Attention-deficit hyperactivity disorder (ADHD) is strongly associated with conduct disorder Reference Thapar, van den Bree, Fowler, Langley and Whittinger1,Reference Mannuzza, Klein, Abikoff and Moulton2 and thought also to increase risk for the development of juvenile psychopathy. Reference Lynam3 Psychopathy traits in adolescence are important. Reference Pardini and Loeber4 They are linked to greater frequency of violent and non-violent acts of delinquency, severity of criminal acts Reference Forth, Kosson and Hare5 and may index meaningful heterogeneity of conduct disorder. Reference Rutter6 The origins of psychopathy are thought to lie in childhood Reference Rutter6,Reference Blair, Peschardt, Budhani, Mitchell and Pine7 but relatively little is known about specific risk factors and the relationship with ADHD. We investigate psychopathy traits in a longitudinal study of children with ADHD and examine the relationship with early adversity.
Methods
Participants
Participants for this study were selected from a sample of 375 children with ADHD who had participated in a research study 5 years earlier. Reference Holmes, Payton, Barrett, Harrington, McGuffin and Owen8 The sample had been recruited from district child and adolescent psychiatry and paediatric clinics in North England, South West England and South Wales (UK). In the UK, the diagnosis of ADHD is given by specialist (secondary care) services. Families of consecutive referrals with a suspected diagnosis of ADHD were asked by the local clinician whether they would consider participating in the study and over 95% agreed. All the children had met diagnostic criteria for DSM–III–R 9 or DSM–IV 10 ADHD after a detailed research assessment, had IQ test scores of above 70 and did not have pervasive developmental disorder, Tourette syndrome or any neurological conditions.
To be eligible, participants were required to be 12 years of age or older. The eligible sample consisted of 197 adolescents (180 boys, 17 girls) aged 12–19 years (mean=14.5 years, s.d.=1.7). Through the UK National Health Service system, 95% of this sample was successfully traced and 79% (n=156) participated in the current study.
Ethical approval for the study was obtained from the NorthWest England Multi-Centre Research Ethics Committee, UK, and written informed consent and assent was obtained from parents and children/adolescents for the original study 5 years previously and for the current follow-up study.
Measures
The interview and questionnaire assessments used in this phase of the study were the same as those used in the original study 5 years earlier with the exception that for this study adolescent as well as parent reports of psychopathology were available and psychopathy traits were assessed.
Interviews
Parent and adolescent interviews were conducted by trained, supervised psychology graduates and a post-doctoral researcher. The parent version of the Child and Adolescent Psychiatric Assessment (CAPA), Reference Angold, Prendergast, Cox, Harrington, Simonoff and Rutter11 a semi-structured research diagnostic interview, was used to assess clinical symptoms of DSM–IV ADHD, oppositional defiant disorder and conduct disorder. The Child Attention-Deficit Hyperactivity Disorder Teacher Telephone Interview (CHATTI) Reference Holmes, Lawson, Langley, Fitzpatrick, Trumper and Pay12 was completed to check whether there was impairment in more than one setting (i.e. school). The adolescent was interviewed using the child version of the CAPA that includes the same questions on antisocial behaviour, anxiety and depression but not ADHD. Reference Angold and Costello13 Conduct disorder and oppositional defiant disorder symptoms were considered present if reported by either parent or child. DSM–III–R/DSM–IV diagnoses were generated using information from the CAPA and the CHATTI. All interviews were audiotaped, interviewers were supervised weekly by an experienced clinician (A.T.) (for all families) and 20 audiotapes were randomly selected for re-rating and to check interrater reliability. Interrater reliability was high, κ=1.00 for DSM–IV ADHD and κ=1.00 for ICD–10 14 hyperkinetic disorder.
Psychopathy traits were assessed using the Hare Psychopathy Checklist–Youth Version Reference Forth, Kosson and Hare5 (PCL–YV), a 20-item semi-structured interview designed and validated in a variety of settings to assess psychopathy in 12–18 year olds (each item is rated on a 3-point scale). It is recommended that a multisource, multi-informant approach is taken in the assessment of PCL–YV items. Reference Forth, Kosson and Hare5 Psychopathy scores were generated using the method advised by its authors, focusing on the adolescent interview information but including a review of file information collected during the original study and the current follow-up study.
