The military conflicts in Iraq and Afghanistan have heightened awareness of the health consequences of traumatic brain injury (TBI). For more severe TBIs, neuropsychological deficits such as impairment of attention, memory and cognitive processing efficiency constitute a major category of potential adverse TBI-related outcomes Reference Dikmen, Corrigan, Levin, Machamer, Stiers and Weisskopf1 and can lead to significant functional impairment. Reference Rassovsky, Satz, Alfano, Light, Zaucha and McArthur2 For milder brain injuries, however, the evidence that these injuries lead to chronic neuropsychological deficits or functional impairment independently of psychiatric factors is less clear. Reference Dikmen, Corrigan, Levin, Machamer, Stiers and Weisskopf1,Reference Dikmen, Machamer, Fann and Temkin3–Reference Ivins, Kane and Schwab8 Because mild TBI (sometimes referred to as concussion, especially at the mildest end of the severity continuum) is associated with increased risk of psychiatric conditions in both war-zone veterans Reference Rona, Jones, Fear, Hull, Murphy and Machell9–Reference Tanielian and Jaycox11 and civilians Reference Bryant, O'Donnell, Creamer, McFarlane, Clark and Silove12,Reference Levin, McCauley, Pedroza Josic, Boake, Brown and Goodman13 there is considerable controversy regarding whether neuropsychological deficits and related functional health impairment enduring beyond the acute phases of recovery from milder deployment-related TBIs are better explained by comorbid psychiatric conditions such as post-traumatic stress disorder (PTSD) and depression. Reference Hoge, Goldberg and Castro14 Understanding of the source(s) of prolonged impairment following relatively mild TBI will be critical to establishing optimal treatment protocols among returning war-zone veterans.
A major shortcoming of the TBI literature is the absence in most studies of pre-injury measures of relevant outcome variables. Without baseline measures, it is difficult to determine whether post-TBI deficits reflect change, premorbid functioning, and/or reporting biases. This problem can be compounded when outcome measures rely solely on subjective self-report, which do not always correspond to objective performances. Reference David, Farrin, Hull, Unwin, Wessely and Wykes15 The overreliance on cross-sectional data is reflected by the 2008 Institute of Medicine 16 recommendation that future work include prospective assessment of objective neuropsychological performances. In keeping with the 2008 Institute of Medicine recommendation, this study examined associations of self-reported TBI, PTSD symptoms and depression symptoms with performance-based neuropsychological outcomes and subjective health-related functioning in 760 US Army soldiers who were deployed to Iraq and underwent neuropsychological assessment before and after their deployments. Reflecting the larger deployed population, the majority of TBI events in this sample would be considered mild.
Method
Human subjects approvals were obtained from US Army, Tulane University Health Sciences Center and US Department of Veterans Affairs review boards. All participants provided written informed consent prior to participation.
Study design and participants
The participants were 760 US Army soldiers enrolled in the Neurocognition Deployment Health Study (NDHS), a longitudinal cohort study. Reference Vasterling, Proctor, Amoroso, Kane, Gackstetter and Ryan17 For this report, we included regular active duty soldiers who deployed to Iraq and who completed both pre- and post-deployment in-person assessments.
Detailed sampling, recruitment and consent procedures are described elsewhere. Reference Vasterling, Proctor, Amoroso, Kane, Heeren and White18 In brief, sampling was conducted at the military battalion level. Because deployment information was classified at the time of the study, units were selected by US Army Forces Command on the basis of each unit's projected deployment schedule and unit function. Military units represented combat (such as the infantry), combat support (such as combat engineers) and service support (such as supply) functions. For most participants (n = 661), pre-deployment assessments were conducted between April and December 2003; post-deployment assessments were conducted between January and May 2005. To centre the assessments around the deployments of the participants, the dates of the assessments varied across battalions, according to when each battalion deployed and subsequently returned from deployment. A subgroup of participants (n = 99), who had previously served as a non-deployed comparison sample but later deployed to Iraq, Reference Vasterling, Proctor, Amoroso, Kane, Heeren and White18 completed pre-deployment assessments between May and July 2004 and post-deployment assessments in December 2005. By selecting units differing in their deployment schedule, geographic location within Iraq and unit-level functions, we were able to capture relatively heterogeneous deployment experiences within the sample. Battalion-level units originated from Fort Hood, Texas, and Fort Lewis, Washington.
