Prevention of suicide is a priority for health services. 1 Historically, older age has been shown to be a risk factor for suicide. Reference Conwell, Duberstein, Cox, Hermann, Forbes and Caine2,3 Over the past 15 years, suicide rates have fallen in some high-income countries, particularly in older age groups. 4,Reference Koponen, Viilo, Hakko, Timonen, Meyer-Rochow, Sarkioja and Rasanen5 However, the world population is aging and the study of suicide in older age remains important. Previous research suggests that suicide in older people is associated with depression, comorbid physical illnesses and substance misuse. Reference Conwell, Duberstein, Cox, Hermann, Forbes and Caine2,Reference Koponen, Viilo, Hakko, Timonen, Meyer-Rochow, Sarkioja and Rasanen5,Reference Waern6
Dementia is one of the major healthcare problems in later life, affecting 24 million people worldwide. Reference Ferri, Prince, Brayne, Brodaty, Fratiglioni and Ganguli7 Although high rates of psychiatric symptoms during the course of illness have been reported, Reference Aalten, De Vught, Jaspers, Jolles and Verhey8 the risk of suicide in people with dementia is generally considered low. Reference Lim, Rubin, Coats and Morris9,Reference Conwell, Duberstein and Caine10 Empirical data on suicide in dementia are scarce and primarily based on case reports (e.g. Rhode et al Reference Rhode, Peskind and Raskind11 ). In a recent summary of those case reports, it has been suggested that early stage of dementia, male gender, high educational level, professional occupation, retention of insight, depressive features post-dating the onset of dementia, suicidal ideation and access to firearms might be risk factors for completed suicide in dementia. Reference Lim, Rubin, Coats and Morris9 Furthermore, some studies have reported significantly more Alzheimer's pathology in the brains of older suicide victims compared with age- and gender-matched controls who died naturally, Reference Rubio, Vestner, Stewart, Forbes, Conwell and Cox12 although findings have not been consistent. Reference Peisah, Snowdon, Gorrie, Kril and Rodriguez13
The National Confidential Inquiry into Suicide and Homicide by People with Mental Illness collects data on all those who die by suicide within 12 months of last contact with mental health services of the National Health Service (NHS) in the UK. Reference Appleby, Shaw, Sherrat, Amos, Robinson and McDonnell14 It currently holds data on 11 512 people aged 10 years and above who died by suicide in the period April 1996 to December 2004 and offers a unique opportunity to examine suicide in dementia in more detail. Our objectives were to describe the behavioural, clinical and care characteristics of patients with dementia who died by suicide, and to compare them with age- and gender-matched controls who died by suicide and who did not have clinical diagnosis of dementia.
Methods
The study was carried out as part of the National Confidential Inquiry into Suicide and Homicide by People with Mental Illness (the Inquiry), Reference Appleby, Shaw, Sherrat, Amos, Robinson and McDonnell14 a complete national clinical sample of all people that had been in contact with mental health services in the 12 months prior to their death by suicide. The Inquiry has research ethics approval (South Manchester Research Ethics Committee ERP/96/2771) and approval under Section 60 of the Health and Social Care Act to process patient-identifiable data without consent. The data collection on suicides involved three stages: (a) collection of a comprehensive national sample, irrespective of mental health history; (b) identification of people in the sample who had been in contact with mental health services in the 12 months before death; and (c) collection of clinical data about these individuals. Data collection has been described in detail elsewhere, Reference Hunt, Kapur, Robinson, Shaw, Flynn, Bailey, Meehan, Bickley, Burns, Appleby and Parsons15 and is summarised below.
