Many countries have difficulty in recruiting adequate numbers of doctors to psychiatry. In the USA, it has been estimated that three-quarters of its counties (the administrative level within US states) have a shortage of psychiatric prescribers. Reference Thomas, Ellis, Konrad, Holzer and Morrissey1 The percentage of medical students pursuing a psychiatry residency in the USA was 7–10% in the 1940s but it dropped to 3–4% in 2002–2007. Reference Tamaskar and McGinnis2,Reference Salsberg, Rockey, Rivers, Brotherton and Jackson3 In England, in 2009, 15% of all unfilled consultant posts were in psychiatry; 4 and a census by the Royal College of Psychiatrists concluded that recruitment to specialty training posts remains difficult. 5 The UK Medical Careers Research Group (UKMCRG) has studied the career preferences of junior doctors and their subsequent career pathways for many years. Reference Goldacre, Turner, Fazel and Lambert6 Here, we update our findings on career choice for psychiatry and report on reasons given by doctors for choosing psychiatry. In addition, unlike our previous study, we have added new findings examining doctors who told us that they had initially considered a career in psychiatry and then decided not to pursue it.
Method
The UKMCRG has undertaken cohort studies of all medical graduates who qualified in the years 1974, 1977, 1980, 1983, 1993, 1996, 1999, 2000, 2002, 2005, 2008 and 2009 from all UK medical schools. Our methods have been described in detail elsewhere. Reference Lambert, Goldacre, Edwards and Parkhouse7,Reference Goldacre, Davidson and Lambert8 Near the end of the first, third and fifth years after qualification (and at longer time intervals after that), postal questionnaires are sent to all the graduates. The starting point for each survey is the cohort as it originally was at the time of qualification. Current addresses are supplied to us by the UK General Medical Council and by the doctors themselves from replies to successive surveys. In calculating our response rate, we excluded those known to have died, those who expressed a wish not to participate and those whose address was untraceable. Others in the original cohort who did not initially reply were sent several reminders.
We ask graduates ‘What is your choice of long-term career?’ This is an open response question, inviting the doctors to name their preferred clinical specialty or any other choice of career. We invite them to list up to three specialty choices. If they specify more than one specialty, they are asked to indicate whether their choices are of equal priority (termed ‘tied’ choices by us). In this paper, we counted first choices for psychiatry tied with another specialty (as well as untied first choices) as doctors choosing psychiatry. We also ask them to indicate whether their choice of specialty is ‘definite’, ‘probable’ or ‘uncertain’.
The graduates of 1993, 1996, 1999, 2000, 2002, 2008 and 2009 were asked to indicate whether each factor from a list of 11 had influenced their choice of specialty ‘not at all’, ‘a little’ or ‘a great deal’. In addition to comments about reasons for choosing their specialty, some doctors provided spontaneous comments to us about career choices they had considered and rejected. Accordingly, we decided to add a structured question on this in the survey of the doctors who qualified in 2002, 2005 and 2008: ‘Is there a choice of long-term career which you have seriously considered but have now decided not to pursue?’ If they answered yes, they were asked ‘What was that choice?’ and ‘What are your most important reasons for rejecting that choice?’ Reasons for rejection were sought as free-text responses. Some respondents gave a single reason for rejection; others gave several reasons. We read the responses and developed a coding scheme to reflect the main themes raised by respondents (Appendix 1). Two coders then independently coded all the reasons given, by theme, and compared each other's coding. Any differences between coders were resolved through discussion. We compared findings from doctors who specified psychiatry with those from doctors who reported that they had considered but not pursued other clinical specialties.
We used χ2 statistics (reporting Yates's continuity correction where there was only one degree of freedom, and Mantel–Haenszel linear-by-linear χ2-test for linear association between two variables) correlation analysis to make comparisons between groups of doctors and to test their statistical significance. A binary logistic regression model was used to investigate variation between medical schools in choice for psychiatry: categorical predictors were gender, cohort and medical school, and the dependent variable was whether or not psychiatry had been chosen as a first, second or third choice.
This study was approved by the UK National Research Ethics Service (ref 04/Q1907/48).