At the pre-deployment assessment sessions, battalion leaders were asked to refer potential participants at random (for example every third name on the unit roster). Figure 1 depicts the sampling and reasons for non-participation at post-deployment assessment. In summary, at pre-deployment, 1276 (93.5%) of 1365 invited regular active duty soldiers volunteered participation. At post-deployment, soldiers who participated at pre-deployment, who remained in active duty military service, and who were still assigned to the same military installation after returning from deployment (n = 912) were again invited to participate. Of the 912 soldiers eligible for post-deployment assessment, 804 (88.2%) completed the on-site assessment at post-deployment. Among eligible soldiers, the predominant reason for non-participation at post-deployment was unavailability due to leave or special training assignments. Less than 9% declined participation. Of the 804 participants completing the on-site assessment at post-deployment, an additional 44 participants were excluded for internally inconsistent questionnaire responses, not completing the neuropsychological evaluation at both time points, or insufficient effort on a cognitive task of motivation, Reference Tombaugh19 resulting in a final sample of 760 participants (Fig. 1).
Among participants for whom deployment dates were available (n = 758), all but 29 served their scheduled 12-month Operation Iraqi Freedom rotation. Pre-deployment assessments occurred an average of 97.9 days (s.d. = 87.5, median 87.5, IQR = 59) prior to deployment; post-deployment assessment of soldiers serving full tours occurred an average of 79.9 days (s.d. = 24.7, median 78, IQR = 29) from each participant's return from Iraq.

FIG. 1 Sample selection and longitudinal retention.
Procedures and assessment protocol
Procedures were conducted at military installations. Written surveys were administered in small groups; interviews and neuropsychological tasks were administered individually. The full NDHS data-set is described elsewhere. Reference Vasterling, Proctor, Amoroso, Kane, Gackstetter and Ryan17 Brief descriptions of measures relevant to this report follow.
Demographic and military (for example rank, deployment history) information was queried via interview and written surveys. Military information was verified by service records. Combat intensity was quantified by a modified version of the Combat Experiences Scales of the Deployment Risk and Resilience Inventory (DRRI). Reference King, King, Vogt, Knight and Samper20 Insufficient cognitive effort was defined as scores below 38 on Trial 1 of the Test of Memory Malingering. Reference Tombaugh19
Traumatic brain injury incurred between the pre- and post-deployment study sessions (inter-session TBI) was assessed via interview. We included non-deployment TBIs within the inter-session interval because the neuropsychological assessment dates spanned an interval slightly broader than the actual deployment, and any TBI incurred outside of deployment but between the two assessment sessions would potentially influence outcomes. Congruent with reports showing stronger associations between clinical outcomes and TBI following loss of consciousness v. altered consciousness, Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10,Reference Luethcke, Bryan, Morrow and Isler21 only those pre- to post-deployment interval injuries resulting in loss of consciousness were queried. If participants reported >1 head injury with loss of consciousness between pre- and post-deployment assessments, the experience of multiple injuries was recorded, and subsequent questions pertained to the most significant injury (index TBI), as identified by the participant. Injury attributes queried pertained to TBI characteristics empirically linked to cognitive outcomes: date of injury, duration of loss of consciousness (<1 min, 1–30 min, >30 min), memory for the event (yes/no) and duration of post-traumatic amnesia (none, <1 h, 1–24 h, >24 h).
At pre-deployment, we screened for history of prior head injury with >15 min loss of consciousness (yes/no) via written survey. Although we anticipated that most participants reporting head injury with loss of consciousness would likely be classified as mild by current severity categorisation methods, reflecting the broader deployed population, we did not exclude participants reporting injury characteristics suggestive of greater than mild TBI.
