It is often reported that, even after taking account of other influences, such as age, gender and social support, people who report religious belief and practice experience better mental and physical health than those who do not. Reference Wong, Rew and Slaikeu1–Reference Johnstone, Franklin, Yoon, Burris and Shigaki3 However, in a meta-analysis of 147 studies on religious belief and depression, Smith et al found only a weak negative correlation (–0.096) between religiousness and depressive symptoms. Reference Smith, McCullough and Poll4 On average, positive religiousness accounted for only 1% of the variance in the severity of depressive symptoms. Furthermore, extrinsic religious orientation and so-called negative religious coping (for example, avoiding difficulties through religious activities, blaming God for difficulties) were associated with higher levels of depressive symptoms.
The way religiosity is measured in research can be problematic, particularly when well-being is included as a component of the measure itself. Reference Koenig5 Furthermore, most research into this association has entailed Judeo-Christian concepts of religion in White, North American populations, and has seldom taken account of spiritual beliefs unconnected with personal or public religious practice. Reference King and Dein6 In a number of studies in the UK, we have reported that religious and spiritual beliefs are not linked to better physical health outcomes Reference King, Speck and Thomas7,Reference King, Speck and Thomas8 and, in particular that spiritual beliefs in the absence of a religious framework may be associated with poorer mental health. Reference King, Weich, Nazroo and Blizard9 The third National Psychiatric Morbidity Survey in England Reference McManus, Meltzer, Brugha, Bebbington and Jennings10 was the first general population survey in this country to include questions on religious and spiritual beliefs. In this study we aimed to examine the association between such beliefs and receipt of psychiatric treatment, and a range of psychiatric symptoms and diagnoses in a random sample of the English population.
Method
Survey methods
The third National Psychiatric Morbidity Study was conducted between October 2006 and December 2007 across England, using individual or groups of postcode sectors as sampling units. Reference McManus, Meltzer, Brugha, Bebbington and Jennings10 In the first stage of sampling, postcode sectors were divided into regions based on strategic health authority. All the sampling units within each strategic health authority were further stratified on the basis of the proportion of people in non-manual classes, and sorted by the proportion of households without a car based on UK 2001 Census data. A total of 519 postal sectors were selected by sampling from each stratum with a probability proportional to size in terms of the number of delivery points. In the second stage of sampling, 28 delivery points were randomly selected within each of the selected postal sectors, providing a sample of 14 532 delivery points. Interviewers visited the addresses to identify private households containing at least one person aged 16 or over. When visited, 1318 of the selected addresses were found not to contain a private household and were excluded from the survey sample. After contact was made with each eligible household, one person was randomly selected to take part, using the Kish method. Reference Kish11 Ethical constraints meant that data on people refusing to participate could not be collected. Trained interviewers conducted a structured, laptop computerised interview in respondents' homes, or elsewhere if requested, each interview lasting on average 90 min. Interviewers were fully briefed on the administration of the survey, and followed full sets of written instructions. Topics covered on 1-day survey-specific training included introducing the survey, questionnaire content, confidentiality and respondent distress.
The survey data were weighted to take account of likelihood of selection and non-response, so that the results were representative of the English household population aged 16 years and over. Sample weights were first applied to take account of the different probabilities of selecting respondents in different sized households. Second, to reduce household non-response bias, a household-level weight was calculated from a logistic regression model using interviewer observation and area-level variables (collected from Census 2001 data) available for responding and non-responding households. Finally, calibration weighting based on age, gender and region weighted the data to represent the structure of the national population, and take account of differential non-response between regions and age×gender groups.
We focus on the weighted results in the text, but provide both weighted and unweighted bases in the table showing sociodemographics and life views (online Table DS1). The unweighted bases are presented where appropriate to show the number of respondents included. The weighted base shows the relative size of the various sample elements after weighting, reflecting their proportions in the English population. The absolute size of the weighted base has no particular significance, since it has been scaled to the achieved sample size. Reference McManus, Meltzer, Brugha, Bebbington and Jennings10
Measures
Following confirmation of demographic data, the following standardised instruments were used.
