Depressive and anxiety disorders are the most common psychiatric condition encountered in primary healthcare, and are the leading neuropsychiatric causes of the global burden of disease. Reference Goldberg and Huxley1,Reference Lopez, Mathers, Ezzati, Jamison and Murray2 Despite strong evidence on the efficacy of specific treatments for depressive and anxiety disorders, notably antidepressant medication and brief structured psychological treatments, Reference Patel, Simon, Chowdhary, Kaaya and Araya3 up to 90% of primary care attendees with these common mental disorders in low- and middle-income countries do not receive these. Reference Wang, Aguilar-Gaxiola, Alonso, Angermeyer, Borges and Bromet4 One major barrier to improving access to evidence-based treatments for common mental disorders is the lack of trained personnel in primary care to provide psychological treatments and case management, which are essential to facilitate recovery from these disorders.
The aim of the trial was to test the effectiveness of a lay health counsellor led collaborative stepped-care intervention for common mental disorders (the MANAS intervention) in individuals attending public and private primary healthcare facilities in Goa, India. The stepped-care model has been shown to be associated with consistently superior outcomes compared with usual care, although almost all trials are from high-income countries Reference Gilbody, Whitty, Grimshaw and Thomas5 with the exception of one trial from Chile, Reference Araya, Rojas, Fritsch, Gaete, Simon and Peters6 and all focused only on depression. The MANAS trial sought to examine how to extend the reach of proven depression treatments to resource-poor primary care settings in two key ways: first, the intervention was designed for delivery by lay health workers; and second, it was designed to be appropriate for the full range of common anxiety and depressive disorders seen in primary care.
Earlier, we published the findings of the impact of the intervention on primary mental health outcomes (recovery from ICD-10 common mental disorders 7 ) at the primary end-point of 6 months. Reference Patel, Weiss, Chowdhary, Naik, Pednekar and Chatterjee8 Those analyses found that there was a modest benefit on these outcomes (risk ratio RR = 1.22, 95% CI 1.00–1.47), but also that the benefits were only evident in patients attending public facilities (RR = 1.55, 95% CI 1.02–2.35); no impact was found in people attending private facilities (RR = 0.95, 95% CI 0.74–1.22). This paper extends those findings and describes the impact of the intervention at three time points over the 12 months following trial enrolment on a wider range of outcomes, including mental health, suicidal behaviour and disability. The trial has been registered with clinicaltrials.gov (NCT00446407).
Method
Setting
The trial was conducted in Goa, a state in West India, by a consortium of organisations led by Sangath, in collaboration with the Government of Goa’s Directorate of Health Services, the Voluntary Health Association of Goa, private general practitioners and the London School of Hygiene & Tropical Medicine.
Hypothesis
A collaborative stepped-care intervention led by lay health counsellors will reduce the prevalence of common mental disorders in individuals over a 12-month period. Secondary hypotheses tested the effect of the intervention on reduction of symptom severity, suicidal behaviour and disability levels.
Design
A stratified cluster randomised design with health facility as the unit of randomisation. The trial was conducted in two consecutive phases from April 2007 to September 2009. Phase 1 involved 12 public facilities, whereas Phase 2 was conducted in 12 private facilities.
Selection of facilities and randomisation
In Phase 1, the sampling frame included all public primary healthcare facilities with the space for lay health counsellors and that were not involved in preliminary phases related to intervention development. Reference Chatterjee, Chowdhary, Pednekar, Cohen, Andrew and Araya9,Reference Patel, Araya, Chowdhary, King, Kirkwood and Nayak10 In Phase 2, we invited the participation of private general practitioners (GPs) through letters to over 400 registered practitioners; however, as the response rate was poor the research team then visited a subsample of practitioners who had not responded. Through this process, 22 eligible facilities were identified of which 12 were randomly selected for inclusion in the trial. Details of the process of identification and stratification of facilities are described elsewhere. Reference Patel, Weiss, Chowdhary, Naik, Pednekar and Chatterjee8 Facilities were randomly allocated within each stratum to either the intervention or control arm using a 1:1 allocation ratio by the trial statistician (H.W.) using the website www.randomization.com.
