Parent psychopathology is strongly associated with offspring psychiatric disorders, Reference Beidel and Turner1-Reference Merikangas, Stolar, Stevens, Goulet, Preisig and Fenton6 a risk transmitted through both genetic and environmental mechanisms. Reference Downey and Coyne4,Reference Hettema, Prescott, Myers, Neale and Kendler7-Reference Kendler, Prescott, Myers and Neale9 A central unresolved question, though, is whether having a parent with a mental disorder creates a generalised vulnerability to psychopathology or whether particular parent disorders are associated with particular offspring disorders. Reference Bornovalova, Hicks, Iacono and McGue2 Numerous studies have examined familial aggregation of psychiatric disorders and found that some disorders appear to ‘breed true’ in families (for example, parental anxiety is associated with an increased risk for offspring anxiety), Reference Clark, Cornelius, Wood and Vanyukov3,Reference Lieb, Isensee, Hofler, Pfister and Wittchen5,Reference Biederman, Petty, Faraone, Henin, Hirshfeld-Becker and Pollack10,Reference Lieb, Wittchen, Hofler, Fuetsch, Stein and Merikangas11 although the pattern of associations differs by disorder. Reference Biederman, Petty, Faraone, Henin, Hirshfeld-Becker and Pollack10,Reference Kendler, Davis and Kessler12 However, much of this research examined a single or limited number of parent disorders without accounting for comorbidity among parent disorders, Reference Beidel and Turner1,Reference Lieb, Isensee, Hofler, Pfister and Wittchen5,Reference Merikangas, Stolar, Stevens, Goulet, Preisig and Fenton6,Reference Biederman, Petty, Faraone, Henin, Hirshfeld-Becker and Pollack10 which may have artificially inflated estimates of associations between specific parent and offspring disorders. Indeed, evidence from a national sample found that the familial aggregation of some mental disorders was substantially attenuated by adjusting for comorbid parent disorders. Reference Kendler, Davis and Kessler12 Several small family studies have reported a similar result. Reference Low, Cui and Merikangas13,Reference Merikangas, Stevens, Fenton, Stolar, O'Malley and Woods14 An additional problem is that those that considered comorbidity among parent disorders assumed additive associations. Given emerging evidence of the existence of sub-additive interactions - that is, the effects of comorbid disorders are less than the sum of their individual effects due to the incremental predictive power of individual disorders decaying as the number of comorbid disorders increases - both among temporally primary mental disorders in predicting secondary comorbid disorders Reference Kessler, Ormel, Petukhova, McLaughlin, Green and Russo15 and among childhood adversities in predicting mental disorders, Reference Green, McLaughlin, Berglund, Gruber, Sampson and Zaslavsky16,Reference Kessler, McLaughlin, Green, Gruber, Sampson and Zaslavsky17 this assumption of additivity needs to be reconsidered. The World Health Organization (WHO) World Mental Health (WMH) Surveys offer a unique opportunity to do so. We provide the first cross-national examination of the associations of parent disorders with offspring disorders from WMH surveys in 22 countries.
Method
Sample
The WMH Surveys were carried out in ten countries classified by the World Bank as high income (Belgium, France, Germany, Italy, Japan, The Netherlands, Northern Ireland, Portugal, Spain, USA), six classified as upper-middle income (Brazil, Bulgaria, Lebanon, Mexico, Romania, South Africa) and six classified as low/lower-middle income (Colombia, India, Iraq, Nigeria, Peoples Republic of China, Ukraine) 18 (online Table DS1). Individual country sample sizes ranged from 2357 (Romania) to 9282 (USA). Respondents were selected in most countries using a stratified multistage clustered-area probability sampling strategy in which samples were either nationally or regionally representative. The weighted average response rate across all countries was 71.8%.
Surveys were administered face to face in respondents' households by trained lay interviewers. Interviews were completed in two parts in all countries except Romania and South Africa, where all respondents completed the entire survey. The Part I interview was administered to all respondents and assessed the presence of core DSM-IV 19 mental disorders. Part II assessed additional disorders as well as disorder correlates. The Part II interview was administered to a probability subsample of Part I respondents that included 100% of those who met lifetime criteria for any Part I mental disorder and a probability subsample of approximately 25% of other respondents. Cases in the Part II sample were weighted by the inverse of their probability of selection to adjust for differential sampling. The current analyses were based on the weighted Part II sample (n = 51 507). Additional weights adjusted for differential probabilities of selection within and between households and matched the samples to population sociodemographic and geographic distributions. A fuller description of these procedures is provided elsewhere. Reference Harkness, Pennell, Villar, Gebler, Aguilar-Gaxiola, Bilgen, Kessler and Üstün20-Reference Pennell, Mneimneh, Bowers, Chardoul, Wells, Viana, Kessler and Üstün22 Recruitment and consent procedures were approved by the local human subjects committee that monitored the study in each country.
Measures
Mental disorders
Mental disorders were assessed with the WHO Composite International Diagnostic Interview (CIDI) Version 3.0, Reference Kessler and Üstün23 a fully structured lay-administered interview that generated diagnoses for 20 lifetime mental disorders, including mood (major depression/dysthymia, bipolar I, II and subthreshold), anxiety (generalised anxiety disorder, panic disorder, agoraphobia without panic disorder, specific phobia, social phobia, post-traumatic stress disorder, separation anxiety disorder), behaviour (attention-deficit hyperactivity disorder (ADHD), oppositional-defiant disorder, conduct disorder, intermittent explosive disorder) and substance disorders (alcohol and drug misuse, alcohol and drug dependence with misuse). The study used DSM-IV organic exclusion and diagnostic hierarchy rules (other than for oppositional-defiant disorder, which was defined with or without conduct disorder, and substance misuse, which was defined with or without dependence). As detailed elsewhere, Reference Haro, Arbabzadeh-Bouchez, Brugha, di Girolamo, Guyer and Jin24 masked clinical reappraisal interviews with the Structured Clinical Interview for DSM-IV (SCID) Reference First, Spitzer, Gibbon and Williams25 in four WMH countries found generally good concordance between diagnoses based on the CIDI and SCID, with area under the receiver operating characteristic curve of 0.75-0.93 for mood disorders, 0.65-0.81 for anxiety disorders, 0.62-0.88 for substance disorders and 0.86 for ADHD. Reference Haro, Arbabzadeh-Bouchez, Brugha, di Girolamo, Guyer and Jin24 Age at onset of lifetime disorders was assessed retrospectively using a special question sequence that has been shown experimentally to yield more plausible distributions than standard age-at-onset questions. Reference Knauper, Cannell, Schwarz, Bruce and Kessler26 The prevalence of respondent disorders has been reported previously, Reference Kessler, Angermeyer, Anthony, de Graaf, Demyttenaere and Gasquet27 and is shown in online Table DS2.
Parent psychopathology
Parent disorders were assessed with an expanded version of the Family History Research Diagnostic Criteria Interview (FHRDCI). Reference Endicott, Andreasen and Spitzer28,Reference Kendler, Silberg, Neale, Kessler, Heath and Eaves29 Respondents reported parent disorders that were present during at least some part of their childhoods. The disorders assessed included major depressive episodes, panic disorder, generalised anxiety disorder, substance dependence and antisocial personality disorder as well as parent suicide attempt and suicide death. Each type of parent disorder was coded present if the respondent reported it for either his/her mother or father. The FHRCDI has high interrater reliability, Reference Kendler, Silberg, Neale, Kessler, Heath and Eaves29 good predictive validity Reference Kendler and Roy30 and good diagnostic agreement between offspring reports and parent interviews. Reference Prescott, Sullivan, Myers, Patterson, Devitt and Halberstadt31 The prevalence of reported parent disorders is shown in online Table DS3.
Analysis methods
The associations between parent psychopathology and lifetime occurrence of respondent disorders were estimated in a series of discrete-time survival models with person-year as the unit of analysis Reference Efron32 and controls for country, respondent age at interview and gender. We first examined a series of bivariate models in which each type of parent disorder was considered individually as a predictor of the full range of respondent disorders. We then estimated a set of multivariate models in which all parent disorders were considered simultaneously in predicting respondent disorders. Subsequent models examined the associations of either (a) number of parent disorders or (b) both number and type of parent disorders with respondent disorders. Each model began by using a consolidated set of 17 separate person-year data files that focused on a single respondent outcome disorder (major depression/dysthymia, and bipolar I, II and subthreshold were each examined in a single person-year file); this forced the estimated slopes of respondent disorders on parent disorders to be constant across outcomes. We then disaggregated this consolidated set of files to predict first onset of disorders within each of four broad disorder classes (mood, anxiety, substance and behaviour disorders).
