussion
A limitation of this study is that it involves an analysis of non-stratified subgroups of a randomised controlled trial, and although the marginally significant interaction corresponds with a clinically relevant differential treatment response to CBT compared with usual care (i.e. 4.02 v. 1.66 relative decrease on the BDI), results still need to be confirmed in future research. Strengths of the study are the detailed and reliable prospective assessment of depression course by questionnaire (BDI) and interview (CIDI), and the fact that it involves primary care patients.
This study makes three clinically valuable contributions to earlier findings of a differential treatment response depending on number of prior depressive episodes. First, we observed a comparable differential treatment response in the primary care setting, in which the vast majority of depressed patients are treated, instead of mixed samples of patients.
Second, we found this differential treatment response not to be restricted to preventive cognitive therapy: it can also be observed with the far more common acute-phase CBT. We found that in patients with three or fewer prior episodes the three treatments perform equally well, whereas in patients with four or more episodes, CBT plus psychoeducation performs clinically better than usual care. This effect is assumed to be attributable to the CBT component of CBT plus psychoeducation, since psychoeducation did not differ from usual care (although a favourable interaction between psychoeducation and CBT cannot be ruled out completely). Therefore, GPs may consider the number of previous depressive episodes, which is a strong predictor of an unfavourable course of depression, Reference Conradi, De Jonge and Ormel8 as a treatment indicator in order to optimise allocation of scarce treatment capacity. Patients with few prior episodes show no additional benefit with CBT, whereas for patients with multiple prior episodes, GPs may advise CBT in addition to usual care.
Third, we found that in the group with multiple prior episodes, treatments differed significantly only on cognitive symptoms (indecisiveness, unclear and slow thinking, and concentration problems). This may suggest that CBT is able to manage ruminative styles of thinking, which are seen as a risk factor for recurrence. Dissolving dysfunctional thinking is central to CBT.






eLetters
No eLetters have been published for this article.