-
(a) Six questions adapted from those in the questionnaire version of the Royal Free interview for religious and spiritual beliefs, which assesses the nature and strength of beliefs and practice. Reference King, Speck and Thomas12,Reference King, Speck and Thomas13 Because of the length of the overall interview, questions on each topic had to be kept as brief as possible. Participants were provided with the statement: ‘By religion, we mean the actual practice of a faith, e.g. going to a temple, mosque, church or synagogue. Some people do not follow a religion but do have spiritual beliefs or experiences. Some people make sense of their lives without any religious or spiritual belief’. Although slightly shorter than in the Royal Free Interview, the words used are exactly the same, in order not to lose the statement's essential meaning or threatening the validity of the original instrument. The interview then went on: ‘Would you say that you have a religious or spiritual understanding of your life?’ Participants could indicate whether their understanding was predominately (i) religious; (ii) spiritual or (iii) neither. If they had a specific religion, they were asked to name it. If religious or spiritual, they were asked to indicate on two sliding scales of zero to ten how strongly they held to their understanding of life and how important practice of their faith (for example private meditation, religious services) was to them. These respondents were also asked to report how often they attended services, prayer meetings or places of worship.
-
(b) The revised Clinical Interview Schedule (CIS-R) collects data on symptoms of common mental disorder and derives psychiatric diagnoses according ICD-10. Reference Goldberg, Cooper, Eastwood, Kedward and Shepherd14–16 The CIS-R enquires about the presence and severity of 14 non-psychotic psychiatric symptoms during the week prior to interview. The CIS-R score may be analysed as: (i) a continuous score, along a single continuum of severity; (ii) a dichotomous variable (case threshold ⩾12); and (iii) ICD-10 diagnostic categories. Reference Lewis, Pelosi, Araya and Dunn15,Reference Meltzer, Gill and Petticrew17 Diagnostic algorithms for use with the CIS-R cover (i) depressive episodes (classified as mild, moderate or severe); (ii) four types of anxiety disorder, namely generalised anxiety disorder, panic disorder, phobias (classified as agoraphobia, social phobia and simple phobia), obsessive– compulsive disorder (OCD); and (iii) mixed anxiety/depressive disorder. The latter include those who scored above the case threshold on the CIS-R, but do not meet diagnostic criteria for any other ICD-10 disorder.
-
(c) The Psychosis Screening Questionnaire (PSQ) is a brief schedule that screens for symptoms commonly found in psychotic disorders. Reference Bebbington and Nayani18 Rather than making a definitive diagnosis, it indicates whether a psychotic disorder may be present.
-
(d) A shortened version of the Close Persons Questionnaire that evaluates social support. Reference Stansfeld and Marmot19 This had been used in previous national surveys. Reference King, Weich, Nazroo and Blizard9,Reference Meltzer, Gill and Petticrew17 Seven questions enquire about the level of intimacy and social support from close friends and family. The answers are scored from one to three and are summed to a total score; higher scores indicate higher social support.
-
(e) The Alcohol Use Disorders Identification Test (AUDIT) questionnaire is a widely used and well validated instrument that contains 10 questions about use of, and attitudes to, alcohol consumption, in this instance over the preceding 12 months. Reference Barbor, de la Fuente, Saunders and Grant20,Reference Coulton, Drummond, James, Godfrey and Bland21 Men who scored more than seven and women who scored more than four were classified as hazardous drinkers.
-
(f) The Trauma Screening Questionnaire (TSQ) Reference Walters, Bisson and Shepherd22 was used to collect information on the presence of trauma-related symptoms in the past week. A traumatic event is one in which a person experiences, witnesses or is confronted with a death or a serious injury or threat to self or close others. It is more severe than a stressful life event. Scoring positively on this questionnaire indicates the presence of trauma-related symptoms in the preceding week and that a clinical assessment for post-traumatic stress disorder (PTSD) is warranted; it does not specify a diagnosis of PTSD, in particular because it evaluates only two of the four criteria taken to identify a traumatising event. As a screening tool it has high sensitivity and specificity but lower positive predictive value (0.48) as a result of the usually low prevalence of PTSD (1%) in most populations. Reference Walters, Bisson and Shepherd22
-
(g) The SCOFF is a five-item screening tool for anorexia and bulimia nervosa that enquires about eating attitudes and behaviour over the preceding year. Reference Morgan, Reid and Lacey23 Endorsement of two or more items represented a positive screening for an eating disorder. A further question (‘in the last year… did your feelings about food interfere with your ability to work, meet personal responsibilities, and/or enjoy a social life?’) was added to judge the impact of such eating attitudes and behaviour.
