Research into social factors in the aetiology of psychotic disorders has demonstrated notable variation observed by age and gender, Reference Kirkbride, Fearon, Morgan, Dazzan, Morgan and Tarrant1 cannabis use, Reference Moore, Zammit, Lingford-Hughes, Barnes, Jones and Burke2 immigrant status and ethnicity, Reference Cantor-Graae and Selten3 and urban birth and upbringing. Reference March, Hatch, Morgan, Kirkbride, Bresnahan and Fearon4 This epidemiological landscape is taken from studies predominately conducted in large cities. Reference March, Hatch, Morgan, Kirkbride, Bresnahan and Fearon4 Less is understood about these risk markers outside of conurbations, where almost one-fifth of the English population lives. 5 Delineating such epidemiology is also relevant to health services planning, particularly given recent reports that early intervention in psychosis services in both urban and rural English communities have observed psychosis rates up to three times higher than those upon which such services were first commissioned (i.e. 15/100 000 person-years). 6,Reference Cheng, Kirkbride, Lennox, Perez, Masson and Lawrence7 We present initial findings from the Social Epidemiology of Psychoses in East Anglia (SEPEA; www.sepea.org) study, a large, 3-year population-based first-episode psychoses study.
Method
The study methodology was based on the principles of a major epidemiological study of first-episode psychosis previously conducted in England, Reference Kirkbride, Fearon, Morgan, Dazzan, Morgan and Tarrant1 modified for use in early intervention services. We established a surveillance system to record socio-demographic and clinical data on all people aged 16–35 years resident within East Anglia, referred and accepted to our early intervention services with first-episode psychosis over 3 years, from 1 August 2009. ICD-10 clinical and research (OPCRIT) diagnoses for psychotic disorder (F10-39) are established at 6 months and 3 years after referral. Here, we report sample characteristics and initial incidence rates from the first 18 months of case ascertainment, using 2009 mid-term census population estimates as the denominator, adjusted for study duration. Poisson regression (Stata, version 11) explored covariate effects. Full method is given in the online supplement.
Results
Over the first 18 months of the study 510 people were referred to early intervention services in East Anglia with suspected first-episode psychosis. In total 70% (n = 357) met inclusion criteria during over 835 000 person-years of follow-up. The main reason for exclusion was not meeting clinical criteria for psychosis at referral (n = 106; 20.8%) (see online Fig. DS1 for a complete breakdown of exclusions).
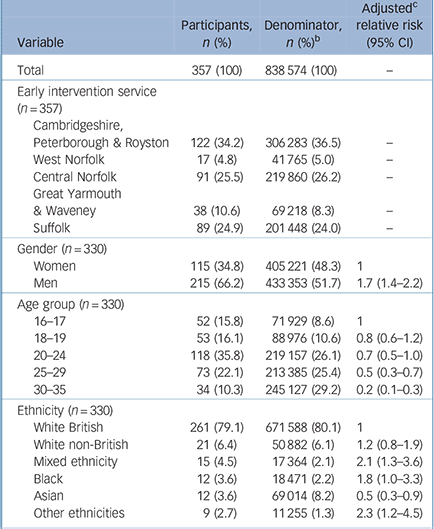
The crude incidence of clinically relevant psychotic disorder in East Anglia was estimated as 42.6/100 000 person-years (95% CI 38.4–47.2). Rates were generally similar across services (online Table DS1), but were notably raised in Great Yarmouth and Waveney (54.9/100 000 person-years; 95% CI 39.9–75.4). Completed demographic data were available on 357 individuals (92.4%) at the time of analysis. Median age at first presentation was similar for women (21.9 years, IQR = 18.2–25.8) and men (22.3 years, IQR = 19.3–26.7). Risk was elevated among men (RR = 1.7, 95% CI 1.4–2.2), after adjustment for age and ethnicity. Our data also suggested risk differed by ethnicity. Compared with the White British group, people of Black (RR = 1.8; 95% CI 1.0–3.3) and mixed ethnicities (RR = 2.1; 95% CI 1.3–3.6) were at elevated risk of psychotic disorder after adjustment for age and gender. By contrast, people of Asian origin (including the Indian subcontinent and Southeast Asia) were at lower risk of psychosis compared with the White British group (adjusted RR = 0.5, 95% CI 0.3–0.9) (Table 1).
A total of 50% of our sample were unemployed at initial referral; 25% were in paid employment, 19% were students and 4% were unpaid family carers; information was missing from 2% of our sample.
Discussion
We identified variation in the incidence of psychosis in a diverse, mainly rural English region. The overall incidence was higher than typically reported in first-episode psychosis studies of the entire adult age range (16–64 years), but this is to be expected given our lower age limit (35 years) and the decline in risk with age. Reference Kirkbride, Fearon, Morgan, Dazzan, Morgan and Tarrant1 For comparison, the incidence for people 16–35 years old in the ÆSOP study varied from 32.0/100 000 person-years in Bristol to 74.0/100 000 person-years in south-east London, placing our estimates within this range. Nevertheless, observations from both SEPEA and ÆSOP are consistent with recent empirical data Reference Cheng, Kirkbride, Lennox, Perez, Masson and Lawrence7 that the incidence of psychotic disorders seen through early intervention services is generally three times greater than the figure upon which such services were commissioned. 6 This has important implications for mental health service provision. In our sample, age at first presentation was similar for both genders before 36 years old, a point easily overlooked in entire adult-onset samples, where median age at onset typically occurs a few years later for women Reference Kirkbride, Fearon, Morgan, Dazzan, Morgan and Tarrant1 as a result of a secondary peak of psychosis close to the time of menopause, Reference Grigoriadis and Seeman8 not captured by our early intervention services data.
