Studies of migration and depression tend to focus on migrants moving from developing and restructuring countries to industrialised ones and rarely consider links between migrants and their households of origin. Reference Swinnen and Selten1 However, internal migration within low- and middle-income countries, especially young adults moving from rural to urban areas, is a major feature of global population change. It tends to alleviate poverty, at least for most of those who migrate. Reference Skeldon2 Very little is known about the impact on older adults left behind in rural areas.
A commonly held view is that outmigration of young people has starkly negative consequences for ageing rural parents, with loneliness, isolation and even loss of basic instrumental and economic support. 3 A contrasting position is that non-migrant family members benefit through remittances Reference Cai4 and that families find adaptive ways to maintain contact. Reference Knodel and Saengtienchai5 If this is true, older people with some of their children migrated may be in a better position than those with all children migrated, having remittances but also local support.
The setting for the current study is Thailand, where traditionally children take responsibility for older parents and older parents continue to support children. With declining co-residence and increase in urbanisation of young adults, older people may be at risk of being left behind in rural Thailand if all their children migrate. Given that depression in older adults is associated with loss of close contacts Reference Djernes6 our hypothesis was that Thai parents aged 60 and over, living without at least one child in the district, would have more depression than those living with some or all children living in the district.
Method
Setting
We nested the study within the Kanchanaburi demographic surveillance system in western Thailand. 7 The demographic surveillance system began in 2000 and is an annual census of households in 100 sampling units comprising 87 villages and 13 urban census blocks. These were selected on ecological, socioeconomic and population criteria by stratified random sampling from the province population of 871 villages and 131 urban census blocks. The census includes a questionnaire for each household completed by the household head, for each individual household member aged 15 years or more and for each village completed by the village headmen, supplemented by a geographic information system.
Sampling
Historical data from 2004 showed which older adults in the surveillance system were living without at least one child in the same household. We did not know which of these had some or all of their children migrated outside the district, or which were childless. We therefore established a sampling frame that over-sampled older adults living without a child in the same household with the aim of capturing parents who had some or all children migrated beyond the district. We would then be able to use the whole sample we obtained to compare parents with all children migrated, parents with some children migrated and parents with no children migrated. There was a potential sample of 3916 households with at least one older adult aged 60 and above, of whom 2432 (62%) had at least one child of the older adult in the same household, and 1484 (38%) did not. For each sampling unit we used simple random sampling to select 60% of households where an older adult was living without at least one child and 30% of households where an older adult was living with at least one of their children, a total of 1593 households. We used random selection to select the participant in situations where there was more than one eligible parent living in a household. Data were collected from November 2006 to January 2007.
Definitions
We defined an outmigrant child as a child living outside the parent's district of residence Reference Knodel and Saengtienchai5 for a minimum of the past 3 months. We used minimum of 3 months to avoid temporary absences. A district is a well-recognised administrative boundary, with a radius of approximately 15 km in this province. Our a priori measure of exposure was having all children migrated outside the district. Given our conceptual model we compared this separately with having some children migrated or having no children migrated.
Recruitment
The interviewing team visited each sampling unit and made contact with the village headman or appropriate administrator prior to visiting each selected household. The populations were mostly already well acquainted with the demographic surveillance system. If the selected older adult and the household head gave consent, the interviewer first interviewed the household head with the household questionnaire and then the older adult with the individual questionnaire.
Inclusion criteria
Fluent Thai-speaking; aged 60 or over; parent of at least one living child (biological, adopted or step-child); living in a demographic surveillance system village since at least 2004.
Exclusion criteria
Change in living arrangement between 2004 and 2006 from living without a child to living with a child (or vice versa). We excluded these to minimise error in measuring duration of exposure and did not consider it would introduce bias as during piloting we found that fewer than 5% of older adults had changed this status between 2004 and 2006.
Exposure
The exposure of interest was location of children inside or outside the district. Early in the interview we established the location of all the participants' children (biological, adopted and step-children) by asking their names, where they lived and length of time living at that location. To assist precision we asked older adults if their child was in the household, the village (or for urban dwellers within average walking distance), the subdistrict/neighbourhood (‘tambon’), or the district (‘amphoe’), all of which are well-recognised. In Kanchanaburi province the average radius of a tambon is 6 km and of a district 15 km. We then stipulated which children we were referring to when we asked subsequently about support exchanges and remittances, cross-checking with the participant and/or another informant to ensure that we were rating contact with the correct child. For the few participants who performed poorly on cognitive tests or who gave vague or inconsistent answers, an informant gave this information.