-
(h) Problem gambling is gambling to a degree that compromises, disrupts or damages family, personal or recreational pursuits. This categorisation was based on the DSM-IV 24 criteria for problem and pathological gambling. Participants who met three or more of these diagnostic criteria were classified as problem gamblers.
-
(i) Questions on use of recreational drugs came from the Diagnostic Interview Schedule. Reference Malgady, Rogler and Tryon25 Use of a drug in the past year and the presence of one of five symptoms were used to indicate drug dependence. Dependence was categorised as dependence on cannabis only and dependence on other drugs (with or without cannabis dependence).
-
(j) One question explored how happy the participants felt ranging from very, to fairly and not too happy.
-
(k) Finally, one binary variable summarised whether or not the respondent was taking any form of psychotropic medication and one summarised whether or not they were receiving any form of psychotherapy or counselling.
Statistical analysis
All analyses were conducted in Stata release 12.0, for Windows, using the survey command to account for the unequal probability of selection and to adjust the standard errors to account for clustering in areas sampled in data collection. Our main analyses concerned possible associations between holding a religious, spiritual or secular life view and: receiving counselling/psychotherapy or psychotropic medication for a mental disorder; mental disorders classified by the CIS-R; possible PTSD, psychosis or an eating disorder; hazardous drinking; recreational drug use and dependence; and level of happiness.
We explored these associations using logistic regression, except for happiness, which utilised ordered logistic regression and for drug dependence where multinomial logistic regression was used. We adjusted for gender, age group, ethnicity, educational attainment, marital status or perceived social support if they were significantly associated with the given outcome. Social support is known to be associated with religious belief and practice. Reference Ferraro and Koch26,Reference George, Larson, Koenig and McCollough27 The reference group chosen for these analyses were participants reporting a secular (neither religious nor spiritual) life view, given it was the largest and most distinct of the three groups in terms of absence of any spiritual belief.
Results
Response rates and description of the population
A total of 9% of sampled addresses contained no private households and 4% were addresses of unknown eligibility. This left a known eligible sample of 12 694 addresses. Applying the eligibility rate among those where it was established, to those where it was not, it was estimated that 91% of those of unknown eligibility would have been eligible to take part. This increased the set sample of households to 13 171. In total, 7403 respondents (56.2%) provided a productive interview. The mean age of the participants was 46.3 years (s.e. = 0.28, unweighted range 16–97), 4206 (51.4%) were women, 85% were White British, 26% had no educational qualifications and 52% were married (online Table DS1).