A total psychopathy score was calculated by summing all the PCL–YV items. Factor analysis of adolescent measures of psychopathy suggests that the ‘emotional-dysfunction’ Reference Cleckley15 component, which includes features such as callousness and a lack of remorse and affect, represents an important and distinctive factor. Reference Forth, Kosson and Hare5 It is thought that the emotional-dysfunction component of psychopathy may have distinct biological origins as well as having a distinctive clinical presentation. Reference Pardini and Loeber4,Reference Blair, Peschardt, Budhani, Mitchell and Pine7 Thus, emotional-dysfunction scores were additionally calculated. Reference Forth, Kosson and Hare5,Reference Hare16
Questionnaires
Questionnaires were completed by mothers of participants. Information from a validated measure of pregnancy and birth complications Reference Lewis and Murray17 and maternal cigarette, alcohol and illicit substance use during pregnancy was collected. Reference Rice, Lewis, Harold, van den Bree, Boivin and Hay18 Items on this measure show very good to excellent agreement with antenatal records. Reference Rice, Lewis, Harold, van den Bree, Boivin and Hay18 The exceptions are length of labour and alcohol use in pregnancy, the latter item having been found to be poorly recorded in medical records. Reference Rice, Lewis, Harold, van den Bree, Boivin and Hay18 Family measures included family conflict and cohesion, Reference Moos and Moos19 the number of children in the household, social class and whether the biological parents of the child were currently separated or had ever been separated. Reference Holmes, Payton, Barrett, Hever, Fitzpatrick and Trumper20,Reference Langley, Marshall, van den Bree, Thomas, Owen and O'Donovan21 Questionnaire information was also obtained from mothers on their current and childhood ADHD symptoms (<18 years of age) Reference Barkley22 and from a checklist of childhood DSM–IV conduct disorder symptoms, which was summed to give a maternal childhood antisocial score.
Data analysis
Total and emotional-dysfunction psychopathy scores from the PCL–YV were transformed using natural log because of their positive skew.
Regression analysis was used to test for associations between early adversity factors and (a) total psychopathy scores and (b) emotional-dysfunction scores. We controlled for current age, use of stimulant medication at follow-up, socio-economic status and adolescent gender (where appropriate). After all analyses had been completed, multiple regression analyses were rerun using the raw outcome data (no differences were found).
The following pre- and perinatal events were examined: maternal smoking, alcohol and drug use during pregnancy, premature birth (before 37 weeks), birth weight and a composite measure of birth complications. Information on the following birth complications was available: forceps delivery, ventouse delivery, breech birth and emergency Caesarean section. Time spent in a special care baby unit or incubator was also taken as indication of birth/neonatal complications. For the purpose of analysis, individuals were divided into those who had and had not experienced birth complications, adopting the approach described by Raine et al. Reference Raine, Brennan and Mednick23 Social class was determined from the occupation of the main earner in the household (reported by parents) according to the UK Standard Occupational Classification. 24 The sample was then separated into high, medium or low social class. High social class consisted of professional and managerial families (n=41, 26%), medium social class was made up of families with skilled occupations and partially skilled workers (n=50, 32%), and low social class consisted of families where the main breadwinners were in unskilled jobs or were unemployed (n=58, 37%) (7 families had missing data). Family factors including family conflict and cohesion scores currently and in childhood (assessed 5 years earlier), family size, relationship of biological parents (i.e. separated ever, currently separated) and social class were also examined individually and simultaneously in a forced entry multiple regression.
