Previous self-harm is an important risk factor for suicide, Reference Sakinofsky, Hawton and van Heeringen1 occurring in 40–60% of instances. Reference Foster, Gillespie and McClelland2–Reference Suokas and Lonnqvist5 One systematic review found that those who harmed themselves had a 0.5–2% risk of suicide within 1 year of the index self-harm act, and a suicide risk in excess of 5% after 9 years. Reference Owens, Horrocks and House6 Long-term follow-up studies have found that the increased risk of suicide persists. Reference Jenkins, Hale, Papanastassiou, Crawford and Tyrer7 The risk of suicide is 30–100 times higher within the first year following the self-harm episode than in the general population. Reference Hawton, Zahl and Weatherall3,Reference Greer and Bagley8–Reference Cooper, Kapur, Webb, Lawlor, Guthrie and Mackway-Jones9 Other studies have suggested that those who self-harm also have higher mortality from other causes. Reference Beautrais10
Male gender and older age have been suggested as predictors of suicide after self-harm, Reference Hawton, Zahl and Weatherall3 although not all studies have found a gender difference. Reference Beautrais10 Other demographic factors and index self-harm methods have received less attention as predictors. Reference Skogman, Alsen and Ojehagen11 Few previous studies have investigated risk factors for both suicide and all causes of death in a systematic and representative sample of people who self-harm. Reference Suominen, Isometsa, Haukka and Lonnqvist12 Methodological problems cited in one systematic review include small and highly selected samples, weak methods for detecting suicide during follow-up and flawed analysis. Reference Owens, Horrocks and House6 Another limitation is that nearly all reports about this topic have come from Europe, North America and Australasia, Reference Owens, Horrocks and House6 with little research from Asia.
In Taiwan, suicide rates have increased more than threefold during the past 10 years, and suicide has been the ninth leading cause of death since 1999. The relationship between self-harm and suicide is important for planning interventions to reduce suicide rates. Reference Owens, Horrocks and House6 In this study, we aimed to assess rates of mortality after self-harm from suicide and other causes in Taiwan through a prospective community-based cohort study. A further objective was to investigate demographic factors and potential lethality of the self-harm as predictors for later mortality.
Method
Study sample
The analysed sample were individuals with an episode of self-harm consecutively recruited from a suicide and self-harm register system in Nantou County from July 2000 to March 2003. Nantou County is located in central Taiwan, with a total population of approximately 500 000. The county is close to the centre of a major earthquake that took place on 21 September 1999, and a community mental health centre was established in this county to provide mental healthcare for survivors from the earthquake disaster, supported by a specific reconstruction fund from the government. The centre was staffed with ten mental health nurses, five psychologists and five social workers, and was actively supervised by two senior psychiatrists. In collaboration with the local health authority, this centre established a new reporting system in June 2000 to identify all inhabitants who carried out an act of suicide/self-harm. This was the first population register in Taiwan to systematically collect data on both suicide and self-harm, and has been described previously. Reference Chen, Tan, Cheng, Chen, Liao and Stewart13,Reference Chen, Cheng, Tan, Chen, Chen and Stewart14
Definition of self-harm
Self-harm was defined as all acts of self-poisoning or self-injury, irrespective of the degree of suicidal intent. 15 Other terms in common use, namely attempted suicide and parasuicide, are subsumed within this definition. Reference Hawton, Townsend, Arensman, Gunnell, Hazell and House16 In this study, in practice, any episodes of self-harm resulting in medical attention referred by a variety of community resources as detailed below were included.
Data collection
A structured data coding form was designed to ensure the quality of the registration system. This form contained sociodemographic information (age, gender, education, marital status, location of residency) and information regarding the suicide/self-harm act (date of the self-harm and method(s) used), and the nature of the referral source(s). A detailed description of the self-harm method included the name of any drugs or chemicals used. This form was completed, for all people who carried out an act of suicide/self-harm, by a group of informants working in all agencies and settings where cases were routinely identified. They included doctors and nurses in the health sector (general hospital emergency room, general practice and local public health centres), and workers in other public and private sectors (firefighters, police officers, social workers and non-governmental organisation workers). A training course was conducted for all potential informants on the use of the form before the inception of the register in 2000. A meeting was held every 3 months with leaders of all referral sources to review the operation of the reporting system. Nantou Health Bureau officers monitored the health sector regularly. All completed forms were forwarded to the community mental health centre within 24 hours. Staff at the centre checked the forms to identify any missing or unclear information, which was then completed during regular weekly visits to the agencies/settings through further questioning of informants. The study received ethical approval from the Tasotun Psychiatric Center Research Ethics Committee. Each person's first self-harm act during the study period was treated as the index episode. Follow-up was then carried out between July 2000 and December 2007.