Results
The survey questionnaires were sent to 51 538 doctors covering all 12 cohorts in year 1; and 33 974 (65.9%) replied. Three years after qualification, the survey questionnaire was sent to 38 131 doctors covering the first ten cohorts: 26 174 (68.6%) replied. Five years after qualification, the survey questionnaire was sent to 29 111 doctors covering the first eight cohorts (1974–1980 and 1993–2002: the 1983 cohort was not surveyed in year 5) and 20 239 (69.5%) replied.
Early career choices for psychiatry: first choices
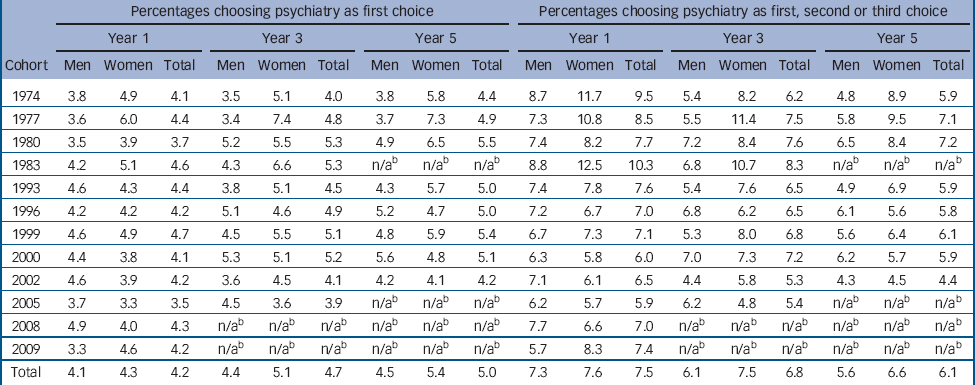
Considering all cohorts combined, 1 year after qualification 4.2% of all respondents (4.1% of men and 4.3% of women) indicated that their first choice of long-term career was psychiatry (χ2 1 = 0.8, P>0.05, comparing men and women; Table 1, online Fig. DS1 and online Table DS1). There was no overall linear trend over time (across cohorts) in career choice for psychiatry (Table 1, Fig. DS1 and Table DS1).
Table 1 Percentages of respondents choosing psychiatry as their first, second or third choice of career at 1 (1974–2009), 3 (1974–2005) and 5 (1974–2000) years after graduationFootnote a
| Percentages choosing psychiatry as first choice | Percentages choosing psychiatry as first, second or third choice | |||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Year 1 | Year 3 | Year 5 | Year 1 | Year 3 | Year 5 | |||||||||||||
| Cohort | Men | Women | Total | Men | Women | Total | Men | Women | Total | Men | Women | Total | Men | Women | Total | Men | Women | Total |
| 1974 | 3.8 | 4.9 | 4.1 | 3.5 | 5.1 | 4.0 | 3.8 | 5.8 | 4.4 | 8.7 | 11.7 | 9.5 | 5.4 | 8.2 | 6.2 | 4.8 | 8.9 | 5.9 |
| 1977 | 3.6 | 6.0 | 4.4 | 3.4 | 7.4 | 4.8 | 3.7 | 7.3 | 4.9 | 7.3 | 10.8 | 8.5 | 5.5 | 11.4 | 7.5 | 5.8 | 9.5 | 7.1 |
| 1980 | 3.5 | 3.9 | 3.7 | 5.2 | 5.5 | 5.3 | 4.9 | 6.5 | 5.5 | 7.4 | 8.2 | 7.7 | 7.2 | 8.4 | 7.6 | 6.5 | 8.4 | 7.2 |
| 1983 | 4.2 | 5.1 | 4.6 | 4.3 | 6.6 | 5.3 | n/aFootnote b | n/aFootnote b | n/aFootnote b | 8.8 | 12.5 | 10.3 | 6.8 | 10.7 | 8.3 | n/aFootnote b | n/aFootnote b | n/aFootnote b |
| 1993 | 4.6 | 4.3 | 4.4 | 3.8 | 5.1 | 4.5 | 4.3 | 5.7 | 5.0 | 7.4 | 7.8 | 7.6 | 5.4 | 7.6 | 6.5 | 4.9 | 6.9 | 5.9 |
| 1996 | 4.2 | 4.2 | 4.2 | 5.1 | 4.6 | 4.9 | 5.2 | 4.7 | 5.0 | 7.2 | 6.7 | 7.0 | 6.8 | 6.2 | 6.5 | 6.1 | 5.6 | 5.8 |
| 1999 | 4.6 | 4.9 | 4.7 | 4.5 | 5.5 | 5.1 | 4.8 | 5.9 | 5.4 | 6.7 | 7.3 | 7.1 | 5.3 | 8.0 | 6.8 | 5.6 | 6.4 | 6.1 |
| 2000 | 4.4 | 3.8 | 4.1 | 5.3 | 5.1 | 5.2 | 5.6 | 4.8 | 5.1 | 6.3 | 5.8 | 6.0 | 7.0 | 7.3 | 7.2 | 6.2 | 5.7 | 5.9 |
| 2002 | 4.6 | 3.9 | 4.2 | 3.6 | 4.5 | 4.1 | 4.2 | 4.1 | 4.2 | 7.1 | 6.1 | 6.5 | 4.4 | 5.8 | 5.3 | 4.3 | 4.5 | 4.4 |
| 2005 | 3.7 | 3.3 | 3.5 | 4.5 | 3.6 | 3.9 | n/aFootnote b | n/aFootnote b | n/aFootnote b | 6.2 | 5.7 | 5.9 | 6.2 | 4.8 | 5.4 | n/aFootnote b | n/aFootnote b | n/aFootnote b |