Results
Descriptive statistics
Overall, 156 families took part (79%). Of these families, 9 adolescents did not wish to be interviewed. Therefore psychopathy scores were available for 147 individuals. There were no significant differences at baseline in the total number of ADHD symptoms (t=–0.66, d.f.=194, P=0.51), conduct disorder symptoms (t=0.50, d.f.=195, P=0.61) and socio-economic status (χ2=3.42, d.f.=2, P=0.198) between individuals with available psychopathy scores and those without (i.e. eligible families that did not wish to take part in the follow-up as well as families where the adolescent did not wish to be interviewed). There were also no baseline clinical and socio-economic differences between families who participated and did not participate in the follow-up. Reference Whittinger, Langley, Fowler, Thomas and Thapar25 The full clinical description of the sample (at baseline and follow-up) has been previously published. Reference Holmes, Payton, Barrett, Harrington, McGuffin and Owen8,Reference Whittinger, Langley, Fowler, Thomas and Thapar25
The original inclusion criterion for the sample was that individuals should meet either DSM–IV (82%, n=128) or DSM–III–R (remaining 18%, n=28) diagnostic criteria for ADHD. In this study, 5 years later, 81% (122/151) continued to meet full DSM–IV (54% (82/151)) or DSM–III–R (26% (40/151)) diagnostic criteria for ADHD and 31% met DSM–IV diagnostic criteria for conduct disorder. Reference Whittinger, Langley, Fowler, Thomas and Thapar25 The mean ADHD score was 14.7 at the original assessment (s.d.=2.5, range 7–18) and 12.2 at the follow-up assessment (s.d.=4.8, range 0–18). The mean conduct disorder symptom score was 0.9 at the original assessment (s.d.=1.4, range 0–8) and 2.0 at the follow-up assessment (s.d.=2, range 0–8).
Psychopathy scores
The mean total psychopathy score was 5.91 (s.d.=4.21, range 0–19), significantly higher (t=6.87, P<0.0001) than published mean scores (mean=2.85, s.d.=2.58) reported in a UK community sample of 110 slightly older high school males aged 15–18 years. Reference Forth, Kosson and Hare5 Asubstantial number (38%) scored higher than 1 standard deviation above the mean score of the UK community high school sample. This was despite the fact that over half of the adolescents were younger than 15 years, the lowest age of the high school comparison sample. Although there is no cut-point for adolescent psychopathy, Reference Forth, Kosson and Hare5 it should be noted that none of the sample scored above cut-points previously used to categorically define psychopathy in adults. Reference Angold and Costello13 The mean emotional-dysfunction score was 1.00 (s.d.=1.29, range 0–6), higher than the mean score of 0.19 (s.d.=0.58) found in a community sample Reference Forth, Kosson and Hare5 of adolescent males (A. Forth, personal communication, 2008).
Total psychopathy scores and emotional-dysfunction psychopathy scores were found to be significantly associated with conduct disorder symptoms (r=0.66, P<0.01 and r=0.50, P<0.01 respectively). Adolescents with ‘high’ total and emotional-dysfunction psychopathy scores (>1 s.d. above the mean; n=26 and n=22 respectively) were found to show higher conduct disorder symptom scores than the remainder of the sample (t=–8.13, P<0.0001 and t=–6.38, P<0.0001 respectively). Total psychopathy scores were associated with concurrent ADHD symptom severity (β=0.26, t=3.16, P=0.002), but the association disappeared when concurrent conduct disorder was used as a covariate. No significant associations were found between concurrent ADHD and emotional-dysfunction scores (β=0.11, t=1.35, P=0.18).
Association of psychopathy scores with pre- and perinatal factors
The results for pre- and perinatal factors are summarised in Table 1. Both unadjusted coefficients for each factor and adjusted coefficients (controlling for all other pre- and perinatal factors examined) are reported.