Identification of suicide
Information regarding personal identification of all individuals (national identifier number, name, gender, location of residency and date of birth) recruited during the study period were checked against the databases of the national death register system, in which all deaths from unnatural causes (suicide, accidental death and homicide) are decided on by a death verdict jointly assigned by a prosecutor and a coroner, whose main concern is the possibility of homicide. Since a suicide verdict is important in this decision, a thorough enquiry is usually made about suicide intentions. In a previous psychological autopsy study in Taiwan, only 2 out of 117 suicides were misclassified by coroners and prosecutors as accidental deaths. Reference Cheng17
Risk and standardised mortality ratios for suicide, other causes and all causes
The risk of suicide, death by other causes, and total mortality (which included all unnatural deaths and deaths by natural causes) were calculated in terms of the number at risk: that is, the number of individuals that entered the respective interval alive minus half of the number of those lost or censored in the respective interval. Each person's first presentation within the study period was used in the calculation of risk over time. Using indirect standardisation, annual age- and gender-specific mortality rates from suicide, non-suicide causes and all causes from Taiwanese national mortality statistics for the period from 2001 to 2003 were applied to the study sample to compute expected numbers of deaths. The standardised mortality ratio (SMR) within 1 year of self-harm in the study sample was calculated as a ratio of actual versus expected numbers of deaths.
Statistical analysis
Each person's first presentation within the study period was used in the calculation of risk over time. All individuals traced until December 2007 by the national death register system for any length of time from their first presentation were entered into a survival analysis. The risk of suicide, of mortality excluding suicide and total mortality during the follow-up period was calculated using survival curves. We calculated annual mortality rates for each of the 7 years following the index episode of self-harm, as well as cumulative mortality rates for the first 5 years since the self-harm episode. In the survival analysis, the time function was calculated as the number of months from the index episode of self-harm to December 2007 (end of follow-up) for those who survived until then, or until the date of death if this preceded the end of the follow-up interval. Cox regression models were fitted to estimate the effects of gender, age, education and marital status as well as potential lethality of method used in the index episode. We categorised the suicide methods as high lethality (fatality proportion >26%) and low lethality (fatality proportion <4%) groups, as previously reported. Reference Chen, Cheng, Tan, Chen, Chen and Stewart14 The high lethality group consisted of pesticide, gas, hanging and other violent methods, whereas the low lethality group included drug ingestion and self-cutting. Hazard ratios with 95% confidence intervals were calculated. Analyses were carried out using the Statistical Package for the Social Sciences version 13.0 for Windows and STATA version 9.0 for Windows.
Results
Sample characteristics
A total of 1083 cases of self-harm were registered between July 2000 and March 2003. Of these, 1080 (99.7%) could be traced. Until December 2007, follow-up information was available for all individuals with a mean follow-up time of 5.8 years (s.d. = 1.7, range 1 day to 7.6 years). The sample consisted of 392 (36.3%) men and 688 (63.7%) women. The mean age was 37.1 years (s.d. = 15.9), ranging from 11 to 90; 67.8% had fewer than 9 years of education; nearly 90% were living in the Nantou area; over half of the individuals were married (52.2%), with 27.9% single, 13.9% divorced and 5.5% widowed. The methods of self-harm included drug overdose (n = 472, 43.7%), self-cutting (n = 253, 23.4%), pesticide poisoning (n = 255, 23.6%) and other violent methods such as jumping from a high place or drowning (n = 48, 4.4%), gas inhalation (n = 32, 3.0%) and hanging (n = 13, 1.2%) (Table 1).
