The International Pilot Study of Schizophrenia (IPSS) 1 and the Determinants of Outcome of Severe Mental Disorders (DOS) study Reference Jablensky, Sartorius, Ernberg, Anker, Korten and Cooper2 were conducted over 25 years ago by the World Health Organization (WHO) to analyse regional differences in the incidence and outcomes of schizophrenia. Outcomes over 2–5 years varied among the different areas; participants living in low- and middle-income countries had better outcomes than those in high-income areas. Reference Sartorius, Jablensky and Shapiro3,Reference Leff, Sartorius, Jablensky, Korten and Ernberg4 This unexpected finding was confirmed in the long-term (15 and 25 years) International Study of Schizophrenia (ISoS) coordinated by the WHO. Reference Harrison, Hopper, Craig, Laska, Siegel and Wanderling5,Reference Hopper and Wanderling6 The reasons for better outcomes in low- and middle-income countries are not fully understood and much debated, but it has been suggested that sociocultural factors including close family support and interactions may play an important role. Reference Kulhara and Chakrabarti7
Some researchers have questioned whether schizophrenia really does have a better course and outcome in low- and middle-income countries. Reference Cohen, Patel, Thara and Gureje8,Reference Patel, Cohen, Thara and Gureje9 These authors highlighted the methodological limitations of the WHO studies, the lack of evidence on specific sociocultural factors as contributing to the better outcomes, and cited new evidence of poor prognosis of schizophrenia from studies in low- and middle-income countries.
In addition to the WHO studies, other long-term follow-up studies have focused on the course of schizophrenia. Reference Ciompi10–Reference Shepherd, Watt, Fallon and Smeeton15 These studies have shown considerable heterogeneity in outcomes, but have tended to be single-country studies. There has not been any recent multinational study with a large enough sample size to analyse whether the geographic differences in outcome seen in the WHO studies are still present today.
Studies have shown that more individuals with schizophrenia achieve clinical remission than functional remission, Reference Lambert, Schimmelmann, Naber, Schacht, Karow and Wagner16 and some people may experience functional remission despite ongoing symptoms, Reference Wunderink, Sytema, Nienhuis and Wiersma17 indicating that different factors may predict symptom versus functional remission. However, clinical remission is associated with better functional outcome than non-remission. Reference Boden, Sundstrom, Lindstrom and Lindstrom18
The aims of this study are to determine the frequency of symptom and functional remission in out-patients with schizophrenia in different regions of the world. We will also analyse the sociodemographic and clinical factors associated with both outcomes. We hypothesise that there will be differences in symptom and functional remission between regions, and that each dimension will follow different patterns.
Method
Study design
The Schizophrenia Outpatient Health Outcomes (SOHO) study was a 3-year, prospective, observational study primarily designed to assess the comparative costs and outcomes associated with antipsychotic use in out-patients initiating or changing antipsychotic medication for schizophrenia (with an emphasis on olanzapine compared with other antipsychotics). The SOHO study was conducted in 10 Western European countries, Reference Haro, Edgell, Jones, Alonso, Gavart and Gregor19,Reference Haro, Edgell, Novick, Alonso, Kennedy and Jones20 and in 27 countries across 4 continents as the Intercontinental SOHO (IC-SOHO). Reference Dossenbach, Arango-Davila, Silva Ibarra, Landa, Aguilar and Caro21 Both studies shared the same methodology. Three-year data from both studies have been published elsewhere. Reference Haro, Novick, Suarez, Alonso, Lepine and Ratcliffe22,Reference Dossenbach, Pecenak, Szuic, Irimia, Anders and Logozar-Perkovic23 Data from all 37 participating countries have been pooled to produce the Worldwide-SOHO (W-SOHO) data-set, which includes a total of 17 384 participants. The SOHO studies were non-interventional, with all treatment (including flexible dosing and use of concomitant therapies and medications) at the discretion of the treating psychiatrist. No medications were provided by the study sponsor; investigators were free to prescribe any antipsychotic medication indicated for schizophrenia. Individuals were assessed at study entry and during scheduled study visits at 3, 6, 12, 18, 24, 30 and 36 months post-baseline. The study was approved and conducted in accordance with local (country) ethics and regulatory requirements; all participants consented to participate.
Participant population
To ensure the study population was representative as much as possible of actual clinical practice, minimal selection criteria were applied. All individuals aged 18 years or over, who met DSM-IV 24 or ICD-10 25 criteria for schizophrenia, and who were initiating or changing antipsychotic medication at study entry in an out-patient, ambulatory or community setting (or in hospital during an admission scheduled for the initiation or change for up to 2 weeks) were considered eligible unless they were participating in another study that included a treatment intervention and/or an investigational drug. Study sites were established in 37 countries across 6 regions. Patient enrolment began in September 2000 for SOHO and in November 2000 for IC-SOHO; the last participant was enrolled in December 2001. The main objective of the study was to compare the outcomes of participants starting olanzapine with other antipsychotics. Participants were enrolled in two groups of similar size: one included those starting olanzapine, and the other included those starting any other antipsychotic. This deliberate oversampling of people taking olanzapine was done to facilitate comparisons between the two groups, as per the primary objective. Importantly, the antipsychotic treatment prescribed to each person was wholly based on the opinion of the treating psychiatrist; individuals were asked to participate in the study after they had received their medication prescription. The enrolment period was intentionally long to avoid interfering with standard medical practice and no minimum number of participants was required per participating psychiatrist.
Measures
All assessment tools were chosen for simplicity and ease of use, bearing in mind the observational nature of the study, cross-cultural relevance and practical needs such as translation into different languages. The Clinical Global Impressions – Schizophrenia (CGI-SCH) scale Reference Haro, Kamath, Ochoa, Novick, Rele and Fargas26 was used to assess symptom severity across positive, negative, depressive and cognitive subdomains in addition to overall symptoms from 1 (normal, not at all ill) to 7 (among the most severely ill). A detailed patient history was taken at baseline, capturing clinical information (including duration of illness, current and past medications, reasons for treatment initiation or change, CGI-SCH score, adverse events) in addition to key sociodemographic, functional and health service use data such as age, alcohol and substance misuse/dependency, housing and employment status, suicidality, hostility (has the patient exhibited verbal or physical hostility/aggression in the past 6 months?) and previous hospital admissions and out-patient clinic visits. This information was obtained from all available sources (direct patient and family interview, clinical chart). The location and type of the principal practice of participating investigators was also collected.