Dependent variable
We measured depression using a Thai version of the EURO–D questionnaire. Reference Prince, Reischies, Beekman, Fuhrer, Jonker and Kivela8 The EURO–D is a 12-item screen for depression using items from standardised validated measures of depression that can be used by lay interviewers, including the Geriatric Mental State/AGECAT. Reference Copeland, Dewey and Griffiths-Jones9 It is strongly correlated with its parent diagnostic instruments and shows high criterion validity against DSM–IV 10 major depression. Reference Prince, Reischies, Beekman, Fuhrer, Jonker and Kivela8 In studies from low- and middle-income countries the EURO–D has a similar factor structure to that in high-income European countries. Reference Prince, Acosta, Chiu, Copeland, Dewey and Scazufca11 Thai mental health professionals, including two non-English speaking locally trained providers, considered that it covered symptoms recognised locally as common in psychological disorders in older adults. A team of bilingual mental health professionals, bilingual social scientists and English psychiatrists with relevant experience developed the first translation, paying particular attention to conceptual and semantic equivalence. We validated the Thai EURO–D in an out-patient setting against structured diagnostic interview by a Thai psychiatrist. The sample size was 150 and the number of people with gold-standard depression was 51. The area under the receiver operating characteristic (ROC) curve was 0.78 (95% CI 0.70–0.85), the kappa (κ) was 0.4 and internal consistency for the total scale measured by Cronbach's alpha was 0.72.
Covariables
Socioeconomic position. We considered years of education, number of household assets (up to 24) and household wealth index. We used principal components analysis to develop a household wealth index comprising 14 household assets (such as ownership of a fridge, motorcycle and mobile telephone) and interviewer's global rating of household quality.
Social network and social support. We modified existing measures, taking into account the importance in the Thai context of the family and of children. We measured size of neighbourhood family network; frequency of talking to a child; frequency of talking to friends; received support (instrumental, emotional, financial), and perceived adequacy of support from and to children; and received support from others. Reference Wenger12–Reference Sherbourne and Stewart14 We also measured financial transfers from children in three separate ways: remittances defined as amount of money per year transferred to parents to use as they chose; Reference Ozden and Maurice15 substantial gifts valued above the equivalent of US$50 such as a television; and household expenses defined as amount of money per year paid by children directly to cover parents household bills, for example payment to electricity company or health insurers.
Cognitive function. We used immediate recall and delayed recall of a ten-word list learning task from the Consortium to Establish a Registry of Alzheimer's Disease Reference Ganguli, Chandra, Gilby, Ratcliff, Sharma and Pandav16,Reference Welsh, Butters, Mohs, Beekly, Edland and Fillenbaum17 and the animal-naming verbal fluency task, also from the Consortium to Establish a Registry of Alzheimer's Disease. We defined significant cognitive impairment as performance at or below 1.5 standard deviations below the norm for the individuals' age group and educational level.
Physical illnesses and impairments. We used a modified version of the Burvill physical illness scales Reference Burvill, Mowry and Hall18 covering the presence of 13 common health problems affecting different systems, including breathlessness, blackouts, arthritis, weakness, hearing difficulties and heart trouble. If the person said they had such a problem we rated it as impairment if they also said yes when asked if it ‘affects your function a lot’.
Disability. We used the brief version (12-items) of the World Health Organization's Disability Assessment Schedule to rate disability over the past 30 days. Reference Epping-Jordan and Ustun19 Domains included understanding and communicating with the world, getting around, self-care, getting along with people, activities and participation in society. One item (any difficulty with learning new tasks) was deleted as it was not found relevant for older rural people.
Life events and difficulties. We adapted the List of Threatening Experiences Reference Brugha and Cragg20 in the light of qualitative work and following advice from experts in measuring life events in older people. The adaptations included adding difficulties as well as events, restricting rating of events and difficulties to those remaining severe for over 3 weeks that occurred to the participant, an immediate family member or someone perceived as ‘very close’, and adding events to do with caring for grandchildren and to do with problems at school or work for children or grown-up grandchildren.
We used a short version of the questionnaire in situations where information had to be gathered from an informant if the older adult had apparent significant cognitive impairment or was too unwell to complete a full interview.