Table 1 Associations of pre- and perinatal factors with total psychopathy scores and emotional-dysfunction scoresa

| Total psychopathy scores | Emotional-dysfunction psychopathy scores | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Unadjusted | Adjustedb | Unadjusted | Adjustedb | |||||||||
| Variable: pre- and perinatal factors | β | t | P | β | t | P | β | t | P | β | t | P |
| Maternal smoking during pregnancy | 0.27 | 3.06 | 0.003** | 0.33 | 3.28 | 0.001** | 0.22 | 2.45 | 0.02* | 0.27 | 2.67 | 0.009** |
| Maternal drug use during pregnancy | -0.04 | -0.45 | 0.64 | -0.11 | -1.05 | 0.30 | -0.06 | -0.68 | 0.50 | 0.09 | 0.98 | 0.33 |
| Maternal alcohol use during pregnancy | -0.02 | -0.27 | 0.79 | -0.05 | -0.53 | 0.60 | 0.07 | 0.73 | 0.47 | -0.11 | -1.09 | 0.28 |
| Birth weight of child, g | -0.04 | -0.48 | 0.64 | 0.06 | 0.52 | 0.61 | 0.006 | 0.07 | 0.95 | 0.07 | 0.69 | 0.50 |
| Born preterm (<37 weeks) | 0.09 | 1.02 | 0.31 | 0.06 | 0.59 | 0.56 | 0.05 | 0.53 | 0.60 | 0.01 | 0.12 | 0.91 |
| Birth complications | 0.21 | 2.17 | 0.03* | 0.20 | 1.95 | 0.052 | 0.26 | 2.83 | 0.006** | 0.28 | 2.81 | 0.006** |
Maternal smoking (n=60, 43%) but not alcohol (n=49, 35%) or illicit drug use (n=4, 3%) during pregnancy was significantly associated with both total psychopathy scores and emotional-dysfunction scores. This association could be an artefact due to the mother's own ADHD and/or antisocial behaviour, which would increase the likelihood of their smoking during pregnancy and influence their child's behaviours. Reference Maughan, Taylor, Caspi and Moffitt26,Reference Silberg, Parr, Neale, Rutter, Angold and Eaves27 The analysis was repeated controlling for maternal conduct disorder and ADHD symptoms during childhood and maternal adult ADHD symptoms. The association of maternal smoking in pregnancy with total psychopathy scores remained significant (β=0.18, t=2.12, P=0.04), but was no longer significant for the emotional-dysfunction scores (β=0.15, t=1.52, P=0.13). Similarly when controlling for adolescent conduct disorder symptoms, the association with total psychopathy scores remained significant (β=0.18, t=2.41, P=0.02) but the association with emotional-dysfunction scores did not (β=0.16, t=1.78, P=0.08).
Birth complications were associated with emotional-dysfunction scores but the association did not achieve conventional levels of significance (P<0.05) for total psychopathy scores. The association with emotional-dysfunction scores remained after controlling for conduct disorder symptoms (β=0.18, t=2.66, P=0.009).
Association between psychopathy scores and family adversity
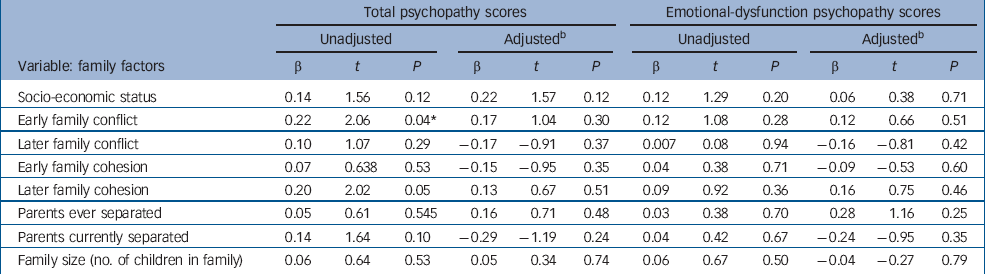
The results for family factors are summarised in Table 2. Both unadjusted coefficients for each factor and adjusted coefficients (while controlling for all other family factors) are reported. Socio-economic status, marital status of the parents and family structure were not associated with total psychopathy scores. Early family conflict (assessed 5 years earlier) but not concurrent family conflict was associated with total psychopathy scores. The association between early family conflict and total psychopathy scores dropped from significance when current ADHD severity and conduct disorder symptoms were controlled for (β=0.06, t=0.77, P=0.44). Earlier conflict also did not remain associated with psychopathy when all family factors were considered together (although this is likely to be an overly stringent test of association). Overall, the results suggest that the association seen between early family conflict and total psychopathy scores appears to be due to the relationship between psychopathy and conduct disorder symptoms. None of the family factors was associated with emotional-dysfunction scores.