Comprehensive national sample
Information on all deaths in England and Wales receiving a suicide or an open verdict at coroner's inquest was obtained from the Office for National Statistics. The cases presented here consist of suicides registered by the Office for National Statistics from 1 April 1996 until 31 December 2004. In the first 3 years of the study, this information was cross-checked against equivalent data from health authorities in England and Wales; inconsistencies were rare. Open verdicts, recorded as deaths from undetermined external cause, are often reached in cases of suicide in the UK. Open verdicts are conventionally included in research on suicide and in official suicide statistics. Reference O'Donnell and Farmer16–Reference Linsley, Schapira and Kelly18 In this study, we adopted this convention and included open (ICD–10 codes Y10–Y34, excluding Y33.9 (verdict pending) and Y87.2 (sequelae of events of undetermined intent)) as well as suicide (ICD–10 Codes X60–X84 and Y87.0) verdicts. 19
Identification of mental health service contact and collection of clinical data
Identifying details on each individual who had died by suicide were submitted to the main hospital and community NHS trusts who provided mental health services to people living in the deceased's district of residence. When NHS records showed that contact had occurred in the 12 months before the suicide, the person became an ‘Inquiry case’. For each Inquiry case, the consultant psychiatrist was sent a questionnaire and asked to complete it based on their knowledge of the patient, psychiatry case notes, and in discussion with other members of the mental health team. The questionnaire consisted of sections covering social/demographic characteristics, clinical history, details of suicide, aspects of care, details of final contact with mental health services and clinicians' views on suicide prevention. Clinicians were asked for an ICD–10 primary diagnosis and also any ICD–10 secondary diagnoses. 19 The social and clinical items reflected many of the most frequently reported risk factors for suicide. The majority of items were factual but some (for example, adherence to treatment) were based on the judgements of clinicians.
Identification of patients with dementia and selection of controls
Based on the information provided by the responsible consultant psychiatrist, we identified all patients with an ICD–10 diagnosis of dementia. 19 A total of 118 patients with dementia were identified. For each individual with dementia, we extracted four gender-matched suicide cases of patients without a diagnosis of dementia (controls) nearest in age to the dementia patients (n=472). This selection was masked, i.e. we were unaware of the behavioural, clinical and care characteristics of these controls. All controls were individually matched for gender and 462/472 (98%) for age within 2 years of the index case (3-year difference for seven cases, 5-year difference for two cases and 6-year difference for one case).
Statistical analysis
All data are presented as absolute numbers and percentages within groups. If an item of information was not known for a case, the case was removed from the analysis of that item; the denominator in all estimates is therefore the number of valid cases for the item. Differences between cases and controls were tested by univariate conditional logistic regression analyses, using Intercooled Stata 9.0 for Windows. As the study was mainly exploratory, main findings are presented as odds ratios (OR) including 95% confidence intervals (CI). Acknowledging heterogeneity in the cases of dementia, we also performed subgroup analyses. The following subgroups were defined: (a) patients with dementia aged 65 years and over; and (b) all dementia cases excluding those in which the individual had a comorbid diagnosis of alcohol dependence and/or schizophrenia and other delusional disorders. Dementia associated with alcohol dependence or schizophrenia and related disorders is thought to be qualitatively different from dementia in older people caused by neurodegenerative and/or cerebrovascular processes (e.g. Alzheimer's disease, vascular dementia and dementia with Lewy bodies). Reference Olde Rikkert, van der Flier, de Leeuw, Verbeek, Jansen, Verhey and Scheltens20 Patients with dementia under the age of 65 years were not selected for subgroup analyses as we anticipated small numbers.
Results
Over the 9-year study period, the Inquiry received notifications of 45 012 deaths by suicide, including 30 794 (68%) cases in which the coroner's verdict was suicide and 14 218 (32%) open verdicts or deaths from undetermined cause. Of these, 11 733 (26.1%) were confirmed to have been in contact with mental health services in the year prior to death. Completed questionnaires were received for 11 512 cases, a response rate of 98.1%. In 11 141 cases (97.9% of the 11 375 cases that included data on primary diagnosis), a psychiatric diagnosis was recorded. In 118 (1.1%) of these cases, the individuals had received a clinical diagnosis of dementia from their psychiatrist and 72 (61%) had received an open verdict. As expected this was a higher proportion of open verdicts than in the control sample (n=131, 28%).