Questionnaire development
We carried out focus group discussions to explore experiences of rural ageing and outmigration of children, exchanges with family members and expectations surrounding children. This informed the development of the questionnaire that was pre-tested by a team of ten experienced interviewers on three separate occasions. After each pre-test we made modifications by consensus. The final version was back-translated to English and checked for consistency by a bilingual psychiatrist and a bilingual social scientist.
Data collection
The data collection team of 4 supervisors and 12 interviewers each had at least a bachelor's degree. Most had previous experience with interviewing for the demographic surveillance system. Residential training took 10 days and included presentations, role play and practice in pilot villages.
The data collection team stayed in the villages at the headman's house or the temple. Quality control included checks on data completeness and consistency. Interviewers had to return to the participant if data were inadequate, which happened six times. Researchers were in frequent telephone contact and regularly visited the data collection teams. We conducted all interviews in Thai and gathered informed consent from all participants. We gained ethical approval from King's College Research Ethics Committee (No. 05/05-68) and from Mahidol University Institutional Review Board.
Sample size calculation
We initially calculated this based on a comparison of prevalence of depression in those with all children migrated v. those with some children migrated and needed a total sample size of 954 given the proportions expected of those exposed and not exposed to having all their children migrate. In the analyses currently presented the interest was the level of depression in three groups (all/some/no children migrated). With the attained sample size in these three groups, we achieved 90% power to detect a difference of 0.75 on the EURO–D scale given the standard deviation in our sample of 2.8.
Analysis
We used Stata version 9 for Windows (Release 9, College Station, TX: Stata Corporation. 2003). Because of the oversampling the sample was not representative; however, the analyses were reweighted to take this into account. We weighted the data using the product of two sets of probability weights to take account of differential sampling at village and household levels, and used the survey commands in Stata (svyset) for analyses. We analysed the univariate associations between continuous depression score, exposure to outmigration of all children (compared with some or none) and covariables. We used multiple regression to assess the effect of outmigration on depression and taking account of confounding variables, carrying out a Wald test to test the effect of the exposure after adding in potential confounding variables. We adjusted first for variables known to be associated with depression that might confound any association, for example sociodemographic characteristics, physical and cognitive impairment and severe life events. We then adjusted for variables more specific to the outmigration situation that could be mediators, for example time since last child left, social support from children and economic remittances from children. We checked the residuals for normality; there was some skewness that appeared to be related to the small number of participants from whom data were gathered from an informant. We re-ran the model excluding these and there was only negligible difference in the effect size of explanatory variables. We explored interaction between outmigration and variables for which there was some a priori reason to suspect this might exist, for example demographic factors, wealth and support. Interaction terms were tested by putting them into the multivariable model. All tests were Wald tests.
Results
In all, 1620 older adults in 1620 households were sampled, of whom 1300 (80%) were eligible to take part. Reasons for not being eligible were having no living biological, adopted or step-children (82, 5%), having died since 2004 (59, 4%), moved out of the village (110, 7%) or having changed exposure status with respect to having or not having at least one child in the household (72, 4%).
Out of the 1300 eligible, 153 (12%) were non-responders of whom 110 were unavailable for an interview (despite up to ten visits to the household), 21 refused to take part and 22 were too unwell. Those unavailable were mostly away visiting their children. Of the 1147 (88%) who agreed to participate, data were complete for 1104 and incomplete for 43 because the older adult was unwell or cognitively impaired.
In the study sample of 1147 parents, 48% lived with at least one child and 52% lived without at least one child. Of the total, 16% had all children migrated from the district, 68% had some children migrated from the district and 16% had no children migrated from the district (i.e. all children living in the district). Taking into account the weighting, this extrapolates to a province estimate of 4966 parents with all children migrated from the district, 28 522 with some children migrated and 7862 with no children migrated from the district.
