The morale of the mental health workforce is important in several ways. First, this large workforce is exposed to substantial stresses and, at times, threats; Reference Reid, Johnson, Morant, Kuipers, Szmukler and Thornicroft1 ensuring staff well-being is thus a key challenge for employers. Second, high levels of staff sickness in the UK National Health Service (NHS) result in a large economic burden on the nation. 2 Third, there is some evidence suggesting links between health staff well-being and patient experiences and outcomes. 2 Finally, staff attitudes are a key factor facilitating or impeding implementation of new service initiatives. Reference Tansella and Thornicroft3 Implementation is particularly relevant to psychiatric in-patient care settings (a central focus of our study), as wards in the UK have been criticised for being threatening and unsafe environments in which therapeutic relationships are impoverished and treatment limited. This has resulted in a series of initiatives aimed at service improvement, which are unlikely to succeed unless a skilled and motivated workforce is recruited and retained. Despite its importance, research into staff morale remains limited, with a lack of large multisite studies that encompass all the main mental health professions and include subspecialties other than services for adults of working age. Reference Paris and Hoge4,Reference Richards, Bee, Barkham, Gilbody, Cahill and Glanville5 Our study aimed to address this need for large-scale evidence on morale in the mental health workforce. Like previous authors, Reference Reininghaus and Priebe6 we use morale as a general term encompassing the main aspects of work-related well-being and satisfaction and engagement with work. Specific objectives were:
-
(a) to describe staff well-being and satisfaction in a large multicentre sample, identifying whether there are subspecialties or professions in which morale problems are especially acutely felt or, conversely, morale levels are exemplary;
-
(b) to investigate the interrelationships of the measures of well-being and satisfaction used, and whether a smaller number of higher-order components can be derived from them;
-
(c) to explore how far variations in morale between settings and professions may be accounted for by job characteristics.
Method
Nineteen mental health trusts in England, each delivering a broad range of mental health services to a catchment area, were the study setting, drawn from the regions surrounding the four main participating universities: University College London and the universities of Warwick, Sheffield and Bristol. Area demographic and geographical characteristics varied widely.
Sample and procedures
The in-patient care sample was recruited on 100 wards. Half were acute general wards serving adults of working age resident within a specific catchment area; the remainder were divided between wards providing care for older people, rehabilitation wards (providing longer-term but time-limited care for severely ill people with major difficulties functioning in the community), forensic wards (caring for mentally ill offenders usually referred by the criminal justice system), child and adolescent mental health wards (for those under 18 years old) and psychiatric intensive care units (PICUs) (for patients too difficult to manage on a general ward). Eighteen community mental health teams (CMHTs) and 18 crisis resolution teams (CRTs) (providing rapid assessment and short-term intensive home treatment in a crisis) formed the community sample.
Researchers approached all frontline clinical staff in the participating teams and their immediate managers, and invited them to complete our questionnaire. Assurances of confidentiality were provided and reminders and tokens of gratitude such as fruit and biscuits distributed. Multicentre ethical approval was obtained. Data collection commenced in late 2007 and was concluded in 2009.
Measures
Morale
Staff well-being and attitudes to work were assessed with the following five measures. First, burnout was rated with the Maslach Burnout Inventory, which yields three dimensions of burnout: emotional exhaustion, assessing the extent to which participants feel overburdened by their work; cynicism (a clearer description of this subscale than the original designation of ‘depersonalisation’ Reference Lasalvia, Bonetto, Bertani, Bissoli, Cristofalo and Marella7 ), assessing how far they feel emotionally hardened and indifferent to patients; and personal accomplishment, measuring whether they feel they can work with patients effectively. Reference Maslach and Jackson8 The second measure was the Job-related Affective Well-being Scale, which in the version used generates two partially independent subscales: Reference Warr9 on the anxiety–contentment scale high scores represent predominance of contentment over anxiety and low scores the reverse, whereas on the depression–enthusiasm scale enthusiasm predominates at high scores and depression at low scores. Third, to assess job satisfaction we used a combination of items from the 2004 Workplace Employment Relations Survey and the NHS Staff Survey to cover the aspects of satisfaction that we wished to include; Reference Kersley, Alpin and Forth10,11 this generated several satisfaction subscores (see online Table DS2). Fourth, overall psychological health was rated with the 12-item version of the General Health Questionnaire (GHQ-12), Reference Goldberg and Williams12 covering depression, anxiety, suicidal ideas, happiness and sleep disturbance; using the Likert version each item is scored from 0 to 3, and a total score of 12 or more out of 36 is the threshold for ‘caseness’, indicating potential morbidity. Finally, the Job Involvement Scale, which defines the degree of an individual's psychological identification with their work, was used as an indicator of motivation; Reference Lodahl and Kejner13 we used a five-item measure. Reference Tummers, Janssen, Landeweerd and Houkes14
Demographic and occupational details
Structured questions elicited the participants’ sociodemographic details and profession, length of service in mental health services and on their current ward, and seniority.