Participants
All primary care patients aged over 17 years were screened with the 12-item General Health Questionnaire (GHQ-12) Reference Goldberg11 using a cut-off score of 5/6 to identify ‘screen-positive’ individuals based on psychometric properties evaluated in these settings. Reference Patel, Araya, Chowdhary, King, Kirkwood and Nayak10 Eligibility criteria for participation in the trial were: screening positive for common mental disorders; being resident in Goa for the subsequent 12 months; speaking Konkani, Marathi, Hindi or English; not requiring urgent medical attention; and not having difficulty with hearing, speaking or cognition that makes interviewing difficult. If the individual gave written or verbal consent, a structured clinical diagnostic interview (the Revised Clinical Interview Schedule or CIS-R) Reference Lewis, Pelosi, Araya and Dunn12 (see below) was administered to provide a baseline assessment of severity and ICD-10 diagnostic categorisation. 7 Based on these assessments, trial participants were categorised into four a priori groups for analyses: all participants (screen-positive group); the subgroup of those who screened positive who had ICD-10 diagnoses of common mental disorders (ICD-10 diagnosis group); the subgroup of those with ICD-10 common mental disorder diagnoses with the specific diagnosis of depression (depression subgroup); and the subgroup of those who screened positive who did not meet ICD-10 criteria for common mental disorders Reference Patel, Kirkwood, Pednekar, Araya, King and Chisholm13 (subthreshold subgroup).
Sample size
Sample size estimates have been described in detail previously. Reference Patel, Kirkwood, Pednekar, Araya, King and Chisholm13 Briefly, we assumed: a coefficient of variation of 0.2; prevalence of ICD-10 common mental disorders of 66% among participants who screened positive; follow-up of 75% at 6 months. The resulting sample of 100 participants who screened positive in 24 clusters provides over 90% power to detect a difference in recovery rates of 70% in the collaborative stepped-care arm v. 50% in the enhanced usual care control arm, estimates based on earlier efficacy trials in Goa Reference Patel, Chisholm, Rabe-Hesketh, Dias-Saxena, Andrew and Mann14 and Chile. Reference Araya, Rojas, Fritsch, Gaete, Simon and Peters15 The observed value of kappa was 0.08 (equivalent to an intraclass correlation coefficient of 0.03) indicating relatively little between-cluster variability within the strata. Reference Patel, Weiss, Chowdhary, Naik, Pednekar and Chatterjee8
Interventions
All interventions were implemented at the individual level within clusters.
The collaborative stepped-care intervention
The intervention was developed following a systematic process that has been described previously. Reference Chatterjee, Chowdhary, Pednekar, Cohen, Andrew and Araya9 In brief, the intervention is based on a stepped-care approach that emphasises that relatively simple interventions such as psychoeducation are provided to all patients, more resource-intensive interventions are reserved for individuals who are severely ill or not responding to the simpler interventions. The collaborative approach involves three key team members: the lay health counsellor, the primary care physician and a visiting psychiatrist (clinical specialist). The lay health counsellors had non-healthcare backgrounds and underwent a structured 2-month training course. Reference Chowdhary, Chatterjee and Patel16 Each facility team was supported by a psychiatrist who visited about once a month and was also available for consultation on the phone. Each lay health counsellor acted as a case manager for participants who screened positive for common mental disorders and took overall responsibility for delivering all non-drug treatments, in collaboration with the primary care physician and the visiting psychiatrist, with the ultimate goal of a planned discharge upon recovery. Individuals could be discharged either in a planned manner (for example, recovered) or unplanned (for example, did not return despite adherence interventions).