Table 2 Associations of family factors with total psychopathy scores and emotional-dysfunction psychopathy scores
| Total psychopathy scores | Emotional-dysfunction psychopathy scores | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Unadjusted | Adjustedb | Unadjusted | Adjustedb | |||||||||
| Variable: family factors | β | t | P | β | t | P | β | t | P | β | t | P |
| Socio-economic status | 0.14 | 1.56 | 0.12 | 0.22 | 1.57 | 0.12 | 0.12 | 1.29 | 0.20 | 0.06 | 0.38 | 0.71 |
| Early family conflict | 0.22 | 2.06 | 0.04* | 0.17 | 1.04 | 0.30 | 0.12 | 1.08 | 0.28 | 0.12 | 0.66 | 0.51 |
| Later family conflict | 0.10 | 1.07 | 0.29 | -0.17 | -0.91 | 0.37 | 0.007 | 0.08 | 0.94 | -0.16 | -0.81 | 0.42 |
| Early family cohesion | 0.07 | 0.638 | 0.53 | -0.15 | -0.95 | 0.35 | 0.04 | 0.38 | 0.71 | -0.09 | -0.53 | 0.60 |
| Later family cohesion | 0.20 | 2.02 | 0.05 | 0.13 | 0.67 | 0.51 | 0.09 | 0.92 | 0.36 | 0.16 | 0.75 | 0.46 |
| Parents ever separated | 0.05 | 0.61 | 0.545 | 0.16 | 0.71 | 0.48 | 0.03 | 0.38 | 0.70 | 0.28 | 1.16 | 0.25 |
| Parents currently separated | 0.14 | 1.64 | 0.10 | -0.29 | -1.19 | 0.24 | 0.04 | 0.42 | 0.67 | -0.24 | -0.95 | 0.35 |
| Family size (no. of children in family) | 0.06 | 0.64 | 0.53 | 0.05 | 0.34 | 0.74 | 0.06 | 0.67 | 0.50 | -0.04 | -0.27 | 0.79 |
Discussion
The present study is to our knowledge the first to examine juvenile psychopathy traits in a UK sample of adolescents who had had childhood ADHD.
Psychopathy traits in ADHD
Our sample showed elevated total psychopathy and emotional-dysfunction trait scores than a UK adolescent school sample, Reference Forth, Kosson and Hare5 in keeping with the proposition that children with ADHD are a risk group for showing psychopathy traits. There is also some evidence from neuropsychological studies Reference Lynam28 and a retrospective study of adult prison inmates and adults with psychopathic traits that children with ADHD Reference Maughan, Taylor, Caspi and Moffitt26 may be ‘fledgling psychopaths’. However, in our sample, the range of scores did not extend into the region in which scorers, in adulthood, are traditionally classed as ‘psychopaths’.
An important consideration is that there is no established cut-off point for defining psychopathy in adolescents for the PCL–YV. Reference Forth, Kosson and Hare5 Current adult cut-off points for psychopathy are unlikely to be appropriate for children and it is also possible that important differences in expected scores between younger and older adolescents exist. There is also evidence that total psychopathy scores vary in different countries. Compared with North American samples, there is a cultural bias towards lower scores in the UK. Reference Cooke, Michie, Hart and Clark30 Given our findings, coupled with the uncertainty about a meaningful cut-off point for psychopathy, we suggest that it is not safe to conclude that children with ADHD grow up to be ‘psychopaths’. However, children with ADHD do appear to be a group with elevated levels of total psychopathy and emotional-dysfunction traits. Rather, our findings concur with those of Piatigorsky & Hinshaw, Reference Piatigorsky and Hinshaw31 who found higher scores of psychopathy traits in a US sample of children with ADHD (aged 6–12 years) than in controls. Recent work also suggests that adolescent psychopathy is best viewed in terms of dimensional scores rather than as a category. Reference Murrie, Marcus, Douglas, Lee, Salekin and Vincent32 Our findings also suggest that the relationship between total psychopathy scores and ADHD occurs not because of the risk effects of ADHD severity, at least within a clinical sample, but rather because of the strong links between psychopathy traits and conduct disorder symptoms.