The population attributable risk proportion (PARP) of respondent disorders predicted by parent disorders was computed for the best-fitting multivariate model using simulation methods that generated individual-level predicted probabilities of the outcome disorders from the coefficients in the model with and without coefficients for parent disorders. The PARP can be interpreted as the proportion of the observed outcomes that would not have occurred in the absence of one or more predictors based on the assumption that the coefficients in the model represents causal effects of the predictor. Survival coefficients and their standard errors were exponentiated and presented as odds ratios (ORs) with 95% confidence intervals. To adjust for sample weighting and clustering, standard errors were estimated using the Taylor series method Reference Wolter33 implemented in the SUDAAN (version 8.01) software system on Unix. Statistical significance was consistently evaluated using 0.05 level two-sided tests.
Results
Preliminary analysis
We first conducted preliminary tests to determine whether the associations between parent and offspring mental disorders differed depending on which parent (i.e. mother or father) had the disorder, how many parents had the disorder (i.e. one or both) and whether the respondent was a male or female. These analyses showed that the associations consistently differed depending on whether one or both parents had a disorder, with the exception of parent suicide death. All subsequent models therefore included separate dummy variables coding whether one or both parents had each disorder and whether either parent had died by suicide. As distinguishing between whether a respondent's mother or father had the disorder influenced only the associations involving parent substance misuse, an additional predictor was included in the final specification to distinguish maternal from paternal substance misuse. Gender of the respondent did not interact with any parent disorder. We also evaluated whether parent suicide attempt and death contributed unique information in predicting offspring disorders or whether they could be combined into a single suicidality indicator. These analyses suggested that both indicators had unique associations with offspring disorders; they were therefore retained as separate variables in all analyses. Parent death by suicide was the only type of parent psychopathology entered as a time-varying covariate, as information was not available on the respondent's age when each parent disorder started. We knew only that the parent disorder was present for at least some of the respondent's childhood, and we coded these disorders as time-invariant predictors.
Associations of parent disorders with offspring disorders
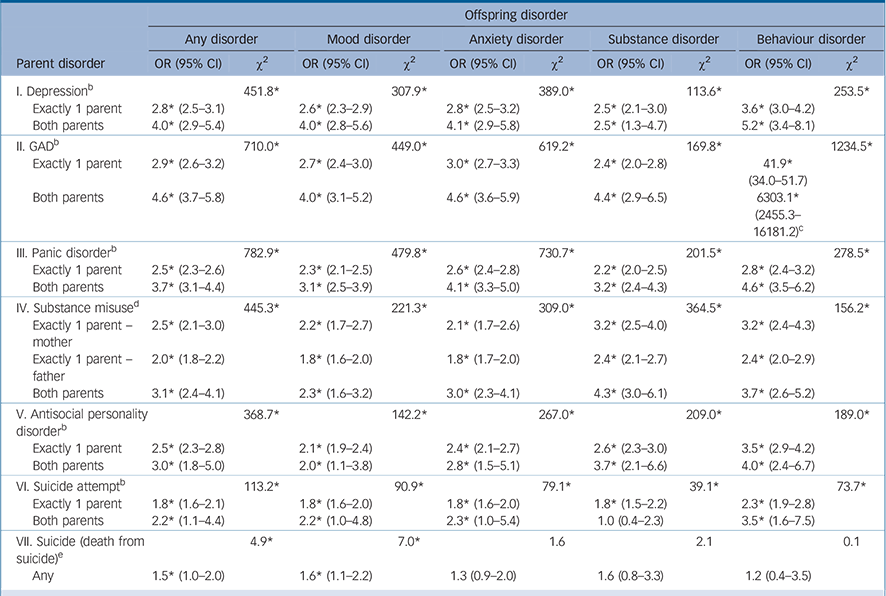
In bivariate models that considered only one type of parent disorder at a time, all parent disorders are significant predictors of lifetime onset of offspring DSM-IV/CIDI disorders in pooled models that combined estimates across all offspring disorders (Table 1). Odds ratios are in the range 1.8-2.9 for one parent having a given disorder and 2.2-4.6 for both parents having a disorder. In all cases, the odds are higher if both parents had the disorder than if only one did. A similar pattern is observed
TABLE 1 Bivariate associations of parent disorders with subsequent onset of offspring lifetime DSM-IV/CIDI disorders a
| Offspring disorder | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Any disorder | Mood disorder | Anxiety disorder | Substance disorder | Behaviour disorder | ||||||
| Parent disorder | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 |
| I. Depression b | 451.8 * | 307.9 * | 389.0 * | 113.6 * | 253.5 * | |||||
| Exactly 1 parent | 2.8 * (2.5–3.1) | 2.6 * (2.3–2.9) | 2.8 * (2.5–3.2) | 2.5 * (2.1–3.0) | 3.6 * (3.0–4.2) | |||||
| Both parents | 4.0 * (2.9–5.4) | 4.0 * (2.8–5.6) | 4.1 * (2.9–5.8) | 2.5 * (1.3–4.7) | 5.2 * (3.4–8.1) | |||||
| II. GAD b | 710.0 * | 449.0 * | 619.2 * | 169.8 * | 1234.5 * | |||||
| Exactly 1 parent | 2.9 * (2.6–3.2) | 2.7 * (2.4–3.0) | 3.0 * (2.7–3.3) | 2.4 * (2.0–2.8) | 41.9 * (34.0–51.7) | |||||
| Both parents | 4.6 * (3.7–5.8) | 4.0 * (3.1–5.2) | 4.6 * (3.6–5.9) | 4.4 * (2.9–6.5) | 6303.1 * (2455.3–16181.2) c | |||||
| III. Panic disorder b | 782.9 * | 479.8 * | 730.7 * | 201.5 * | 278.5 * | |||||
| Exactly 1 parent | 2.5 * (2.3–2.6) | 2.3 * (2.1–2.5) | 2.6 * (2.4–2.8) | 2.2 * (2.0–2.5) | 2.8 * (2.4–3.2) | |||||
| Both parents | 3.7 * (3.1–4.4) | 3.1 * (2.5–3.9) | 4.1 * (3.3–5.0) | 3.2 * (2.4–4.3) | 4.6 * (3.5–6.2) | |||||
| IV. Substance misuse d | 445.3 * | 221.3 * | 309.0 * | 364.5 * | 156.2 * | |||||
| Exactly 1 parent – mother | 2.5 * (2.1–3.0) | 2.2 * (1.7–2.7) | 2.1 * (1.7–2.6) | 3.2 * (2.5–4.0) | 3.2 * (2.4–4.3) | |||||
| Exactly 1 parent – father | 2.0 * (1.8–2.2) | 1.8 * (1.6–2.0) | 1.8 * (1.7–2.0) | 2.4 * (2.1–2.7) | 2.4 * (2.0–2.9) | |||||
| Both parents | 3.1 * (2.4–4.1) | 2.3 * (1.6–3.2) | 3.0 * (2.3–4.1) | 4.3 * (3.0–6.1) | 3.7 * (2.6–5.2) | |||||
| V. Antisocial personality disorder b | 368.7 * | 142.2 * | 267.0 * | 209.0 * | 189.0 * | |||||
| Exactly 1 parent | 2.5 * (2.3–2.8) | 2.1 * (1.9–2.4) | 2.4 * (2.1–2.7) | 2.6 * (2.3–3.0) | 3.5 * (2.9–4.2) | |||||
| Both parents | 3.0 * (1.8–5.0) | 2.0 * (1.1–3.8) | 2.8 * (1.5–5.1) | 3.7 * (2.1–6.6) | 4.0 * (2.4–6.7) | |||||
| VI. Suicide attempt b | 113.2 * | 90.9 * | 79.1 * | 39.1 * | 73.7 * | |||||
| Exactly 1 parent | 1.8 * (1.6–2.1) | 1.8 * (1.6–2.0) | 1.8 * (1.6–2.0) | 1.8 * (1.5–2.2) | 2.3 * (1.9–2.8) | |||||
| Both parents | 2.2 * (1.1–4.4) | 2.2 * (1.0–4.8) | 2.3 * (1.0–5.4) | 1.0 (0.4–2.3) | 3.5 * (1.6–7.5) | |||||
| VII. Suicide (death from suicide) e | 4.9 * | 7.0 * | 1.6 | 2.1 | 0.1 | |||||
| Any | 1.5 * (1.0–2.0) | 1.6 * (1.1–2.2) | 1.3 (0.9–2.0) | 1.6 (0.8–3.3) | 1.2 (0.4–3.5) | |||||
GAD, generalised anxiety disorder.