Post-traumatic stress disorder symptom severity was measured with the PTSD Checklist, Civilian Version (PCL-C), Reference Ruggiero, Del–Ben, Scotti and Rabalais22 yielding a summary score ranging from 17 to 85. Following other Iraq deployment studies, Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10,Reference Hotopf, Hull, Fear, Browne, Horn and Iversen23,Reference Smith, Ryan, Wingard, Slymen, Sallis and Kritz–Silverstein24 PTSD screening ‘cases’ required DSM-IV-TR 25 symptom congruency and a PCL-C cut-off score of >50. Depression symptom severity was measured at post-deployment with the Center for Epidemiological Studies Depression Scale (CES-D) (9-item version), Reference Santor and Coyne26 yielding a summary score ranging from 0 to 9. Depression screening ‘caseness’ was established using validated cut-off values. Reference Santor and Coyne26
The NDHS neuropsychological battery Reference Vasterling, Proctor, Amoroso, Kane, Heeren and White18 was designed to optimise sensitivity to more general potential deployment exposures (for example neurotoxicants, stress). This report includes NDHS measures judged to be of greatest relevance to diffuse brain injuries, including computer-assisted and interactive paper-and-pencil measures of sustained attention, executive functioning, inhibition, reaction time speed, learning, memory and cognitive efficiency (online Table DS1). All scores were free of subjective judgement except for visual reproductions, which was scored according to set criteria. Reliability ratings performed on 10% of randomly selected drawings by a second rater masked to unit and deployment status indicated high interrater reliability (interclass correlations 0.75–0.95).
Physical and cognitive health-related functioning was measured with the Veterans RAND 12-item Health Survey (VR-12) Reference Selim, Rogers, Fleishman, Qian, Fincke and Rothendler27 physical health component score and the 4-item version of the Medical Outcomes Study, Cognitive Functioning (MOS-CF) Reference Stewart, Ware, Sherbourne, Wells, Stewart and Ware28 scale respectively. Summary scores are standardised for both measures, yielding a range of 0–100 for each measure.
Statistical analyses
Data were analysed using SPSS v.16 on Windows XP. Missing values for specific items on psychometric questionnaires (<3% of participants) were replaced according to methods outlined by Selim and colleagues for the VR-12 Reference Selim, Rogers, Fleishman, Qian, Fincke and Rothendler27 and, for other measures, by the mean value of the individual's completed items for that measure. If <50% of the items on a measure were completed, summary scores were not computed, and we instead substituted the grand mean. Data substitutions within the regression analyses were infrequent (an average of 0.8% of the sample with missing data requiring a substitution per outcome variable). When data distributions departed significantly from normal, raw scores were normalised via logarithmic transformation.
Differences in pre-deployment characteristics between participants completing both pre- and post-deployment assessments v. those completing only the pre-deployment assessment, and differences in sample characteristics between participants reporting inter-session head injury with loss of consciousness (TBI+) and those not reporting inter-session head injury with loss of consciousness (TBI–) were examined via t-test or chi-squared, as appropriate.
Hierarchical linear regression was used to examine associations of inter-session TBI, PTSD (Model 1) and depression (Model 2) with neuropsychological performances and self-reported health-related functioning. This method allows evaluation of the independent associations of key predictive variables with outcomes, adjusting for the influence of other variables entered into the equation. The scores for PCL-C and CES-D were entered separately within each model because of their high collinearity. To account for baseline functioning, the pre-deployment value of each outcome measure was entered as a covariate in each model, creating a residualised index of longitudinal change. Other covariates included pre-deployment age and education, average number of alcohol drinks per week for the previous month at post-deployment assessment, duration of the pre- to post-deployment assessment interval (Step 1). Following entry of covariates, TBI status (TBI+, TBI–) was entered in the model (Step 2). Post-deployment PCL-C or CES-D summary scores (Models 1 and 2 respectively) were entered as Step 3. Finally, the interaction between TBI status and post-deployment PCL-C or CES-D summary scores (Models 1 and 2 respectively) was entered (Step 4). To account for multiple comparisons, we applied Bonferroni corrections within each outcome variable class (neuropsychological performance, health-related functioning). We applied Bonferroni corrections by modifying the value of P that is required for statistical significance. This allows P-values to remain unadjusted. Therefore, P-values presented in the tables and text are unadjusted. Following application of Bonferroni corrections, an unadjusted P<0.004 (0.05/12 variables) is required for significance for neuropsychological variables and an unadjusted P<0.025 (0.05/2 variables) is required for significance for health-related functioning variables.