Table 1 Characteristics of 1080 individuals who self-harmed, Nantou, Taiwan, 2000–2003

| Characteristics | Self-harm,a n (%) |
|---|---|
| Gender | |
| Female | 688 (63.7) |
| Male | 392 (36.3) |
| Age, years | |
| <25 | 273 (25.3) |
| 25–44 | 526 (48.7) |
| 45–64 | 196 (18.1) |
| ≥ 65 | 85 (7.9) |
| Residence | |
| Other area | 110 (10.2) |
| Suburban | 624 (57.8) |
| Rural | 346 (32.0) |
| Education | |
| > 9 years | 327 (30.3) |
| ≤ 9 years | 732 (67.8) |
| Missing | 21 (1.9) |
| Marital status | |
| Single | 301 (27.9) |
| Married | 564 (52.2) |
| Divorced | 150 (13.9) |
| Widowed | 59 (5.5) |
| Missing | 6 (0.6) |
| Method | |
| Drug overdose | 472 (43.7) |
| Self-cutting | 253 (23.4) |
| Pesticide poisoning | 255 (23.6) |
| Other violent | 48 (4.4) |
| Gas inhalation | 32 (3.0) |
| Hanging | 13 (1.2) |
| Missing | 7 (0.6) |
Risk of suicide following self-harm
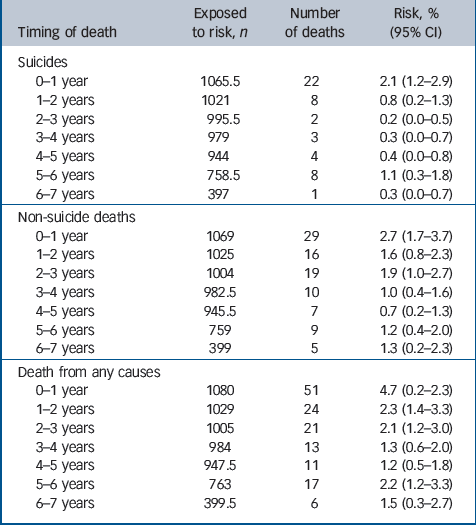
By the end of the follow-up period, 48 (4.4%) individuals had completed suicide: 31 men (2.9%) and 17 women (1.6%). More suicides (n = 22, 45.8%) occurred during the first year after the self-harm index episode than in any other year. The cumulative risk by 1 year was 2.1%, by 2 years 2.8% and by 5 years 3.8%. The risk continued to accumulate but the amplitude was highest within the first year (Table 2). In unadjusted Cox regression analyses, risk factors for suicide mortality were found to be male gender, an older age and higher lethality of method used in the index self-harm act. Men had nearly a 3.5-fold higher suicide mortality compared with women and those aged above 64 had 5.9 times higher suicide mortality than those aged 10–24 years. After adjusting for gender, there was no significant difference in the association between self-harm method and risk of suicide. The final independent predictors were male gender and increased age in the adjusted model (Table 3).
Table 2 Comparison of risk by timing of death, by suicide, non-suicide causes and any causes
| Timing of death | Exposed to risk, n | Number of deaths | Risk, % (95% CI) |
|---|---|---|---|
| Suicides | |||
| 0–1 year | 1065.5 | 22 | 2.1 (1.2–2.9) |
| 1–2 years | 1021 | 8 | 0.8 (0.2–1.3) |
| 2–3 years | 995.5 | 2 | 0.2 (0.0–0.5) |
| 3–4 years | 979 | 3 | 0.3 (0.0–0.7) |
| 4–5 years | 944 | 4 | 0.4 (0.0–0.8) |
| 5–6 years | 758.5 | 8 | 1.1 (0.3–1.8) |
| 6–7 years | 397 | 1 | 0.3 (0.0–0.7) |
| Non-suicide deaths | |||