| 2008 | 4.9 | 4.0 | 4.3 | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | 7.7 | 6.6 | 7.0 | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b |
| 2009 | 3.3 | 4.6 | 4.2 | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | 5.7 | 8.3 | 7.4 | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b | n/aFootnote b |
| Total | 4.1 | 4.3 | 4.2 | 4.4 | 5.1 | 4.7 | 4.5 | 5.4 | 5.0 | 7.3 | 7.6 | 7.5 | 6.1 | 7.5 | 6.8 | 5.6 | 6.6 | 6.1 |
a. Numbers of respondents were: 16 488 (men), 17 486 (women) and 33 974 (total) in year 1; 13 429 (men), 12 745 (women) and 26 174 (total) in year 3; and 10 544 (men), 9695 (women) and 20 239 (total) in year 5.
b. Third- and fifth-year choices not yet available for graduates of 2008/9; fifth-year choices not yet available for graduates of 2005; the 1983 cohort was not surveyed in year 5.
Three years after qualification, 4.7% of all respondents (4.4% of men and 5.1% of women) gave psychiatry as their first choice, as did 5.0% of all respondents 5 years after (4.5% of men and 5.4% of women). Three and five years after qualification, the percentage of women who chose psychiatry was significantly higher than that of men (χ2 1 = 8.7, P<0.01, comparing men and women, in each year). Although there was no significant linear relationship in career choice across cohorts overall, from about 1999 the percentage of women who chose psychiatry in years 3 and 5 started to decline (χ2 1 for linear trend 14.2, P<0.001 and χ2 1 = 10.2, P<0.01 respectively; Table 1, Fig. DS1 and Table DS1).
Early career choices for psychiatry: first, second and third choices
Considering first, second and third choices of career combined, 7.5% of all respondents (7.3% of men and 7.6% of women) indicated that they were at least considering a choice for psychiatry in year 1 (χ2 1 = 0.9, P>0.05, comparing men and women; Table 1, Fig. DS1 and Table DS1). Three years after graduation, 6.8% of respondents (6.1% of men, 7.5% of women) gave psychiatry as a possible choice (χ2 1 = 19.3, P<0.001, comparing men and women). Five years after, 6.1% of respondents (5.6% of men, 6.6% of women) gave psychiatry as a choice (χ2 1 = 8.3, P<0.01, comparing men and women).
Considering all choices for psychiatry – first, second and third choices combined – there was a significant downward linear trend over time (P<0.001 for choices given at years 1 and 3, P<0.01 for choices at year 5). There was a steeper decline in women than men. Psychiatry had been a more popular choice among women than men in the earlier cohorts; and the decline from early to late cohorts was greater in women than men (Table 1, Fig. DS1 and Table DS1). Against the general trend in first-year choices, there was a slight upturn in the 2008 and 2009 cohorts in year 1 (Table 1, Fig. DS1 and Table DS1).