Behavioural, clinical and care characteristics of the dementia group
The 118 patients who had died by suicide and had a clinical diagnosis of dementia had a median age of 75 years (range 32–95) and 63 (53%) were male. The sample was predominantly White, including only 5 (4%) individuals from an ethnic minority group. Furthermore, 36 (32%) individuals were married and 58 (49%) lived alone at the time of suicide.
Online Table DS1 describes behavioural, clinical and care characteristics of the dementia group as a whole, and by predefined subgroups. For 91 (80%) of the group, the last contact with services was routine or non-urgent, and for 57 (50%) it occurred in patients' homes. A care-coordinator was allocated in 84 (81%) cases and 47 (40%) individuals were on an enhanced care programme approach (a form of enhanced aftercare indicative of clinical complexity and involvement of at least two members of a multidisciplinary team with different professional backgrounds, usually a community psychiatry nurse and a psychiatrist). The time between last contact and the suicide was less than 1 week for 50 (44%) individuals, and less than 24 h for 18 (16%). A further 29 (25%) individuals had their last contact between 1 and 4 weeks before suicide, 13 (11%) between 5 and 13 weeks, and 23 (20%) more than 3 months before. Evidence of psychiatric symptoms at the last contact was noted for 41 (35%) individuals, most often depressive illness (n=18, 16%), hopelessness (n=10, 9%) and delusions or hallucinations (n=8, 7%). In four patients (4%) suicidal ideation was recorded at the last contact. A deterioration in physical health was noted for 27 (24%) patients.
A total of 26 individuals who had died by suicide and had a diagnosis of dementia were aged below 65 years, and half of this younger subgroup (n=13, 50%) had a history of alcohol and/or drug misuse, including 6 (23%) with a diagnosis of alcohol dependence. As shown in online Table DS1, this subgroup had more involved psychiatric histories and received more intense psychiatric care.
Method of suicide
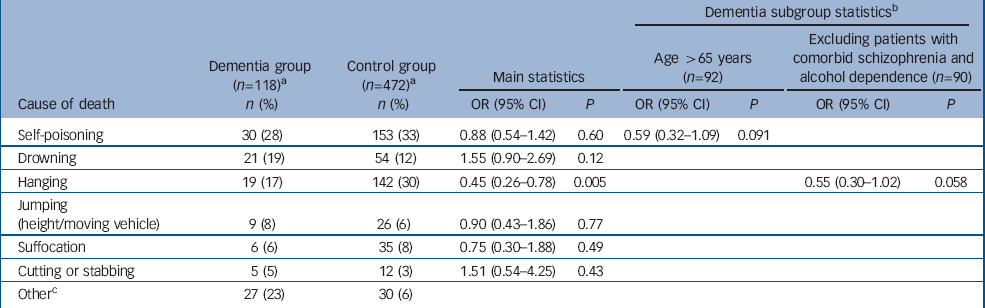
Similar to the control group, self-poisoning was the most common method of suicide in the dementia group, accounting for almost a third of deaths (Table 1). The substance used was highly variable, most often being analgesics (n=12: paracetamol, n=4; codeine-containing preparations and other opiate analgesics, n=4; other analgesics, n=4), psychotropic drugs (n=4, all different classes), or other poisons such as weed killer (n=4). All other substances were used only once. After self-poisoning, drowning (19%) and hanging (17%) were the second and third most common methods of suicide among patients in the dementia group. The main analysis showed that hanging was used significantly less often by those in the dementia group compared with controls. Three suicides in the dementia group were part of a suicide pact.