| 0–1 year | 1069 | 29 | 2.7 (1.7–3.7) |
| 1–2 years | 1025 | 16 | 1.6 (0.8–2.3) |
| 2–3 years | 1004 | 19 | 1.9 (1.0–2.7) |
| 3–4 years | 982.5 | 10 | 1.0 (0.4–1.6) |
| 4–5 years | 945.5 | 7 | 0.7 (0.2–1.3) |
| 5–6 years | 759 | 9 | 1.2 (0.4–2.0) |
| 6–7 years | 399 | 5 | 1.3 (0.2–2.3) |
| Death from any causes | |||
| 0–1 year | 1080 | 51 | 4.7 (0.2–2.3) |
| 1–2 years | 1029 | 24 | 2.3 (1.4–3.3) |
| 2–3 years | 1005 | 21 | 2.1 (1.2–3.0) |
| 3–4 years | 984 | 13 | 1.3 (0.6–2.0) |
| 4–5 years | 947.5 | 11 | 1.2 (0.5–1.8) |
| 5–6 years | 763 | 17 | 2.2 (1.2–3.3) |
| 6–7 years | 399.5 | 6 | 1.5 (0.3–2.7) |
Table 3 Cox's proportional hazards regression models for death from suicide (n = 1080)

| Unadjusted hazard ratio | Adjusted hazard ratio | ||||
|---|---|---|---|---|---|
| Variable | Deaths from suicide,a n/N (%) | Estimate (95% CI) | P | Estimate (95% CI) | P |
| Gender | |||||
| Female | 17/688 (2.5) | 1.00 | 1.00 | ||
| Male | 31/392 (7.9) | 3.46 (1.92–6.26) | <0.001 | 2.47 (1.28–4.75) | 0.007 |
| Age, years | |||||
| 10–24 | 5/273 (1.8) | 1.00 | 1.00 | ||
| 25–44 | 25/526 (4.8) | 2.66 (1.02–6.95) | 0.046 | 3.24 (1.14–9.23) | 0.028 |
| 45–64 | 11/196 (5.6) | 3.34 (1.16–9.62) | 0.025 | 4.32 (1.22–15.32) | 0.023 |
| ≥ 65 | 7/85 (8.2) | 5.87 (1.86–18.53) | 0.003 | 8.00 (1.95–32.88) | 0.004 |
| Residence | |||||
| Rural | 17/346 (4.9) | 1.00 | 1.00 | ||
| Suburban | 28/624 (4.5) | 0.91 (0.50–1.65) | 0.746 | 0.88 (0.48–1.63) | 0.694 |
| Other area | 3/110 (2.7) | 0.55 (0.16–1.88) | 0.342 | 0.58 (0.17–1.99) | 0.384 |
| Education | |||||
| > 9 years | 16/327 (4.9) | 1.00 | 1.00 | ||
| ≤ 9 years | 32/732 (4.4) | 0.94 (0.52–1.72) | 0.844 | 0.74 (0.39–1.41) | 0.363 |
| Marital status | |||||
| Single | 14/301 (4.7) | 1.00 | 1.00 | ||
| Married | 22/564 (3.9) | 0.85 (0.43–1.65) | 0.624 | 0.49 (0.22–1.11) | 0.086 |
| Divorced | 9/150 (6.0) | 1.30 (0.56–3.00) | 0.542 | 0.93 (0.37–2.33) | 0.871 |
| Widowed | 3/59 (5.1) | 1.23 (0.35–4.28) | 0.746 | 0.50 (0.12–2.14) | 0.348 |
| Method | |||||
| Low fatalityb | 25/725 (3.4) | 1.00 | 1.00 | ||
| High fatalityc | 23/348 (6.6) | 2.05 (1.16–3.60) | 0.013 | 1.33 (0.72–2.46) | 0.358 |
Risk of general and non-suicide mortality following self-harm
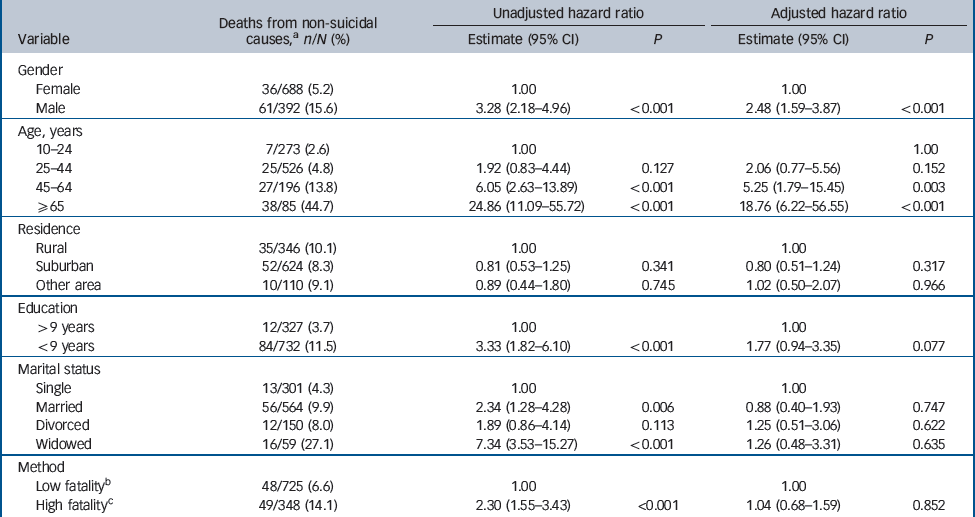
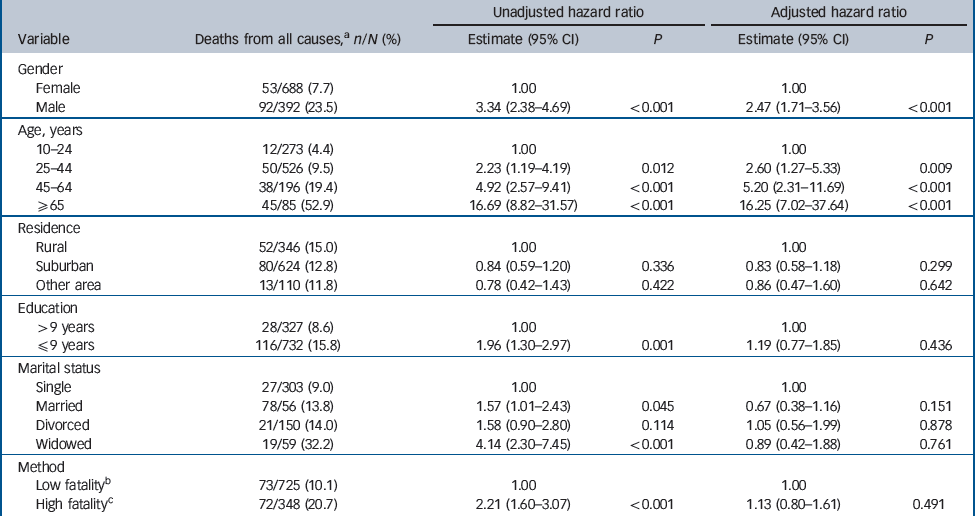