Job characteristics
Perceived job characteristics measured in the study originated from Karasek's ‘demand–control’ model of work-related strain, Reference Karasek15 subsequently extended to include ‘support’. Reference Johansson, Johnson and Hall16 Central to occupational psychology for the past two decades, this model has been widely replicated, although not prior to our study in a multidisciplinary sample of mental health staff. Reference Wood, Stride, Threapleton, Wearn, Nolan and Osborn17 Job strain is conceptualised as resulting from the triad of high demands, low decisional latitude (autonomy) and low support. Good evidence also supports an extension of this – the idea that a combination of high demands, high autonomy and high support results in good motivation and job satisfaction. Reference De Jonge and Kompier18 We measured demands and control using questions developed by Haynes et al for health staff, all rated on a five-point scale. Reference Haynes, Wall, Bolden and Stride19 Seven items related to the extent of demands made by jobs, including whether these exceeded available time and resources, conflicted with one another or made it impossible to follow best practice. Five items related to control: how much autonomy respondents had in deciding how to do their work. Three items in the same format measured support (including willingness to listen and helpfulness) from immediate managers, and four items measured support from colleagues.
Statistical analysis
We first estimated unadjusted mean morale indicators by service type and profession and tested for differences using analysis of variance. We originally planned to test the hypothesis that in-patient unit staff would have worse morale than those working in the community; this was not pursued, because descriptive statistics revealed large differences between hospital specialties. To ascertain relationships between indicators of morale we examined pairwise Pearson's correlations between all the subscales listed above. We then used principal components analysis to explore whether we could obtain plausible components onto which several indicators loaded to be used in further analyses. We then examined the associations between the components of staff morale and service type and profession, adjusted for other demographic and occupational variables. Mixed effects multilevel regression was used so that we could simultaneously model effects at both individual and service level, taking account of the non-independence of observations at each level. Reference Snijders and Bosker20 Multilevel models were then derived with each of the morale components as dependent variables: individuals were nested within services. Initially, profession and service type were included along with the demographic and job-related variables shown in Table 1. We then added job demands, support and control variables to the multilevel models obtained, assessing how far significant relationships between morale and service type and profession persisted with these variables included.
Less than 5% of the data were missing (between 13 and 144 cases per variable), but exclusion of all cases with missing data would have substantially reduced the sample. We therefore used multiple imputation, which fills in missing values based on values of other variables and a ‘missing at random’ assumption. Multiple imputation acknowledges uncertainty about the missing values by creating several imputed data-sets, in this case five following standard guidance that the number of imputed data-sets should exceed the overall proportion of missing data. Reference White, Royston and Wood21 The ice command in Stata version 10 for Windows was used to generate imputed data-sets and the mim commands to combine them in our multilevel regression analyses. Reference Royston22
Results
One hundred wards in 19 mental health trusts provided the in-patient staff sample: 50 acute general wards, 10 child and adolescent mental health service (CAMHS), 9 rehabilitation, 9 older people's, 12 forensic and 10 PICU wards. In the community we recruited 18 CMHTs and 18 CRTs. A total of 3545 questionnaires were distributed, of which 2258 valid responses were returned, a 64% response rate. At trust level the response rate varied from 52% to 72%, median 60%. Ward response rates ranged between 22% and 100%, median 62%.
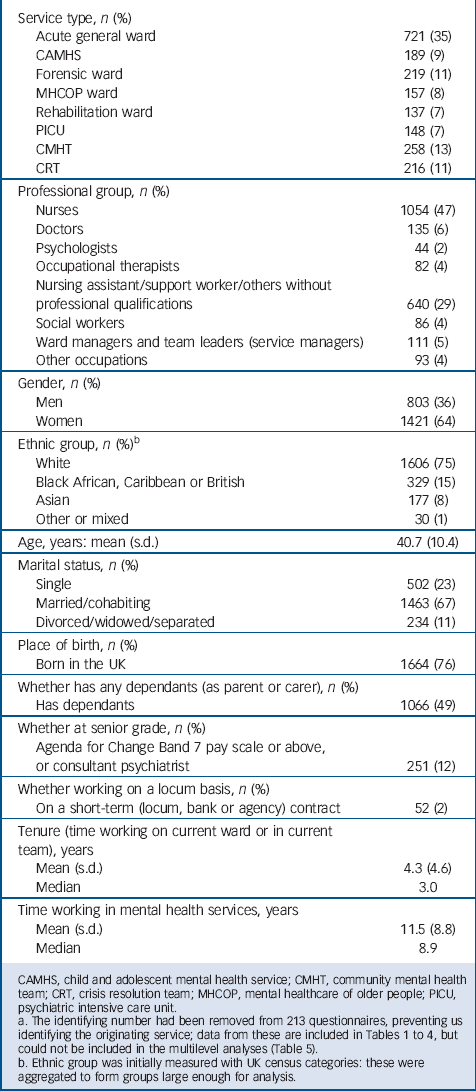
Just over a third of respondents were men, three-quarters were from a White ethnic background and the mean age was 40.7 years (Table 1). Around half the participants were nurses and just over a quarter were nursing assistants, healthcare assistants or others without a relevant professional qualification. All other main mental health professions were represented in smaller groups. Five per cent were ward or community team managers, subsequently referred to as service managers. Temporary staff who had worked on the ward in a locum, bank or agency capacity for at least a month were encouraged to participate, but constituted only 2% of the sample. Staff on the national pay scales that reflect substantial managerial responsibilities (NHS Agenda for Change pay scales Band 7) and consultant psychiatrists were classified as senior: 12% met these criteria. Mean tenure in current service was 4.3 years and mean total service in mental healthcare was just under 12 years.