Table 1 Method of suicide in patients with dementia compared with controls
| Dementia subgroup statistics b | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Dementia group (n=118) a n (%) | Control group (n=472) a n (%) | Main statistics | Age >65 years (n=92) | Excluding patients with comorbid schizophrenia and alcohol dependence (n=90) | |||||||
| Cause of death | OR (95% CI) | P | OR (95% CI) | P | OR (95% CI) | P | |||||
| Self-poisoning | 30 (28) | 153 (33) | 0.88 (0.54–1.42) | 0.60 | 0.59 (0.32–1.09) | 0.091 | |||||
| Drowning | 21 (19) | 54 (12) | 1.55 (0.90–2.69) | 0.12 | |||||||
| Hanging | 19 (17) | 142 (30) | 0.45 (0.26–0.78) | 0.005 | 0.55 (0.30–1.02) | 0.058 | |||||
| Jumping (height/moving vehicle) | 9 (8) | 26 (6) | 0.90 (0.43–1.86) | 0.77 | |||||||
| Suffocation | 6 (6) | 35 (8) | 0.75 (0.30–1.88) | 0.49 | |||||||
| Cutting or stabbing | 5 (5) | 12 (3) | 1.51 (0.54–4.25) | 0.43 | |||||||
| Other c | 27 (23) | 30 (6) | |||||||||
a. The denominator in all estimates is the number of valid cases for each item
b. To improve readability, only OR (95% CI) reported with a P < 0.10
c. To prevent the possibility of individuals being identified, all methods used by fewer than three patients in the dementia group are not described (examples include the use of firearms, burning, electrocution, etc.)
Comparison with the non-dementia group
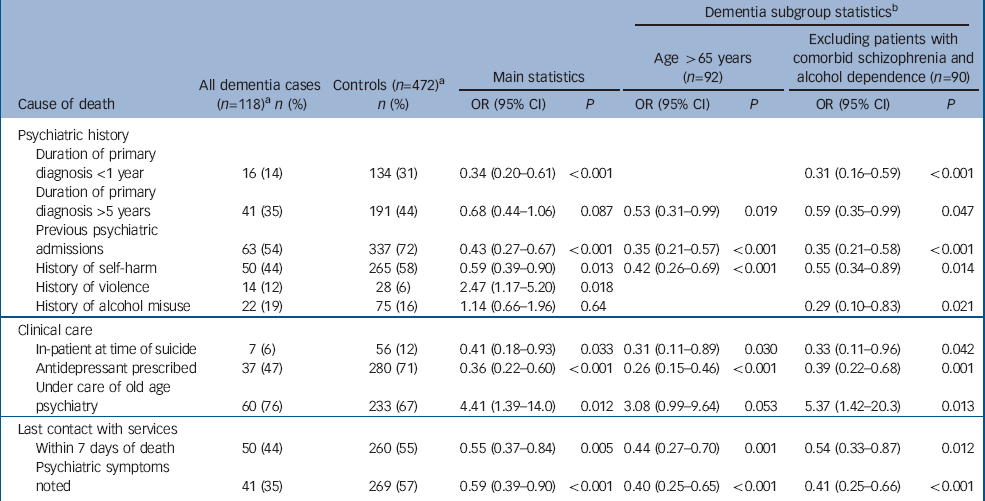
Patients with dementia who died by suicide were compared with their matched controls on all variables presented in online Table DS1. All demographic characteristics were similar for those in the dementia group and their age- and gender-matched controls (P>0.43). In Table 2, behavioural, clinical and care variables that were significantly different in patients with dementia and their controls are presented. With respect to psychiatric history, patients with dementia less often died by suicide within 1 year of diagnosis, were less often prescribed antidepressants, and were less likely to have a history of self-harm. Although the main analysis suggests that patients with dementia were more likely to have a history of violence (12% v. 6%, P=0.018), the difference was quite small and was not replicated in the two subgroup analyses (Table 2). In line with these findings, patients with dementia had fewer psychiatric admissions and were also less likely to die by suicide while psychiatric in-patients. Significantly fewer psychiatric symptoms were reported during the last contact with a mental health service professional in patients with dementia compared with their matched controls, of which emotional problems (31% v. 16%, P=0.002) and depressive symptoms (40% v. 16%, P<0.001) reached statistical significance. Life events within 3 months prior to suicide were evaluated systematically in 14 different categories (e.g. interpersonal problems with significant others, financial problems, victim of violence). The frequency of all different life events was similar in patients with dementia and controls, including ‘own physical health problems’ which was the most often reported life event in both groups (15% v. 17%, P=0.82).