There were four components to the intervention. First, all patients were offered psychoeducation, which involved explanation about the nature of the symptoms; the association of common mental disorders with interpersonal difficulties; the need to share emotional symptoms with the doctor and to share personal difficulties with caring family members or other key persons in their social network; strategies for symptom alleviation, for example breathing exercises for anxiety symptoms; the need for adherence to other treatments; and providing information about social/welfare agencies when required. Antidepressants were recommended for moderate or severe common mental disorders and for individuals who did not respond to psychoeducation alone on the basis of routine clinical assessments by the lay health counsellor. In the public facilities, the antidepressant of choice, fluoxetine, was provided free. In the private facilities, doctors could prescribe antidepressants of their choice, which were purchased by patients as usual. Once initiated, antidepressants were recommended for a minimum of 90 days at an adequate dose (for example, at least 20 mg per day of fluoxetine). Physicians were given training over half a day and a manual. Physicians were asked to encourage participants to meet the lay health counsellor, to avoid the use of unnecessary medications and to provide usual care for any coexisting physical health problems. Interpersonal psychotherapy delivered by the lay health counsellor was offered to participants who had moderate or severe common mental disorders, either in addition to antidepressants or as an alternative to antidepressants for those who did not respond to them. Interpersonal psychotherapy was chosen because of it demonstrated effectiveness in another low-income country, Reference Verdeli, Clougherty, Bolton, Speelman, Lincoln and Bass17 and for its focus on interpersonal problems such as grief, disputes and role transitions, which were common themes in the adverse life experiences among individuals with common mental disorders in Goa. Reference Pereira, Andrew, Pednekar, Pai, Pelto and Patel18 A minimum of six sessions were offered. Referral to a visiting psychiatrist was reserved for individuals who were unresponsive to the earlier treatments; were assessed to be at high suicide risk at any stage; had significant comorbidity with alcohol dependence; had associated significant other medical problems; posed diagnostic dilemmas; or for whom the primary care physician requested a consultation.
Control intervention – enhanced usual care
Physicians in usual care practices received screening results and were given a treatment manual prepared for primary care physicians. They were allowed to initiate treatments of their choice.
Measurement and outcomes
The mental health outcomes were assessed using the CIS-R, a structured interview for use by trained lay interviewers. Reference Lewis, Pelosi, Araya and Dunn12 The CIS-R is one of the most widely used measures of common mental disorders globally with extensive prior use in the study setting. Reference Patel, Chisholm, Rabe-Hesketh, Dias-Saxena, Andrew and Mann14,Reference Patel, Pereira and Mann19,Reference Patel, Kirkwood, Pednekar, Pereira, Barros and Fernandes20 The disability outcomes were assessed using the 12-item WHO Disability Assessment Schedule (WHODAS II), 21 a brief questionnaire that has been used in Goa Reference Von Korff, Ustun, Ormel, Kaplan and Simon22,Reference Patel, Pereira, Coutinho, Fernandes, Fernandes and Mann23 previously and has been used in the World Health Surveys. Both measures were used at each follow-up time point. Based on the trial protocol (http://clinicaltrials.gov/ct2/show/NCT00446407?term=MANAS&rank=1), the following outcomes are reported in this paper.
-
(a) Prevalence of common mental disorders, computed from an algorithm that generates ICD-10 diagnoses from CIS-R responses.
-
(b) Mean CIS-R score, computed from the total of the CIS-R items.
-
(c) Days of no work or reduced work in previous month, computed from two WHODAS items that ask about each of these two experiences.
-
(d) Any reported suicide plans or attempt, computed from two items that ask about these in the CIS-R.
-
(e) WHODAS scores, computed from the total score of the 12 WHODAS scoring items.
Research assessors underwent 2 weeks’ training in the use of the interview and quality assurance, including using hand-held electronic personal digital assistants to collect data.
Masking
Masking of the research assessor was maximised by: carrying out evaluations at home and by an independent research institution not associated with the intervention; randomly allocating unique participant IDs; and carrying out the primary outcome assessment prior to all other assessments.