TABLE 1 Sample characteristics (n = 2258)Footnote a
| Service type, n (%) | |
| Acute general ward | 721 (35) |
| CAMHS | 189 (9) |
| Forensic ward | 219 (11) |
| MHCOP ward | 157 (8) |
| Rehabilitation ward | 137 (7) |
| PICU | 148 (7) |
| CMHT | 258 (13) |
| CRT | 216 (11) |
| Professional group, n (%) | |
| Nurses | 1054 (47) |
| Doctors | 135 (6) |
| Psychologists | 44 (2) |
| Occupational therapists | 82 (4) |
| Nursing assistant/support worker/others without professional qualifications | 640 (29) |
| Social workers | 86 (4) |
| Ward managers and team leaders (service managers) | 111 (5) |
| Other occupations | 93 (4) |
| Gender, n (%) | |
| Men | 803 (36) |
| Women | 1421 (64) |
| Ethnic group, n (%)Footnote b | |
| White | 1606 (75) |
| Black African, Caribbean or British | 329 (15) |
| Asian | 177 (8) |
| Other or mixed | 30 (1) |
| Age, years: mean (s.d.) | 40.7 (10.4) |
| Marital status, n (%) | |
| Single | 502 (23) |
| Married/cohabiting | 1463 (67) |
| Divorced/widowed/separated | 234 (11) |
| Place of birth, n (%) | |
| Born in the UK | 1664 (76) |
| Whether has any dependants (as parent or carer), n (%) | |
| Has dependants | 1066 (49) |
| Whether at senior grade, n (%) | |
| Agenda for Change Band 7 pay scale or above, or consultant psychiatrist | 251 (12) |
| Whether working on a locum basis, n (%) | |
| On a short-term (locum, bank or agency) contract | 52 (2) |
| Tenure (time working on current ward or in current team), years | |
| Mean (s.d.) | 4.3 (4.6) |
| Median | 3.0 |
| Time working in mental health services, years | |
| Mean (s.d.). | 5 (8.8) |
| Median | 8.9 |
CAMHS, child and adolescent mental health service; CMHT, community mental health team; CRT, crisis resolution team; MHCOP, mental healthcare of older people; PICU, psychiatric intensive care unit.
a The identifying number had been removed from 213 questionnaires, preventing us identifying the originating service; data from these are included in Tables 1 to 4, but could not be included in the multilevel analyses (Table 5).
b Ethnic group was initially measured with UK census categories: these were aggregated to form groups large enough for analysis.
Levels of morale by service type and profession
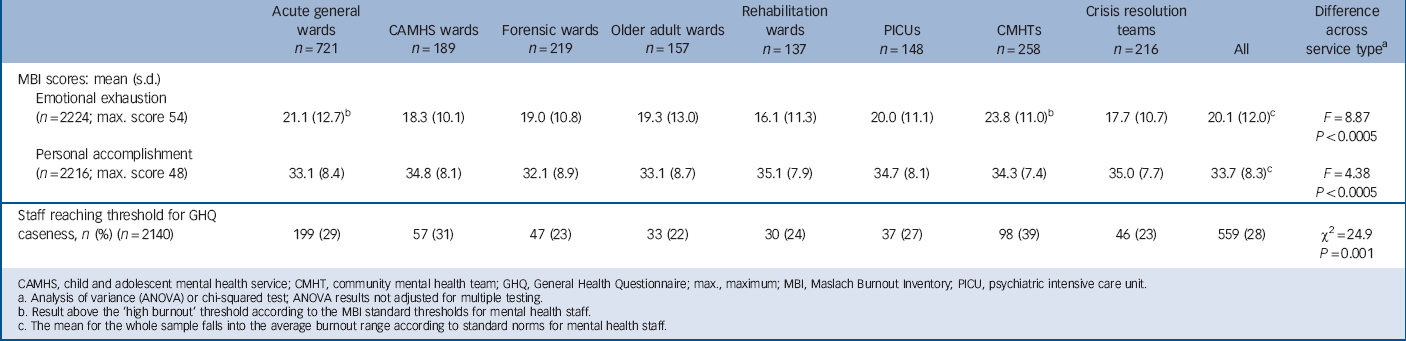
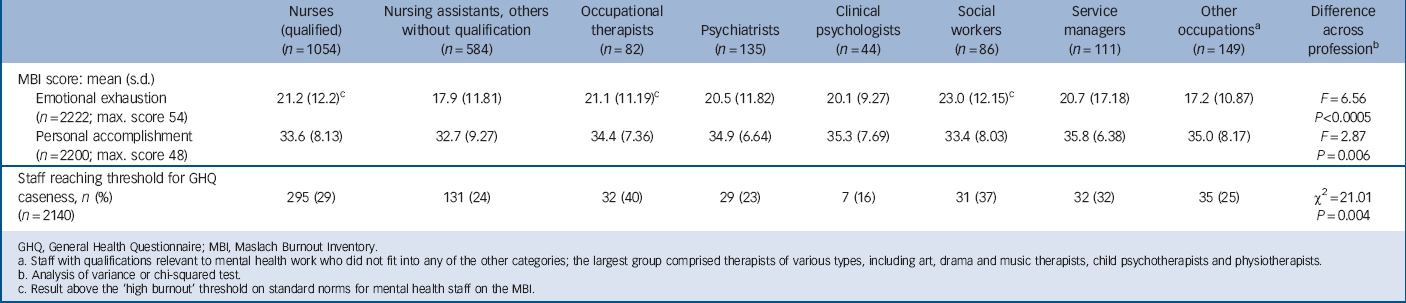
Tables 2 and 3 summarise levels of morale categorised by service type and by profession for three indicators frequently used in previous research: emotional exhaustion and personal accomplishment measured on the Maslach Burnout Inventory, and whether the GHQ caseness threshold was reached. All other measures are shown in the online supplement to this paper (Tables DS1–4). Mean scores for burnout were below the standard high burnout threshold for most groups. Reference Maslach and Jackson8 Exceptions for emotional exhaustion were acute general wards, with a mean just above the burnout threshold and 49% of staff reaching this level, and CMHTs with a mean almost 3 points above the threshold and 60% reaching the threshold. Among professions, the mean for nurses and occupational therapists just reached the high burnout threshold, and social workers had the highest mean, 2 points above the threshold. No group reached high burnout thresholds on cynicism or lack of personal accomplishment.