a Assessed in the Part II sample. Models control for country, person-year, age and gender.
b For χ2 d.f. = 2.
c Although the number of respondents who reported that both their parents had GAD is small, the consistency of these respondents having multiple behaviour disorders is so great that the association between both-parent GAD and offspring behaviour disorders is statistically significant despite the instability of the OR and CI.
d For χ2 d.f. = 3.
e Parent death from suicide is a time-varying predictor; all other parent disorders are considered time-invariant. For χ2 d.f. = 1.
* Significant at the 0.05 level, two-sided test.
in bivariate models predicting each of the four disorder classes. Each type of parent disorder significantly predicts each of the four types of offspring disorders, with the exception of parent death by suicide. Within-class associations (such as parent depression predicting offspring mood disorders) are somewhat higher than across-class associations (such as parent depression predicting offspring behaviour disorders). However, this pattern is not pronounced and there are notable exceptions to it, such as parent generalised anxiety disorder having an odds ratio as large as that of parent depression in predicting offspring mood disorders, and parent generalised anxiety disorder as well as parent depression both having higher odds ratios than parent antisocial personality disorder in predicting offspring behaviour disorders.
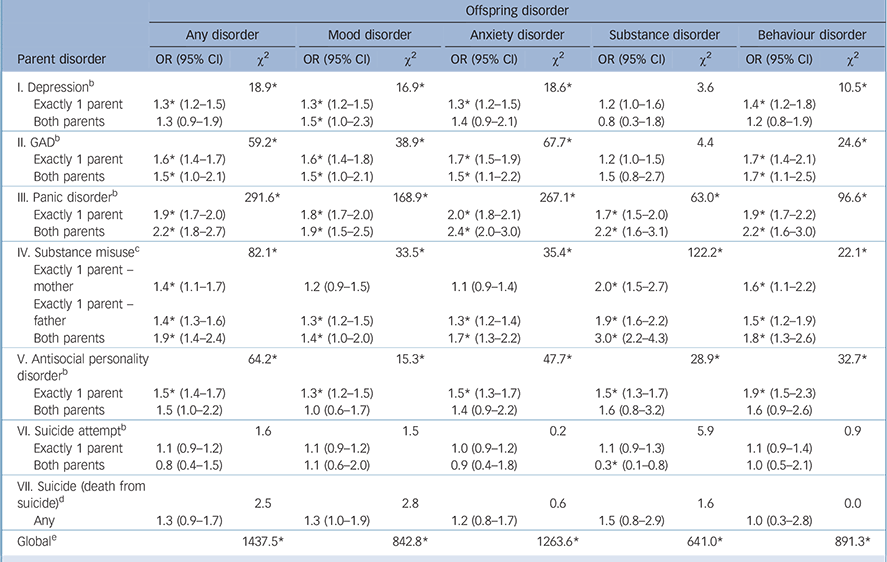
The bivariate associations are uniformly attenuated in the additive multivariate model (Table 2). Five of the seven types of parent psychopathology are significantly associated with offspring mental disorders in the pooled model (odds ratios in the range 1.3-1.9 for one parent and 1.5-2.2 for both parents). Neither parent suicide attempt nor suicide death are associated with offspring disorders in this model. The odds of offspring disorder was higher if both parents had the disorder only in the cases of parent panic disorder and substance misuse. A test for the joint associations of all parent disorders in this model was significant (χ2 14 = 1437.5, P<0.001).
Disaggregation of this model by type of offspring disorders reveals little variation. All types of parent disorder other than suicide attempt and suicide death predict offspring mood, anxiety
TABLE 2 Multivariate associations of parent disorders with subsequent onset of offspring lifetime DSM-IV/CIDI disorders based on an additive model a
| Offspring disorder | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Any disorder | Mood disorder | Anxiety disorder | Substance disorder | Behaviour disorder | ||||||
| Parent disorder | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 |
| I. Depression b | 18.9 * | 16.9 * | 18.6 * | 3.6 | 10.5 * | |||||
| Exactly 1 parent | 1.3 * (1.2–1.5) | 1.3 * (1.2–1.5) | 1.3 * (1.2–1.5) | 1.2 (1.0–1.6) | 1.4 * (1.2–1.8) | |||||
| Both parents | 1.3 (0.9–1.9) | 1.5 * (1.0–2.3) | 1.4 (0.9–2.1) | 0.8 (0.3–1.8) | 1.2 (0.8–1.9) | |||||
| II. GAD b | 59.2 * | 38.9 * | 67.7 * | 4.4 | 24.6 * | |||||
| Exactly 1 parent | 1.6 * (1.4–1.7) | 1.6 * (1.4–1.8) | 1.7 * (1.5–1.9) | 1.2 (1.0–1.5) | 1.7 * (1.4–2.1) | |||||
| Both parents | 1.5 * (1.0–2.1) | 1.5 * (1.0–2.1) | 1.5 * (1.1–2.2) | 1.5 (0.8–2.7) | 1.7 * (1.1–2.5) | |||||
| III. Panic disorder b | 291.6 * | 168.9 * | 267.1 * | 63.0 * | 96.6 * | |||||
| Exactly 1 parent | 1.9 * (1.7–2.0) | 1.8 * (1.7–2.0) | 2.0 * (1.8–2.1) | 1.7 * (1.5–2.0) | 1.9 * (1.7–2.2) | |||||
| Both parents | 2.2 * (1.8–2.7) | 1.9 * (1.5–2.5) | 2.4 * (2.0–3.0) | 2.2 * (1.6–3.1) | 2.2 * (1.6–3.0) | |||||
| IV. Substance misuse c | 82.1 * | 33.5 * | 35.4 * | 122.2 * | 22.1 * | |||||
| Exactly 1 parent – mother | 1.4 * (1.1–1.7) | 1.2 (0.9–1.5) | 1.1 (0.9–1.4) | 2.0 * (1.5–2.7) | 1.6 * (1.1–2.2) | |||||
| Exactly 1 parent – father | 1.4 * (1.3–1.6) | 1.3 * (1.2–1.5) | 1.3 * (1.2–1.4) | 1.9 * (1.6–2.2) | 1.5 * (1.2–1.9) | |||||
| Both parents | 1.9 * (1.4–2.4) | 1.4 * (1.0–2.0) | 1.7 * (1.3–2.2) | 3.0 * (2.2–4.3) | 1.8 * (1.3–2.6) | |||||
| V. Antisocial personality disorder b | 64.2 * | 15.3 * | 47.7 * | 28.9 * | 32.7 * | |||||
| Exactly 1 parent | 1.5 * (1.4–1.7) | 1.3 * (1.2–1.5) | 1.5 * (1.3–1.7) | 1.5 * (1.3–1.7) | 1.9 * (1.5–2.3) | |||||
| Both parents | 1.5 (1.0–2.2) | 1.0 (0.6–1.7) | 1.4 (0.9–2.2) | 1.6 (0.8–3.2) | 1.6 (0.9–2.6) | |||||
| VI. Suicide attempt b | 1.6 | 1.5 | 0.2 | 5.9 | 0.9 | |||||
| Exactly 1 parent | 1.1 (0.9–1.2) | 1.1 (0.9–1.2) | 1.0 (0.9–1.2) | 1.1 (0.9–1.3) | 1.1 (0.9–1.4) | |||||
| Both parents | 0.8 (0.4–1.5) | 1.1 (0.6–2.0) | 0.9 (0.4–1.8) | 0.3 * (0.1–0.8) | 1.0 (0.5–2.1) | |||||
| VII. Suicide (death from suicide) d | 2.5 | 2.8 | 0.6 | 1.6 | 0.0 | |||||
| Any | 1.3 (0.9–1.7) | 1.3 (1.0–1.9) | 1.2 (0.8–1.7) | 1.5 (0.8–2.9) | 1.0 (0.3–2.8) | |||||
| Global e | 1437.5 * | 842.8 * | 1263.6 * | 641.0 * | 891.3 * | |||||
GAD, generalised anxiety disorder.
a Assessed in the Part II sample. Models include dummy variables for all parent mental disorders and control for country, person-year, age and gender.
b For χ2 d.f. = 2.
c For χ2 d.f. = 3.
d Parent death from suicide is a time-varying predictor; all other parent disorders are not time-varying. For χ2 d.f. = 1.
e For χ2 d.f. = 14. Global chi-squared test for the joint associations of all parent disorder types with each of the offspring outcome disorder classes.