Analyses
The primary analyses showed consistent effect modification between public and private facilities, for all outcomes. 7 Therefore in this paper, we have stratified all analyses by facility type. Furthermore, analyses testing for effect modification by type of facility over the 12-month period showed consistent evidence of effect modification for all outcomes except suicide (online Tables DS1 and DS2), confirming our decision to present stratified results in the paper. Intention-to-treat analyses were based on cluster-level summary values for each of the outcomes, the recommended approach for cluster randomised trials with fewer than 15 clusters per arm. Reference Hayes and Moulton24 The overall common mental disorders prevalence was estimated as the geometric mean of the cluster (facility) prevalences (summing across the three visits) within each arm. For suicide plans/attempts, one cluster had zero outcomes, and so the arithmetic mean of cluster suicide prevalences was estimated. For continuous outcomes, the overall means were estimated as the arithmetic mean of the cluster-level mean scores within each arm. For CIS-R scores, results are presented as the mean score and the mean percentage change in score from baseline.
Risk ratios were estimated using data from all follow-up time points (maximum of three) for which there were data. Although missing data at baseline was associated with age and gender, there was no evidence that this was associated with outcomes measured at follow-up, suggesting that the data were missing at random after conditioning on age and gender. Thus, data were not imputed, and analyses excluding missing data but adjusted for age and gender should be unbiased. Risk ratio estimation also assumed a constant effect during follow-up. To test this assumption, we used an extension of the method of Cheung et al Reference Cheung, Jeffries, Thomson and Milligan25 to test evidence for a linear trend in intervention effect over time, and also tested for effect modification between the effect at 2 and 12 months respectively to assess whether the effect waned over time.
All intervention–control comparisons were adjusted for: the imbalance between arms of case type at baseline (depression, anxiety, subthreshold symptoms); age and gender, since the probability of missing data was associated with these at baseline; and within-individual correlation between visits. For binary outcomes, adjustment was done by calculating the expected number of cases at each time point in each cluster using generalised estimating equation logistic regression, adjusting for strata, case type, age and gender and within-individual correlation between visits. The total expected number of cases over the three visits in each cluster was then compared with the total observed number, and expressed as a ratio of total observed/total expected. The adjusted risk ratio (RR) was obtained as the ratio of the geometric mean of the cluster total observed/total expected ratios in the intervention arm compared with the geometric mean of the cluster ratios in the control arm. An approximate variance for the log risk ratio in each arm was obtained from the residual mean square from a two-way analysis of variance of cluster log (total observed/total expected) on stratum and study arm. A 95% confidence interval for the risk ratio was calculated from this variance using a stratified t-statistic. Reference Hayes and Moulton24 For the continuous outcomes, the analogous analysis was carried out using linear regression. Details of trial protocol approval and consent have been published previously. Reference Patel, Kirkwood, Pednekar, Araya, King and Chisholm13
Results
The trial flow chart is shown in Fig. 1. The trial population was predominantly female (82%), with a mean age of 46.3 years (s.d. = 13.3). Of the 2242 (81%) with an ICD-10 diagnosis at baseline (ICD-10 diagnosis group), 774 (35%) had depression, including comorbid anxiety disorders (depression subgroup). The most common diagnosis was mixed anxiety–depressive disorder (n = 1032; 46% of all those with common mental disorders); the remaining 436 (19%) had a ‘pure’ anxiety disorder. In general, there was good balance between arms; although participants in the enhanced usual care arm were more likely to have depression, the proportion of those with ICD-10 diagnosis and mean CIS-R scores were similar. The proportions completing the outcome assessment were were 89% at month 2, 87% at month 6 and 85% at month 12. Overall, 2181 (78%) of all screen-positive participants were seen at all three follow-up visits. Among the primary analysis group of those with an ICD-10 diagnosis, the overall proportion with complete follow-up data was 79%. The proportion of participants with complete follow-up data was higher in the enhanced usual care arm than the collaborative stepped-care arm (80.9% v. 76.5%, P = 0.01).
Impact on mental health outcomes
In participants attending the public facilities, there was a strong impact of the intervention on reduced prevalence of common mental disorders in all analysis groups at all three time points (Fig. 2). The overall effect was a 30% reduction in prevalence in the ICD-10 diagnosis group between arms (P = 0.02); 24% reduction in the depression subgroup (P = 0.04); 34% reduction

Fig. 1 Trial flow chart.
PHC, Public health centre; GP, general practitioner, CSC, collaborative stepped care; EUC, enhanced usual care.