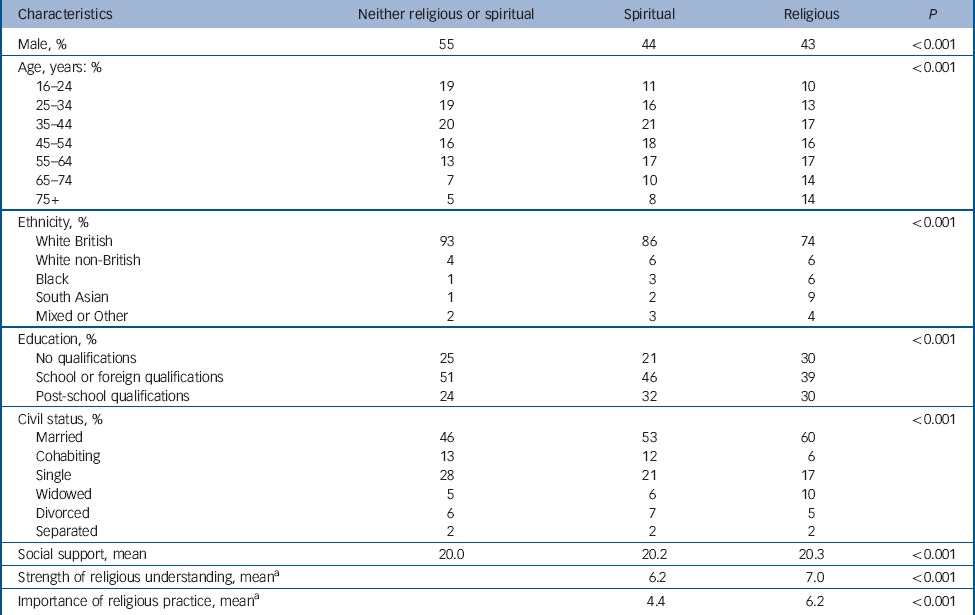
Table 1 Univariable associations with life view: sociodemographics (n = 7403)
| Characteristics | Neither religious or spiritual | Spiritual | Religious | P |
|---|---|---|---|---|
| Male, % | 55 | 44 | 43 | <0.001 |
| Age, years: % | <0.001 | |||
| 16–24 | 19 | 11 | 10 | |
| 25–34 | 19 | 16 | 13 | |
| 35–44 | 20 | 21 | 17 | |
| 45–54 | 16 | 18 | 16 | |
| 55–64 | 13 | 17 | 17 | |
| 65–74 | 7 | 10 | 14 | |
| 75+ | 5 | 8 | 14 | |
| Ethnicity, % | <0.001 | |||
| White British | 93 | 86 | 74 | |
| White non-British | 4 | 6 | 6 | |
| Black | 1 | 3 | 6 | |
| South Asian | 1 | 2 | 9 | |
| Mixed or Other | 2 | 3 | 4 | |
| Education, % | <0.001 | |||
| No qualifications | 25 | 21 | 30 | |
| School or foreign qualifications | 51 | 46 | 39 | |
| Post-school qualifications | 24 | 32 | 30 | |
| Civil status, % | <0.001 | |||
| Married | 46 | 53 | 60 | |
| Cohabiting | 13 | 12 | 6 | |
| Single | 28 | 21 | 17 | |
| Widowed | 5 | 6 | 10 | |
| Divorced | 6 | 7 | 5 | |
| Separated | 2 | 2 | 2 | |
| Social support, mean | 20.0 | 20.2 | 20.3 | <0.001 |
| Strength of religious understanding, meanFootnote a | 6.2 | 7.0 | <0.001 | |
| Importance of religious practice, meanFootnote a | 4.4 | 6.2 | <0.001 |
a. Only applicable for those who are religious or spiritual.
Understanding of life
Of the participants 35% had a religious understanding of life, 19% were spiritual (without religious participation) and 46% were neither religious nor spiritual in outlook (online Table DS1). In total 53% gave a nominal religious affiliation, with the majority citing Christianity (86%). Demographic characteristics of the sample stratified by understanding of life are shown in Table 1. People with no religious or spiritual understanding were significantly younger and more often White British, but were less likely to have qualifications beyond secondary school or to be married. Religious people had stronger beliefs and placed more importance on practice of those beliefs than people with a purely spiritual understanding (Table 1).
Mental disorders and substance use
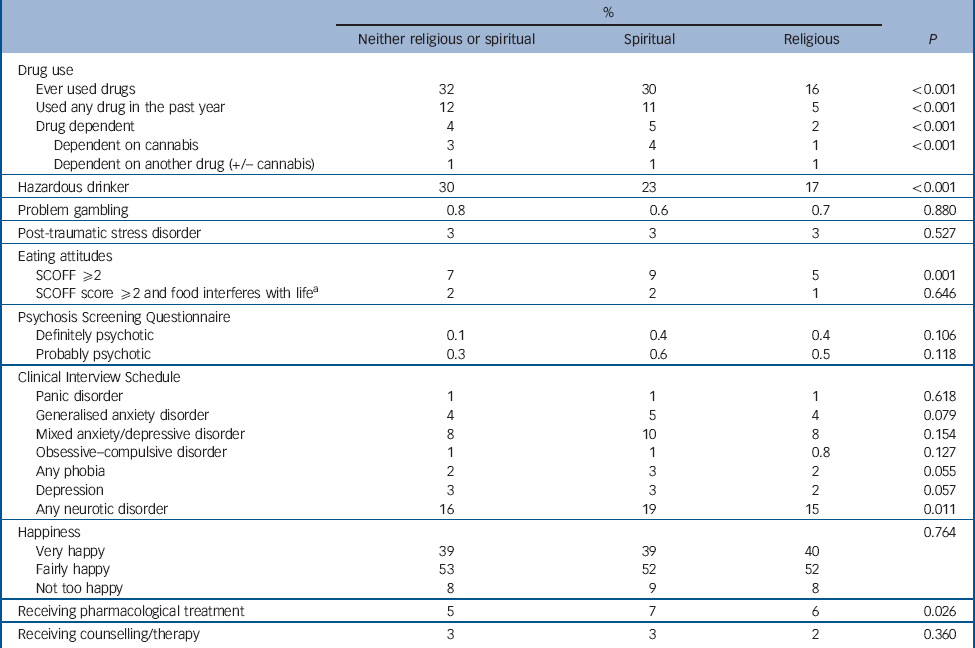
People with a religious understanding of life were less likely to use or be dependent on drugs, or be hazardous drinkers (Table 2). People with a spiritual understanding of life were more likely to have abnormal eating attitudes and any neurotic disorder. There were no differences in overall happiness or level of social support. People with no religious or spiritual understanding were least likely to be taking psychotropic medication.