Statistical analysis
Only participants with at most one missing visit (except the final one) were included in the analysis. For participants with one missing visit, values from the previous visit were carried forward and used to impute the values of the missing visit. Results from the 3-month visit were not used in the analysis unless data from the 6-month visit were missing; in such cases, data from the 3-month visit were used in the imputation.
The 37 countries participating in the study were grouped into 6 regions as follows: North Europe (France, Germany, UK, The Netherlands, Ireland, Denmark); South Europe (Spain, Italy, Portugal, Greece, Israel (Israel has been included in the South Europe group based on ethnicity, economic and healthcare systems)); Central and Eastern Europe (Czech Republic, Hungary, Lithuania, Poland, Romania, Russia, Slovakia, Slovenia); Latin America (Argentina, Chile, Colombia, Costa Rica, El Salvador, Guatemala, Honduras, Mexico, Peru, Puerto Rico, Venezuela); North Africa and Middle East (Algeria, Egypt, Saudi Arabia, Turkey); and East Asia (Korea, Malaysia, Taiwan).
Approximately a third of the participants (36.3%) were lost to follow-up before the end of the study at 3 years and were not included in the analysis. The percentage varied across regions. The highest attrition rate was in East Asia (62.8%), followed by Africa and Middle East (47.7%), Latin America (41.7%), North Europe (37.5%), South Europe (28.2%) and Central and Eastern Europe (26.9%). There were small differences in participant characteristics between those included and not included in the analyses, both overall and by region. All statistical analyses were done using SAS version 9.1 for Windows.
Definition of remission
Clinical remission was defined as achieving CGI-SCH overall, positive, negative and cognitive symptom scores lower than or equal to 3 on the scale from 1 to 7 for 6 months (i.e. for two consecutive visits) plus no in-patient admission during the same period. As two consecutive visits were considered this meant clinical remission could not occur before the 12-month visit. This definition of clinical remission was based on the Andreasen criteria as presented and validated in previous reports of the SOHO study. Reference Haro, Kamath, Ochoa, Novick, Rele and Fargas26,Reference Haro, Ochoa, Gervin, Mavreas and Jones27
Functional remission was defined as having good social functioning for a period of 6 months (two consecutive visits). Good social functioning included those participants who had: (a) a positive occupational/vocational status, i.e. paid or unpaid full- or part-time employment, being an active student in university or housewife; (b) independent living; and (c) active social interactions, i.e. having more than one social contact during the past 4 weeks or having a spouse or partner. Functional remission was also defined from the 12-month visit.
Descriptive analysis
Baseline characteristics were described overall and for each of the six regions for those participants with no more than one missing visit (n = 11 078). In addition, the baseline characteristics of participants who did and did not achieve clinical remission and functional remission at some point during the 3-year follow-up were summarised using descriptive statistics. Differences between the groups who did and did not achieve remission were compared using chi-squared or Fisher’s exact tests for categorical data and Wilcoxon or Mann–Whitney tests for numerical variables. For all comparisons, the level of significance was 0.05. The baseline sociodemographic and clinical variables compared included: number of participants, gender, age, previously untreated, age at first treatment for schizophrenia, duration of illness (years since first treatment for schizophrenia), alcohol dependency, substance misuse, suicide attempts, overall CGI-SCH, positive CGI-SCH, negative CGI-SCH, depressive CGI-SCH, cognitive CGI-SCH, hostility, adherence, body mass index, marital status, living independently, having paid employment and being socially active.
Regression model
Logistic regression models were used to identify variables independently associated with clinical remission and those associated with functional remission for the overall W-SOHO sample. Stepwise model reduction was conducted by dropping from the model any non-significant variables. Data from the logistic regression models are presented as odds ratios (OR), 95% confidence intervals and P-values. The CGI was treated as a continuous variable in the models. The odds ratios in this case and other continuous variables estimate the change in the response variable by point of change in variable. The logistic regression models were repeated by region, including all significant covariates in any of the regions.
Results
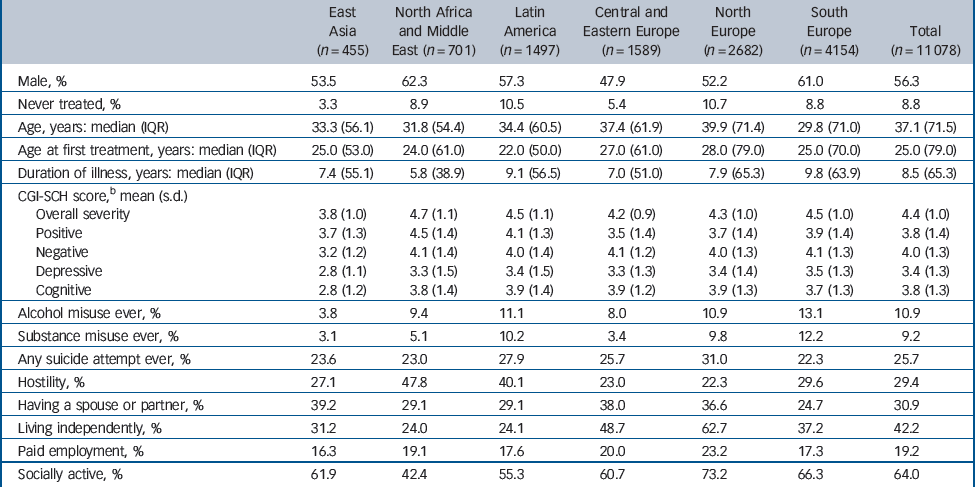
The overall W-SOHO sample analysed included 11 078 participants with at most one missing visit. The number of participants in each of the six regions was: South Europe (n = 4154); North Europe (n = 2682); Central and Eastern Europe (n = 1589); Latin America (n = 1497); North Africa and Middle East (n = 701); and East Asia (n = 455). Table 1 summarises the baseline characteristics of the overall W-SOHO sample and of participants in each of the six regions.