For other measures, most service types and professions had mean scores above 3.0 on the depression–enthusiasm and anxiety–contentment scales, indicating inclination towards contentment and enthusiasm (online Tables DS1, DS3). Exceptions just below this threshold for anxiety–contentment were CMHT staff and social workers. The proportion of staff reaching caseness levels on the GHQ ranged from 22% of older adult ward staff to 39% of CMHT staff. Staff were reasonably satisfied with most aspects of work, with means well above the 3.0 level indicating neutrality (online Tables DS2, DS4). The exception was satisfaction with pay – only psychiatrists and psychologists were satisfied overall. Scores for satisfaction with colleagues were especially high. Job involvement did not vary significantly level by service type (Table DS2), but more by profession (Table DS4), with psychiatrists and service managers reporting the highest and nurses and social workers the lowest job involvement. The overall mean was 2.52 and means for all groups fell below 3.0: most participants did not agree strongly with items identifying work as central to their lives.
Interrelationship of morale indicators and principal components analysis
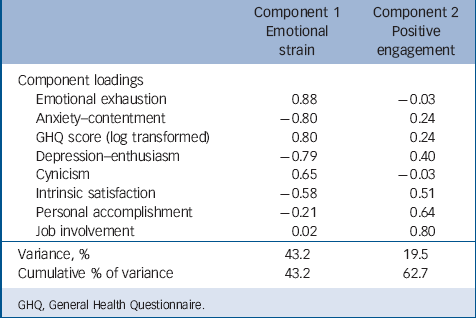
All the main morale indicators were highly significantly intercorrelated (online Table DS5), although the size of the correlations ranged from weak to fairly strong, with many in the medium range. Table 4 and online Fig. DS1 show results of a principal components analysis, exploring whether this large number of morale variables could be captured by a smaller number of components. With an eigenvalue threshold of 1.0 for retention of components and following varimax rotation, two components emerged. The first accounted for 43.2% of the variance, with loadings of more than 0.5 for all variables except personal accomplishment and job involvement. Loadings exceeded 0.7 for emotional exhaustion, GHQ-12 and the two job-related well-being variables. Thus, this component appeared to reflect emotional strain and/or distress and is subsequently referred to as the emotional strain component. The second component accounted for 19.5% of the variance: job involvement and personal accomplishment had the largest loadings, with substantial relationships also for intrinsic satisfaction and depression–enthusiasm, but not for other variables. This seemed to reflect how far staff members are engaged with and derive satisfaction from doing their work and is subsequently referred to as the positive engagement component. For further analyses, these components were scaled to the standard normal distribution so that mean differences reported below are measured in standard deviations.
Multiply adjusted analyses
Table 5 summarises and online Table DS6 shows in full the associations between emotional strain, positive engagement and service type and profession, derived from multilevel regression analyses and multiply adjusted for demographic and other job-related variables. The proportion of variance at the service rather than individual level was estimated as 3.9% for emotional strain and 4.3% for positive engagement. We initially also included healthcare trust as a higher level, but omitted it in the final analysis as the variance at trust level did not reach 1% for either component.
TABLE 2 Emotional exhaustion, personal accomplishment and General Health Questionnaire scores analysed by service
| Acute general wards n = 721 |
CAMHS wards n = 189 |
Forensic wards n = 219 |
Older
adult wards n = 157 |
Rehabilitation wards n = 137 |
PICUs n = 148 |
CMHTs n = 258 |
Crisis
resolution teams n = 216 |
All | Difference across service typeFootnote a |
|
|---|---|---|---|---|---|---|---|---|---|---|
| MBI scores: mean (s.d.) | ||||||||||
| Emotional exhaustion (n = 2224; max. score 54) | 21.1 (12.7)Footnote b | 18.3 (10.1) | 19.0 (10.8) | 19.3 (13.0) | 16.1 (11.3) | 20.0 (11.1) | 23.8 (11.0)Footnote b | 17.7 (10.7) | 20.1 (12.0)Footnote c | F = 8.87 P <0.0005 |
| Personal accomplishment (n = 2216; max. score 48) | 33.1 (8.4) | 34.8 (8.1) | 32.1 (8.9) | 33.1 (8.7) | 35.1 (7.9) | 34.7 (8.1) | 34.3 (7.4) | 35.0 (7.7) | 33.7 (8.3)Footnote c | F = 4.38 P < 0.0005 |
| Staff reaching threshold for GHQ caseness, n (%) (n = 2140) | 199 (29) | 57 (31) | 47 (23) | 33 (22) | 30 (24) | 37 (27) | 98 (39) | 46 (23) | 559 (28) | χ2=24.9 P = 0.001 |
CAMHS, child and adolescent mental health service; CMHT, community mental health team; GHQ, General Health Questionnaire; max., maximum; MBI, Maslach Burnout Inventory; PICU, psychiatric intensive care unit.
a Analysis of variance (ANOVA) or chi-squared test; ANOVA results not adjusted for multiple testing.
b Result above the ‘high burnout’ threshold according to the MBI standard thresholds for mental health staff.
c The mean for the whole sample falls into the average burnout range according to standard norms for mental health staff.