Table 2 Behavioural, clinical and characteristics of patients with dementia that differed significantly from their controls at time of suicide
| Dementia subgroup statistics b | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| All dementia cases (n=118) a n (%) | Controls (n=472) a n (%) | Main statistics | Age >65 years (n=92) | Excluding patients with comorbid schizophrenia and alcohol dependence (n=90) | |||||||
| Cause of death | OR (95% CI) | P | OR (95% CI) | P | OR (95% CI) | P | |||||
| Psychiatric history | |||||||||||
| Duration of primary diagnosis <1 year | 16 (14) | 134 (31) | 0.34 (0.20–0.61) | <0.001 | 0.31 (0.16–0.59) | <0.001 | |||||
| Duration of primary diagnosis >5 years | 41 (35) | 191 (44) | 0.68 (0.44–1.06) | 0.087 | 0.53 (0.31–0.99) | 0.019 | 0.59 (0.35–0.99) | 0.047 | |||
| Previous psychiatric admissions | 63 (54) | 337 (72) | 0.43 (0.27–0.67) | <0.001 | 0.35 (0.21–0.57) | <0.001 | 0.35 (0.21–0.58) | <0.001 | |||
| History of self-harm | 50 (44) | 265 (58) | 0.59 (0.39–0.90) | 0.013 | 0.42 (0.26–0.69) | <0.001 | 0.55 (0.34–0.89) | 0.014 | |||
| History of violence | 14 (12) | 28 (6) | 2.47 (1.17–5.20) | 0.018 | |||||||
| History of alcohol misuse | 22 (19) | 75 (16) | 1.14 (0.66–1.96) | 0.64 | 0.29 (0.10–0.83) | 0.021 | |||||
| Clinical care | |||||||||||
| In-patient at time of suicide | 7 (6) | 56 (12) | 0.41 (0.18–0.93) | 0.033 | 0.31 (0.11–0.89) | 0.030 | 0.33 (0.11–0.96) | 0.042 | |||
| Antidepressant prescribed | 37 (47) | 280 (71) | 0.36 (0.22–0.60) | <0.001 | 0.26 (0.15–0.46) | <0.001 | 0.39 (0.22–0.68) | 0.001 | |||
| Under care of old age psychiatry | 60 (76) | 233 (67) | 4.41 (1.39–14.0) | 0.012 | 3.08 (0.99–9.64) | 0.053 | 5.37 (1.42–20.3) | 0.013 | |||
| Last contact with services | |||||||||||
| Within 7 days of death | 50 (44) | 260 (55) | 0.55 (0.37–0.84) | 0.005 | 0.44 (0.27–0.70) | 0.001 | 0.54 (0.33–0.87) | 0.012 | |||
| Psychiatric symptoms noted | 41 (35) | 269 (57) | 0.59 (0.39–0.90) | <0.001 | 0.40 (0.25–0.65) | <0.001 | 0.41 (0.25–0.66) | <0.001 | |||
a. The denominator in all estimates is the number of valid cases for each item
b. To improve readability, only OR (95% CI) reported with a P < 0.10
Discussion
This paper describes a complete national sample of people with dementia who died by suicide while in the care, or having recently been in the care, of mental health services in England and Wales, a geographical area including over 55 million citizens. These cases comprise only 1% (equivalent to 13.5 deaths per year) of the full 9-year sample of people who died by suicide within 12 months of contact with mental health services. This number may be considered to be low given that about 550 000 people in England and Wales are suffering from dementia; 21 however, we only included individuals who had been seen by specialist mental health services in the 12 months before death. Over a fifth of suicide cases in the dementia group were aged below 65 years, an age group in which the prevalence of dementia is rare (<0.5%) compared with people aged over 65 years (in whom the prevalence increases sharply from 1.5% in those aged 65–70 years to 24.8% in those aged over 85 years). Reference Ferri, Prince, Brayne, Brodaty, Fratiglioni and Ganguli7 This finding indicates a high proportional risk of suicide in younger patients with dementia compared with older patients with dementia, although this might also suggest that younger patients with dementia are more likely to be in contact with specialist services than their older counterparts. Detailed inspection of this younger age group showed high levels of psychiatric comorbidity and long-standing psychiatric problems.