* Significant at the 0.05 level, two-sided test.
and behaviour disorders. The one exception is offspring substance disorders, where parent generalised anxiety disorder and depression are not significant predictors. The joint associations of all parent disorders as a set are significant in predicting all four classes of offspring disorders (χ2 14 = 641.0-1263.6, P<0.001). Within-class associations are generally stronger than across-class associations, with two exceptions. First, parent generalised anxiety disorder and panic disorder are stronger predictors than parent depression of offspring mood disorders. Second, parent panic disorder is as strong a predictor as parent antisocial personality disorder of offspring behaviour disorders.
Associations of number of parent disorders with offspring disorders
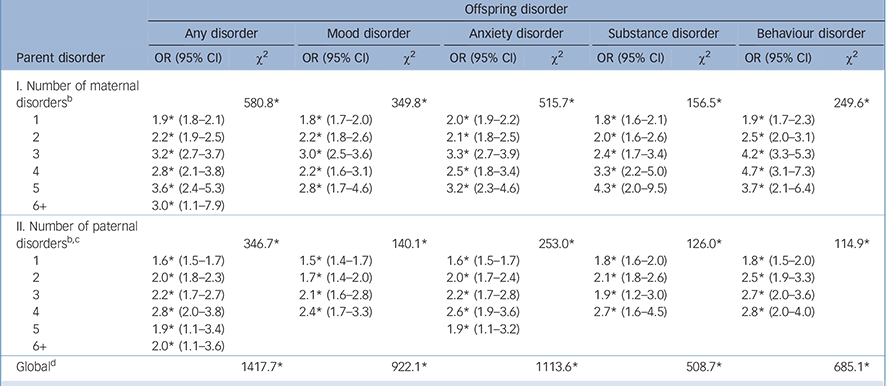
A generally increasing association exists between number of parent disorders and odds of offspring disorders in the pooled model, with odds ratios ranging from 1.9 for exactly one maternal disorder to 3.0-3.6 for five and six or more maternal disorders (Table 3). The odds ratios increase from 1.6 for exactly one paternal disorder to 2.8 for exactly four paternal disorders and then decrease to 1.9-2.0 for five and six or more paternal disorders. The joint associations of number-of-parental disorders with pooled offspring disorders is significant for both maternal (χ2 5 = 580.8, P<0.001) and paternal (χ2 5 = 346.7, P<0.001) disorders.
Disaggregation of this model shows a similar pattern in predicting each class of offspring disorders, with joint associations of both maternal and paternal number-of-disorders significant in predicting each class of offspring disorders (χ2 5 = 114.9-515.7, P<0.001). A monotonic dose-response relationship exists between number of maternal disorders and odds of offspring substance disorder.
Associations of type-number of parent disorders with offspring disorders
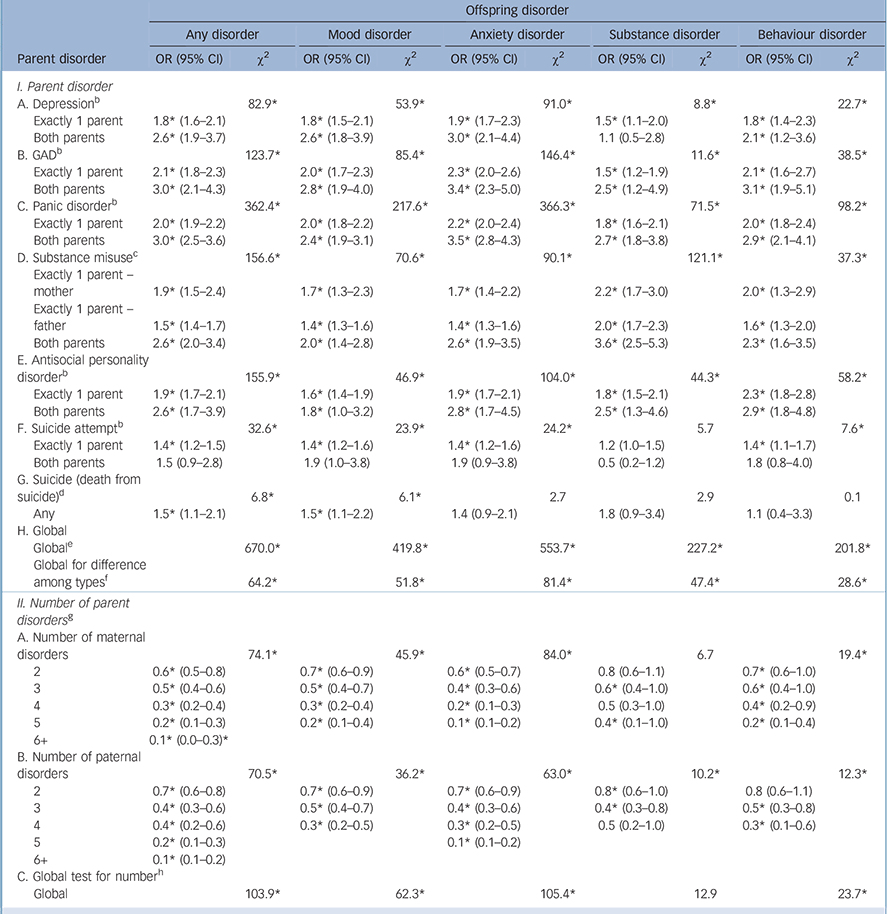
We next estimated a series of multivariate models that included both type and number of parent disorders as predictors (Table 4). Each type of parent disorder is significantly associated with odds of offspring disorders in the pooled model (odds ratios in the range 1.4-2.1 for one parent and 1.5-3.0 for both parents), controlling for number of disorders. Types of parent disorders are significant as a set after controlling for number of disorders (χ2 14 = 670.0, P<0.001). The odds ratio associated with parent disorder types in this model are generally higher than in the additive model. This means that the additivity assumption led to a downward bias in the estimated associations of parent disorders with offspring disorders in the earlier model. This bias occurred because the odds ratios associated with number of parent disorders are significant as a set (χ2 5 = 74.1, P<0.001 for maternal disorders and χ2 5 = 70.5, P<0.001 for paternal disorders) and consistently less than 1.0 in the pooled model that includes terms for both type and number of disorders. This pattern of associations suggests the presence of sub-additive interactions among comorbid parent disorders; that is, the odds ratios of
TABLE 3 Multivariate associations between number of parent disorders and subsequent onset of offspring lifetime DSM-IV/CIDI disorders a
| Offspring disorder | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Any disorder | Mood disorder | Anxiety disorder | Substance disorder | Behaviour disorder | ||||||
| Parent disorder | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 |
| I. Number of maternal disorders b | 580.8 * | 349.8 * | 515.7 * | 156.5 * | 249.6 * | |||||
| 1 | 1.9 * (1.8–2.1) | 1.8 * (1.7–2.0) | 2.0 * (1.9–2.2) | 1.8 * (1.6–2.1) | 1.9 * (1.7–2.3) | |||||
| 2 | 2.2 * (1.9–2.5) | 2.2 * (1.8–2.6) | 2.1 * (1.8–2.5) | 2.0 * (1.6–2.6) | 2.5 * (2.0–3.1) | |||||
| 3 | 3.2 * (2.7–3.7) | 3.0 * (2.5–3.6) | 3.3 * (2.7–3.9) | 2.4 * (1.7–3.4) | 4.2 * (3.3–5.3) | |||||
| 4 | 2.8 * (2.1–3.8) | 2.2 * (1.6–3.1) | 2.5 * (1.8–3.4) | 3.3 * (2.2–5.0) | 4.7 * (3.1–7.3) | |||||
| 5 | 3.6 * (2.4–5.3) | 2.8 * (1.7–4.6) | 3.2 * (2.3–4.6) | 4.3 * (2.0–9.5) | 3.7 * (2.1–6.4) | |||||
| 6+ | 3.0 * (1.1–7.9) | |||||||||
| II. Number of paternal disorders b,c | 346.7 * | 140.1 * | 253.0 * | 126.0 * | 114.9 * | |||||
| 1 | 1.6 * (1.5–1.7) | 1.5 * (1.4–1.7) | 1.6 * (1.5–1.7) | 1.8 * (1.6–2.0) | 1.8 * (1.5–2.0) | |||||
| 2 | 2.0 * (1.8–2.3) | 1.7 * (1.4–2.0) | 2.0 * (1.7–2.4) | 2.1 * (1.8–2.6) | 2.5 * (1.9–3.3) | |||||
| 3 | 2.2 * (1.7–2.7) | 2.1 * (1.6–2.8) | 2.2 * (1.7–2.8) | 1.9 * (1.2–3.0) | 2.7 * (2.0–3.6) | |||||
| 4 | 2.8 * (2.0–3.8) | 2.4 * (1.7–3.3) | 2.6 * (1.9–3.6) | 2.7 * (1.6–4.5) | 2.8 * (2.0–4.0) | |||||
| 5 | 1.9 * (1.1–3.4) | 1.9 * (1.1–3.2) | ||||||||
| 6+ | 2.0 * (1.1–3.6) | |||||||||
| Global d | 1417.7 * | 922.1 * | 1113.6 * | 508.7 * | 685.1 * | |||||
a Assessed in the Part II sample. Models include dummy variables for number of parent mental disorders and control for country, person-year, age and gender.