Comparison of groups after adjustment for other influences
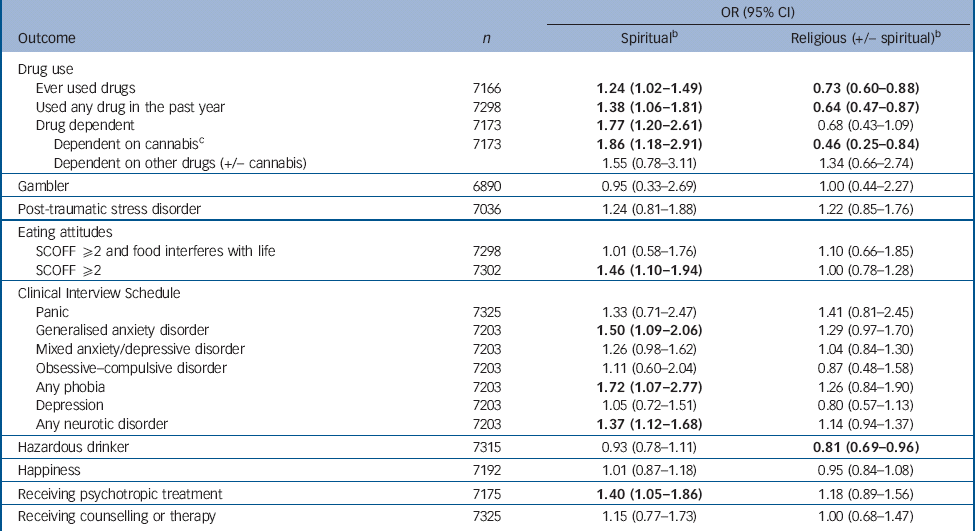
In a multivariate regression, we selected those people with neither a religious nor spiritual understanding of life (the largest group) to serve as a reference against which to compare the other two groups, namely those with a religious understanding and those with a spiritual understanding of life. After adjustment for important associated influences, there were few substantial differences in prevalence of mental disorder or receipt of treatment between people with no religious or spiritual understanding and those who were religious, except for less drug use and hazardous drinking in the latter (Table 3). However, people with a spiritual understanding were more likely than those who were neither religious nor spiritual to take psychotropic medication, to use recreational drugs or be dependent on them, to have a generalised anxiety disorder, phobia or any neurotic disorder or to have abnormal eating attitudes.