The methods of suicide used by patients with dementia were comparable to those used by controls. Moreover, we did not find differences with respect to the classic risk factors for suicide in later life, such as physical illness and life events. Reference Conwell, Duberstein and Caine10 Suicide in dementia, however, was characterised by fewer behavioural and clinical indicators of suicide risk compared with controls in our study, as well as when compared with previous studies on older suicide victims in general. Reference Heisel22 The individuals with dementia who died by suicide were significantly less likely to have a history of self-harm or a history of psychiatric admissions. At the last contact prior to suicide, psychiatric symptoms were less likely to be noted in the dementia group than in the control group. It may be that in people with dementia, the cognitions or concerns about the progression of dementia are more important determinants of suicide. Alternatively, psychiatric symptoms, especially depressive symptoms, may be underrecognised in patients with dementia or wrongly attributed to being core symptoms of dementia because of overlap between depression and dementia. Reference Purandare, Burns, Craig, Faragher and Scott23 This latter explanation is especially relevant as depressive illness is the most important risk factor for suicide in older adults, with a population attributable risk of up to 74%. Reference Beautrais24 In addition, depressive illness may negatively mediate the effect of physical illness. Reference Lim, Rubin, Coats and Morris9
Interestingly, the time since diagnosis in the dementia group was more often between 1 and 5 years compared with patients who had other psychiatric diagnoses, which is in line with results of a retrospective study of suicide in dementia cases admitted to a psychiatric hospital. Reference Barak and Aizenberg25 This time period corresponds to the first two-thirds of the disease process, with a median survival time of 10.5 years from onset and 5.7 years from diagnosis, Reference Waring, Doody, Pavlik, Massman and Chan26 which significantly decreases with advancing age. Reference Xie, Brayne and Matthews27 The predominance of suicide in the first half of the dementia process might be explained by significantly less interference of cognitive deficits with the planning and executing of the suicide act at this stage. Reference Rubin, Veiel, Kinscherf, Morris and Storandt28,Reference Ready, Ott, Grace and Cahn-Weiner29 Moreover, depressive symptoms, which may have been underestimated in our sample, predominate the initial stage of the dementia process, whereas the latter stages are more dominated by apathy. Reference Ready, Ott, Grace and Cahn-Weiner29,Reference Migliorelli, Teson, Sabe, Petracchi, Leiguarda and Starkstein30 Importantly, our data show a very low prevalence of suicide in the first 12 months after dementia has been diagnosed. This finding may indicate that disclosure of diagnosis, although it might evoke suicidal thoughts, is not a risk factor as sometimes suggested. Reference Turnbull, Wolf and Holroyd31 Our results are most consistent with the view that the risk for suicide is highest at the stage of the disease process where patients experience increasing difficulties in daily living activities due to their dementia, but still have a preservation of insight into ongoing and impending cognitive deterioration. Reference Vogel, Stokholm, Gade, Andersen, Hejl and Waldemar32 This point of view contrasts with suicides in other psychiatric disorders in which lack of insight is generally a risk factor for suicide. Reference Hunt, Kapur, Robinson, Shaw, Flynn, Bailey, Meehan, Bickley, Burns, Appleby and Parsons15
Study limitations
Although the large size of the database used in this study and high absolute number of dementia suicide cases enhances its inferential value, the findings of this study need to be interpreted in the context of certain methodological issues. First, this study is a survey of the clinical circumstances preceding suicide, and we are unable to make causal inferences. A control group of patients with dementia who had not died by suicide would have been relevant for identification of suicide risk factors specific for dementia. Controls were mental health patients who died by suicide with a diagnosis other than dementia. Therefore, the differences we observed could simply be due to differences between diagnostic groups (rather than differences in suicide