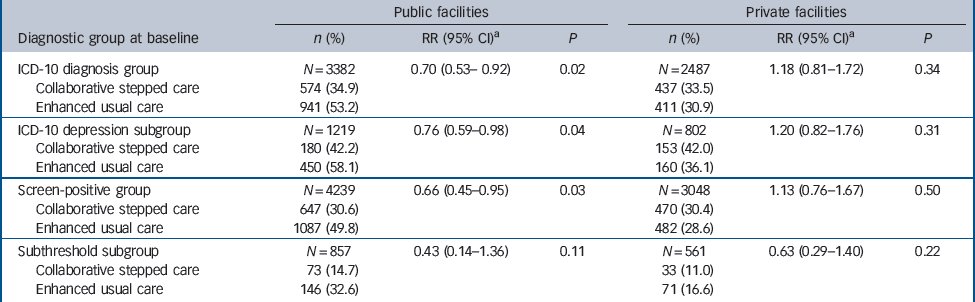
in the screen-positive group (P = 0.03); and 57% reduction in the subthreshold subgroup (P = 0.11) (Table 1). There was no evidence that the size of the effect differed over time on a relative scale (P<0.20 in each diagnostic group). The absolute difference in risk did appear to decrease from about 20% at 2 months to 12% at 12 months for all except those in the subthreshold subgroup, where it was 18% at each time point. However, this difference was not statistically significant (P<0.1 in each diagnostic group). Among all those who screened positive, treatment of five individuals will avert an average of one common mental disorder case at 2 months, and treatment of seven people will avert one case at 12 months. In contrast, no impact was observed in any analysis group among participants attending private facilities.
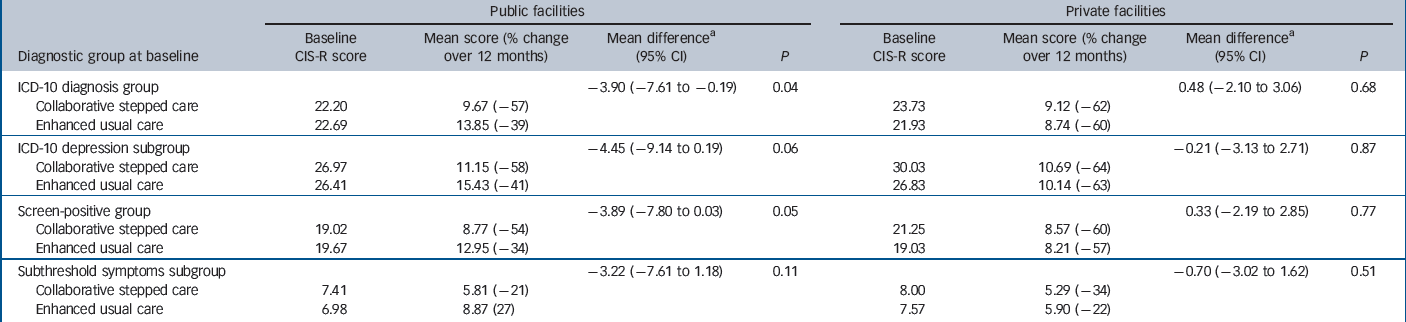
A similar picture emerged on analyses of the impact of the intervention on severity of symptoms. In public facility participants, the CIS-R scores in the intervention arm decreased by about 50% in all but the subthreshold subgroup by 2 months, compared with a decrease of about 30% in the controls. The difference persisted to 12 months (Fig. 3, Table 2) with no significant trend in effect over time. Again, no effect was observed in any analysis group among participants attending private facilities.
There was a generally high prevalence (14.0%) of reported suicide plans or attempts over the 12 months of follow-up, but evidence of a beneficial effect in the public facilities: 36% reduction in the ICD-10 group between arms (P = 0.04) and 45% reduction in the depression group (P = 0.06). Similar reductions were seen in the private facilities, but these were not significant, partly because of the smaller sample size and slightly greater variability in prevalence between clinics.