To assess the influence of TBI-related variables, partial correlations were conducted examining associations between residualised outcomes measures (shared variance from pre-deployment values of the outcome measure removed) and: (a) report of prior v. no prior TBI with loss of consciousness at Time 1; and (b) time since the most significant inter-session TBI. Because a minority of participants reported >30 min loss of consciousness, >24 h post-traumatic amnesia or multiple inter-session TBIs, we were not able to examine associations of length of loss of consciousness, post-traumatic amnesia and presence of multiple inter-session TBIs with outcomes. Significance levels for partial correlations were Bonferroni-adjusted.
Results
Sample characteristics
The final sample (online Table DS2) reflected the Operation Iraqi Freedom-deployed US Army population at the time of the study, although women and commissioned officers were under-represented. At pre-deployment assessment, 0.2% had previous overseas operational deployment since 2001 to Iraq, Afghanistan or Kuwait. At post-deployment, 84 participants (11.1%) screened positive for PTSD, 135 (17.8%) screened positive for depression and 68 (9.0%) reported experiencing head injury with loss of consciousness (TBI) since their pre-deployment assessment, with 53 (7.0% of all participants) reporting TBI during the actual deployment. Of the 15 participants with non-deployment interassessment TBI, 7 reported a TBI after the first study session but prior to deployment, 4 reported a TBI after return from deployment and the timing of 4 could not be determined in relation to deployment. As compared with TBI–participants (n = 692), TBI+ participants (n = 68) were less likely to be women, and more likely to have reported a lifetime history of at least one pre-deployment head injury with >15 min loss of consciousness, screen positive for PTSD at pre-deployment, screen positive for depression at post-deployment and report higher levels of combat exposure during deployment and more severe post-deployment PTSD and depression symptoms. The injuries of the majority of TBI+ participants would be classified as mild TBI, 86.7% (n = 59) reporting <30 min loss of consciousness and 91.2% (n = 62) reporting <24 h post-traumatic amnesia.
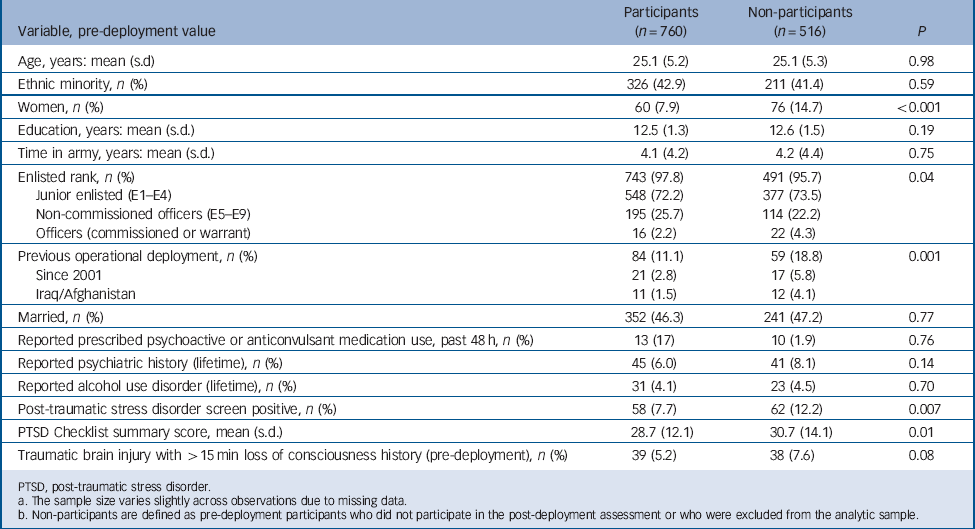
Among soldiers who underwent pre-deployment assessment, those in the final post-deployment analytic sample did not differ from post-deployment non-participants and those excluded from the analytic sample on most demographic variables, but post-deployment participants were less likely to be officers, women, and have previous deployment experience. Additionally, at pre-deployment, post-deployment participants were less likely to screen positive for PTSD and reported less severe PTSD symptoms (Table 1).
Associations of TBI, PTSD and depression with neurocognitive and functional outcomes
Hierarchical regression analyses revealed that inter-session TBI, even prior to adjustment for PTSD and depression symptoms, was not significantly associated with neuropsychological performances. In contrast, PCL-C scores and CES-D scores adjusted for TBI were significantly and negatively correlated with simple reaction time throughput, and code substitution learning and delayed recall throughput scores (online Table DS3), indicating that more severe post-deployment PTSD and depression symptomatology was associated with pre- to post-deployment decrements in simple reaction time efficiency and efficiency in learning and subsequently recalling digit–symbol pairs. Trends that approached but did not reach statistical significance following Bonferroni adjustment included negative correlations between PCL-C scores and visual reproductions, immediate recall (standardised B = –0.09, P = 0.005), a measure of short-term visual memory, and between CES-D scores and verbal paired associates, learning (standardised B = –0.08, P = 0.005), a measure of verbal–auditory learning.