TABLE 1 Sample characteristics and adjusted rate ratios in the SEPEA study at 18 monthsFootnote a
| Variable | Participants, n (%) |
Denominator, n (%)Footnote b |
AdjustedFootnote
c
relative risk (95% CI) |
|---|---|---|---|
| Total | 357 (100) | 838 574 (100) | – |
| Early intervention service (n = 357) | |||
| Cambridgeshire, | |||
| Peterborough & Royston | 122 (34.2) | 306 283 (36.5) | – |
| West Norfolk | 17 (4.8) | 41 765 (5.0) | – |
| Central Norfolk | 91 (25.5) | 219 860 (26.2) | – |
| Great Yarmouth | |||
| & Waveney | 38 (10.6) | 69 218 (8.3) | – |
| Suffolk | 89 (24.9) | 201 448 (24.0) | – |
| Gender (n = 330) | |||
| Women | 115 (34.8) | 405 221 (48.3) | 1 |
| Men | 215 (66.2) | 433 353 (51.7) | 1.7 (1.4–2.2) |
| Age group (n = 330) | |||
| 16–17 | 52 (15.8) | 71 929 (8.6) | 1 |
| 18–19 | 53 (16.1) | 88 976 (10.6) | 0.8 (0.6–1.2) |
| 20–24 | 118 (35.8) | 219 157 (26.1) | 0.7 (0.5–1.0) |
| 25–29 | 73 (22.1) | 213 385 (25.4) | 0.5 (0.3–0.7) |
| 30–35 | 34 (10.3) | 245 127 (29.2) | 0.2 (0.1–0.3) |
| Ethnicity (n = 330) | |||
| White British | 261 (79.1) | 671 588 (80.1) | 1 |
| White non-British | 21 (6.4) | 50 882 (6.1) | 1.2 (0.8–1.9) |
| Mixed ethnicity | 15 (4.5) | 17 364 (2.1) | 2.1 (1.3–3.6) |
| Black | 12 (3.6) | 18 471 (2.2) | 1.8 (1.0–3.3) |
| Asian | 12 (3.6) | 69 014 (8.2) | 0.5 (0.3–0.9) |
| Other ethnicities | 9 (2.7) | 11 255 (1.3) | 2.3 (1.2–4.5) |
a Because the study is ongoing, detailed sociodemographic data were only available for a subset (n = 309) of the total incidence sample (n = 378). Thus, incidence rates were reported where we had data on the full sample (n =378), with relative risks reported from Poisson regression on demographic data for the subsample (n = 309).
b Adjusted for duration of case ascertainment in each early intervention service (18 months).
c Adjusted for other variables in model (age group, gender and ethnicity).
We also reported elevated psychosis risk for some minority groups in East Anglia, although not, even at the upper limit of the confidence interval, to the extent observed in more urban settings. Reference Cantor-Graae and Selten3 Strikingly, relative risk estimates in people from Asian populations were half those observed in the White British group. Although we cannot exclude the possibility that these differences were explained by differential service utilisation, our findings are consistent with the possibility that migrant and minority groups in more rural communities may not be exposed to the same degree to the factors that drive elevated psychosis rates in cities. This hypothesis will be pursued in the full dataset, but there is already supporting evidence: cumulative social disadvantage and separation and loss events in childhood are reported to be associated with increased odds of psychosis for both White British and ethnic minority groups but the impact of such events appears to be more pervasive among some minority groups. Reference Morgan, Kirkbride, Hutchinson, Craig, Morgan and Dazzan9,Reference Morgan, Kirkbride, Leff, Hutchinson, McKenzie and Morgan10 If socioenvironmental exposures were also amplified in urban compared with rural populations, or led to greater stress responses in urban dwellers, as has been recently observed in a small sample of healthy adults, Reference Lederbogen, Kirsch, Haddad, Streit, Tost and Schuch11 this could potentially explain the attenuation in elevated rates among rural minority populations.
Our initial data suggested that incidence rates were elevated in one of our services, and we will consider multivariate, multilevel explanations for this in our final data-set, including the possibility that the variation may be partially driven by service-side factors, such as the degree of active outreach provided by different services and the length of time services have been established. We will also be able to inspect differences in rates according to diagnostic subgroup and demographic factors not reported here (including country of birth, age at migration, generation status, occupation), compare clinical- and research-based diagnoses, and inspect the evolution of symptomatology in a first-episode sample over 3 years of treatment. Nevertheless, the incepted incidence rates assessed here through clinical early intervention services highlight a substantial burden of psychotic disorder beyond cities, and potentially provide important aetiological clues.
Funding
J.B.K. was supported by a Sir Henry Wellcome Research Fellowship from the Wellcome Trust (grant number ), through which the SEPEA study was established. P.B.J. directs the NIHR Collaboration for Leadership in Applied Health Research and Care (CLAHRC) for Cambridgeshire & Peterborough and is supported by NIHR grant . The SEPEA study has been adopted by the Mental Health Research Network (MHRN).
Acknowledgements
The authors are grateful to the clinical services and staff participating in the SEPEA study, and the MHRN for their generous support.






eLetters
No eLetters have been published for this article.