Impact on disability
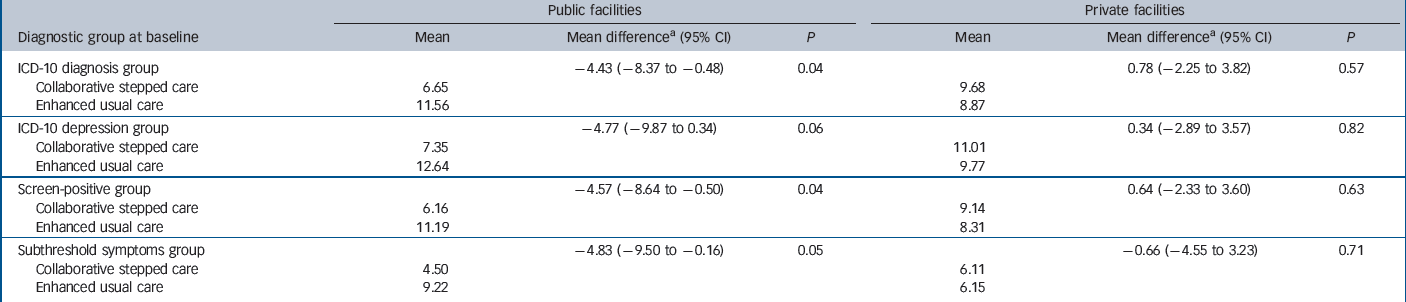
In the public facilities, there was evidence of an intervention effect on disability days (no work or reduced work) reported in the previous month in all diagnostic groups (Table 3; Fig. 5), with participants in the intervention arm reporting 4–5 fewer days of disability in the previous month than those in the control arm. As with all other outcomes, there was no impact observed in private facility participants.
There were trends towards reductions in WHODAS total disability scores observed in public facility participants, but these
Table 1 Impact of intervention on prevalence of ICD-10 common mental disorders over 12 months
| Public facilities | Private facilities | |||||
|---|---|---|---|---|---|---|
| Diagnostic group at baseline | n (%) | RR (95% CI) a | P | n (%) | RR (95% CI) a | P |
| ICD-10 diagnosis group | N = 3382 | 0.70 (0.53– 0.92) | 0.02 | N = 2487 | 1.18 (0.81–1.72) | 0.34 |
| Collaborative stepped care | 574 (34.9) | 437 (33.5) | ||||
| Enhanced usual care | 941 (53.2) | 411 (30.9) | ||||
| ICD-10 depression subgroup | N = 1219 | 0.76 (0.59–0.98) | 0.04 | N = 802 | 1.20 (0.82–1.76) | 0.31 |
| Collaborative stepped care | 180 (42.2) | 153 (42.0) | ||||
| Enhanced usual care | 450 (58.1) | 160 (36.1) | ||||
| Screen-positive group | N = 4239 | 0.66 (0.45–0.95) | 0.03 | N = 3048 | 1.13 (0.76–1.67) | 0.50 |
| Collaborative stepped care | 647 (30.6) | 470 (30.4) | ||||
| Enhanced usual care | 1087 (49.8) | 482 (28.6) | ||||
| Subthreshold subgroup | N = 857 | 0.43 (0.14–1.36) | 0.11 | N = 561 | 0.63 (0.29–1.40) | 0.22 |
| Collaborative stepped care | 73 (14.7) | 33 (11.0) | ||||
| Enhanced usual care | 146 (32.6) | 71 (16.6) | ||||
a The risk ratio (RR) is adjusted for ‘case type’ at baseline, age at baseline, gender and repeated observations per individual.

Fig. 2 Impact of the intervention on prevalence of ICD-10 common mental disorders (CMD) at 2, 6 and 12 months (m). (a) Public facilities, (b) private facilities.
did not reach statistical significance (online Figs DS1 and DS2, Table DS3).