Regarding subjective functional outcomes, inter-session TBI was significantly and negatively correlated with VR-12 scores, both before and after adjustment for PCL-C and CES-D scores (online Table DS3), indicating that TBI was associated with decrements in self-reported health-related functioning, even after adjustment for PTSD and depression symptom severity. Results failed to reveal a significant relationship between TBI and MOS-CF scores. After adjustment for TBI, PCL and CES-D scores were significantly and negatively correlated with VR-12 and MOS-CF scores, indicating that PTSD and depression severity were also associated with decrements in both general self-reported health-related functioning and self-reported cognitive-related functioning. There were no significant interactions between either TBI and PCL-C scores or TBI and CES-D scores for any outcome measure.
TABLE 1 Comparison of post-deployment participants with post-deployment non-participants on pre-deployment characteristicsFootnote a , Footnote b
| Variable, pre-deployment value | Participants (n = 760) |
Non-participants (n = 516) |
P |
|---|---|---|---|
| Age, years: mean (s.d) | 25.1 (5.2) | 25.1 (5.3) | 0.98 |
| Ethnic minority, n (%) | 326 (42.9) | 211 (41.4) | 0.59 |
| Women, n (%) | 60 (7.9) | 76 (14.7) | <0.001 |
| Education, years: mean (s.d.) | 12.5 (1.3) | 12.6 (1.5) | 0.19 |
| Time in army, years: mean (s.d.) | 4.1 (4.2) | 4.2 (4.4) | 0.75 |
| Enlisted rank, n (%) | 743 (97.8) | 491 (95.7) | 0.04 |
| Junior enlisted (E1–E4) | 548 (72.2) | 377 (73.5) | |
| Non-commissioned officers (E5–E9) | 195 (25.7) | 114 (22.2) | |
| Officers (commissioned or warrant) | 16 (2.2) | 22 (4.3) | |
| Previous operational deployment, n (%) | 84 (11.1) | 59 (18.8) | 0.001 |
| Since 2001 | 21 (2.8) | 17 (5.8) | |
| Iraq/Afghanistan | 11 (1.5) | 12 (4.1) | |
| Married, n (%) | 352 (46.3) | 241 (47.2) | 0.77 |
| Reported prescribed psychoactive or anticonvulsant medication use, past 48 h, n (%) | 13 (17) | 10 (1.9) | 0.76 |
| Reported psychiatric history (lifetime), n (%) | 45 (6.0) | 41 (8.1) | 0.14 |
| Reported alcohol use disorder (lifetime), n (%) | 31 (4.1) | 23 (4.5) | 0.70 |
| Post-traumatic stress disorder screen positive, n (%) | 58 (7.7) | 62 (12.2) | 0.007 |
| PTSD Checklist summary score, mean (s.d.) | 28.7 (12.1) | 30.7 (14.1) | 0.01 |
| Traumatic brain injury with >15 min loss of consciousness history (pre-deployment), n (%) | 39 (5.2) | 38 (7.6) | 0.08 |
PTSD, post-traumatic stress disorder.
a The sample size varies slightly across observations due to missing data.
b Non-participants are defined as pre-deployment participants who did not participate in the post-deployment assessment or who were excluded from the analytic sample.
Post hoc analyses repeating the hierarchical regressions without the 15 participants who reported inter-session TBI outside of the deployment did not alter the overall pattern of results. Post hoc analyses repeating the hierarchical regression procedures using dichotomous (less statistically sensitive) screening measures of PTSD and depression based on PCL-C and CES-D cut-points likewise did not alter the general pattern of results, although associations of PTSD with code substitution learning throughput (standardised B = –0.06, P = 0.01), and associations of depression with VR-12 (standardised B = –0.06, P = 0.07), simple reaction time throughput (standardised B = –0.03, P = 0.43), code substitution learning throughput (standardised B = –0.05, P = 0.05), and code substitution delay throughput (standardised B = –0.06, P = 0.02) no longer reached the Bonferroni-adjusted level of significance. The association of depression with visual reproductions immediate recall, previously a non-significant trend using the continuous CES-D summary score, reached statistical significance (standardised B = –0.09, P = 0.003) using the dichotomous depression index.