b For χ2 d.f. = 2.
c For number of parental disorders, the last odds ratio represents the odds of the number or more. For example, for mood disorders, the last odds ratio for maternal disorders represents 5 or more maternal disorders.
d For χ2 d.f. = 12. Global chi-squared test for the joint associations of number of parent disorders with each of the offspring outcome disorder classes.
* Significant at the 0.05 level, two-sided test.
parent disorders predicting offspring disorders decrease as the number of comorbid parent disorders increases.
Disaggregation of this model shows that the same basic pattern of associations exists in predicting all four classes of offspring disorders. Every type of parent disorder is associated with elevated odds of offspring mood disorders; all types other than suicide death with offspring anxiety and behaviour disorders; and all types other than suicide attempt and suicide death with offspring substance disorders. Significant sub-additive interactions among parent disorders occur for both maternal and paternal disorders in predicting all classes of offspring disorder, with the exception of maternal disorders predicting offspring substance disorders. Patterns of within-class and between-class coefficients associated with types of parent disorders are similar to those in the additive model.
Population-level associations of parent disorders with offspring disorders
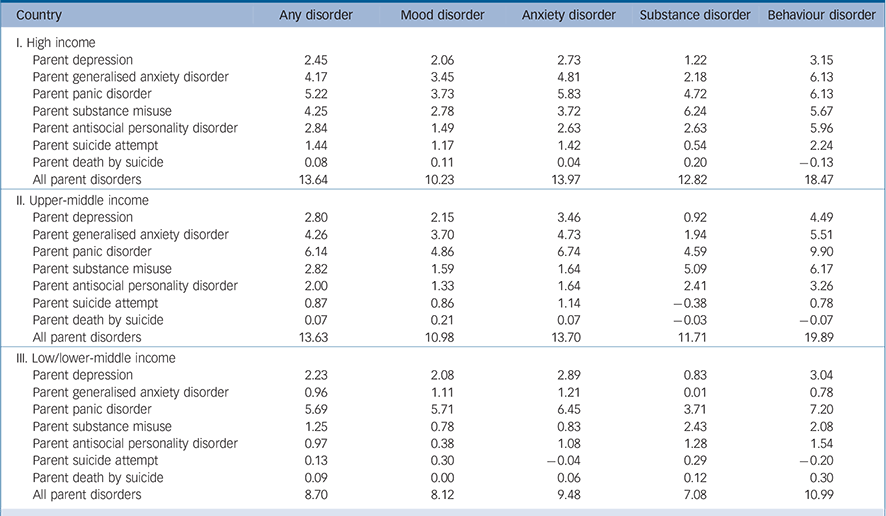
The PARPs based on the most complex multivariate model show that parent disorders explain, in a predictive sense, 12.4% of all offspring disorders (9.8% of offspring mood disorders, 13.0% of anxiety disorders, 11.4% of substance disorders and 17.3% of behaviour disorders) (Table 5). Parent panic disorder has the largest disorder-specific PARP (5.5% for all disorders, and 4.5-7.2% for disorder classes), whereas parent suicide attempt and death have the lowest PARPs. Disaggregation of results by income level of country (high, upper-middle and low/lower-middle) reveals remarkable consistency across country groups (Table 6). The highest PARP in all country groups is associated with parent disorders predicting offspring behaviour disorders. Parent panic disorder has the largest disorder-specific PARP in all country groups (5.2-6.1% of all disorders) and parent suicide attempt and death have the lowest (0.1-1.4% of all disorders). The PARPs are relatively comparable in high- and upper-middle-income countries and smaller in low/lower-middle-income countries (80% of comparisons). The PARP of all parent disorders predicting all offspring disorder is 13.6% in high-income, 13.6% in upper-middle-income and 8.7% in low/lower-middle-income countries.
Discussion
Main findings
This study provides novel information about the relationship between parent psychopathology and offspring mental disorders using data from a coordinated set of surveys conducted in 22 countries around the world. Study results indicated that each parent disorder examined, with the exception of suicide, was associated with increased risk for every class of offspring mental disorder. This pattern was evident even after controlling for the presence of comorbid parent disorders as well as for number of parent disorders. Although we found within-class associations involving pure parent disorders generally to be higher than across-class associations, this pattern was weak. We also found consistent evidence of sub-additive interactions, which means that the joint odds ratios of multiple parent disorders with offspring disorders are for the most part significantly less than the product of the odds ratios associated with the component pure disorders. At a population-level, parent disorders were associated with a meaningful (7.1-19.9% across country and outcome disorder groups), although not overwhelming, proportion of all offspring disorders. To our knowledge, we provided the first estimates of the population-level influence of parent psychopathology on offspring disorders.