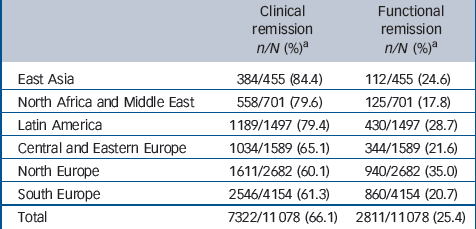
Of the 11 078 participants analysed, 7322 (66.1%) achieved clinical remission during the 3-year follow-up, whereas only 2811 (25.4%) achieved functional remission during follow-up. Table 2 summarises the frequency of clinical and functional remission for each of the six regions. The frequency of clinical
Table 1 Baseline characteristics of the Worldwide Schizophrenia Outpatient Health Outcomes (W-SOHO) sample (n = 11 078) and participants in each of the six regionsa
| East Asia (n = 455) | North Africa and Middle East (n = 701) | Latin America (n = 1497) | Central and Eastern Europe (n = 1589) | North Europe (n = 2682) | South Europe (n = 4154) | Total (n = 11 078) | |
|---|---|---|---|---|---|---|---|
| Male, % | 53.5 | 62.3 | 57.3 | 47.9 | 52.2 | 61.0 | 56.3 |
| Never treated, % | 3.3 | 8.9 | 10.5 | 5.4 | 10.7 | 8.8 | 8.8 |
| Age, years: median (IQR) | 33.3 (56.1) | 31.8 (54.4) | 34.4 (60.5) | 37.4 (61.9) | 39.9 (71.4) | 29.8 (71.0) | 37.1 (71.5) |
| Age at first treatment, years: median (IQR) | 25.0 (53.0) | 24.0 (61.0) | 22.0 (50.0) | 27.0 (61.0) | 28.0 (79.0) | 25.0 (70.0) | 25.0 (79.0) |
| Duration of illness, years: median (IQR) | 7.4 (55.1) | 5.8 (38.9) | 9.1 (56.5) | 7.0 (51.0) | 7.9 (65.3) | 9.8 (63.9) | 8.5 (65.3) |
| CGI-SCH score,b mean (s.d.) | |||||||
| Overall severity | 3.8 (1.0) | 4.7 (1.1) | 4.5 (1.1) | 4.2 (0.9) | 4.3 (1.0) | 4.5 (1.0) | 4.4 (1.0) |
| Positive | 3.7 (1.3) | 4.5 (1.4) | 4.1 (1.3) | 3.5 (1.4) | 3.7 (1.4) | 3.9 (1.4) | 3.8 (1.4) |
| Negative | 3.2 (1.2) | 4.1 (1.4) | 4.0 (1.4) | 4.1 (1.2) | 4.0 (1.3) | 4.1 (1.3) | 4.0 (1.3) |
| Depressive | 2.8 (1.1) | 3.3 (1.5) | 3.4 (1.5) | 3.3 (1.3) | 3.4 (1.4) | 3.5 (1.3) | 3.4 (1.3) |
| Cognitive | 2.8 (1.2) | 3.8 (1.4) | 3.9 (1.4) | 3.9 (1.2) | 3.9 (1.3) | 3.7 (1.3) | 3.8 (1.3) |
| Alcohol misuse ever, % | 3.8 | 9.4 | 11.1 | 8.0 | 10.9 | 13.1 | 10.9 |
| Substance misuse ever, % | 3.1 | 5.1 | 10.2 | 3.4 | 9.8 | 12.2 | 9.2 |
| Any suicide attempt ever, % | 23.6 | 23.0 | 27.9 | 25.7 | 31.0 | 22.3 | 25.7 |
| Hostility, % | 27.1 | 47.8 | 40.1 | 23.0 | 22.3 | 29.6 | 29.4 |
| Having a spouse or partner, % | 39.2 | 29.1 | 29.1 | 38.0 | 36.6 | 24.7 | 30.9 |
| Living independently, % | 31.2 | 24.0 | 24.1 | 48.7 | 62.7 | 37.2 | 42.2 |
| Paid employment, % | 16.3 | 19.1 | 17.6 | 20.0 | 23.2 | 17.3 | 19.2 |
| Socially active, % | 61.9 | 42.4 | 55.3 | 60.7 | 73.2 | 66.3 | 64.0 |
a Total n varies for each variable because of missing data. Total n and numbers by categories are available from the authors on request. For variables given as percentages, the percentages refer to the total n available for that variable.
b CGI-SCH, Clinical Global Impression – Schizophrenia scale (ranges from 1, normal (not at all ill) to 7, among the most severely ill).
remission ranged from 60.1% in North Europe to 84.4% in East Asia, and the frequency of functional remission ranged from 17.8% in North Africa and Middle East to 35.0% in North Europe.
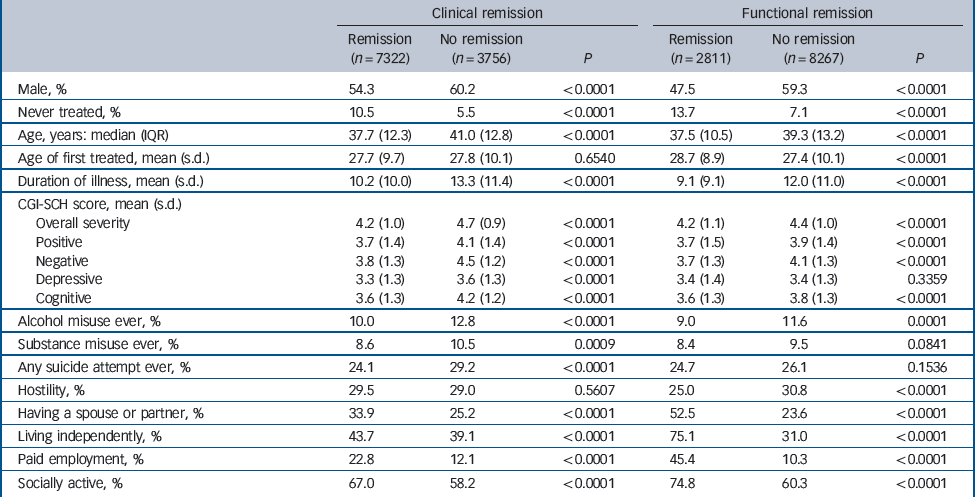
Compared with participants who did not achieve clinical remission, those who achieved clinical remission in the overall sample were more frequently women, younger, had a shorter duration of illness, previously untreated, had less alcohol and substance misuse in the past, fewer suicide attempts in the past, had a good level of social functioning at baseline (more frequently working for pay, having a spouse or partner, living independently and being socially active) and lower symptoms at baseline (Table 3). Similarly, comparisons between participants who did and did not achieve functional remission (Table 3) showed that those achieving functional remission also had an older age at first contact and displayed less hostility at baseline, but had no difference in depressive symptoms at baseline or a history of substance misuse and suicide attempts.