Discussion
Main findings
Our main finding is that people who had a spiritual understanding of life had worse mental health than those with an understanding that was neither religious nor spiritual. Those who were religious were broadly similar, in terms of prevalence of mental disorder and use of mental health treatments, to those who were neither religious nor spiritual after adjustment for potential confounders, except they were significantly less likely to use, or be dependent on, drugs or alcohol. This supports evidence from a national UK sample of people from a range of Black and minority ethnic groups Reference King, Weich, Nazroo and Blizard9 on the vulnerability of people who describe themselves as spiritual. It adds to the evidence that people with a spiritual understanding in the absence of a religious framework appear to have the worst mental health. It also confirms that religious people are less likely to use alcohol Reference Michalak, Trocki and Bond28 and recreational drugs Reference Hope and Cook29 but fails to confirm North American evidence that holding a religious understanding of life provides protection against mental disorders. Reference Koenig30 It also concurs with other evidence from England that there is no clear relationship between religiosity and happiness. Reference Lewis, Maltby and Day31
Table 2 Univariable associations with life view: outcomes (n = 7403)
| % | ||||
|---|---|---|---|---|
| Neither religious or spiritual | Spiritual | Religious | P | |
| Drug use | ||||
| Ever used drugs | 32 | 30 | 16 | <0.001 |
| Used any drug in the past year | 12 | 11 | 5 | <0.001 |
| Drug dependent | 4 | 5 | 2 | <0.001 |
| Dependent on cannabis | 3 | 4 | 1 | <0.001 |
| Dependent on another drug (+/– cannabis) | 1 | 1 | 1 | |
| Hazardous drinker | 30 | 23 | 17 | <0.001 |
| Problem gambling | 0.8 | 0.6 | 0.7 | 0.880 |
| Post-traumatic stress disorder | 3 | 3 | 3 | 0.527 |
| Eating attitudes | ||||
| SCOFF ≥2 | 7 | 9 | 5 | 0.001 |
| SCOFF score ≥2 and food interferes with lifeFootnote a | 2 | 2 | 1 | 0.646 |
| Psychosis Screening Questionnaire | ||||
| Definitely psychotic | 0.1 | 0.4 | 0.4 | 0.106 |
| Probably psychotic | 0.3 | 0.6 | 0.5 | 0.118 |
| Clinical Interview Schedule | ||||
| Panic disorder | 1 | 1 | 1 | 0.618 |
| Generalised anxiety disorder | 4 | 5 | 4 | 0.079 |
| Mixed anxiety/depressive disorder | 8 | 10 | 8 | 0.154 |
| Obsessive–compulsive disorder | 1 | 1 | 0.8 | 0.127 |
| Any phobia | 2 | 3 | 2 | 0.055 |
| Depression | 3 | 3 | 2 | 0.057 |
| Any neurotic disorder | 16 | 19 | 15 | 0.011 |
| Happiness | 0.764 | |||
| Very happy | 39 | 39 | 40 | |
| Fairly happy | 53 | 52 | 52 | |
| Not too happy | 8 | 9 | 8 | |
| Receiving pharmacological treatment | 5 | 7 | 6 | 0.026 |
| Receiving counselling/therapy | 3 | 3 | 2 | 0.360 |
a. ≥2 on the SCOFF questionnaire and an affirmative reply to whether or not the eating difficulties has a serious impact on their lives.
Strengths and limitations
The strengths of this study are the random selection of a nationally representative sample of participants, the sample size, an in-depth assessment of mental health and the use of standardised questions on religion and spirituality that were developed and standardised in the UK and do not overlap with questions on well-being. However, there are also a number of limitations. First, our results depend on the definitions of religion and spirituality that were posed to participants. Although spirituality is notoriously difficult to define, Reference King and Koeing32 this way of describing it to research participants has at least been shown to be reliable. Reference King, Speck and Thomas12,Reference King, Speck and Thomas13 However, we did not examine religious belief in detail, nor to what extent it was intrinsic or extrinsic. Reference Pargament33 Second, the cross-sectional nature of the data means that we cannot attribute cause and effect to any relationship between spiritual beliefs and mental health.