Definite, probable and uncertain choices
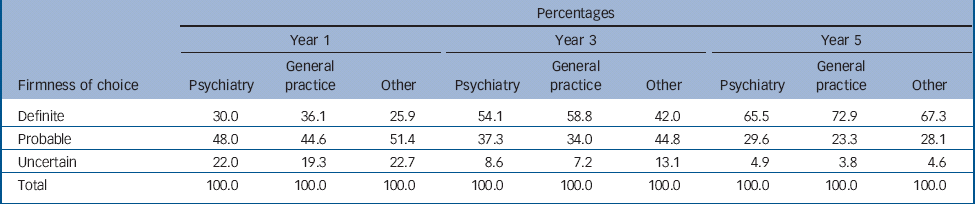
We compared certainty of choice between aspiring psychiatrists and those who gave their first choice as general practice or a non-psychiatric hospital specialty (Table 2 and online Table DS2). In years 1, 3 and 5, those who chose psychiatry were less certain about their career preference than those who chose general practice, but more certain than doctors who chose other hospital specialties.
Choices by medical school
Choices for psychiatry varied little by medical school attended (online Table DS3). Comparing year-1 choices for the 23 schools on which we had more than 1 year's data, and taking a cut-off of P = 0.01 for significance, one school was significantly high and two were significantly low (Table DS3). At year 3, no school was significantly high or low. At year 5, one school was significantly low and two were significantly high. There was an indication in the results that a slightly higher percentage of graduates from Scotland and Northern Ireland favoured a career in psychiatry (Table DS3).
Factors influencing career choice
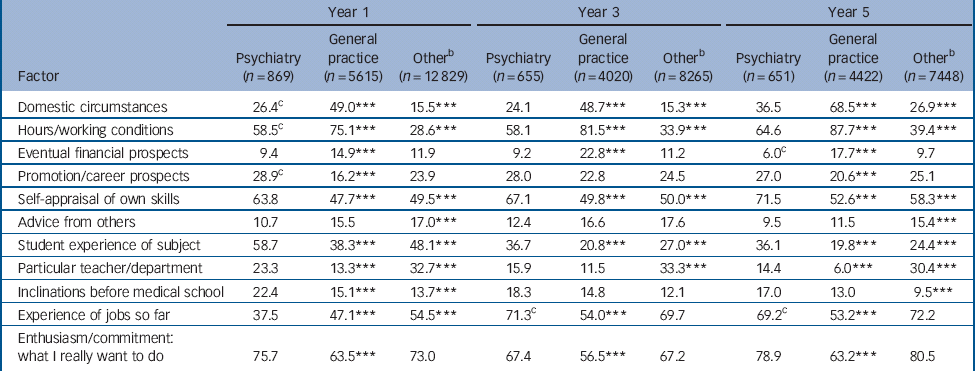
In year 1, three-quarters of respondents rated ‘enthusiasm/commitment: what I really want to do’ as influencing their choice of psychiatry a great deal (Table 3 and online Table DS4). ‘Self-appraisal of own skills’, ‘student experience of subject’ and ‘hours/working conditions’ were rated as having a great deal of influence by over half of respondents. ‘Self-appraisal of own skills’, ‘student experience of subject’ and ‘inclinations before medical school’ were rated as having a ‘great deal of influence’ by a higher percentage of aspiring psychiatrists than of those who chose general practice or other hospital specialties. ‘Hours/working conditions’ were rated as influential by a higher percentage of doctors who chose psychiatry than those who chose other hospital specialties. Women who chose psychiatry rated ‘domestic circumstances’ as having influenced their choice a ‘great deal’ more than did men (33% of women, 18% of men; χ2 1 = 20.3, P<0.001). Women who chose psychiatry rated ‘hours/working conditions’ as more influential on their career choice than did men (62% of women, 54% of men; χ2 1 = 5.1, P<0.05). Men who chose psychiatry rated ‘promotion/career prospects’ as influential, more so than did women (33% of men, 25% of women; χ2 1 = 5.1, P<0.05).