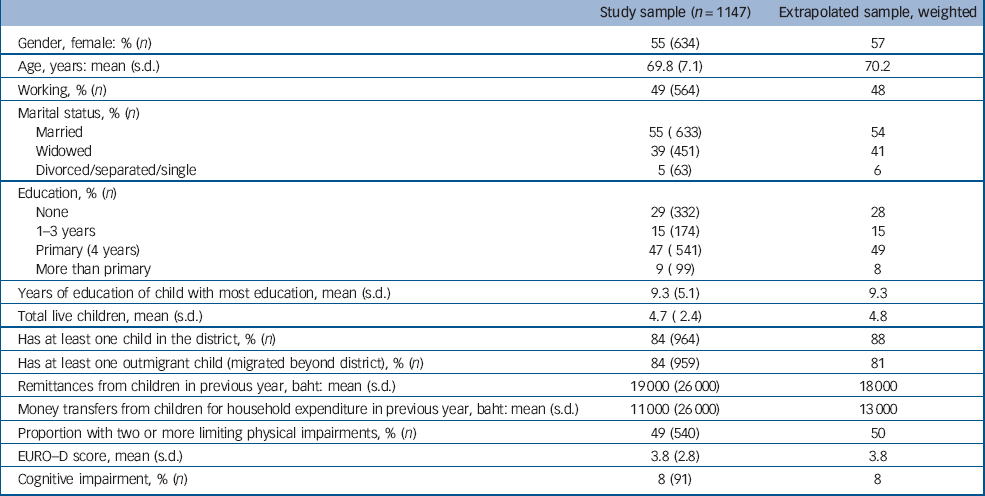
The mean age of the study participants was 70 years (the range was 60–93), 55% were female, 55% were married, and 29% had no education (Table 1). Fourteen per cent lived alone, a further 19% lived with a spouse only and 48% lived with at least one child with or without a spouse or others (data not shown). There were no significant differences from non-responders in terms of age (non-responders 69 years), gender (55% female), living alone (12%), being currently married (54%), or education (27% no education). Weighted estimates of the characteristics extrapolated for the wider province population from which the sample was drawn revealed few differences between the study sample and the estimated province population (Table 1, col. 2). Because we oversampled those not co-resident with a child, the study population has a lower proportion living with a child (48%) than did the estimated province population (63%) and is slightly more likely to have outmigrant children (data not shown). Otherwise there are few differences between the study sample and the estimated province population. The average time living in the district was nearly 50 years.
Table 1 Characteristics of parents
| Study sample (n=1147) | Extrapolated sample, weighted | |
|---|---|---|
| Gender, female: % (n) | 55 (634) | 57 |
| Age, years: mean (s.d.) | 69.8 (7.1) | 70.2 |
| Working, % (n) | 49 (564) | 48 |
| Marital status, % (n) | ||
| Married | 55 (633) | 54 |
| Widowed | 39 (451) | 41 |
| Divorced/separated/single | 5 (63) | 6 |
| Education, % (n) | ||
| None | 29 (332) | 28 |
| 1-3 years | 15 (174) | 15 |
| Primary (4 years) | 47 (541) | 49 |
| More than primary | 9 (99) | 8 |
| Years of education of child with most education, mean (s.d.) | 9.3 (5.1) | 9.3 |
| Total live children, mean (s.d.) | 4.7 (2.4) | 4.8 |
| Has at least one child in the district, % (n) | 84 (964) | 88 |
| Has at least one outmigrant child (migrated beyond district), % (n) | 84 (959) | 81 |
| Remittances from children in previous year, baht: mean (s.d.) | 19 000 (26 000) | 18 000 |
| Money transfers from children for household expenditure in previous year, baht: mean (s.d.) | 11 000 (26 000) | 13 000 |
| Proportion with two or more limiting physical impairments, % (n) | 49 (540) | 50 |
| EURO—D score, mean (s.d.) | 3.8 (2.8) | 3.8 |
| Cognitive impairment, % (n) | 8 (91) | 8 |
Most older parents had at least one child living inside the district and at least one living outside the district. Three-quarters either lived with a child or saw a child daily (79% for the weighted province population).
The distribution of remittances given by children in the previous year was skewed and broad, ranging from none to 300 000 baht with a median of 9000 baht (about US$300). The amount paid directly by children for expenses in the previous year was also skewed and broad, ranging from none to 350 000 baht with a median amount of zero baht.