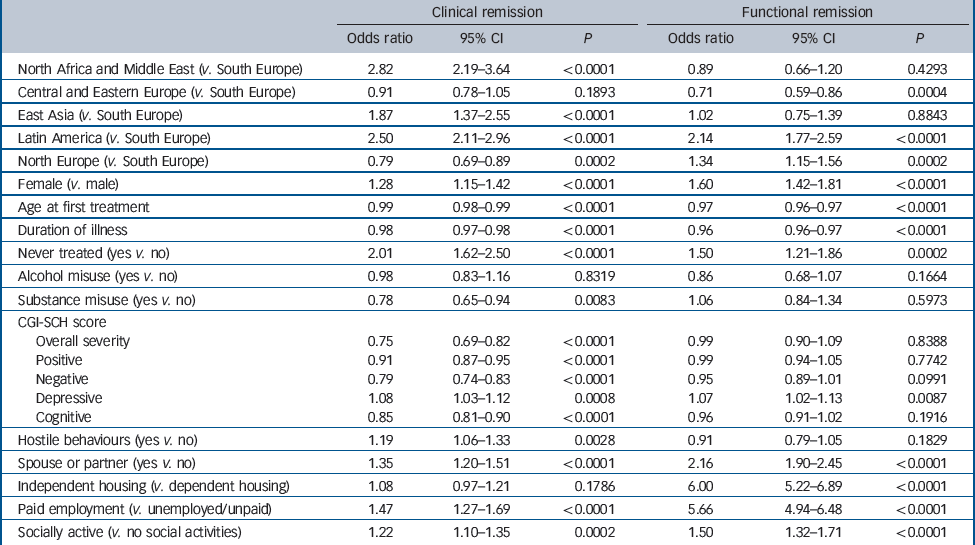
Logistic regression analysis of factors independently associated with achieving clinical remission at some point during the 3-year follow-up for the overall sample (Table 4) showed that region was one of the most important predictors of clinical remission: compared with South Europe, individuals in the regions of North Africa and Middle East, Latin America and East Asia were significantly more likely to achieve clinical remission. Other baseline factors significantly associated with an increased likelihood of clinical remission were: being female, first treatment for schizophrenia ever, having good social functioning at baseline (paid employment, spouse/partner, being socially active), displaying hostile behaviour and having higher depressive symptoms at baseline. In contrast, older age at first treatment, a longer duration of illness, history of substance misuse and higher clinical severity at baseline (overall severity, positive, negative and cognitive symptoms) were associated with a lower likelihood of achieving clinical remission.
Table 2 Remission rates for the W-SOHO sample (n = 11 078) and for each of the six regions
| Clinical remission n/N (%)a | Functional remission n/N (%)a | |
|---|---|---|
| East Asia | 384/455 (84.4) | 112/455 (24.6) |
| North Africa and Middle East | 558/701 (79.6) | 125/701 (17.8) |
| Latin America | 1189/1497 (79.4) | 430/1497 (28.7) |
| Central and Eastern Europe | 1034/1589 (65.1) | 344/1589 (21.6) |
| North Europe | 1611/2682 (60.1) | 940/2682 (35.0) |
| South Europe | 2546/4154 (61.3) | 860/4154 (20.7) |
| Total | 7322/11 078 (66.1) | 2811/11 078 (25.4) |
a Differences among regions P < 0.001.
Logistic regression showed that region was also an important predictor of achieving functional remission (Table 4): compared with participants in South Europe, those in Latin America and North Europe were significantly more likely to achieve functional remission, whereas individuals in Central and Eastern Europe were significantly less likely to achieve functional remission. Baseline social functioning (independent housing, paid employment, spouse/partner and being socially active) was another important predictor of functional remission, together with being female, never treated for schizophrenia before study entry and a higher depressive symptom score at baseline. Older age at first treatment and a longer duration of illness were significantly associated with less likelihood of functional remission. The magnitude of the effect of independent housing and having paid employment at baseline on functional remission was particularly large (odds ratio around 6).
Table 5 summarises the baseline factors independently associated with achieving clinical remission and Table 6 those for achieving functional remission for each of the six regions.
Table 3 Baseline characteristics of participants achieving and not achieving clinical or functional remission in the W-SOHO sample (n = 11 078)
| Clinical remission | Functional remission | |||||
|---|---|---|---|---|---|---|
| Remission (n = 7322) | No remission (n = 3756) | P | Remission (n = 2811) | No remission (n = 8267) | P | |
| Male, % | 54.3 | 60.2 | < 0.0001 | 47.5 | 59.3 | < 0.0001 |
| Never treated, % | 10.5 | 5.5 | < 0.0001 | 13.7 | 7.1 | < 0.0001 |
| Age, years: median (IQR) | 37.7 (12.3) | 41.0 (12.8) | < 0.0001 | 37.5 (10.5) | 39.3 (13.2) | < 0.0001 |
| Age of first treated, mean (s.d.) | 27.7 (9.7) | 27.8 (10.1) | 0.6540 | 28.7 (8.9) | 27.4 (10.1) | < 0.0001 |
| Duration of illness, mean (s.d.) | 10.2 (10.0) | 13.3 (11.4) | < 0.0001 | 9.1 (9.1) | 12.0 (11.0) | < 0.0001 |
| CGI-SCH score, mean (s.d.) | ||||||
| Overall severity | 4.2 (1.0) | 4.7 (0.9) | < 0.0001 | 4.2 (1.1) | 4.4 (1.0) | < 0.0001 |
| Positive | 3.7 (1.4) | 4.1 (1.4) | < 0.0001 | 3.7 (1.5) | 3.9 (1.4) | < 0.0001 |
| Negative | 3.8 (1.3) | 4.5 (1.2) | < 0.0001 | 3.7 (1.3) | 4.1 (1.3) | < 0.0001 |
| Depressive | 3.3 (1.3) | 3.6 (1.3) | < 0.0001 | 3.4 (1.4) | 3.4 (1.3) | 0.3359 |
| Cognitive | 3.6 (1.3) | 4.2 (1.2) | < 0.0001 | 3.6 (1.3) | 3.8 (1.3) | < 0.0001 |
| Alcohol misuse ever, % | 10.0 | 12.8 | < 0.0001 | 9.0 | 11.6 | 0.0001 |
| Substance misuse ever, % | 8.6 | 10.5 | 0.0009 | 8.4 | 9.5 | 0.0841 |
| Any suicide attempt ever, % | 24.1 | 29.2 | < 0.0001 | 24.7 | 26.1 | 0.1536 |
| Hostility, % | 29.5 | 29.0 | 0.5607 | 25.0 | 30.8 | < 0.0001 |
| Having a spouse or partner, % | 33.9 | 25.2 | < 0.0001 | 52.5 | 23.6 | < 0.0001 |
| Living independently, % | 43.7 | 39.1 | < 0.0001 | 75.1 | 31.0 | < 0.0001 |
| Paid employment, % | 22.8 | 12.1 | < 0.0001 | 45.4 | 10.3 | < 0.0001 |
| Socially active, % | 67.0 | 58.2 | < 0.0001 | 74.8 | 60.3 | < 0.0001 |
CGI-SCH, Clinical Global Impression – Schizophrenia scale.