Table 2 Comparison between doctors who chose psychiatry, general practice or other clinical specialties: percentages of doctors who specified that they were ‘definite’, ‘probable’ or ‘uncertain’ about their first choice of long-term career, at 1, 3 and 5 years after graduation
| Percentages | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Year 1 | Year 3 | Year 5 | |||||||
| Firmness of choice | Psychiatry | General practice |
Other | Psychiatry | General practice |
Other | Psychiatry | General practice |
Other |
| Definite | 30.0 | 36.1 | 25.9 | 54.1 | 58.8 | 42.0 | 65.5 | 72.9 | 67.3 |
| Probable | 48.0 | 44.6 | 51.4 | 37.3 | 34.0 | 44.8 | 29.6 | 23.3 | 28.1 |
| Uncertain | 22.0 | 19.3 | 22.7 | 8.6 | 7.2 | 13.1 | 4.9 | 3.8 | 4.6 |
| Total | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 |
Table 3 Percentages of doctors who specified each factor as influencing their choice of long-term career a great deal: graduates of 1993, 1996, 1999, 2000, 2002, 2008 and 2009Footnote a
| Year 1 | Year 3 | Year 5 | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Factor | Psychiatry (n = 869) |
General practice (n = 5615) |
OtherFootnote
b
(n = 12 829) |
Psychiatry (n = 655) |
General practice (n = 4020) |
OtherFootnote
b
(n = 8265) |
Psychiatry (n = 651) |
General practice (n = 4422) |
OtherFootnote
b
(n = 7448) |
| Domestic circumstances | 26.4Footnote c | 49.0Footnote *** | 15.5Footnote *** | 24.1 | 48.7Footnote *** | 15.3Footnote *** | 36.5 | 68.5Footnote *** | 26.9Footnote *** |
| Hours/working conditions | 58.5Footnote c | 75.1Footnote *** | 28.6Footnote *** | 58.1 | 81.5Footnote *** | 33.9Footnote *** | 64.6 | 87.7Footnote *** | 39.4Footnote *** |
| Eventual financial prospects | 9.4 | 14.9Footnote *** | 11.9 | 9.2 | 22.8Footnote *** | 11.2 | 6.0Footnote c | 17.7Footnote *** | 9.7 |
| Promotion/career prospects | 28.9Footnote c | 16.2Footnote *** | 23.9 | 28.0 | 22.8 | 24.5 | 27.0 | 20.6Footnote *** | 25.1 |
| Self-appraisal of own skills | 63.8 | 47.7Footnote *** | 49.5Footnote *** | 67.1 | 49.8Footnote *** | 50.0Footnote *** | 71.5 | 52.6Footnote *** | 58.3Footnote *** |
| Advice from others | 10.7 | 15.5 | 17.0Footnote *** | 12.4 | 16.6 | 17.6 | 9.5 | 11.5 | 15.4Footnote *** |
| Student experience of subject | 58.7 | 38.3Footnote *** | 48.1Footnote *** | 36.7 | 20.8Footnote *** | 27.0Footnote *** | 36.1 | 19.8Footnote *** | 24.4Footnote *** |
| Particular teacher/department | 23.3 | 13.3Footnote *** | 32.7Footnote *** | 15.9 | 11.5 | 33.3Footnote *** | 14.4 | 6.0Footnote *** | 30.4Footnote *** |
| Inclinations before medical school | 22.4 | 15.1Footnote *** | 13.7Footnote *** | 18.3 | 14.8 | 12.1 | 17.0 | 13.0 | 9.5Footnote *** |
| Experience of jobs so far | 37.5 | 47.1Footnote *** | 54.5Footnote *** | 71.3Footnote c | 54.0Footnote *** | 69.7 | 69.2Footnote c | 53.2Footnote *** | 72.2 |
| Enthusiasm/commitment: what I really want to do | 75.7 | 63.5Footnote *** | 73.0 | 67.4 | 56.5Footnote *** | 67.2 | 78.9 | 63.2Footnote *** | 80.5 |
a. The numbers for this table are provided in online Table DS4.
b. Other hospital specialties (i.e. all hospital specialties other than psychiatry).
c. Significant difference between men and women within the group that chose psychiatry.
*** P<0.001 when compared with psychiatry.
By the third year after graduation, ‘experience of jobs so far’ was rated as the most influential factor. Women who chose psychiatry rated this as having had more influence than did men (77% of women, 63% of men; χ2 1 = 6.9, P<0.01). By the fifth year ‘enthusiasm/commitment’ was rated most important. Women who chose psychiatry continued to rate ‘experience of jobs so far’ as influential in higher numbers than did men (73% of women, 65% of men; χ2 1 = 4.2, P<0.05). ‘Student experience of subject’ was more important for those choosing psychiatry than those who chose general practice or other hospital specialties across all three periods after qualification.