Discussion
Main findings
The MANAS collaborative stepped-care intervention led by lay health counsellors reduced the prevalence of ICD-10 common mental disorders and the severity of symptoms of depression and anxiety in individuals attending public primary healthcare facilities with a common mental disorder (defined either on the basis of a formal diagnostic interview or a screening questionnaire) and in the subgroup of individuals with depression, over a 12-month period following enrolment in the trial. The intervention also showed benefits in reduction in the risk of suicidal behaviours (plans or attempts) and disability days (days of no work or reduced work) and weaker effects on overall disability scores in these participants. Although some benefit was noted in reduction in the prevalence of ICD-10 common mental disorders, psychological morbidity scores and disability days in those in the subthreshold subgroup, in general these were of a smaller magnitude and weaker statistical significance. Moreover, no impact was observed on any outcome, apart from a non-significant reduction in the risk of suicidal behaviours, for any diagnostic group in participants attending private primary healthcare facilities.
The findings in this paper extend in three important ways the findings of the 6-month primary end-point analyses Reference Patel, Weiss, Chowdhary, Naik, Pednekar and Chatterjee8 that the intervention improved the mental health outcomes of people with common mental disorders, and that these benefits are only evident in public primary care attendees. First, they show substantial benefits sustained across the 12-month follow-up period on both clinical outcomes in individuals attending public healthcare facilities. Second, they demonstrate an overall benefit for the diagnostic subgroup of individuals with depression in these longitudinal analyses. Third, they demonstrate the impact of the intervention on suicidal behaviour and disability outcomes, both of which are important health outcomes in their own right. To the best of our knowledge, this is the first trial from a low- and middle-income country demonstrating the impact of interventions for a mental disorder on suicidal behaviours, a major public health priority in these countries. Reference Vijayakumar, Nagaraj, Pirkis and Whiteford26 The apparently larger absolute effects of the intervention in the short-term are in line with other trials for the treatment of common mental disorders,
Table 2 Impact of intervention on psychological morbidity scores over 12 months
| Public facilities | Private facilities | |||||||
|---|---|---|---|---|---|---|---|---|
| Diagnostic group at baseline | Baseline CIS-R score | Mean score (% change over 12 months) | Mean difference a (95% CI) | P | Baseline CIS-R score | Mean score (% change over 12 months) | Mean difference a (95% CI) | P |
| ICD-10 diagnosis group | –3.90 (–7.61 to –0.19) | 0.04 | 0.48 (–2.10 to 3.06) | 0.68 | ||||
| Collaborative stepped care | 22.20 | 9.67 (–57) | 23.73 | 9.12 (–62) | ||||
| Enhanced usual care | 22.69 | 13.85 (–39) | 21.93 | 8.74 (–60) | ||||
| ICD-10 depression subgroup | –4.45 (–9.14 to 0.19) | 0.06 | –0.21 (–3.13 to 2.71) | 0.87 | ||||
| Collaborative stepped care | 26.97 | 11.15 (–58) | 30.03 | 10.69 (–64) | ||||
| Enhanced usual care | 26.41 | 15.43 (–41) | 26.83 | 10.14 (–63) | ||||
| Screen-positive group | –3.89 (–7.80 to 0.03) | 0.05 | 0.33 (–2.19 to 2.85) | 0.77 | ||||
| Collaborative stepped care | 19.02 | 8.77 (–54) | 21.25 | 8.57 (–60) | ||||
| Enhanced usual care | 19.67 | 12.95 (–34) | 19.03 | 8.21 (–57) | ||||
| Subthreshold symptoms subgroup | –3.22 (–7.61 to 1.18) | 0.11 | –0.70 (–3.02 to 1.62) | 0.51 | ||||
| Collaborative stepped care | 7.41 | 5.81 (–21) | 8.00 | 5.29 (–34) | ||||
| Enhanced usual care | 6.98 | 8.87 (27) | 7.57 | 5.90 (–22) | ||||
a Adjusted for difference in baseline Revised Clinical Interview Schedule (CIS-R) score, age at baseline, gender and repeated observations by individuals.