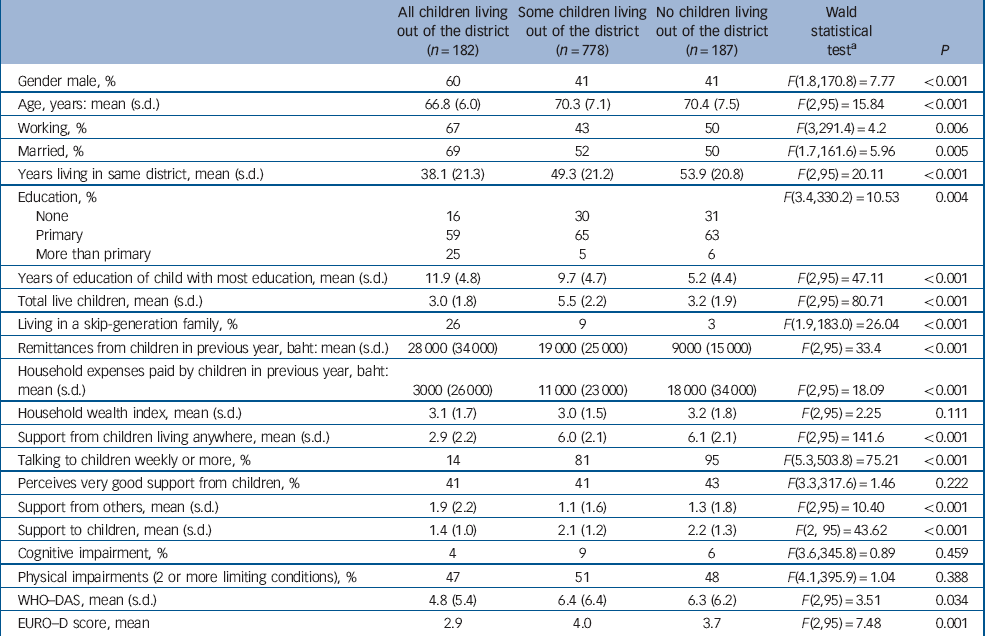
Table 2 shows that those parents with all children living out of the district differed in many ways from those with some children living beyond the district or with all children living inside the district. They were more likely to be younger, male, currently married, working, to have higher education, to live in a skip-generation family (i.e. live with a grandchild but without the grandchild's mother or father) and to get a greater amount in remittances. They were less likely to have household expenses paid by their children. Although they got less overall support from children living anywhere and they talked far less frequently to their children, they were equally as likely to perceive very good support from their children as those with some or all children living close by. They got more support from ‘others’ (not children or grandchildren) and they gave less support to their children. They scored lower for depression and disability than those with some or all children in the district.
Table 2 Weighted characteristics of 1147 parents: with all children living outside the district; with some children living outside the district; and with no children living outside the district
| All children living out of the district (n = 182) | Some children living out of the district (n = 778) | No children living out of the district (n = 187) | Wald statistical testa | P | |
|---|---|---|---|---|---|
| Gender male, % | 60 | 41 | 41 | F(1.8,170.8) = 7.77 | <0.001 |
| Age, years: mean (s.d.) | 66.8 (6.0) | 70.3 (7.1) | 70.4 (7.5) | F(2,95) = 15.84 | <0.001 |
| Working, % | 67 | 43 | 50 | F(3,291.4) = 4.2 | 0.006 |
| Married, % | 69 | 52 | 50 | F(1.7,161.6) = 5.96 | 0.005 |
| Years living in same district, mean (s.d.) | 38.1 (21.3) | 49.3 (21.2) | 53.9 (20.8) | F(2,95) = 20.11 | <0.001 |
| Education, % | F(3.4,330.2) = 10.53 | 0.004 | |||
| None | 16 | 30 | 31 | ||
| Primary | 59 | 65 | 63 | ||
| More than primary | 25 | 5 | 6 | ||
| Years of education of child with most education, mean (s.d.) | 11.9 (4.8) | 9.7 (4.7) | 5.2 (4.4) | F(2,95) = 47.11 | <0.001 |
| Total live children, mean (s.d.) | 3.0 (1.8) | 5.5 (2.2) | 3.2 (1.9) | F(2,95) = 80.71 | <0.001 |
| Living in a skip-generation family, % | 26 | 9 | 3 | F(1.9,183.0) = 26.04 | <0.001 |