Associations of TBI-related variables with outcome measures
There were no significant associations between time since index TBI or pre-deployment TBI history and neuropsychological and functional outcomes.
Discussion
To our knowledge, this is the first published study of the post-acute outcomes of deployment-related TBI to capture pre-deployment levels of relevant outcome variables, including both objective neuropsychological performances and subjective complaints. Our findings revealed that self-reported deployment TBI, even prior to taking into account PTSD and depression symptoms, was not associated with performance decrements on any of 12 neurocognitive measure or on a subjective measure of the functional impact of cognitive impairment. The predominantly mild TBI in this sample was related only to decrements in subjective health-related functioning, which remained significant after adjustment for psychiatric symptoms. In contrast, PTSD and depression were associated with both neuropsychological performance decrements and subjective indices of cognitive and somatic health-related functional impairment.
Associations of deployment TBI with neuropsychological and functional outcomes
The general pattern of findings indicating that both performance-based and subjective outcomes were more strongly associated with psychiatric variables, as compared with deployment TBI, is consistent with previous research examining the relationship between self-reported post-concussive symptoms and mild TBI in returning service members. Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10,Reference Vanderploeg, Belanger and Curtiss29–Reference Schneiderman, Braver and Kang31 With rare exception, Reference Levin, Wilde, Troyanskaya, Petersen, Scheibel and Newsome6 studies of war-zone veterans have suggested that neuropsychological deficits do not commonly persist following mild TBI. Reference Brenner, Terrio, Homaifar, Gutierrez, Staves and Harwood7,Reference Ivins, Kane and Schwab8 Our findings are also consistent with prior civilian research suggesting that objective, neurocognitive performance deficits resolve after the acute phase of injury recovery in most individuals with milder TBIs, Reference Dikmen, Corrigan, Levin, Machamer, Stiers and Weisskopf1 whereas subjective health-related dysfunction may persist in a larger subset of individuals with mild TBI. Reference Dikmen, Machamer, Fann and Temkin3
Although participants reporting deployment TBI in our sample reported injury characteristics suggestive of mild TBI, a small subgroup (<13% of all participants reporting TBI) reported injury characteristics suggestive of greater than mild TBI, increasing the probability of associations between TBI status and outcomes. It is likely that soldiers with the most disabling TBI would not have been available for testing at our post-deployment sessions because of being in hospital or because of early medical discharge. Nonetheless, the absence of such associations between TBI status and neuropsychological outcomes is all the more striking because we did not limit the sample to those unambiguously categorised as ‘mild’ TBI. Prior research has demonstrated significant relationships between mild deployment TBI and subjective outcome measures prior to adjustment for psychiatric factors, but has also found that most of these associations were no longer significant following adjustment for depression and/or PTSD. Reference Rona, Jones, Fear, Hull, Murphy and Machell9,Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10 Because TBI may contribute to PTSD and depression symptoms, adjusting TBI analyses by removing shared variance attributable to PTSD and depression could lead to an overly conservative estimate of the influence of TBI on outcomes. Our results, however, indicated that predominantly mild deployment-related TBI was not significantly associated with objective neuropsychological performances even prior to adjustment for PTSD and depression symptoms, suggesting that findings could not be explained by statistical artifact.
It is also noteworthy that there was no meaningful pattern of association between time since most significant TBI, prior TBI or single v. multiple inter-session TBIs with outcomes. Likewise, removal of the few participants with non-deployment TBI between the study assessments did not alter the pattern of results.
Given the lack of significant association between TBI status and objective neuropsychological performances, it is not surprising that TBIs at the milder end of the severity spectrum were not significantly associated with difficulties managing daily activities due to cognitive impairment. However, the relatively mild TBI in our sample was associated with decrements in somatic health-related functioning that could not be explained by psychiatric symptoms or pre-TBI functioning. We did not control for non-brain physical injuries. In UK veterans, report of multiple physical symptoms most strongly accounted for the relationship between mild TBI and post-concussive symptoms. Reference Rona, Jones, Fear, Hull, Murphy and Machell9 Thus, the extent to which functional impairment in our sample was related specifically to TBI or more generally to either physical injury or self-report of physical symptoms is unclear. Notably, however, Hoge et al Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10 found that mild TBI, especially when associated with loss of consciousness, was associated with poorer outcomes as compared with non-TBI injuries.