TABLE 3 Emotional exhaustion, personal accomplishment and General Health Questionnaire scores analysed by profession
| Nurses (qualified) (n = 1054) |
Nursing assistants, others without qualification (n = 584) |
Occupational therapists (n = 82) |
Psychiatrists (n = 135) |
Clinical psychologists (n = 44) |
Social workers (n = 86) |
Service managers (n = 111) |
Other occupationsFootnote a (n = 149) |
Difference across professionFootnote b |
|
|---|---|---|---|---|---|---|---|---|---|
| MBI score: mean (s.d.) | |||||||||
| Emotional exhaustion (n = 2222; max. score 54) | 21.2 (12.2)Footnote c | 17.9 (11.81) | 21.1 (11.19)Footnote c | 20.5 (11.82) | 20.1 (9.27) | 23.0 (12.15)Footnote c | 20.7 (17.18) | 17.2 (10.87) | F = 6.56 P<0.0005 |
| Personal accomplishment (n = 2200; max. score 48) | 33.6 (8.13) | 32.7 (9.27) | 34.4 (7.36) | 34.9 (6.64) | 35.3 (7.69) | 33.4 (8.03) | 35.8 (6.38) | 35.0 (8.17) | F = 2.87 P = 0.006 |
| Staff reaching threshold for GHQ caseness, n (%) (n = 2140) | 295 (29) | 131 (24) | 32 (40) | 29 (23) | 7 (16) | 31 (37) | 32 (32) | 35 (25) | χ2 = 21.01 P = 0.004 |
GHQ, General Health Questionnaire; MBI, Maslach Burnout Inventory.
a Staff with qualifications relevant to mental health work who did not fit into any of the other categories; the largest group comprised therapists of various types, including art, drama and music therapists, child psychotherapists and physiotherapists.
b Analysis of variance or chi-squared test.
c Result above the ‘high burnout’ threshold on standard norms for mental health staff on the MBI.
TABLE 4 Components obtained from morale indicators with principal components analysis with varimax rotation
| Component 1 Emotional strain |
Component 2 Positive engagement |
|
|---|---|---|
| Component loadings | ||
| Emotional exhaustion | 0.88 | –0.03 |
| Anxiety–contentment | –0.80 | 0.24 |
| GHQ score (log transformed) | 0.80 | 0.24 |
| Depression–enthusiasm | –0.79 | 0.40 |
| Cynicism | 0.65 | –0.03 |
| Intrinsic satisfaction | –0.58 | 0.51 |
| Personal accomplishment | –0.21 | 0.64 |
| Job involvement | 0.02 | 0.80 |
| Variance, % | 43.2 | 19.5 |
| Cumulative % of variance | 43.2 | 62.7 |
GHQ, General Health Questionnaire.
Variables associated with emotional strain
Emotional strain varied substantially by service type, with CAMHS, PICU, older people's, forensic and rehabilitation wards and CRTs all having significantly lower adjusted levels than acute general wards (P<0.05) and CMHTs having higher levels. The largest adjusted effect was for rehabilitation wards, 0.41 s.d. below acute general wards. Variations by profession were less marked: the only significant differences were for staff without professional qualifications and for the other occupations group, 0.2 s.d. and 0.21 s.d. respectively below nurses. Other differences (online Table DS6) were less strain among older staff, married or cohabiting staff and temporary staff. Emotional strain tended to be higher among staff with longer tenure in their current service and those with longer total service in mental healthcare.