risk). As depression (and rarely other psychiatric illnesses) may precede dementia, it is possible that some of the controls may in fact have undiagnosed early dementia. Reference Ownby, Crocco, Acevedo, John and Loewenstein33 This raises the possibility that that observed differences between dementia suicides and the control group of non-dementia suicides may be underestimated. Known risk factors for suicide in later life (i.e. male gender and older age, could not be examined because of matched analyses). Reference Conwell, Duberstein and Caine10,Reference O'Connell, Chin, Cunningham and Lawlor34 Second, the generalisability of our findings is limited to patients with dementia in contact with mental health services, most likely patients with dementia with significant behavioural and psychological symptoms. Therefore, suicides in patients with ‘uncomplicated’ dementia or those who are not receiving treatments to enhance cognition may be under-represented in this sample. Such a bias towards patients with dementia with behavioral difficulties or psychiatric comorbidity make the findings in relation to less symptomatology and comorbidity more remarkable. Moreover, this may also explain the low number of ethnic minorities, as elderly suicide victims from ethnic minorities are less likely to be in contact with psychiatric services. Reference Salib and Green35 Third, the clinicians who provided the information by filling out the study questionnaires were not masked to patient outcome and this may have affected their response to certain questions, for example, the preventability of suicide in their patient. However, this will not affect the comparison between cases and controls, and the accuracy of the Inquiry questionnaire has been shown to be good. Reference Appleby, Shaw, Sherrat, Amos, Robinson and McDonnell14
We used the wider definition of suicide that included both suicide and deaths of undetermined intent. This is the standard definition that is used in official statistics and previous research. Excluding open verdicts may underestimate the number of actual suicide deaths by 50%. Reference Linsley, Schapira and Kelly18 However, the number of open verdicts was much higher in the dementia group than the control group in this study – why might this be? A study of all suicide and open verdicts over a 10-year period in one coroner's court found that the factors which most reliably distinguished suicide from open verdicts included method of death (hanging and death from car exhaust poisoning more common; drowning and falling from a height less common) and presence of a suicide note. A small study of deaths in individuals aged 65 years found that evidence of suicidal intent, psychiatric history and method of death distinguished suicide and open verdicts. Reference Salib36 In our study, the cases with dementia included a lower proportion of hanging deaths and a higher proportion of drowning deaths than controls. Those with dementia were less likely to have a significant psychiatric history. Individuals with dementia who died by suicide were also presumably less likely than those with other diagnosis who died by suicide to indicate suicidal intent or to write a suicide note, although we did not investigate these factors directly.
Clinical implications
The antecedents and clinical characteristics of patients with dementia who die by suicide differ from age- and gender-matched suicide victims with other psychiatric diagnoses. The low prevalence of suicide in dementia combined with fewer long-standing psychiatric problems, as well as fewer psychiatric symptoms just before death compared with controls, means that identifying people with dementia who are at risk of suicide remains a significant clinical challenge. Patients may be at particular risk 1–5 years after diagnosis; during this period, suicidal thoughts could be openly discussed with patients and their families. This may help improve underrecognition and undertreatment of psychiatric comorbidity such as depression.
Acknowledgements
R.C.O.V and N.K. had full access to all the data in the study and are responsible for the integrity of the data and the accuracy of the data analysis. The National Confidential Inquiry receives funding from the National Patient Safety Agency of the Department of Health in England and Wales, the Scottish Executive, and the Department of Health, Social Security and Public Services in Northern Ireland.







eLetters
No eLetters have been published for this article.