Table 3 Impact of intervention on total disability days in past 30 days (no work or reduced work) over 12 months
| Public facilities | Private facilities | |||||
|---|---|---|---|---|---|---|
| Diagnostic group at baseline | Mean | Mean difference a (95% CI) | P | Mean | Mean difference a (95% CI) | P |
| ICD-10 diagnosis group | –4.43 (–8.37 to –0.48) | 0.04 | 0.78 (–2.25 to 3.82) | 0.57 | ||
| Collaborative stepped care | 6.65 | 9.68 | ||||
| Enhanced usual care | 11.56 | 8.87 | ||||
| ICD-10 depression group | –4.77 (–9.87 to 0.34) | 0.06 | 0.34 (–2.89 to 3.57) | 0.82 | ||
| Collaborative stepped care | 7.35 | 11.01 | ||||
| Enhanced usual care | 12.64 | 9.77 | ||||
| Screen-positive group | –4.57 (–8.64 to –0.50) | 0.04 | 0.64 (–2.33 to 3.60) | 0.63 | ||
| Collaborative stepped care | 6.16 | 9.14 | ||||
| Enhanced usual care | 11.19 | 8.31 | ||||
| Subthreshold symptoms group | –4.83 (–9.50 to –0.16) | 0.05 | –0.66 (–4.55 to 3.23) | 0.71 | ||
| Collaborative stepped care | 4.50 | 6.11 | ||||
| Enhanced usual care | 9.22 | 6.15 | ||||
a Adjusted for difference in baseline Revised Clinical Interview Schedule (CIS-R) score, age at baseline, gender and repeated observations by individuals.

Fig. 3 Impact of the intervention on psychological morbidity (mean Revised Clinical Interview Schedule (CIS-R) score) at 2, 6 and 12 months (m). (a) Public facilities, (b) private facilities.

Fig. 4 Impact of the intervention on suicide attempts or plans over 12 months. (a) Public facilities, (b) private facilities.
RR, risk ratio.
including those in this study setting, Reference Patel, Chisholm, Rabe-Hesketh, Dias-Saxena, Andrew and Mann14,Reference Rojas, Fritsch, Solis, Jadresic, Castillo and Gonzalez27 although the difference in effect over time was not statistically significant in our study.
Process indicators for the intervention up to 6 months, which marked the maximum intervention period, were published earlier; Reference Patel, Weiss, Chowdhary, Naik, Pednekar and Chatterjee8 they showed excellent uptake of the low-intensity psychoeducation component, moderate uptake of the antidepressant component and low uptake of the more intensive interpersonal psychotherapy component. It may be argued that more intensive and longer treatments, such as aggressive pharmacotherapy and structured psychological treatments, could further increase the size and durability of the effect of the intervention.
The large difference in effect by facility type (public or private) may be attributed to at least two key factors: first, that the great difficulty we had in enroling GPs from private facilities meant that those who did participate were a non-representative, highly motivated group of practitioners committed to care for common mental disorders. Second, it is possible that the ‘personalised client-centred’ care that characterises such private practices 28 cancelled out the added value of the lay health counsellor in the intervention. Preliminary findings from in-depth interviews with the participating practitioners supports the latter possibility. It is notable that our intervention was able to lead to outcomes in public facility attendees that were at least as good as those observed in private facility patients.
Implications
The MANAS trial is the largest such trial in psychiatry from a low- and middle-income country. Apart from the limited coverage of the high-intensity psychological treatment component of the intervention, the trial was able to achieve all its a priori recruitment, intervention and follow-up targets. Based on our findings, we recommend the extension of the MANAS model to public primary healthcare facilities in India. Future research should focus on promoting the development and evaluation of culturally appropriate, affordable and acceptable psychological treatments, and more aggressive and longer-term management in those individuals whose condition is refractory.
Funding
The MANAS Project is entirely funded by a Wellcome Trust Senior Research Fellowship in Clinical Science to V.P.
Acknowledgements
We are grateful to the members of the Trial Steering and Data Monitoring & Ethics Committees for their inputs, which led to the final protocol described in this paper. We are grateful to the managements of the Directorate of Health Services, Government of Goa and of Sangath and VHAG. We are grateful to the staff of the 12 public health centres and 12 general practitioner practices.












eLetters
No eLetters have been published for this article.