| Remittances from children in previous year, baht: mean (s.d.) | 28 000 (34 000) | 19 000 (25 000) | 9000 (15 000) | F(2,95) = 33.4 | <0.001 |
| Household expenses paid by children in previous year, baht: mean (s.d.) | 3000 (26 000) | 11 000 (23 000) | 18 000 (34 000) | F(2,95) = 18.09 | <0.001 |
| Household wealth index, mean (s.d.) | 3.1 (1.7) | 3.0 (1.5) | 3.2 (1.8) | F(2,95) = 2.25 | 0.111 |
| Support from children living anywhere, mean (s.d.) | 2.9 (2.2) | 6.0 (2.1) | 6.1 (2.1) | F(2,95) = 141.6 | <0.001 |
| Talking to children weekly or more, % | 14 | 81 | 95 | F(5.3,503.8) = 75.21 | <0.001 |
| Perceives very good support from children, % | 41 | 41 | 43 | F(3.3,317.6) = 1.46 | 0.222 |
| Support from others, mean (s.d.) | 1.9 (2.2) | 1.1 (1.6) | 1.3 (1.8) | F(2,95) = 10.40 | <0.001 |
| Support to children, mean (s.d.) | 1.4 (1.0) | 2.1 (1.2) | 2.2 (1.3) | F(2, 95) = 43.62 | <0.001 |
| Cognitive impairment, % | 4 | 9 | 6 | F(3.6,345.8) = 0.89 | 0.459 |
| Physical impairments (2 or more limiting conditions), % | 47 | 51 | 48 | F(4.1,395.9) = 1.04 | 0.388 |
| WHO—DAS, mean (s.d.) | 4.8 (5.4) | 6.4 (6.4) | 6.3 (6.2) | F(2,95) = 3.51 | 0.034 |
| EURO—D score, mean | 2.9 | 4.0 | 3.7 | F(2,95) = 7.48 | 0.001 |
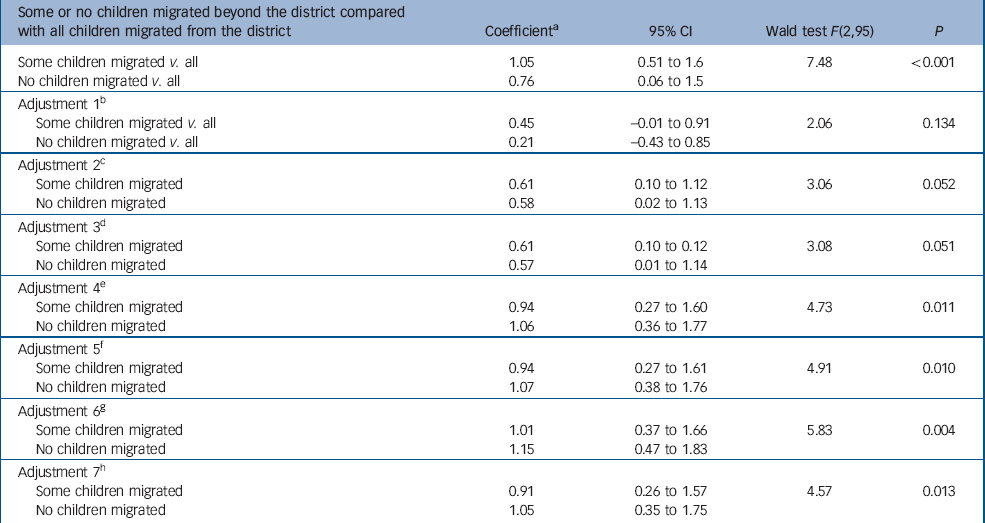
Table 3 shows the multivariate association between outmigration and depression score. Having all children living outside the district is crudely associated with less depression. However, this association is positively confounded by sociodemographic characteristics. After adjusting for all these, the coefficient for having some children migrated fell from 1.05 to 0.45 and the coefficient for having no migrant children fell from 0.76 to 0.21 with a fall in P from <0.001 to 0.134. The association between having all children living outside the district and less depression was negatively confounded by health and social adversity, by social support from children and by payment of expenses by children. After adjusting for these, the coefficient for depression among those having some children migrated rose to 1.01 and among those with no migrant children rose to 1.15 (P = 0.004). There was a slight drop in the effect of migration after taking account of support to children. Even after adjusting for all the variables shown in Table 3, having all children living outside the district remained independently associated with less depression.