Of the 1080 individuals who self-harmed, a total of 145 (13.4%) died during the follow-up period, 97 of whom died from causes other than suicide (9.0%). The risk by 1 year was 2.7%, 2 years 4.2% and 5 years 7.8% for non-suicide causes and was 4.7%, 6.9% and 11.4% respectively for all-cause mortality (Table 2). The frequency was also highest within the first year for both of these outcomes (Table 2). In the unadjusted Cox regression model, risk factors for death from any cause and non-suicide mortality were male gender, increased age, lower education, widowed status, and use of self-harm methods that had high lethality. In the adjusted model, only male gender and older age were independent predictors of both outcomes (Tables 4 and5).
Table 4 Cox's proportional hazards regression models for death from non-suicide causes (n = 1080)
| Deaths from non-suicidal causes,a n/N (%) | Unadjusted hazard ratio | Adjusted hazard ratio | |||
|---|---|---|---|---|---|
| Variable | Estimate (95% CI) | P | Estimate (95% CI) | P | |
| Gender | |||||
| Female | 36/688 (5.2) | 1.00 | 1.00 | ||
| Male | 61/392 (15.6) | 3.28 (2.18–4.96) | <0.001 | 2.48 (1.59–3.87) | <0.001 |
| Age, years | |||||
| 10–24 | 7/273 (2.6) | 1.00 | 1.00 | ||
| 25–44 | 25/526 (4.8) | 1.92 (0.83–4.44) | 0.127 | 2.06 (0.77–5.56) | 0.152 |
| 45–64 | 27/196 (13.8) | 6.05 (2.63–13.89) | <0.001 | 5.25 (1.79–15.45) | 0.003 |
| ≥ 65 | 38/85 (44.7) | 24.86 (11.09–55.72) | <0.001 | 18.76 (6.22–56.55) | <0.001 |
| Residence | |||||
| Rural | 35/346 (10.1) | 1.00 | 1.00 | ||
| Suburban | 52/624 (8.3) | 0.81 (0.53–1.25) | 0.341 | 0.80 (0.51–1.24) | 0.317 |
| Other area | 10/110 (9.1) | 0.89 (0.44–1.80) | 0.745 | 1.02 (0.50–2.07) | 0.966 |
| Education | |||||
| > 9 years | 12/327 (3.7) | 1.00 | 1.00 | ||
| <9 years | 84/732 (11.5) | 3.33 (1.82–6.10) | <0.001 | 1.77 (0.94–3.35) | 0.077 |
| Marital status | |||||
| Single | 13/301 (4.3) | 1.00 | 1.00 | ||
| Married | 56/564 (9.9) | 2.34 (1.28–4.28) | 0.006 | 0.88 (0.40–1.93) | 0.747 |
| Divorced | 12/150 (8.0) | 1.89 (0.86–4.14) | 0.113 | 1.25 (0.51–3.06) | 0.622 |
| Widowed | 16/59 (27.1) | 7.34 (3.53–15.27) | <0.001 | 1.26 (0.48–3.31) | 0.635 |
| Method | |||||
| Low fatalityb | 48/725 (6.6) | 1.00 | 1.00 | ||
| High fatalityc | 49/348 (14.1) | 2.30 (1.55–3.43) | <0.001 | 1.04 (0.68–1.59) | 0.852 |
Table 5 Cox's proportional hazards regression models for death from all causes (n = 1080)
| Unadjusted hazard ratio | Adjusted hazard ratio | ||||
|---|---|---|---|---|---|
| Variable | Deaths from all causes,a n/N (%) | Estimate (95% CI) | P | Estimate (95% CI) | P |