Association with early adversity
Early biological and social adversity have been considered likely to play an important role in juvenile psychopathy Reference Viding33,Reference Lykken34 but as yet there is little empirical evidence available. In the initial analyses, we found that maternal smoking during pregnancy was associated with both total psychopathy scores and the emotional-dysfunction dimension of psychopathy. There is evidence that the association of exposure to prenatal smoking with conduct disorder and antisocial behaviour may be explained by maternal characteristics, in particular maternal antisocial behaviour. Reference Maughan, Taylor, Caspi and Moffitt26,Reference Silberg, Parr, Neale, Rutter, Angold and Eaves27 In our sample the association of maternal smoking in pregnancy with total psychopathy scores was, however, not accounted for by measures of maternal antisocial and ADHD behaviours or by adolescent ADHD severity and conduct disorder symptoms. In contrast, the relationship with emotional-dysfunction psychopathy scores became non-significant when these factors were controlled for.
There is also evidence of association between maternal smoking in pregnancy and ADHD, with a pooled analysis showing a significant association with a reported odds ratio of 2.39 (95% CI 1.61–3.52, P<0.001). Reference Langley, Rice, van den Bree and Thapar35 Animal studies suggest plausible mechanisms for the association Reference Ernst, Moolchan and Robinson36 but causality has yet to be established and the association may mainly index genetic liability. To our knowledge, there has been no previous study examining the relationship between maternal smoking in pregnancy and psychopathy traits. It is possible that previous findings of association (even if genetically mediated) between maternal smoking in pregnancy and ADHD, adult criminality and antisocial behaviour Reference Langley, Rice, van den Bree and Thapar35,Reference Brennan, Grekin and Mednick37 are in part driven by the relationship with psychopathy traits. This needs further investigation.
Obstetric complications have also previously been suggested as a possible contributor to developmental disturbance that, in turn, may predispose to psychopathy traits. Reference Lykken34 Others have suggested that these may be risk factors for violent antisocial behaviour, rather than likely to be linked with the instrumental (i.e. proactive and planned) aggression characteristic of psychopathy. Reference Blair, Peschardt, Budhani, Mitchell and Pine7 One of the few studies to examine birth complications and psychopathy found a higher incidence of obstetric complications in violent adult offenders compared with non-offender controls but not more so in those classed as psychopathic than in those classed as non-psychopathic. Reference Lalumiere, Harris and Rice38 However, emotional-dysfunction scores were not specifically examined. In our study, we found an association between birth complications and emotional-dysfunction psychopathy scores, with birth complications accounting for 7% of the variance. This finding may be important, given that there has been much interest and speculation about the role of early brain damage, especially affecting prefrontal cortical and amygdala functioning, in the aetiology of psychopathy, Reference Viding, Williamson and Hariri39,Reference Blair40 particularly as the lack of emotional reactivity characterised by high emotional-dysfunction psychopathy scores has been posited as the mechanism through which psychopathy may lead to elevated antisocial behaviour. Reference Blair, Peschardt, Budhani, Mitchell and Pine7 However, there will be other pathways, including genetic liability, that can lead to altered brain function.
Finally, we found no clear evidence that psychopathy traits in ADHD are associated with family adversity. This contrasts with findings for conduct disorder, where family and social factors are established and are important correlates. Indeed in our sample, higher conduct disorder scores were associated with family adversity, specifically lower socio-economic status and higher levels of family conflict (results available from corresponding author). Moreover, there is evidence to suggest that some of these factors, notably parenting Reference Patterson, DeGarmo and Knutson41 and poverty, Reference Costello, Compton, Keeler and Angold42 play a causal role in childhood disruptive behaviours. The one possible exception in our sample was the observed association between family conflict in childhood (reported by mothers 5 years earlier) and total psychopathy scores (reported by adolescents). It is interesting and important that the association is found across raters and across time. However, the association appeared to be explained by associated conduct disorder symptoms.