Being previously untreated was generally associated with a greater chance of clinical remission across all regions, whereas a higher negative symptoms score was associated with less chance of clinical remission. The strongest predictors of an increased odds of functional remission across all or nearly all regions were the social functioning variables (being in paid employment, living in independent housing or being socially active). Being female, previously treated, and having a spouse/partner was associated with a greater chance of functional remission in some regions, whereas an older age at first treatment and a longer duration of illness were associated with less chance of remission in all three European regions and Latin America.
Discussion
Study limitations
The W-SOHO study is the largest prospective observational study on the outcome of schizophrenia in an out-patient setting. However, there are several limitations that must be considered when discussing the results. First, although the 37 countries participating in the W-SOHO study belong to 6 regions of the world with different economic and cultural characteristics, the countries are not necessarily representative of these regions and some regions, such as East Asia, had a relatively small number of participants. In addition, the centres or investigators participating in the study in each country may not be representative of the whole country. Second, although sociodemographic and clinical characteristics were assessed in individuals participating and were taken into account in the analyses, we cannot rule out that different types of individuals with schizophrenia were enrolled in different countries, that there were other confounding variables not recorded in the study and that service contexts and residual confounding may be influencing the results. Third, we did not collect detailed information on the cultural environment of the participants, which could have influenced outcomes, and limits the exploration of the reasons for the regional differences. Fourth,
Table 4 Baseline factors associated with achieving clinical and functional remission during the 3-year follow-up for the W-SOHO sample (n = 11 078)a
| Clinical remission | Functional remission | |||||
|---|---|---|---|---|---|---|
| Odds ratio | 95% CI | P | Odds ratio | 95% CI | P | |
| North Africa and Middle East (v. South Europe) | 2.82 | 2.19–3.64 | < 0.0001 | 0.89 | 0.66–1.20 | 0.4293 |
| Central and Eastern Europe (v. South Europe) | 0.91 | 0.78–1.05 | 0.1893 | 0.71 | 0.59–0.86 | 0.0004 |
| East Asia (v. South Europe) | 1.87 | 1.37–2.55 | < 0.0001 | 1.02 | 0.75–1.39 | 0.8843 |
| Latin America (v. South Europe) | 2.50 | 2.11–2.96 | < 0.0001 | 2.14 | 1.77–2.59 | < 0.0001 |
| North Europe (v. South Europe) | 0.79 | 0.69–0.89 | 0.0002 | 1.34 | 1.15–1.56 | 0.0002 |
| Female (v. male) | 1.28 | 1.15–1.42 | < 0.0001 | 1.60 | 1.42–1.81 | < 0.0001 |
| Age at first treatment | 0.99 | 0.98–0.99 | < 0.0001 | 0.97 | 0.96–0.97 | < 0.0001 |
| Duration of illness | 0.98 | 0.97–0.98 | < 0.0001 | 0.96 | 0.96–0.97 | < 0.0001 |
| Never treated (yes v. no) | 2.01 | 1.62–2.50 | < 0.0001 | 1.50 | 1.21–1.86 | 0.0002 |
| Alcohol misuse (yes v. no) | 0.98 | 0.83–1.16 | 0.8319 | 0.86 | 0.68–1.07 | 0.1664 |
| Substance misuse (yes v. no) | 0.78 | 0.65–0.94 | 0.0083 | 1.06 | 0.84–1.34 | 0.5973 |
| CGI-SCH score | ||||||
| Overall severity | 0.75 | 0.69–0.82 | < 0.0001 | 0.99 | 0.90–1.09 | 0.8388 |
| Positive | 0.91 | 0.87–0.95 | < 0.0001 | 0.99 | 0.94–1.05 | 0.7742 |
| Negative | 0.79 | 0.74–0.83 | < 0.0001 | 0.95 | 0.89–1.01 | 0.0991 |
| Depressive | 1.08 | 1.03–1.12 | 0.0008 | 1.07 | 1.02–1.13 | 0.0087 |
| Cognitive | 0.85 | 0.81–0.90 | < 0.0001 | 0.96 | 0.91–1.02 | 0.1916 |
| Hostile behaviours (yes v. no) | 1.19 | 1.06–1.33 | 0.0028 | 0.91 | 0.79–1.05 | 0.1829 |
| Spouse or partner (yes v. no) | 1.35 | 1.20–1.51 | < 0.0001 | 2.16 | 1.90–2.45 | < 0.0001 |
| Independent housing (v. dependent housing) | 1.08 | 0.97–1.21 | 0.1786 | 6.00 | 5.22–6.89 | < 0.0001 |
| Paid employment (v. unemployed/unpaid) | 1.47 | 1.27–1.69 | < 0.0001 | 5.66 | 4.94–6.48 | < 0.0001 |
| Socially active (v. no social activities) | 1.22 | 1.10–1.35 | 0.0002 | 1.50 | 1.32–1.71 | < 0.0001 |
CGI-SCH, Clinical Global Impression – Schizophrenia scale.
Values are odds ratios (OR) obtained from the logistic regression model. An OR <1 indicates a lower likelihood of achieving remission.