Strengths and limitations
The cross-national population-based nature of our data is unique and consequently may have produced results that are more generalisable than those reported from smaller and more selected samples. Nonetheless, these findings should be interpreted in light of study limitations. Most notably, parent disorders were assessed via informant reports made by their grown children. Although
TABLE 4 Multivariate associations of types and number of parent psychopathology and mental disorders a
| Offspring disorder | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Any disorder | Mood disorder | Anxiety disorder | Substance disorder | Behaviour disorder | ||||||
| Parent disorder | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 | OR (95% CI) | χ 2 |
| I. Parent disorder | ||||||||||
| A. Depression b | 82.9 * | 53.9 * | 91.0 * | 8.8 * | 22.7 * | |||||
| Exactly 1 parent | 1.8 * (1.6–2.1) | 1.8 * (1.5–2.1) | 1.9 * (1.7–2.3) | 1.5 * (1.1–2.0) | 1.8 * (1.4–2.3) | |||||
| Both parents | 2.6 * (1.9–3.7) | 2.6 * (1.8–3.9) | 3.0 * (2.1–4.4) | 1.1 (0.5–2.8) | 2.1 * (1.2–3.6) | |||||
| B. GAD b | 123.7 * | 85.4 * | 146.4 * | 11.6 * | 38.5 * | |||||
| Exactly 1 parent | 2.1 * (1.8–2.3) | 2.0 * (1.7–2.3) | 2.3 * (2.0–2.6) | 1.5 * (1.2–1.9) | 2.1 * (1.6–2.7) | |||||
| Both parents | 3.0 * (2.1–4.3) | 2.8 * (1.9–4.0) | 3.4 * (2.3–5.0) | 2.5 * (1.2–4.9) | 3.1 * (1.9–5.1) | |||||
| C. Panic disorder b | 362.4 * | 217.6 * | 366.3 * | 71.5 * | 98.2 * | |||||
| Exactly 1 parent | 2.0 * (1.9–2.2) | 2.0 * (1.8–2.2) | 2.2 * (2.0–2.4) | 1.8 * (1.6–2.1) | 2.0 * (1.8–2.4) | |||||
| Both parents | 3.0 * (2.5–3.6) | 2.4 * (1.9–3.1) | 3.5 * (2.8–4.3) | 2.7 * (1.8–3.8) | 2.9 * (2.1–4.1) | |||||
| D. Substance misusec | 156.6 * | 70.6 * | 90.1 * | 121.1 * | 37.3 * | |||||
| Exactly 1 parent – mother | 1.9 * (1.5–2.4) | 1.7 * (1.3–2.3) | 1.7 * (1.4–2.2) | 2.2 * (1.7–3.0) | 2.0 * (1.3–2.9) | |||||
| Exactly 1 parent – father | 1.5 * (1.4–1.7) | 1.4 * (1.3–1.6) | 1.4 * (1.3–1.6) | 2.0 * (1.7–2.3) | 1.6 * (1.3–2.0) | |||||
| Both parents | 2.6 * (2.0–3.4) | 2.0 * (1.4–2.8) | 2.6 * (1.9–3.5) | 3.6 * (2.5–5.3) | 2.3 * (1.6–3.5) | |||||
| E. Antisocial personality disorder b | 155.9 * | 46.9 * | 104.0 * | 44.3 * | 58.2 * | |||||
| Exactly 1 parent | 1.9 * (1.7–2.1) | 1.6 * (1.4–1.9) | 1.9 * (1.7–2.1) | 1.8 * (1.5–2.1) | 2.3 * (1.8–2.8) | |||||
| Both parents | 2.6 * (1.7–3.9) | 1.8 * (1.0–3.2) | 2.8 * (1.7–4.5) | 2.5 * (1.3–4.6) | 2.9 * (1.8–4.8) | |||||
| F. Suicide attempt b | 32.6 * | 23.9 * | 24.2 * | 5.7 | 7.6 * | |||||
| Exactly 1 parent | 1.4 * (1.2–1.5) | 1.4 * (1.2–1.6) | 1.4 * (1.2–1.6) | 1.2 (1.0–1.5) | 1.4 * (1.1–1.7) | |||||
| Both parents | 1.5 (0.9–2.8) | 1.9 (1.0–3.8) | 1.9 (0.9–3.8) | 0.5 (0.2–1.2) | 1.8 (0.8–4.0) | |||||
| G. Suicide (death from suicide) d | 6.8 * | 6.1 * | 2.7 | 2.9 | 0.1 | |||||
| Any | 1.5 * (1.1–2.1) | 1.5 * (1.1–2.2) | 1.4 (0.9–2.1) | 1.8 (0.9–3.4) | 1.1 (0.4–3.3) | |||||
| H. Global | ||||||||||
| Global e | 670.0 * | 419.8 * | 553.7 * | 227.2 * | 201.8 * | |||||
| Global for difference among types f | 64.2 * | 51.8 * | 81.4 * | 47.4 * | 28.6 * | |||||
| II. Number of parent disorders g | ||||||||||
| A. Number of maternal disorders | 74.1 * | 45.9 * | 84.0 * | 6.7 | 19.4 * | |||||
| 2 | 0.6 * (0.5–0.8) | 0.7 * (0.6–0.9) | 0.6 * (0.5–0.7) | 0.8 (0.6–1.1) | 0.7 * (0.6–1.0) | |||||
| 3 | 0.5 * (0.4–0.6) | 0.5 * (0.4–0.7) | 0.4 * (0.3–0.6) | 0.6 * (0.4–1.0) | 0.6 * (0.4–1.0) | |||||
| 4 | 0.3 * (0.2–0.4) | 0.3 * (0.2–0.4) | 0.2 * (0.1–0.3) | 0.5 (0.3–1.0) | 0.4 * (0.2–0.9) | |||||
| 5 | 0.2 * (0.1–0.3) | 0.2 * (0.1–0.4) | 0.1 * (0.1–0.2) | 0.4 * (0.1–1.0) | 0.2 * (0.1–0.4) | |||||
| 6+ | 0.1 * (0.0–0.3) * | |||||||||
| B. Number of paternal disorders | 70.5 * | 36.2 * | 63.0 * | 10.2 * | 12.3 * | |||||
| 2 | 0.7 * (0.6–0.8) | 0.7 * (0.6–0.9) | 0.7 * (0.6–0.9) | 0.8 * (0.6–1.0) | 0.8 (0.6–1.1) | |||||
| 3 | 0.4 * (0.3–0.6) | 0.5 * (0.4–0.7) | 0.4 * (0.3–0.6) | 0.4 * (0.3–0.8) | 0.5 * (0.3–0.8) | |||||
| 4 | 0.4 * (0.2–0.6) | 0.3 * (0.2–0.5) | 0.3 * (0.2–0.5) | 0.5 (0.2–1.0) | 0.3 * (0.1–0.6) | |||||
| 5 | 0.2 * (0.1–0.3) | 0.1 * (0.1–0.2) | ||||||||
| 6+ | 0.1 * (0.1–0.2) | |||||||||
| C. Global test for number h | ||||||||||
| Global | 103.9 * | 62.3 * | 105.4 * | 12.9 | 23.7 * | |||||
GAD, generalised anxiety disorder.
a Assessed in the Part II sample. Models include dummy variables for both type and number of parent mental disorders and control for country, person–year, age and gender.
b For χ2 d.f. = 2.
d Parent death from suicide is a time-varying predictor; all other parent disorders are not time-varying. For χ2 d.f. = 1.
e For χ2 d.f. = 14. Global chi-squared test for the joint associations of all parent disorder types with each of the offspring outcome disorder classes.
f For χ2 d.f. = 12. Global chi-squared test to determine whether the odds ratios are the same for all parent disorder types.
g For number of parental disorders, the last odds ratio represents the odds of the number or more. For example, for mood disorders, the last odds ratio for maternal disorders represents five or more maternal disorders. No variable for exactly one parent disorder in included in the model, as this value is redundant with the information on types of disorders. For χ2 d.f. = 5.
h For χ2 d.f. = 10.
* Significant at the 0.05 level, two-sided test.
known to provide useful information about the presence of mental disorders in relatives, Reference Kendler and Roy30,Reference Prescott, Sullivan, Myers, Patterson, Devitt and Halberstadt31 this method of collecting information is susceptible to recall error and bias, Reference Roy, Walsh and Kendler34 with respondents who have a psychiatric disorder more likely than those without to report psychopathology in their family members. Reference Kendler, Silberg, Neale, Kessler, Heath and Eaves29,Reference Milne, Caspi, Crump, Poulton, Rutter and Sears35 Because previous research suggests that respondents with a mental disorder are more likely than unaffected siblings to report that same disorder in a parent, Reference Kendler, Silberg, Neale, Kessler, Heath and Eaves29 any such bias would have inflated within-class associations in the current study. However, our results indicate less familial aggregation of specific disorder classes than prior studies. Reference Low, Cui and Merikangas13
Second, the survey only assessed parent disorders present during the respondent's childhood. This likely resulted in under-reporting of parent disorders, given that respondents may not have had a full appreciation of parental symptoms. If respondents consequently reported only the most severe parent disorders, this may have inflated estimates of parent-offspring disorder
TABLE 5 Population attributable risk proportions (PARP) of parent psychopathology predicting lifetime mental disorders in the total sample a

| All countries | Any disorder | Mood disorder | Anxiety disorder | Substance disorder | Behaviour disorder |
|---|---|---|---|---|---|
| Parent depression | 2.63 | 2.22 | 3.10 | 1.42 | 3.83 |
| Parent generalised anxiety disorder | 3.36 | 2.85 | 4.02 | 1.77 | 4.95 |
| Parent panic disorder | 5.46 | 4.48 | 6.18 | 4.37 | 7.23 |
| Parent substance misuse | 3.16 | 1.96 | 2.59 | 5.02 | 4.97 |
| Parent antisocial personality disorder | 2.19 | 1.20 | 2.08 | 2.29 | 4.52 |
| Parent suicide attempt | 0.98 | 0.85 | 1.00 | 0.46 | 1.45 |
| Parent death by suicide | 0.07 | 0.09 | 0.04 | 0.12 | 0.02 |
| All parent disorders | 12.37 | 9.81 | 13.00 | 11.41 | 17.28 |
a The model presented in Table 4 was used to estimate the PARP. Each row displays the proportion of disorder onsets in the population that are attributable to each parental disorder. The final row of the table shows the proportion of disorder onsets in the population that are attributable to all parental disorders jointly.