TABLE 5 Adjusted associations between morale components and service type and profession
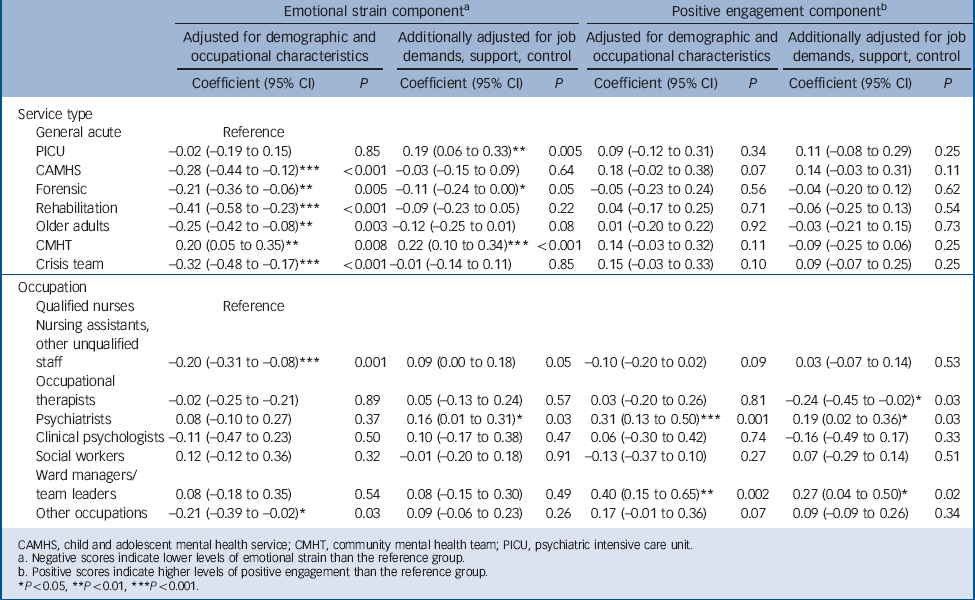
| Emotional strain componentFootnote a | Positive engagement componentFootnote b | |||||||
|---|---|---|---|---|---|---|---|---|
| Adjusted for
demographic and occupational characteristics |
Additionally adjusted
for job demands, support, control |
Adjusted for
demographic and occupational characteristics |
Additionally adjusted
for job demands, support, control |
|||||
| Coefficient (95% CI) | P | Coefficient (95% CI) | P | Coefficient (95% CI) | P | Coefficient (95% CI) | P | |
| Service type | ||||||||
| General acute | Reference | |||||||
| PICU | –0.02 (–0.19 to 0.15) | 0.85 | 0.19 (0.06 to 0.33)** | 0.005 | 0.09 (–0.12 to 0.31) | 0.34 | 0.11 (–0.08 to 0.29) | 0.25 |
| CAMHS | –0.28 (–0.44 to –0.12)*** | <0.001 | –0.03 (–0.15 to 0.09) | 0.64 | 0.18 (–0.02 to 0.38) | 0.07 | 0.14 (–0.03 to 0.31) | 0.11 |
| Forensic | –0.21 (–0.36 to –0.06)** | 0.005 | –0.11 (–0.24 to 0.00)Footnote * | 0.05 | –0.05 (–0.23 to 0.24) | 0.56 | –0.04 (–0.20 to 0.12) | 0.62 |
| Rehabilitation | –0.41 (–0.58 to –0.23)*** | <0.001 | –0.09 (–0.23 to 0.05) | 0.22 | 0.04 (–0.17 to 0.25) | 0.71 | –0.06 (–0.25 to 0.13) | 0.54 |
| Older adults | –0.25 (–0.42 to –0.08)** | 0.003 | –0.12 (–0.25 to 0.01) | 0.08 | 0.01 (–0.20 to 0.22) | 0.92 | –0.03 (–0.21 to 0.15) | 0.73 |
| CMHT | 0.20 (0.05 to 0.35)** | 0.008 | 0.22 (0.10 to 0.34)*** | <0.001 | 0.14 (–0.03 to 0.32) | 0.11 | –0.09 (–0.25 to 0.06) | 0.25 |
| Crisis team | –0.32 (–0.48 to –0.17)*** | <0.001 | –0.01 (–0.14 to 0.11) | 0.85 | 0.15 (–0.03 to 0.33) | 0.10 | 0.09 (–0.07 to 0.25) | 0.25 |
| Occupation | ||||||||
| Qualified nurses | Reference | |||||||
| Nursing assistants, other unqualified staff | –0.20 (–0.31 to –0.08)*** | 0.001 | 0.09 | (0.00 to 0.18) | 0.05 –0.10 (–0.20 to 0.02) | 0.09 | 0.03 (–0.07 to 0.14) | 0.53 |
| Occupational therapists | –0.02 (–0.25 to –0.21) | 0.89 | 0.05 (–0.13 to 0.24) | 0.57 | 0.03 (–0.20 to 0.26) | 0.81 | –0.24 (–0.45 to –0.02)Footnote * | 0.03 |
| Psychiatrists | 0.08 (–0.10 to 0.27) | 0.37 | 0.16 (0.01 to 0.31)Footnote * | 0.03 | 0.31 (0.13 to 0.50)*** | 0.001 | 0.19 (0.02 to 0.36)Footnote * | 0.03 |
| Clinical psychologists | –0.11 (–0.47 to 0.23) | 0.50 | 0.10 (–0.17 to 0.38) | 0.47 | 0.06 (–0.30 to 0.42) | 0.74 | –0.16 (–0.49 to 0.17) | 0.33 |
| Social workers | 0.12 (–0.12 to 0.36) | 0.32 | –0.01 (–0.20 to 0.18) | 0.91 | –0.13 (–0.37 to 0.10) | 0.27 | 0.07 (–0.29 to 0.14) | 0.51 |
| Ward managers/team leaders | 0.08 (–0.18 to 0.35) | 0.54 | 0.08 (–0.15 to 0.30) | 0.49 | 0.40 (0.15 to 0.65)** | 0.002 | 0.27 (0.04 to 0.50)Footnote * | 0.02 |
| Other occupations | –0.21 (–0.39 to –0.02)Footnote * | 0.03 | 0.09 (–0.06 to 0.23) | 0.26 | 0.17 (–0.01 to 0.36) | 0.07 | 0.09 (–0.09 to 0.26) | 0.34 |
CAMHS, child and adolescent mental health service; CMHT, community mental health team; PICU, psychiatric intensive care unit.
a Negative scores indicate lower levels of emotional strain than the reference group.
b Positive scores indicate higher levels of positive engagement than the reference group.
* P<0.05, ** P<0.01, *** P<0.001.