| Gender | |||||
| Female | 53/688 (7.7) | 1.00 | 1.00 | ||
| Male | 92/392 (23.5) | 3.34 (2.38–4.69) | <0.001 | 2.47 (1.71–3.56) | <0.001 |
| Age, years | |||||
| 10–24 | 12/273 (4.4) | 1.00 | 1.00 | ||
| 25–44 | 50/526 (9.5) | 2.23 (1.19–4.19) | 0.012 | 2.60 (1.27–5.33) | 0.009 |
| 45–64 | 38/196 (19.4) | 4.92 (2.57–9.41) | <0.001 | 5.20 (2.31–11.69) | <0.001 |
| ≥ 65 | 45/85 (52.9) | 16.69 (8.82–31.57) | <0.001 | 16.25 (7.02–37.64) | <0.001 |
| Residence | |||||
| Rural | 52/346 (15.0) | 1.00 | 1.00 | ||
| Suburban | 80/624 (12.8) | 0.84 (0.59–1.20) | 0.336 | 0.83 (0.58–1.18) | 0.299 |
| Other area | 13/110 (11.8) | 0.78 (0.42–1.43) | 0.422 | 0.86 (0.47–1.60) | 0.642 |
| Education | |||||
| > 9 years | 28/327 (8.6) | 1.00 | 1.00 | ||
| ≤ 9 years | 116/732 (15.8) | 1.96 (1.30–2.97) | 0.001 | 1.19 (0.77–1.85) | 0.436 |
| Marital status | |||||
| Single | 27/303 (9.0) | 1.00 | 1.00 | ||
| Married | 78/56 (13.8) | 1.57 (1.01–2.43) | 0.045 | 0.67 (0.38–1.16) | 0.151 |
| Divorced | 21/150 (14.0) | 1.58 (0.90–2.80) | 0.114 | 1.05 (0.56–1.99) | 0.878 |
| Widowed | 19/59 (32.2) | 4.14 (2.30–7.45) | <0.001 | 0.89 (0.42–1.88) | 0.761 |
| Method | |||||
| Low fatalityb | 73/725 (10.1) | 1.00 | 1.00 | ||
| High fatalityc | 72/348 (20.7) | 2.21 (1.60–3.07) | <0.001 | 1.13 (0.80–1.61) | 0.491 |
SMR in the first year following self-harm
Age and gender SMRs were applied to compare self-harm case outcomes with those of the general population. Standardised mortality ratios were described as simple ratios rather than according to the convention of 100 = no difference, because of the large size of the effects. Compared with the annual expected numbers of suicide deaths derived from general population data in Nantou County and in Taiwan, individuals who self-harmed had an 87-fold and a 131-fold respective risk of suicide within the first year after the index self-harm act. The respective SMRs for non-suicide death were 4.3 and 4.7, and for all causes were 7.3 and 8.1. Similar SMRs were observed for non-suicide mortality between men and women, whereas suicide SMRs were twice as strong in men compared with women. The higher SMR for suicide and non-suicide death also existed for 4-year cumulative risk. Individuals who self-harmed had a 35-fold and a 52-fold cumulative risk of suicide within 4 years after the index self-harm act compared with the risks of the general populations in Nantou County and Taiwan respectively.