Table 3 Association between depression score and migration of children beyond the district (n = 1147): weighted regression
| Some or no children migrated beyond the district compared with all children migrated from the district | Coefficienta | 95% CI | Wald test F(2,95) | P |
|---|---|---|---|---|
| Some children migrated v. all | 1.05 | 0.51 to 1.6 | 7.48 | <0.001 |
| No children migrated v. all | 0.76 | 0.06 to 1.5 | ||
| Adjustment 1b | ||||
| Some children migrated v. all | 0.45 | -0.01 to 0.91 | 2.06 | 0.134 |
| No children migrated v. all | 0.21 | -0.43 to 0.85 | ||
| Adjustment 2c | ||||
| Some children migrated | 0.61 | 0.10 to 1.12 | 3.06 | 0.052 |
| No children migrated | 0.58 | 0.02 to 1.13 | ||
| Adjustment 3d | ||||
| Some children migrated | 0.61 | 0.10 to 0.12 | 3.08 | 0.051 |
| No children migrated | 0.57 | 0.01 to 1.14 | ||
| Adjustment 4e | ||||
| Some children migrated | 0.94 | 0.27 to 1.60 | 4.73 | 0.011 |
| No children migrated | 1.06 | 0.36 to 1.77 | ||
| Adjustment 5f | ||||
| Some children migrated | 0.94 | 0.27 to 1.61 | 4.91 | 0.010 |
| No children migrated | 1.07 | 0.38 to 1.76 | ||
| Adjustment 6g | ||||
| Some children migrated | 1.01 | 0.37 to 1.66 | 5.83 | 0.004 |
| No children migrated | 1.15 | 0.47 to 1.83 | ||
| Adjustment 7h | ||||
| Some children migrated | 0.91 | 0.26 to 1.57 | 4.57 | 0.013 |
| No children migrated | 1.05 | 0.35 to 1.75 |
We found an interaction between poverty and location of children. Depression in parents was highest when the household was poorer. Depression was especially high when the household was poor and no children had migrated (mean EURO–D level 4.8, 95% CI 3.9–5.6) compared with when the household was wealthier and no children had migrated (mean EURO–D level 3.5, 95% CI 2.5–3.6) or compared with when the household was poor and all children had migrated. The interaction term F(2,95) was 4.02, P = 0.021. Depression in parents was also especially common when support from children was low and no children or only some had migrated (Wald test for interaction term F(2,95) = 3.15, P = 0.047).
Discussion
Our findings contradict the notion of widespread abandonment of older people in areas of high outmigration. 3 Although most parents in this rural Thai setting of high outmigration had at least one child living outside the district, around three-quarters either still lived with a child or talked to a child daily and it was rare for all children to be living away from the parents' district. Comparable results have been found in the Philippines, Singapore, other parts of Thailand and China. Reference Chen, Wei, Hu, Qin, Copeland and Hemingway21,Reference Knodel, Ofstedal and Hermalin22
Our findings also do not support the hypothesis that depression is more common in older parents living without any of their children in the same district. In contrast, depression was less common among older parents with all children living outside the district, compared with those living either with some or all children in the same district.
Chance is an unlikely explanation for the finding as the crude and adjusted associations were highly significant. Because the sample was obtained through stratified random sampling and the sampling design was built into the analysis, and because the response rate was good, the likelihood of major biases is small. We were unable to interview those who were travelling to visit their children at the time of the study. It is possible that these were more depressed and seeking support. However, non-responders did not differ on demographic characteristics, hence this is unlikely to explain our findings. We were able to adjust for a large range of confounders that were selected carefully at the outset, although there could be residual confounding, for example measurement of remittances is likely to be prone to non-systematic error. There could be uncontrolled confounding by several factors on which we lacked data, including premorbid mental health and autonomy of the older person that might both encourage migration of family members and promote good mental health. We were however able to adjust for education and household assets, which may to some extent control for prior achievements and capabilities. The construct of depression, and our approach to measurement, were seen as valid by the local mental health providers who were trained locally in psychiatry and are non-English speaking. Also, the EURO–D scale has been validated internationally and in Thailand. It was applied by lay interviewers who were masked to the study hypothesis. Any measurement error should bias towards the null so should not explain our findings. We adjusted for factors that could have been mediators, such as social support and economic remittances, but the effect remained robust.
The findings regarding depression are very interesting and challenge popular notions of the consequences for older people of family separation. 3,Reference Djernes6,Reference King and Vullnetari23 We propose two reasons to explain them.