Table 3 Regression modelling showing the relationship between psychiatric outcomes and life viewFootnote a
| OR (95% CI) | |||
|---|---|---|---|
| Outcome | n | SpiritualFootnote b | Religious (+/– spiritual)Footnote b |
| Drug use | |||
| Ever used drugs | 7166 | 1.24 (1.02–1.49) | 0.73 (0.60–0.88) |
| Used any drug in the past year | 7298 | 1.38 (1.06–1.81) | 0.64 (0.47–0.87) |
| Drug dependent | 7173 | 1.77 (1.20–2.61) | 0.68 (0.43–1.09) |
| Dependent on cannabisFootnote c | 7173 | 1.86 (1.18–2.91) | 0.46 (0.25–0.84) |
| Dependent on other drugs (+/– cannabis) | 1.55 (0.78–3.11) | 1.34 (0.66–2.74) | |
| Gambler | 6890 | 0.95 (0.33–2.69) | 1.00 (0.44–2.27) |
| Post-traumatic stress disorder | 7036 | 1.24 (0.81–1.88) | 1.22 (0.85–1.76) |
| Eating attitudes | |||
| SCOFF ≥2 and food interferes with life | 7298 | 1.01 (0.58–1.76) | 1.10 (0.66–1.85) |
| SCOFF ≥2 | 7302 | 1.46 (1.10–1.94) | 1.00 (0.78–1.28) |
| Clinical Interview Schedule | |||
| Panic | 7325 | 1.33 (0.71–2.47) | 1.41 (0.81–2.45) |
| Generalised anxiety disorder | 7203 | 1.50 (1.09–2.06) | 1.29 (0.97–1.70) |
| Mixed anxiety/depressive disorder | 7203 | 1.26 (0.98–1.62) | 1.04 (0.84–1.30) |
| Obsessive–compulsive disorder | 7203 | 1.11 (0.60–2.04) | 0.87 (0.48–1.58) |
| Any phobia | 7203 | 1.72 (1.07–2.77) | 1.26 (0.84–1.90) |
| Depression | 7203 | 1.05 (0.72–1.51) | 0.80 (0.57–1.13) |
| Any neurotic disorder | 7203 | 1.37 (1.12–1.68) | 1.14 (0.94–1.37) |
| Hazardous drinker | 7315 | 0.93 (0.78–1.11) | 0.81 (0.69–0.96) |
| Happiness | 7192 | 1.01 (0.87–1.18) | 0.95 (0.84–1.08) |
| Receiving psychotropic treatment | 7175 | 1.40 (1.05–1.86) | 1.18 (0.89–1.56) |
| Receiving counselling or therapy | 7325 | 1.15 (0.77–1.73) | 1.00 (0.68–1.47) |
a. Numbers were insufficient to investigate psychosis. Results in bold are significant.
b. Reference category is not religious or spiritual, models adjust for those that are significant from age, gender, marital status, ethnicity, educational attainment and social support.
c. Reference category for the outcome is no drug use.
Comparison with findings from other studies
A recent large USA internet survey of people who regarded themselves as non-religious Reference Galen34 also reported that non-religious people who held spiritual beliefs (only 2% of the survey population) had less emotional stability as measured by a personality rating scale. However, it is difficult to know how far we can compare such people with our spiritual group, which made up 19% of the study population. Although the authors concluded that belief is a measure of negative personality traits, their findings (and ours) are in opposition to earlier evidence from the UK that spirituality is associated with greater extraversion and optimism (rather than neuroticism and psychoticism), particularly among men. Reference Maltby and Day35 The limitation of the latter study, however was that it was based on a volunteer student population and is therefore unlikely to be generalisable. Another possible explanation for our finding concerning people with a spiritual life view is that they are caught up in an existential search that is driven by their emotional distress. Reference King, Weich, Nazroo and Blizard9,Reference Bhui, King, Dein and O'Connor36
Why might findings in Europe concerning the emotional stability of religious people vary from those in the USA? There is considerable evidence that the UK is a less religious country than the USA in terms of the number of people professing a belief in God or attending places of worship. Reference Taylor37 We found that a relatively low number of people expressed some sort of spiritual or religious belief in this survey (54%) in comparison with that found in recent surveys both in the UK and around the world where levels have been closer to 70%. Reference Ashworth and Farthing38,39 Given that religious participation in English society is a minority activity, it may be that the social support intrinsic to a more religious society is missing. A further possibility is the way in which we measured spiritual and religious understanding. The Royal Free Interview for Religious and Spiritual Beliefs was developed and standardised in the UK and has not been used extensively in the USA. However, this is not strictly a limitation as one could argue that instruments should be most appropriate to the setting in which they were developed. Certainly, the difference in the findings concerning religion and mental health between the USA and the UK would bear greater investigation.
We conclude that there is increasing evidence that people who profess spiritual beliefs in the absence of a religious framework are more vulnerable to mental disorder. The nature of this association needs greater examination in qualitative and in prospective quantitative research.








eLetters
No eLetters have been published for this article.