Discussion
To our knowledge, this is the first epidemiological study to investigate mortality following self-harm in a defined community population in Asia. The main findings were that the risk of suicide in the subsequent year was 2.1% (95% CI 1.2–2.9) representing an approximately 131-fold age and gender standardised increase compared with the general population in Taiwan. The risk of all-cause mortality in the first year was 4.7% (95% CI 3.5–6.0): approximately eight times the risk in the general population. Male gender and older age were independent risk factors for both suicide and non-suicide mortality. Use of more lethal methods in the index self-harm episode was associated with subsequent mortality before adjustment but this association was confounded by gender.
Strengths and limitations
Through the cooperation of many different agencies, including local government, public health, social services, firefighters as well as police and medical services, the present study has several strengths. First, the large sample data-set is based on a consecutive community sample of people who were registered following an act of self-harm, and is not restricted to individuals seen by mental health services or those admitted to general hospital wards or emergency rooms. Second, we used survival analysis that takes account of the variable duration of follow-up. Third, we were able to trace a high proportion of the sample, with only 0.3% untraced. Finally, besides the record at the index event, mental health centre staff and local public health nurses attempted to follow-up all cases, in order to correct missing data, resulting in a high-quality data-set and high tracing rate.
Loss to follow-up is a major methodological consideration in cohort studies, and we had three individuals that were untraceable and they were all male. Nonetheless, due to our large sample size and high tracing rate, we feel this will have had little impact on the findings. The identification of suicide mortality in Taiwan has already been demonstrated to have high validity in one previous study, which found higher than 98% accuracy. Reference Cheng17 However, a few suicide deaths may still be missed owing to their inclusion in other categories. Compared with previous studies, some of which have chosen to define suicide as including deaths from undetermined causes and accidental poisonings as well as official suicides, Reference Hawton, Zahl and Weatherall3 our definition is relatively restrictive. If we adopted a definition of suicide that included deaths from undetermined causes and accidental poisonings, the number would increase to 52 (4.8%), with a cumulative risk by 1 year of 2.3%, by 2 years of 3.2% and by 5 years of 4.2%: slightly higher than the original results.
High suicide risk after self-harm
Our findings demonstrate an important risk of fatal repetition of self-harm in this sample, especially within the following year. The 2.1% risk in the first year is relatively high compared with corresponding figures reported in the UK ranging from 0.5 to 0.7%, Reference Hawton, Zahl and Weatherall3,Reference Cooper, Kapur, Webb, Lawlor, Guthrie and Mackway-Jones9,Reference Owens, Wood, Greenwood, Hughes and Dennis18 but is very close to the finding from a systematic review with a median value of 2.0%. Reference Owens, Horrocks and House6 Heterogeneity in research of this nature may arise from different distributions of risk factors between samples and source populations, such as higher proportions of younger people with lower consequent suicide, or differences in underlying suicide rates between different countries. Reference Hawton, Zahl and Weatherall3 In our sample, the risk was highest in the first year and continues to accumulate. Cooper and colleagues Reference Cooper, Kapur, Webb, Lawlor, Guthrie and Mackway-Jones9 also found that risk was particularly high immediately (6 months) after the index self-harm act. This has clearly important implications for suicide prevention. However, several longer follow-up studies have suggested that the risk of consequent suicide remains raised even 16–37 years later Reference Jenkins, Hale, Papanastassiou, Crawford and Tyrer7,Reference Owens, Wood, Greenwood, Hughes and Dennis18,Reference Suominen, Isometsa, Suokas, Haukka, Achte and Lonnqvist19 and have stressed the importance of long-term follow-up.