Pre-existing advantages in families
First, households sending a large proportion of migrants may have advantages at outset from households from where migration is less common. Migration is known to be a ‘selective process’, described as movement of the ‘brightest’ and more advantaged. Reference Skeldon24 In our study, parents with all children migrated were more likely to be male, better educated and married – all variables that would reduce risk for depression – and to have better educated children. Households enabling all children to migrate may have greater personal resources, for example facilitating social networks for their children in the destination area. Although migration can be a response to poverty it is also a search for prosperity by those coming from households able to take up the challenge. Rather than seeing the left behind as ‘passive recipients’ Reference Toyota, Yeoh and Nguyen25 it is likely that they contributed to the decision to migrate as part of family diversification. In contrast having few children migrate could be linked to failed aspirations, increasing the risk for family conflict and parental depression. It is notable that well-planned migration, including family involvement, has been associated with better mental health in Irish migrants to the UK. Reference Ryan, Leavey, Golden, Blizard and King26 Furthermore, in the Thai context, migrant households adapted to separation by keeping contact through telephones (increasingly available and affordable and often shared with relatives and neighbours) and through short visits at crucial times. These approaches enabled children to respond to emergency situations. Although parents with all children migrated received less overall social support from children, they were as likely to perceive very adequate support from children and more likely to receive support from others. Many older people continued to live with a grandchild, which has been shown to be protective against depression in China. Reference Silverstein, Cong and Li27 For special festivals it was standard for children to travel back for 24 h. Knodel has called this ‘the modified extended family’, which he describes as dynamic and unbound by the ‘solid traditional family structure relationship’, with parents linked into their children's migration processes. Reference Knodel and Saengtienchai5
Economic and health benefit v. social cost
Second, the benefits of migration may outweigh the social costs. Many families with migrant members moving within and between low- and middle-income countries tend to benefit economically Reference Ozden and Maurice15 and to have improved general health. Reference Hadi28 Benefits for those who stay behind are influenced by remittances received and by factors for the migrant such as improved income, shared language in the host setting and lower distance between home and host setting. Reference Ozden and Maurice15 For low-skilled migrants from and within low-income settings there is an emphasis on sacrifice, strong family ties and strong obligation. Reference Rigg29,Reference Stockdale30 In our setting, having outmigrant children was strongly associated with receiving more remittances. This will provide not only short-term aid but may give security and well-being. Reference Silverstein, Cong and Li27 Very few older Thais receive a pension but instead rely on children as a main source of income. Reference Knodel, Ofstedal and Hermalin22 The ability to lift households out of poverty may be an important influence on better mental health of those left behind. We found that those with all children migrated gave less support to children and that this in turn was associated with less depression. Having one less mouth to feed or one less to support may reduce parental burden. Reference Rigg29 Another consideration could be that successful outmigrant children raise the social standing of the family. Parents in our study indicated their pride and relief when children found employment and advanced their careers in urban centres, in contrast to the heavy work in the fields for less-educated young people.
Reverse causality of return or non-migration
A contrasting explanation for a higher level of depression in parents with children living close by could be reverse causality. It is possible that children return in response to concerns about parents' mental state and to the onset of disability. We did not have data on return migration. If this was a key explanation we might have seen more evidence of confounding by impairment, disability and life events, which we did not.
Strikingly we found that depression was particularly high in poorer households with no outmigrant children. This inequality raises questions about barriers to migration in poorer households, and potential benefits of interventions and policies to support migration from poorer households. Low socioeconomic status was strongly related to worse depression among older people in rural China. Reference Chen, Wei, Hu, Qin, Copeland and Hemingway21
Study limitations
The limitations of our study include that it is cross-sectional hence many of the links we propose are speculative. Data from our 1-year follow-up of the same parents will be available later and may allow us to show how having migrated children influences chronicity of depressive symptoms in parents but these data may not have the power to address questions about onset. We did not have enough power to study the differential effect of migrant gender, given the concerns about the feminisation of migration, which may adversely affect health of parents left behind. 3 It is not possible to say how much our findings can be generalised to other populations given that migration is context-dependent. However, this study complements other work on migration and depression, Reference Swinnen and Selten1,Reference Ryan, Leavey, Golden, Blizard and King26 and may have implications for the families of migrants moving within other developing and restructuring countries. Future prospective research should test the hypothesis that poor mental health in the parents of young migrants and in young migrants themselves may adversely influence migration decisions or impair successful migration.
Funding
This work was funded by the Wellcome Trust (WT 078567).
Acknowledgements
We thank Dr Bencha Yoddumnern-Attig, Dr Qin Min, Khaing Khaing Soe and the field staff of the Kanchanaburi DSS for their support.








eLetters
No eLetters have been published for this article.