The role of family adversity in the development of psychopathy has been uncertain. Some view the origins of psychopathy as being primarily innate, with evidence of family environment and parenting Reference Viding33,Reference Devita, Forth and Hare43,Reference Wooton, Frick, Shelton and Silverthorn44 not being linked to antisocial behaviour in those with psychopathy or psychopathy traits. Other researchers have considered that exposure to early family adversity and disruption is likely to be important. Reference Farrington45 Our findings suggest that it is conduct disorder symptoms rather than psychopathy traits in ADHD that are more closely associated with family adversity.
Distinction of emotional-dysfunction scores
Emotional dysfunction seen in adult, adolescent and child psychopathy has been posited to represent a distinct component of psychopathy and the mechanism through which psychopathy may lead to elevated antisocial behaviour. Reference Forth, Kosson and Hare5 In children, the concept of ‘callous-unemotional traits’ has been developed to describe what is thought to be the key feature of childhood psychopathy. Reference Frick, O'Brien, Wootton and McBurnett46 These traits bear many similarities to the emotional-dysfunction component of adult psychopathy although the concordance is not perfect. Reference Lee, Vincent, Hart and Corrado47,Reference Murrie and Cornell48 Given the potential importance of the emotional-dysfunction aspect of psychopathy as a mechanism through which psychopathy traits may develop, a key question is whether pre- and perinatal factors and family correlates for emotional-dysfunction psychopathy scores are the same as those for total psychopathy scores. The results from this study suggest that the pattern of correlates is similar but not identical for total and emotional-dysfunction psychopathy scores. Adjusting for associated conduct disorder symptoms, maternal smoking during pregnancy was associated with total psychopathy scores but not emotional-dysfunction scores. Birth complications were associated with emotional-dysfunction scores. These results would partially support the distinction of emotional dysfunction in terms of its link with early adversity in the form of birth complications. This increased rate of reported birth complications may of course simply index an underlying pre-existing biological and genetic vulnerability rather than represent a causal risk factor. Indeed, the evidence is that perinatal complications index underlying genetic liability for other neurodevelopmental disorders such as autism. Reference Bolton, Murphy, Macdonald, Whitlock, Pickles and Rutter49
Limitations
This study has several limitations which should be considered. First, the elevated psychopathy scores were not so high as to be within the range of what might be classed as ‘psychopathy’. Thus, the correlates of individuals with higher psychopathy scores may differ. Although higher psychopathy scores were found than in a published sample of high school males, they were not matched geographically, by age, gender or social class. However, this was the only published community-based normative information available and the older age range of the high school sample (15–18 years) makes it likely that, if anything, we have underestimated differences. Second, our findings relate to psychopathy traits in those with ADHD, and may not apply to psychopathy traits in a general or forensic population. Third, our sample size may have been insufficient to detect some small effects and given the number of potential predictive factors included in statistical tests the possibility of type 1 and type 2 errors should also be considered. The limited variation in the emotional-dysfunction scores may also have influenced results. Similarly, as we are examining a clinical sample, the restricted range in ADHD scores may attenuate the relationship with predictive factors. Fourth, it is not possible to draw conclusions as to whether the associated early factors are causal or merely indicate risk of psychopathy. Finally, despite the high rate of follow-up (79%), differences between participants and non-participants at follow-up cannot be completely discounted, although we found no clinical and demographic differences.
Conclusions
Children with ADHD show higher than expected levels of total psychopathy traits but do not score above previously used clinical cut-points for psychopathy, and there is no association with severity of ADHD. This suggests that for community clinics, children with ADHD do not grow up to be ‘psychopaths’. Pre- and perinatal adversity appear to be associated with total psychopathy trait scores and emotional-dysfunction scores. Family adversity seems to be linked with conduct disorder rather than psychopathy traits in ADHD.







eLetters
No eLetters have been published for this article.