Table 5 Baseline factors associated with achieving clinical remission during the 3-year follow-up for each of the six regionsa
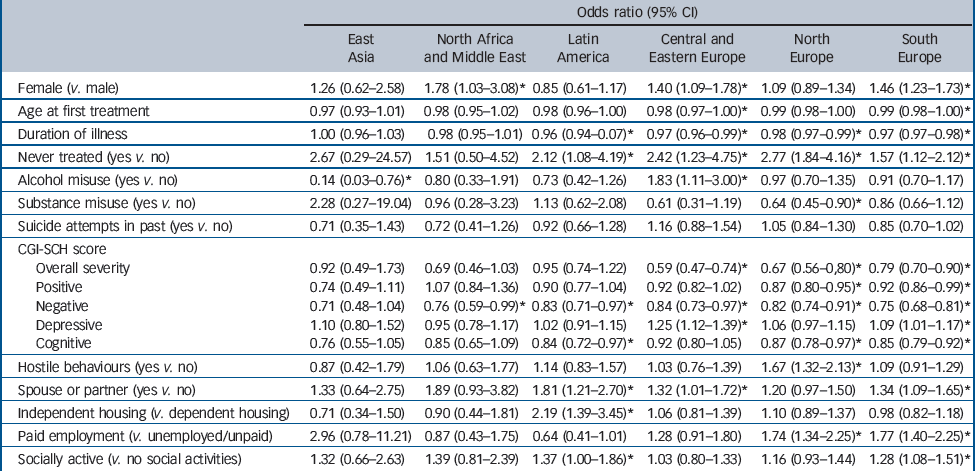
| Odds ratio (95% CI) | ||||||
|---|---|---|---|---|---|---|
| East Asia | North Africa and Middle East | Latin America | Central and Eastern Europe | North Europe | South Europe | |
| Female (v. male) | 1.26 (0.62–2.58) | 1.78 (1.03–3.08)* | 0.85 (0.61–1.17) | 1.40 (1.09–1.78)* | 1.09 (0.89–1.34) | 1.46 (1.23–1.73)* |
| Age at first treatment | 0.97 (0.93–1.01) | 0.98 (0.95–1.02) | 0.98 (0.96–1.00) | 0.98 (0.97–1.00)* | 0.99 (0.98–1.00) | 0.99 (0.98–1.00)* |
| Duration of illness | 1.00 (0.96–1.03) | 0.98 (0.95–1.01) | 0.96 (0.94–0.07)* | 0.97 (0.96–0.99)* | 0.98 (0.97–0.99)* | 0.97 (0.97–0.98)* |
| Never treated (yes v. no) | 2.67 (0.29–24.57) | 1.51 (0.50–4.52) | 2.12 (1.08–4.19)* | 2.42 (1.23–4.75)* | 2.77 (1.84–4.16)* | 1.57 (1.12–2.12)* |
| Alcohol misuse (yes v. no) | 0.14 (0.03–0.76)* | 0.80 (0.33–1.91) | 0.73 (0.42–1.26) | 1.83 (1.11–3.00)* | 0.97 (0.70–1.35) | 0.91 (0.70–1.17) |
| Substance misuse (yes v. no) | 2.28 (0.27–19.04) | 0.96 (0.28–3.23) | 1.13 (0.62–2.08) | 0.61 (0.31–1.19) | 0.64 (0.45–0.90)* | 0.86 (0.66–1.12) |
| Suicide attempts in past (yes v. no) | 0.71 (0.35–1.43) | 0.72 (0.41–1.26) | 0.92 (0.66–1.28) | 1.16 (0.88–1.54) | 1.05 (0.84–1.30) | 0.85 (0.70–1.02) |
| CGI-SCH score | ||||||
| Overall severity | 0.92 (0.49–1.73) | 0.69 (0.46–1.03) | 0.95 (0.74–1.22) | 0.59 (0.47–0.74)* | 0.67 (0.56–0,80)* | 0.79 (0.70–0.90)* |
| Positive | 0.74 (0.49–1.11) | 1.07 (0.84–1.36) | 0.90 (0.77–1.04) | 0.92 (0.82–1.02) | 0.87 (0.80–0.95)* | 0.92 (0.86–0.99)* |
| Negative | 0.71 (0.48–1.04) | 0.76 (0.59–0.99)* | 0.83 (0.71–0.97)* | 0.84 (0.73–0.97)* | 0.82 (0.74–0.91)* | 0.75 (0.68–0.81)* |
| Depressive | 1.10 (0.80–1.52) | 0.95 (0.78–1.17) | 1.02 (0.91–1.15) | 1.25 (1.12–1.39)* | 1.06 (0.97–1.15) | 1.09 (1.01–1.17)* |
| Cognitive | 0.76 (0.55–1.05) | 0.85 (0.65–1.09) | 0.84 (0.72–0.97)* | 0.92 (0.80–1.05) | 0.87 (0.78–0.97)* | 0.85 (0.79–0.92)* |
| Hostile behaviours (yes v. no) | 0.87 (0.42–1.79) | 1.06 (0.63–1.77) | 1.14 (0.83–1.57) | 1.03 (0.76–1.39) | 1.67 (1.32–2.13)* | 1.09 (0.91–1.29) |
| Spouse or partner (yes v. no) | 1.33 (0.64–2.75) | 1.89 (0.93–3.82) | 1.81 (1.21–2.70)* | 1.32 (1.01–1.72)* | 1.20 (0.97–1.50) | 1.34 (1.09–1.65)* |
| Independent housing (v. dependent housing) | 0.71 (0.34–1.50) | 0.90 (0.44–1.81) | 2.19 (1.39–3.45)* | 1.06 (0.81–1.39) | 1.10 (0.89–1.37) | 0.98 (0.82–1.18) |
| Paid employment (v. unemployed/unpaid) | 2.96 (0.78–11.21) | 0.87 (0.43–1.75) | 0.64 (0.41–1.01) | 1.28 (0.91–1.80) | 1.74 (1.34–2.25)* | 1.77 (1.40–2.25)* |
| Socially active (v. no social activities) | 1.32 (0.66–2.63) | 1.39 (0.81–2.39) | 1.37 (1.00–1.86)* | 1.03 (0.80–1.33) | 1.16 (0.93–1.44) | 1.28 (1.08–1.51)* |
CGI-SCH, Clinical Global Impression – Schizophrenia scale.
a Values are odds ratios (OR) obtained from the logistic regression model. An OR <1 indicates a lower likelihood of achieving remission.
* P < 0.05.