TABLE 6 Population attributable risk proportions (PARP) of parent psychopathology predicting lifetime mental disorders disaggregated by country income group a
| Country | Any disorder | Mood disorder | Anxiety disorder | Substance disorder | Behaviour disorder |
|---|---|---|---|---|---|
| I. High income | |||||
| Parent depression | 2.45 | 2.06 | 2.73 | 1.22 | 3.15 |
| Parent generalised anxiety disorder | 4.17 | 3.45 | 4.81 | 2.18 | 6.13 |
| Parent panic disorder | 5.22 | 3.73 | 5.83 | 4.72 | 6.13 |
| Parent substance misuse | 4.25 | 2.78 | 3.72 | 6.24 | 5.67 |
| Parent antisocial personality disorder | 2.84 | 1.49 | 2.63 | 2.63 | 5.96 |
| Parent suicide attempt | 1.44 | 1.17 | 1.42 | 0.54 | 2.24 |
| Parent death by suicide | 0.08 | 0.11 | 0.04 | 0.20 | –0.13 |
| All parent disorders | 13.64 | 10.23 | 13.97 | 12.82 | 18.47 |
| II. Upper-middle income | |||||
| Parent depression | 2.80 | 2.15 | 3.46 | 0.92 | 4.49 |
| Parent generalised anxiety disorder | 4.26 | 3.70 | 4.73 | 1.94 | 5.51 |
| Parent panic disorder | 6.14 | 4.86 | 6.74 | 4.59 | 9.90 |
| Parent substance misuse | 2.82 | 1.59 | 1.64 | 5.09 | 6.17 |
| Parent antisocial personality disorder | 2.00 | 1.33 | 1.64 | 2.41 | 3.26 |
| Parent suicide attempt | 0.87 | 0.86 | 1.14 | –0.38 | 0.78 |
| Parent death by suicide | 0.07 | 0.21 | 0.07 | –0.03 | –0.07 |
| All parent disorders | 13.63 | 10.98 | 13.70 | 11.71 | 19.89 |
| III. Low/lower-middle income | |||||
| Parent depression | 2.23 | 2.08 | 2.89 | 0.83 | 3.04 |
| Parent generalised anxiety disorder | 0.96 | 1.11 | 1.21 | 0.01 | 0.78 |
| Parent panic disorder | 5.69 | 5.71 | 6.45 | 3.71 | 7.20 |
| Parent substance misuse | 1.25 | 0.78 | 0.83 | 2.43 | 2.08 |
| Parent antisocial personality disorder | 0.97 | 0.38 | 1.08 | 1.28 | 1.54 |
| Parent suicide attempt | 0.13 | 0.30 | –0.04 | 0.29 | –0.20 |
| Parent death by suicide | 0.09 | 0.00 | 0.06 | 0.12 | 0.30 |
| All parent disorders | 8.70 | 8.12 | 9.48 | 7.08 | 10.99 |
a The model presented in Table 4 was used to estimate the PARP. Each row displays the proportion of disorder onsets in the population that are attributable to each parental disorder. The final row of each of the three sections the table shows the proportion of disorder onsets in the population that are attributable to all parental disorders jointy.
associations. On the other hand, lack of information on parent disorders occurring later in the respondent's life likely produced conservative estimates of the associations between parent and offspring disorders.
Third, the WMH Surveys do not have a genetically informative design, making it impossible to estimate the heritability of specific disorders or determine the proportion of parent-offspring disorder associations that were due to genetic v. environmental factors.
Fourth, we focused only on a small number of common parent disorders rather than on more severe but uncommon disorders (such as psychotic disorders). Because familial transmission is likely to be most evident for severe disorders, Reference Merikangas, Stevens, Fenton, Stolar, O'Malley and Woods14 inclusion of less severe parent disorders would have attenuated associations with offspring disorders. Finally, although PARP is a joint function of the prevalence of parent disorder and the strength of association with offspring disorders, we did not distinguish between these two factors in our comparisons across country groups. Examination of these joint effects at a disaggregated country level represents an important area for future research.
Comparison with previous findings
Within the context of these limitations, our results are similar to those of previous studies in documenting significant associations between parent and offspring disorders. Indeed, we found that virtually every type of parent mental disorder was associated with elevated odds of every class of offspring disorder. This was true even after accounting for type and number of comorbid parent disorders. Because the controls for number of disorders can be interpreted as pooled interactions, the net associations of individual parent disorders with offspring disorders (in the model that controls number of disorders) can be interpreted as the estimated associations of pure parent disorders (i.e. comparisons between parents who had a history of only that one disorder v. parents who had no disorders) with offspring disorders. This means that pure parent disorders have relatively pervasive associations with offspring disorders.
We found less familial aggregation of specific disorder classes than many prior studies, Reference Lieb, Isensee, Hofler, Pfister and Wittchen5,Reference Merikangas, Stolar, Stevens, Goulet, Preisig and Fenton6,Reference Lieb, Wittchen, Hofler, Fuetsch, Stein and Merikangas11 with little specificity in the associations of particular parent disorders with particular offspring disorders, other than a modest pattern of within-class associations being larger than across-class associations. This pattern is indirectly consistent with research suggesting that most genetic liability factors are associated with a propensity to experience internalising and externalising pathology rather than with elevated risk of specific disorders. Reference Kendler, Prescott, Myers and Neale9,Reference Kendler, Davis and Kessler12,Reference Hicks, Krueger, Iacono, McGue and Patrick36 Other data consistent with this general pattern has been reported, such as a finding that parent depression was associated with increased risk for a wide range of offspring disorders Reference Lieb, Isensee, Hofler, Pfister and Wittchen5 and that numerous parent disorders were associated with offspring social phobia. Reference Lieb, Wittchen, Hofler, Fuetsch, Stein and Merikangas11 Although other studies found more specificity in the intergenerational transmission of particular disorders, including anxiety disorders, Reference Beidel and Turner1,Reference Biederman, Petty, Faraone, Henin, Hirshfeld-Becker and Pollack10 substance use disorders, Reference Merikangas, Stolar, Stevens, Goulet, Preisig and Fenton6 behavioural disorders Reference Clark, Cornelius, Wood and Vanyukov3 and major depression, Reference Lieb, Isensee, Hofler, Pfister and Wittchen5 the majority of these studies were based on relatively small samples and examined only a single or limited number of parent disorders. The few previous studies with sufficient sample sizes that included controls for comorbid disorders have typically found a more generalised pattern of intergenerational transmission of mental disorders similar to the pattern found here. Reference Bornovalova, Hicks, Iacono and McGue2,Reference Kendler, Davis and Kessler12,Reference Hicks, Krueger, Iacono, McGue and Patrick36
This pattern raises important questions about why parent psychopathology is a relatively non-specific risk factor for offspring disorders. One possibility is that parents with mental disorders not only transmit genetic vulnerability to their offspring, but also are more likely than parents without psychopathology to engage in negative parenting behaviours that do not vary substantially by type of parent disorder. Reference Downey and Coyne4,Reference Lieb, Wittchen, Hofler, Fuetsch, Stein and Merikangas11,Reference Chen and Johnston37 Consistent with this possibility, parent psychopathology has been associated in several studies with a wide range of maladaptive family-related adversities, such as maltreatment and family violence. Reference Green, McLaughlin, Berglund, Gruber, Sampson and Zaslavsky16,Reference Kessler, McLaughlin, Green, Gruber, Sampson and Zaslavsky17,Reference Conron, Beardslee, Koenen, Buka and Gortmaker38 These adversities, in turn, have been shown to be robust and relatively non-specific risk factors of adult psychiatric disorders. Reference Green, McLaughlin, Berglund, Gruber, Sampson and Zaslavsky16,Reference Kessler, McLaughlin, Green, Gruber, Sampson and Zaslavsky17