In contrast to TBI status, PTSD and depression were associated with adverse post-deployment neuropsychological and functional somatic and cognitive health outcomes, which cannot be attributed to TBI incurred between pre- and post-deployment assessment or to pre-morbid functioning. The pattern of association held regardless of whether we examined the full continuum of psychiatric symptoms or dichotomous (yes/no) PTSD and depression variables reflecting clinically significant symptom levels. Associations between psychiatric symptoms and neuropsychological deficits are not surprising, given well-documented findings from cross-sectional studies of mild neuropsychological impairment in both PTSD Reference Brewin, Kleiner, Vasterling and Field32 and depression. Reference Douglas and Porter33 Such deficits are believed to be attributable in part to neurobiological abnormalities associated with the disorders. Reference Southwick, Rasmusson, Barron, Arnsten, Vasterling and Brewin34
Prevalence of deployment TBI and comorbid psychiatric disorders
We found that 9% of the sample reported a head injury associated with loss of consciousness between pre- and post-deployment assessments. Although the majority (79%) of these injuries occurred during deployment, it is noteworthy that almost a quarter (21%) transpired during the short interval between the pre- and post-deployment assessments but outside the context of deployment. Using a more stringent definition requiring 15 min loss of consciousness, at pre-deployment, an additional 5% of the sample reported experiencing a TBI prior to deployment. Taken together, these figures suggest that deployment is by no means the only source of TBI for military personnel. This is not surprising, given that over 1.1 million people per year in the USA sustain a TBI for which they receive medical attention, Reference Corrigan, Selassie and Orman35 with mild TBIs likely to be more prevalent because many individuals incurring a mild TBI are less likely to have received medical attention for the injury. Of relevance to service members who are deployed more than once to a war-zone, it is also noteworthy that participants reporting a head injury with >15 min loss of consciousness at pre-deployment assessment were more likely to report a head injury with associated loss of consciousness between pre- and post-deployment assessment, raising the question of whether prior TBI increases risk of subsequent TBI. This finding, however, should be viewed cautiously, given the manner in which we queried for pre-deployment head injury (questionnaire only and without a continuous index of severity) and that we did not measure potential confounding or mechanistic factors (such as risk-taking behaviour, response biases).
The prevalence of TBI with loss of consciousness in our sample was significantly higher than that reported in a UK sample (0.7%) Reference Rona, Jones, Fear, Hull, Murphy and Machell9 and somewhat higher than that reported in a sample of US Army soldiers (4.9%). Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10 Our higher rates may reflect differences in the specific experiences of each cohort and/or differences in how our data were obtained (interviews with examiners available to explain terms such as loss of consciousness v. written survey). As in other studies, Reference Rona, Jones, Fear, Hull, Murphy and Machell9 TBI in our sample was predominantly mild and associated with higher levels of combat, which would presumably be associated with greater risk of injury. Consistent with the UK sample, PTSD at pre-deployment was associated with increased risk of reporting a TBI between pre- and post-deployment.
At post-deployment, of those participants reporting head injury with loss of consciousness, approximately 18% screened positive for PTSD, and 31% screened positive for depression. The comorbidity of milder TBI and psychiatric disorders among service members returning from deployment is striking both in our sample and in previous research. Reference Rona, Jones, Fear, Hull, Murphy and Machell9–Reference Tanielian and Jaycox11 Collectively, these findings highlight the importance of directing clinical attention to both the psychiatric and physical injuries of returning service members and military veterans. Our findings further warn against assuming that neuropsychological deficits among returning service members with self-reported mild TBI are necessarily attributable to TBI, especially when the injury is at the milder end of severity range and is post-acute. Nonetheless, mild TBI is an independent risk factor for functional health impairment suggesting that, even when not resulting in chronic neuropsychological dysfunction, the health-related concerns of individuals with TBI of all severity levels warrant attention.