data were collected at 6-month intervals and limited information was gathered between assessment visits. Fifth, data were only collected over 3 years and, therefore, are unlikely to represent the full course of schizophrenia: some individuals may have experienced remission at a later time. Sixth, given the limitations of the ascertainment tools, our methods do not allow us to separate the effects of regional clinical practices (and therefore their ratings on the CGI-SCH) of the participating psychiatrists from the predictors of outcome analysed. Seventh, interrater reliability was not assessed given the large number of participating investigators. However, measures were chosen based on clarity and ease of use. Eighth, participants included in the analysis are those
Table 6 Baseline factors associated with achieving functional remission during the 3-year follow-up for each of the six regions
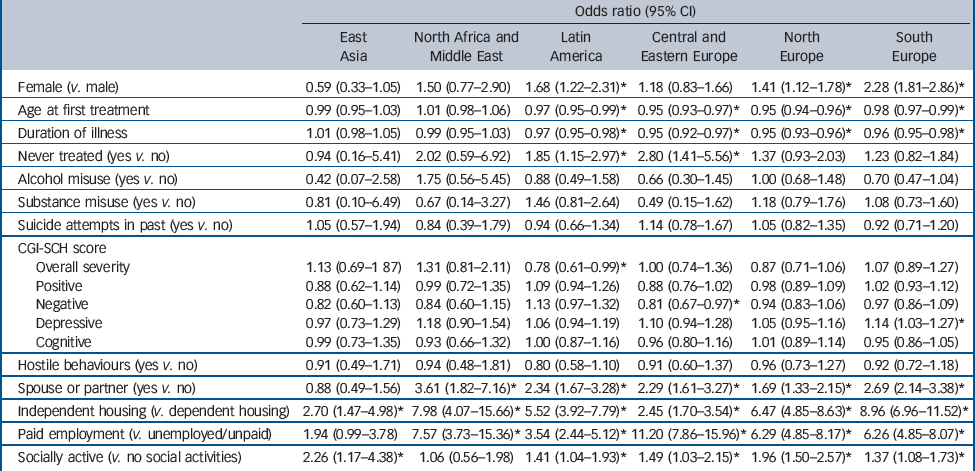
| Odds ratio (95% CI) | ||||||
|---|---|---|---|---|---|---|
| East Asia | North Africa and Middle East | Latin America | Central and Eastern Europe | North Europe | South Europe | |
| Female (v. male) | 0.59 (0.33–1.05) | 1.50 (0.77–2.90) | 1.68 (1.22–2.31)* | 1.18 (0.83–1.66) | 1.41 (1.12–1.78)* | 2.28 (1.81–2.86)* |
| Age at first treatment | 0.99 (0.95–1.03) | 1.01 (0.98–1.06) | 0.97 (0.95–0.99)* | 0.95 (0.93–0.97)* | 0.95 (0.94–0.96)* | 0.98 (0.97–0.99)* |
| Duration of illness | 1.01 (0.98–1.05) | 0.99 (0.95–1.03) | 0.97 (0.95–0.98)* | 0.95 (0.92–0.97)* | 0.95 (0.93–0.96)* | 0.96 (0.95–0.98)* |
| Never treated (yes v. no) | 0.94 (0.16–5.41) | 2.02 (0.59–6.92) | 1.85 (1.15–2.97)* | 2.80 (1.41–5.56)* | 1.37 (0.93–2.03) | 1.23 (0.82–1.84) |
| Alcohol misuse (yes v. no) | 0.42 (0.07–2.58) | 1.75 (0.56–5.45) | 0.88 (0.49–1.58) | 0.66 (0.30–1.45) | 1.00 (0.68–1.48) | 0.70 (0.47–1.04) |
| Substance misuse (yes v. no) | 0.81 (0.10–6.49) | 0.67 (0.14–3.27) | 1.46 (0.81–2.64) | 0.49 (0.15–1.62) | 1.18 (0.79–1.76) | 1.08 (0.73–1.60) |
| Suicide attempts in past (yes v. no) | 1.05 (0.57–1.94) | 0.84 (0.39–1.79) | 0.94 (0.66–1.34) | 1.14 (0.78–1.67) | 1.05 (0.82–1.35) | 0.92 (0.71–1.20) |
| CGI-SCH score | ||||||
| Overall severity | 1.13 (0.69–1 87) | 1.31 (0.81–2.11) | 0.78 (0.61–0.99)* | 1.00 (0.74–1.36) | 0.87 (0.71–1.06) | 1.07 (0.89–1.27) |
| Positive | 0.88 (0.62–1.14) | 0.99 (0.72–1.35) | 1.09 (0.94–1.26) | 0.88 (0.76–1.02) | 0.98 (0.89–1.09) | 1.02 (0.93–1.12) |
| Negative | 0.82 (0.60–1.13) | 0.84 (0.60–1.15) | 1.13 (0.97–1.32) | 0.81 (0.67–0.97)* | 0.94 (0.83–1.06) | 0.97 (0.86–1.09) |
| Depressive | 0.97 (0.73–1.29) | 1.18 (0.90–1.54) | 1.06 (0.94–1.19) | 1.10 (0.94–1.28) | 1.05 (0.95–1.16) | 1.14 (1.03–1.27)* |
| Cognitive | 0.99 (0.73–1.35) | 0.93 (0.66–1.32) | 1.00 (0.87–1.16) | 0.96 (0.80–1.16) | 1.01 (0.89–1.14) | 0.95 (0.86–1.05) |
| Hostile behaviours (yes v. no) | 0.91 (0.49–1.71) | 0.94 (0.48–1.81) | 0.80 (0.58–1.10) | 0.91 (0.60–1.37) | 0.96 (0.73–1.27) | 0.92 (0.72–1.18) |
| Spouse or partner (yes v. no) | 0.88 (0.49–1.56) | 3.61 (1.82–7.16)* | 2.34 (1.67–3.28)* | 2.29 (1.61–3.27)* | 1.69 (1.33–2.15)* | 2.69 (2.14–3.38)* |
| Independent housing (v. dependent housing) | 2.70 (1.47–4.98)* | 7.98 (4.07–15.66)* | 5.52 (3.92–7.79)* | 2.45 (1.70–3.54)* | 6.47 (4.85–8.63)* | 8.96 (6.96–11.52)* |
| Paid employment (v. unemployed/unpaid) | 1.94 (0.99–3.78) | 7.57 (3.73–15.36)* | 3.54 (2.44–5.12)* | 11.20 (7.86–15.96)* | 6.29 (4.85–8.17)* | 6.26 (4.85–8.07)* |
| Socially active (v. no social activities) | 2.26 (1.17–4.38)* | 1.06 (0.56–1.98) | 1.41 (1.04–1.93)* | 1.49 (1.03–2.15)* | 1.96 (1.50–2.57)* | 1.37 (1.08–1.73)* |
CGI-SCH, Clinical Global Impression – Schizophrenia scale.
a. Values are odds ratios (OR) obtained from the logistic regression model. An OR < 1 indicates a lower likelihood of achieving remission.