Excess total and non-suicide mortality
The present study also found higher overall and non-suicide mortality rates after self-harm, compared with the general population. These risks were also highest in the first year after self-harm and continued to accumulate. Previous studies have also found that only part of the elevated all-cause mortality rate following self-harm is explained by suicide, and that there remains an unexplained component. Reference Suominen, Isometsa, Haukka and Lonnqvist12,Reference Carter, Reith, Whyte and McPherson20 Some investigators have argued that the elevated non-suicide mortality may be explained by accidental deaths rather than deaths from natural causes Reference Beautrais10,Reference Gibb, Beautrais and Fergusson21 and some of these in turn may result from misclassified suicide deaths. Reference Mohler and Earls22 However, one study found that natural causes of death besides accidents were also higher after self-harm. Reference Carter, Reith, Whyte and McPherson20 One possible explanation lies in worse physical health caused by the method of self-harm such as damage incurred as a result of pesticide ingestion, burns, gas and other chemical substances. In unadjusted analyses, we found that the lethality of the self-harm method was associated with higher non-suicide and overall mortality. However, men and older people have been found to be more likely to choose more violent methods that will result in more negative physical consequences. In addition, older people may be more physically vulnerable to any damage incurred, even potentially from lower lethality methods such as drug overdose. Consistent with this, the association between method lethality and subsequent non-suicide mortality was reduced substantially after adjustment for age and gender. Another possibility is that individuals who self-harm have a high proportion of mental disorder such as depression, Reference Skegg23 which itself is associated with an increased all-cause mortality risk, Reference Prince, Patel, Saxena, Maj, Maselko and Phillips24 an association which is not fully explained by confounding or mediation by behavioural or lifestyle factors, and possibly implying specific biological mechanisms and/or limited healthcare access as underlying causal pathways. Related to this, mental disorder is also associated with the risk of incident physical disorders such as coronary heart disease Reference Hemingway and Marmot25 and diabetes, Reference Golden, Williams, Ford, Yeh, Paton Sanford and Nieto26 as well as with reduced treatment adherence. Reference Blazer, Hybels and Pieper27 These may all play a role in non-suicide mortality following self-harm.
Age and gender
We found that the risk of suicide following self-harm was much higher in men than in women, even after controlling for the effect of age and method used in the index episode. This finding is consistent with reports from Western countries. Reference Hawton, Zahl and Weatherall3,Reference Nordstrom, Samuelsson and Asberg28,Reference Suokas, Suominen, Isometsa, Ostamo and Lonnqvist29 For SMRs, both within 1 year and over the full follow-up period, men were at a higher risk than women. The risk was also found to increase prominently with age at the time of the self-harm episode and those aged over 64 years had a nearly sixfold higher risk than those aged 10–24 years, which also accords with a previous report. Reference Hawton, Zahl and Weatherall3 This finding is consistent with the suggestion in other settings that self-harm in men and older people is associated with higher suicidal intent, even after a failed attempt. This would have obvious clinical implications regarding the need to assess and monitor intent, and develop appropriate and acceptable psychosocial and supportive interventions for those most at risk.
Other factors
Apart from male gender and increased age, other demographic factors such as education, marriage and living area had no influence on consequent suicide or other mortality in adjusted models. Although lethality of suicide method was associated with a higher risk of suicide in the unadjusted model, this association was confounded by gender. For non-suicide and all-cause mortality, the method of self-harm was again not associated in the final model after controlling for gender and age.
Implications
Suicide is a relative rare event that has made its prediction and prevention difficult. Results from this report, as with findings from other studies, support the view that people with a history of self-harm should be a particular focus for prevention programmes. This is particularly the case for men and older people, for whom risk-reducing interventions are most pressingly required. The higher death rate from non-suicidal causes after self-harm emphasises the importance of physical healthcare among those who self-harm, both in terms of delayed or chronic effects of the self-harm act itself, and in terms of general health promotion and disease prevention.
Funding
R.S. is funded by the NIHR Specialist Biomedical Research Centre for Mental Health at the South London and Maudsley NHS Foundation Trust and Institute of Psychiatry, King's College London.
Acknowledgements
The authors thank the staffs of Nantou Mental Health Center for their excellent work in data collection.










eLetters
No eLetters have been published for this article.