Limitations
Our designation of TBI relied on self-report, which renders report of exposures vulnerable to reporting biases. Reference Wessely, Unwin, Hotopf, Hull, Ismail and Nicolaou36 The lack of objective verification reflects the absence of consistent war-zone documentation of mild TBI, especially during the early stages of Operation Iraqi Freedom. Interestingly, at the time our post-deployment data were obtained (in 2005), awareness of deployment-related TBI, including injuries at the milder end of the severity spectrum, was increasing among military healthcare providers, but there was not as yet significant media coverage or widespread knowledge of concerns about TBI among deploying service members. In addition, we did not ask participants about ‘TBI’, ‘traumatic brain injury’, or ‘concussion’ but instead asked about whether participants received any injury to their head and whether that injury resulted in loss of consciousness. Thus, it is unlikely that reporting biases stemming specifically from over concern about ‘TBI’ served as a major reason that head injury with loss of consciousness was endorsed at higher rates in our sample.
We adopted a clinically relevant approach to defining TBI, requiring at least momentary loss of consciousness. Thus, we did not capture TBI with milder alterations of consciousness in the absence of outright loss of consciousness. It is possible that group differences in neuropsychological outcomes were attenuated because participants in the no-TBI group had experienced head injuries with mild alterations of consciousness that nonetheless resulted in enduring neuropsychological impairment. Prior research, however, suggests little, if any, association between mild TBI without loss of consciousness and post-acute outcomes, Reference Hoge, McGurk, Thomas, Cox, Engel and Castro10,Reference Luethcke, Bryan, Morrow and Isler21 making this an unlikely explanation. Further, reliable measurement of alteration of consciousness in war-zones is suspect given that psychological reactions (such as feeling stunned) could be misinterpreted as neurologically based altered consciousness.
Our neuropsychological battery, although containing multiple elements of relevance to TBI, was also not designed specifically around TBI and therefore may not have been optimally sensitive to milder TBI. As mentioned earlier, we did not control for more general physical injury, which may influence some outcomes. Finally, the sample does not generalise to the full duration of Operation Iraqi Freedom, US military branches other than the army, activated reservists, to individuals with more severe levels of brain injury or to international forces.
Implications
The limitations in our study are offset by the rare prospective design and inclusion of objective measures in a relatively large sample. Findings draw attention to the complex comorbidity of TBI and psychiatric symptoms and provide support that milder deployment-related TBI has limited lasting neuropsychological consequences in contrast to PTSD and depression, which are associated with more enduring cognitive compromise. Our data do not directly address the utility of pre- and post-deployment TBI screenings, as such screenings are intended to target functional impairments more broadly than the primary focus of this study, which was neuropsychological performance. Our findings nonetheless highlight the potential utility of routine neuropsychological surveillance, given that pre-deployment data can be helpful in establishing whether or not post-deployment neuropsychological impairment reflects long-standing weaknesses or reflects a new decline across deployments. The pattern of associations in our findings, however, suggests that there may be multiple factors, including psychiatric status, that contribute to any observed neuropsychological decrements. Our results further suggest that, as policy makers and clinicians consider appropriate healthcare strategies for returning veterans who report mild TBI, attention to the management of psychiatric symptoms, including PTSD and depression, will be paramount. It may be that swift and effective psychiatric and psychosocial intervention may have broad effects by not only alleviating emotional distress but by also providing an important secondary benefit in terms of reversing deployment-related neuropsychological decrements.
Funding
Funding was provided by the US Department of Defense CDMRP (W81XWH-08-2-0035), US Army Medical Research and Materiel Command (DAMD 17-03-0020); and US Veterans Affairs Clinical Sciences Research and Development. The primary funding organisation had no role in the scientific aspects of the study or the preparation of the manuscript. The manuscript underwent scientific and administrative review within the US Army Research Institute for Environmental Medicine and US Army Medical Research and Materiel Command. The content of this article does not necessarily reflect the position or policy of the US government, and no official endorsement should be inferred.
Acknowledgements
We are grateful for the input provided by Drs Brian Marx, Laura Grande and Frank Castro. We also thank the skilled examiner team involved in data collection. The assistance of military leaders and unit level facilitators was invaluable. Finally, we thank the soldiers for volunteering their time to participate in the study and for their military service more generally.







eLetters
No eLetters have been published for this article.