* P < 0.05.
requiring a treatment change in routine clinical practice, which allowed us to study treatment outcomes but are obviously not representative of the overall patient population. Ninth, attrition was highest in the regions with the highest remission rates, which could explain some of the findings if attrition was higher in individuals with severe schizophrenia. Finally, our definition of clinical remission required a low level of symptoms for at least 6 months, consistent with the definition proposed by Andreasen. Reference Andreasen, Carpenter, Kane, Lasser, Marder and Weinberger28 However, our definition of remission was based on the CGI-SCH, which is a valid but less specific measure of clinical severity than other scales such as the Positive and Negative Syndrome Scale (PANSS). Reference Kay, Fiszbein and Opler29 Previous analyses have shown a good agreement between this and Andreasen’s definition. Reference Haro, Ochoa, Gervin, Mavreas and Jones27
Regional differences in outcomes
With these limitations in mind, the results of the W-SOHO study show that the clinical outcomes of schizophrenia seem to be worse in Europe compared with other regions. Remarkably, the regional differences were different for functional remission. The frequency of clinical remission was lower in the three European regions (60–65%) than in East Asia, Latin America, and North Africa and Middle East (79–84%). Participants living in the latter three regions had a much greater likelihood of achieving clinical remission than those living in South Europe. Moreover, the variations in clinical remission rates between regions were not accounted for by differences in baseline clinical and sociodemographic characteristics evaluated in the study. Economic development, cultural factors such as family support or other country characteristics may explain the differences. Differences in economic development are not necessarily translated to differences in the course of schizophrenia. For example, South Europe and Central and Eastern Europe show similar clinical remission rates but have different levels of economic development. Our findings support the earlier WHO studies reporting differences in outcomes between regions. 1–Reference Hopper and Wanderling6
However, regional differences in functional remission followed a different pattern. Although it was more likely for individuals in Latin America to achieve functional remission compared with South Europe, there were no clear differences with East Asia or North Africa and Middle East. A new pattern emerged when compared with Central and Eastern Europe and North Europe; Central and Eastern Europe seemed to have a lower functional remission rate compared with South Europe, whereas North Europe tended to have a higher functional remission rate.
When comparing the descriptive and regression differences between the regions, we wanted to highlight that the logistic model showed that individuals with schizophrenia in Central and Eastern Europe were significantly less likely to achieve functional remission than those in South Europe. However, this was not detected in the descriptive analysis, probably due to the fact that some social functioning variables (independent housing and having a spouse/partner) are confounding variables.
Although this is somewhat speculative, differences in remission rates seem to be the result of economic, cultural and environmental factors more than differences in schizophrenic disorder. The same diagnostic criteria were applied in all regions and similarities in predictors of outcome were seen across the regions, which may indicate similar characteristics of the disorder. The reasons for the better clinical outcome in low- and middle-income countries are unknown but may be related to differences in the balance between treatment and vulnerability experienced by the individuals. Reference Nuechterlein and Dawson30 Differences in functional remission between regions were mostly driven by differences in independent living and paid employment. Thus, these differences in functional remission rates may be influenced by differences in access to accommodation, the presence of rehabilitation services and social benefits, the development of specific policies for individuals with severe mental disorders and the level of societal stigma about mental illness.
Our results indicate that there are several other baseline predictors of outcome. We found that women were more likely to achieve remission compared with men. This is consistent with many reports that women with schizophrenia experience better outcomes than men. Reference Grossman, Harrow, Rosen and Faull31,Reference Usall, Ochoa, Araya and Marquez32 Younger age, shorter duration of illness and no previous treatment for schizophrenia were also associated with a better chance of achieving remission, whereas substance misuse was associated with a lower chance of clinical remission, especially in North Europe. Our findings are consistent with systematic reviews and meta-analyses, which found that a shorter duration of untreated psychosis is associated with better symptomatic and functional outcomes in high-income and low- and middle-income countries. Reference Marshall, Lewis, Lockwood, Drake, Jones and Croudace33,Reference Farooq, Large, Nielssen and Waheed34 Although it has been reported that comorbid substance misuse is highly prevalent in schizophrenia and associated with poorer clinical outcomes, Reference Volkow35 most of the evidence is based on studies in Western countries; the prevalence and impact of substance use disorders among people with schizophrenia in low- and middle-income countries has not been well studied. The frequency of alcohol or substance misuse was low in the overall W-SOHO population at baseline compared with other samples, Reference Buhler, Hambrecht, Loffler, an der Heiden and Hafner36 and its role as an independent predictor of remission varied across regions. Further work on substance misuse as a factor influencing outcome of schizophrenia across a wide range of countries is needed.
Higher symptom severity at baseline in terms of positive, negative, cognitive and overall symptoms was associated with less likelihood of clinical remission, but the severity of these symptoms was not significantly associated with functional remission. However, a higher level of depressive symptoms at baseline was associated with a higher likelihood of achieving both clinical and functional remission in the logistic regression analyses of the overall W-SOHO population. This supports previous findings that high levels of depressive symptoms at baseline predict favourable short-term outcomes in individuals with schizophrenia. Reference Oosthuizen, Emsley, Roberts, Turner, Keyter and Keyter37 However, other researchers have found that people with depressive symptoms have poorer long-term functional outcomes. Reference Conley, Ascher-Svanum, Zhu, Faries and Kinon38
Social functioning variables were important prognostic factors for remission in all regions. Participants with a spouse/partner, in paid employment and who were socially active at baseline were more likely to achieve clinical and functional remission, supporting previous findings that better baseline social functioning is associated with recovery (when defined as achieving symptomatic plus functional remission). Reference Wunderink, Sytema, Nienhuis and Wiersma17 The direction of the causality, however, may not be clear. For example, although working appears to help people recover from schizophrenia, Reference Warner39 the converse may also be true, i.e. individuals who maintain work are those who have a good prognosis. In the W-SOHO population at baseline, the frequency of paid employment was low (19%), ranging from 16% in East Asia to 23% in North Europe. This is similar to the employment rates reported for people with schizophrenia in Western countries, Reference Marwaha and Johnson40 which vary both between and within countries. However, fully dissecting the role of social functioning on outcomes in schizophrenia is complicated because clinical changes can have an impact on social functioning. Reference Warner39 There are also high rates of stigma and discrimination against people with schizophrenia across countries, Reference Thornicroft, Brohan, Rose, Sartorius and Leese41 which can have an impact on their social functioning. Reference Yanos, Roe, Markus and Lysaker42
The W-SOHO study has shown that there are cross-national differences in outcomes among out-patients with schizophrenia. Outcomes in terms of remission seem to be better for people living in low- and middle-income regions, especially Latin America. In general, the regional variation in outcome persisted even after adjusting for clinical and sociodemographic variables at baseline. Several predictive factors were identified suggesting that outcome differences are related to cultural and environmental factors rather than to differences in the disorder itself.
Acknowledgements
The authors thank Deirdre Elmhirst, PhD, for helping with the editorial development of this manuscript.











eLetters
No eLetters have been published for this article.