Variables associated with positive engagement
Positive engagement did not vary significantly by service type in these adjusted analyses. It was significantly associated with profession, with psychiatrists having a mean score 0.31 s.d. and service managers 0.40 s.d. above nurses (the reference group) (see Table 5). Another strong association was with ethnic group (Table DS6), with staff from both Black and Asian groups having adjusted means for positive engagement around a third of a standard deviation above the White groups (0.32 s.d. and 0.37 s.d. respectively). Those with longer total service in mental healthcare and those who had worked in their current service for more than a year had significantly lower positive engagement.
Levels of demand, control and support
There were highly significant differences between service types in demand and control variables (online Tables DS7 and DS8), with CMHT staff scoring higher than the rest on both demands and control. Rehabilitation ward, CAMHS and CRT staff also reported relatively high levels of autonomy in their work. Rehabilitation ward, PICU and CRT staff were at the lowest end of the range for demands, and forensic ward, older adult ward and PICU staff for control. Means for support from colleagues and managers varied less by service type and profession, although differences still reached statistical significance.
Demands and control varied still more widely by profession. Social workers and service managers reported the greatest demands and staff without professional qualifications the least, whereas the latter group also scored lowest for autonomy. Clinical psychologists reported levels of autonomy more than half a standard deviation above all other groups. Support varied less between professions than demands and control, with no significant difference for support from colleagues.
Models including demand–control–support variables
Table 5 shows the effects on associations between emotional strain, positive engagement and service type and profession of adding the demand, support and control variables; online Table DS9 shows in full the results of multilevel analyses including these variables and demographic and occupational characteristics. Emotional strain had highly significant associations with job demands, control and support from both managers and colleagues. The relationship with demands was especially large: one point greater job demands (on a five-point scale) were associated with half a standard deviation greater emotional strain. Some of the associations between emotional strain and service type or profession were no longer significant following adjustment for demands, control and support, including those with not having a professional qualification and with working on CAMHS, rehabilitation and older adult wards or in a CRT, and associations with length of service variables were attenuated. However, the association between greater emotional strain and working in a CMHT was unchanged.
All the Karasek model variables were also associated with positive engagement, but in the reverse direction for high job demands, which were associated with greater positive engagement. The association with control was especially strong, with 1 point higher score for control associated with a 0.38 s.d. increase in positive engagement. Adding demand, support and control to the model made little difference to the associations previously described with professions and demographic groups, indicating that perceived job characteristics do not explain these differences.
Discussion
The overall pattern of morale found in the mental health workforce was fairly encouraging. Staff tended to be satisfied with work and very satisfied with their colleagues, and they reported low levels of cynicism and good personal accomplishment. Where they were burnt out, as in most previous mental health workforce investigations this tended to take the form of high emotional exhaustion and the numbers reaching the threshold for caseness on the GHQ-12 were also substantial. That mental health work should have a high emotional impact is unsurprising, but a better understanding of this finding, its antecedents, its effect on patients and any effective means of alleviating psychological strain is nonetheless desirable.
There were considerable variations between service types. Acute general ward staff had mean emotional exhaustion scores just above the threshold for burnout, which is a matter for concern as these wards are numerous and have a key role in the mental health system. We compared these findings with levels reported in a previous systematic review; Reference Richards, Bee, Barkham, Gilbody, Cahill and Glanville5 compared both with the mixed in-patient ward samples and with the acute ward samples in this review, emotional exhaustion in our study was at the higher end of the range. However, many previous studies had small samples and low response rates, so more confidence may be placed in our findings. Less explicably, we also found emotional exhaustion around 3 points higher than in the one previous large multicentre investigation of acute in-patient ward staff morale. Reference Bowers, Allan, Simpson, Jones and Whittington23 Potential sources for this difference include a slightly higher response rate in our study, a mixed professional sample and the period of around 4 years that elapsed between the earlier study and our data collection. A small prospective cohort study of mental health staff morale showed relatively stable burnout over 2 years of follow-up; Reference Prosser, Johnson, Kuipers, Dunn, Szmukler and Reid24 nonetheless, it may be that differences between our study and others reflect a tendency for overall workforce morale to fluctuate over time, especially at times of considerable change in the NHS.
Little has previously been published on variations between in-patient ward types. Reference Richards, Bee, Barkham, Gilbody, Cahill and Glanville5 Morale indicators tended to be more positive on specialist wards, rehabilitation wards showing a particularly exemplary pattern of high personal accomplishment and low emotional exhaustion.
Turning to the community staff, our findings confirm a previous observation from a London study of good crisis resolution team staff morale despite the potential stresses of working with an acutely ill group in community settings. Reference Nelson, Johnson and Bebbington25 These staff rated support from colleagues very highly, suggesting a potential positive effect of the team approach implemented in CRTs. However, morale in CMHTs gives cause for concern. Despite good satisfaction, 60% of team members reached the burnout threshold on emotional exhaustion and 39% were GHQ stressed ‘cases’. These findings echo studies from the 1990s reporting high levels of burnout among CMHT staff, Reference Prosser, Johnson, Kuipers, Szmukler, Bebbington and Thornicroft26 yet burnout in the investigations of the past decade has tended to be lower. Reference Priebe, Fakhoury, Hoffmann and Powell27,Reference Billings, Johnson, Bebbington, Greaves, Priebe and Muijen28 Thus, in our study burnout seems to have reverted to levels that caused substantial concern about the teams’ sustainability in the 1990s when this form of care was relatively new. Reference Wykes, Stevens and Everitt29
Relationships between morale indicators
Most correlations between the commonly used morale indicators were moderate, suggesting constructs that are partially independent of one another. However, two principal components captured 62% of the variation in the indicators, one that appeared to reflect emotional strain, the other positive engagement with work. This structure is in keeping with the recent theory (based on a range of occupational samples) that work-related well-being has two distinct underlying higher-order dimensions – negative states of burnout and positive engagement with work. Reference Schaufeli and Bakker30 Future research on the mental health workforce should ensure good coverage of these two dimensions.