Our findings that the associations of maternal and paternal psychopathology with offspring disorders were relatively similar, that these associations did not vary by gender of offspring and that the odds of offspring disorder were consistently higher when both parents had a disorder rather than only one parent are all broadly consistent with previous research. Reference Lieb, Isensee, Hofler, Pfister and Wittchen5,Reference Dierker, Merikangas and Szatmari39 Although parent-offspring associations within-disorder classes were found to be generally stronger than across-class associations, these patterns were weak and had some exceptions, such as parent generalised anxiety disorder and panic disorder predicting offspring mood disorders more strongly than parent depression. Most of these deviations are consistent with evidence from behaviour genetics research that genetic liability factors broadly predispose individuals to develop internalising pathology Reference Kendler, Prescott, Myers and Neale9 and that similar genetic factors underlie generalised anxiety disorder and depression Reference Kendler, Neale, Kessler, Heath and Eaves8 as well as generalised anxiety disorder and panic disorder. Reference Hettema, Prescott, Myers, Neale and Kendler7 We also found that parent depression and generalised anxiety disorder were associated with offspring behaviour disorders as strongly as parent antisocial personality disorder. This pattern is similar to the previous finding of a high degree of familial co-aggregation between depressive and behavioural disorders. Reference Biederman, Faraone, Hirshfeld-Becker, Friedman, Robin and Rosenbaum40
The pervasive pattern of sub-additive interactions among comorbid parent disorders in predicting offspring disorders reported here represents a unique contribution of this study. This pattern mirrors associations observed among a wide range of childhood adversities in predicting subsequent first onset of mental disorders Reference Green, McLaughlin, Berglund, Gruber, Sampson and Zaslavsky16,Reference Kessler, McLaughlin, Green, Gruber, Sampson and Zaslavsky17 as well as associations among temporally primary disorders in predicting the subsequent first onset of other secondary disorders. Reference Kessler, Ormel, Petukhova, McLaughlin, Green and Russo15 It is important to recognise that these negative interactions do not mean that additional parent disorders are associated with decreased risk of offspring disorders, but that increases in risk occur at a decreasing rate. This can be seen most clearly in Table 3, where we find that the odds ratios associated with high parent comorbidity are elevated but not dramatically higher than the odds ratios associated with lower numbers of parent disorders. We observed these sub-additive interactions for all disorder classes in offspring, other than for the association of maternal disorders with offspring substance disorders.
Implications
Our findings suggest that future behaviour genetics studies should both assess comorbid parent disorders and utilise appropriate statistical models to account for the non-additive associations of comorbid parent disorders with offspring disorders. To the extent that the sub-additive interactions reflect causal effects of parent disorders, this pattern implies that intervening to treat any single parent disorder in the presence of comorbidity would likely have little effect on offspring disorder, as odds of offspring disorder are not markedly lower in the presence of a small compared with a large number of parent disorders. Effective interventions to prevent offspring disorders would consequently require intervening so as to protect the child from the full range of parent disorders. Given that parent disorders are robust predictors of offspring disorders across all the disorder classes and country groups considered here, it is important to recognise the potential public health importance of such interventions not only to improve the functioning of mentally ill parents but also to reduce the intergenerational transmission of mental disorders.
Funding
The World Health Organization (WHO) World Mental Health (WMH) Survey Initiative was supported by the United States National Institute of Mental Health (, ), NIMH - Mental Health Burden Study: Contract number , the John D. and Catherine T. MacArthur Foundation, the Pfizer Foundation, the US Public Health Service (, and ), the Fogarty International Center (), the Pan American Health Organization (PAHO), the Eli Lilly & Company Foundation, Ortho-McNeil Pharmaceutical, GlaxoSmithKline, Bristol-Myers Squibb and Shire. Each WMH country obtained funding for its own survey. The São Paulo Megacity Mental Health Survey is supported by the State of São Paulo Research Foundation (FAPESP) Thematic Project Grant . The Bulgarian Epidemiological Study of common mental disorders EPIBUL is supported by the Ministry of Health and the National Center for Public Health Protection. The Chinese World Mental Health Survey Initiative is supported by the Pfizer Foundation. The Shenzhen Mental Health Survey is supported by the Shenzhen Bureau of Health and the Shenzhen Bureau of Science, Technology, and Information. The Colombian National Study of Mental Health (NSMH) is supported by the Ministry of Social Protection. The ESEMeD project is funded by the European Commission (Contracts ; ), the Piedmont Region (Italy), Fondo de Investigación Sanitaria, Instituto de Salud Carlos III, Spain (), Ministerio de Ciencia y Tecnología, Spain (), Departament de Salut, Generalitat de Catalunya, Spain, Instituto de Salud Carlos III (, ) and other local agencies and by an unrestricted educational grant from GlaxoSmithKline. The Epidemiological Study on Mental Disorders in India was funded jointly by Government of India and WHO. Implementation of the Iraq Mental Health Survey (IMHS) and data entry were carried out by the staff of the Iraqi MOH and MOP with direct support from the Iraqi IMHS team with funding from both the Japanese and European Funds through United Nations Development Group Iraq Trust Fund (UNDG ITF). The World Mental Health Japan (WMHJ) Survey is supported by the Grant for Research on Psychiatric and Neurological Diseases and Mental Health (, , ) from the Japan Ministry of Health, Labour and Welfare. The Lebanese National Mental Health Survey (LEBANON) is supported by the Lebanese Ministry of Public Health, the WHO (Lebanon), National Institute of Health/Fogarty International Center (), anonymous private donations to IDRAAC, Lebanon, and unrestricted grants from Janssen Cilag, Eli Lilly, GlaxoSmithKline, AstraZeneca, Hikma Pharm and Novartis. The Mexican National Comorbidity Survey (MNCS) is supported by The National Institute of Psychiatry Ramon de la Fuente () and by the National Council on Science and Technology (), with supplemental support from PAHO. The Nigerian Survey of Mental Health and Wellbeing (NSMHW) is supported by the WHO (Geneva), the WHO (Nigeria) and the Federal Ministry of Health, Abuja, Nigeria. The Northern Ireland Study of Mental Health was funded by the Health & Social Care Research & Development Division of the Public Health Agency. The Portuguese Mental Health Study was carried out by the Department of Mental Health, Faculty of Medical Sciences, NOVA University of Lisbon, with collaboration of the Portuguese Catholic University, and was funded by Champalimaud Foundation, Gulbenkian Foundation, Foundation for Science and Technology (FCT) and Ministry of Health. The Romania WMH study projects ‘Policies in Mental Health Area’ and ‘National Study regarding Mental Health and Services Use’ were carried out by National School of Public Health & Health Services Management (former National Institute for Research & Development in Health, present National School of Public Health Management & Professional Development, Bucharest), with technical support of Metro Media Transilvania, the National Institute of Statistics - National Centre for Training in Statistics, SC. Cheyenne Services SRL, Statistics Netherlands and were funded by Ministry of Public Health (former Ministry of Health) with supplemental support of Eli Lilly Romania SRL. The South Africa Stress and Health Study (SASH) is supported by the US National Institute of Mental Health () and National Institute of Drug Abuse with supplemental funding from the South African Department of Health and the University of Michigan. The Ukraine Comorbid Mental Disorders during Periods of Social Disruption (CMDPSD) study was funded by the US National Institute of Mental Health (). The US National Comorbidity Survey Replication (NCS-R) is supported by the National Institute of Mental Health () with supplemental support from the National Institute of Drug Abuse, the Substance Abuse and Mental Health Services Administration, the Robert Wood Johnson Foundation (grant ) and the John W. Alden Trust.
Acknowledgements
We thank the WHO WMH staff for assistance with instrumentation, fieldwork and data analysis. A complete list of all within-country and cross-national WMH publications can be found at www.hcp.med.harvard.edu/wmh/.











eLetters
No eLetters have been published for this article.