Explanatory value of the demand–support–control model
As in many other occupational samples, Reference Karasek15 the explanatory value of Karasek's demand–support–control model was confirmed. As elsewhere, high perceived demands were strongly associated with negative emotional states, and the extension of Karasek's theory that proposes an association between good job satisfaction and engagement and high job demands, high control and high support levels was also supported. Autonomy in carrying out job roles emerged as a key factor in staff well-being, strongly associated with both low emotional strain and high positive engagement. Support from colleagues and managers was also confirmed as associated with both components, but more modestly than the other Karasek variables. This suggests that interventions intended to reduce job demands or increase autonomy may be more likely to improve morale than strategies designed to enhance support.
A further aim was to explore how far variations in demands, control and support might account for differences between service types and between professions. These variables had substantial explanatory value for variations in emotional strain: several of the initially significant variations between service types and professional and demographic groups in emotional strain were no longer significant with the Karasek variables in the model. Thus, for example, the lower emotional strain reported by rehabilitation ward and CRT staff can be accounted for by the finding that staff in these services report both substantially lower levels of job demands and greater control (Table DS7) than acute general ward staff. Higher levels of emotional strain in CMHTs, however, persisted unchanged when the Karasek variables were added to the model, suggesting that explanations need to be sought in terms of other aspects of their culture and working environments. Addition of the Karasek variables to the model for positive engagement had less influence on relationships with other variables, suggesting a need for alternative explanations of its variations. For example, the striking relationship between greater positive engagement and non-White ethnic groups did not appear related to differences in demand, support and control variables.
Limitations and strengths of the study
Strengths of our study include its size, which substantially exceeds any other investigation of the mental health workforce in the national and international literature, Reference Paris and Hoge4,Reference Richards, Bee, Barkham, Gilbody, Cahill and Glanville5 both in numbers participating and in geographical reach and coverage of different professions and subspecialties. The response rate is respectable, and we included a range of morale indicators, allowing comparison both with previous mental health investigations and with other samples in occupational psychology.
Limitations include the possibility of systematic differences between non-responders and responders, and we had no formal test of representativeness of the workforce as a whole. There were also wide differences in response rates per ward, with outliers at 22% and 100%; thus, scores for some wards with low response rates might have been particularly unrepresentative. Despite excellent numbers overall, some groups within the sample are small. The cross-sectional nature of the study is also a significant limitation, especially in examination of the demand–support–control model where causality cannot be established; for example, we cannot ascertain whether those with high work demands develop high levels of emotional strain, or whether the emotionally exhausted perceive work demands as high.
Implications for research and service development
Our study suggests several questions for further investigation. The interrelationship of morale indicators, the extent to which they are distinct and their potential reducibility to a smaller number of main dimensions bears further exploration using more sophisticated psychometric techniques within both this and other data-sets. Other candidate explanatory variables for variations in morale include organisational context, negative events, built environment, patient population and staff personality attributes. Prospective examination of the relationship between explanatory variables and morale indicators is also desirable. Links between staff morale and patient well-being and outcomes also remain poorly understood.
Our study suggests a need to focus on CMHT staff, and, to a lesser extent, those on acute general wards in further research and development of interventions. Our findings do not adequately explain the high levels of emotional strain in CMHTs – further quantitative and qualitative work on their antecedents, including an analysis of the many organisational changes experienced or anticipated by CMHT staff in the NHS, might help arrive at such an understanding, underpinning the development of interventions.
Although not all differences between groups can be accounted for by them, the Karasek model variables (demand, control/autonomy and support) have substantial associations with both morale components, making the model a potential basis for developing interventions to raise morale. Mutual and managerial support tends currently to be the basis for interventions to improve mental health workforce morale and this is supported, but the effects for support are smaller than those for demands and autonomy. Designing interventions to reduce job demands is a challenge in the current climate of austerity in the NHS. Reference Holloway31 Nonetheless, initiatives such as the Productive Wards programme, Reference Wilson32 involving redesign of working environments and practices aimed at increasing staff time available for direct patient care and reducing other demands, may have some potential to reduce emotional strain. The substantial relationship between autonomy and both emotional strain and positive engagement suggests that this relatively neglected factor might be an appropriate focus for interventions, examining in detail the organisation of jobs and teams to identify ways in which autonomy might be increased, especially in groups of staff reporting low levels of this factor.
Funding
This project was funded by the National Institute for Health Services and Delivery Research Programme (project number/08/1604/142).
Acknowledgements
We wish to acknowledge the contribution of the other members of the In-patient Staff Morale Study research team, and are also very grateful for extensive support received from the North and South London, South-west, East of England and Heart of England hubs of the Mental Health Research Network, and for the helpfulness of staff in the 136 participating services. The views and opinions expressed in this paper are those of the authors and do not necessarily reflect those of the HS&DR programme, NIHR, NHS or the Department of Health.










eLetters
No eLetters have been published for this article.