Doctors who considered psychiatry as a career and then decided not to pursue it
This part of the study was based on questionnaires that had been sent to 16 361 doctors who had qualified in 2002, 2005 or 2008. The percentage of respondents who specified that they had seriously considered but then not pursued a specialty were very similar in the successive cohorts: this was specified by 29% (797/2778) of graduates in 2002, 27% (843/3128) in 2005, and 29% (933/3249) in 2008. After exclusions of statements that could not be coded, and doctors whose switches of specialty were within the same broader specialty group (e.g. between different branches of hospital medicine or surgery, as described elsewhere Reference Goldacre, Goldacre and Lambert9 ), there were 2267 respondents – 811 men and 1456 women – who had considered and rejected a specialty and who gave at least one classifiable reason for doing so (25% of the total number of respondents).
Of the 2267 respondents, 99 (4.4%) specified that they had considered and then decided not to pursue psychiatry (4.2% of men, 4.5% of women, a very similar percentage to those who chose it, Table 1). There was no significant upward or downward trend across the cohorts in the percentage that considered and rejected psychiatry: it was 4.8% in the 2002 cohort, 3.7% in 2005 and 4.7% in 2008.
Reasons for rejecting psychiatry, after having seriously considered it as a career
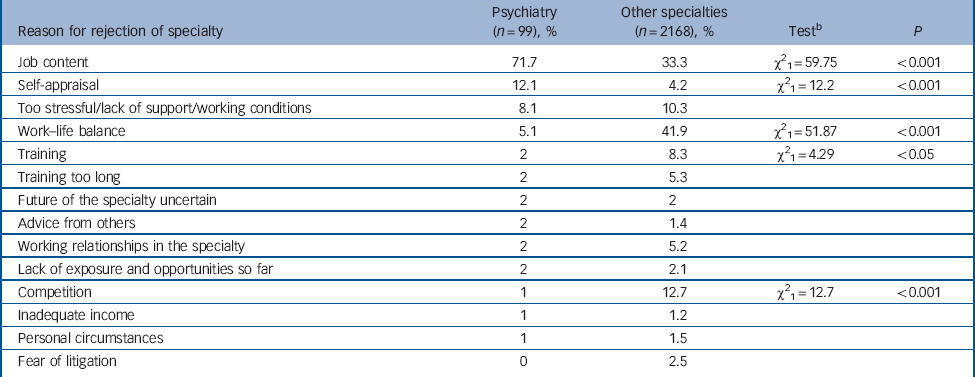
We compared the reasons for rejecting a specialty given by doctors who rejected psychiatry with those given by the 2168 doctors who had seriously considered but then decided not to pursue other specialties. Statements that we classified as ‘job content’ were given by 71% of the doctors who rejected psychiatry and by 33% of doctors who rejected other specialties (Table 4 and online Table DS5).
Illustrative examples of comments that we coded as ‘job content’ are reproduced, exactly as written by the doctors, in Appendix 2.
Twelve per cent of doctors who rejected psychiatry and four per cent of those who rejected other specialties gave reasons that we classified as ‘self-appraisal’ (Appendix 2). All other reasons, such as those relating to competition, training and working relationships within the specialty were mentioned by less than 10% of doctors rejecting psychiatry. ‘Work–life balance’ was the most frequently mentioned reason given by those rejecting specialties other than psychiatry (41%), but was only mentioned by 5% of those rejecting psychiatry.
Table 4 Percentage distribution of reasons given for rejecting psychiatry and for rejecting all other specialties combinedFootnote a
| Reason for rejection of specialty | Psychiatry (n = 99), % |
Other specialties (n = 2168), % |
TestFootnote b | P |
|---|---|---|---|---|
| Job content | 71.7 | 33.3 | χ2 1 = 59.75 | <0.001 |
| Self-appraisal | 12.1 | 4.2 | χ2 1 = 12.2 | <0.001 |
| Too stressful/lack of support/working conditions | 8.1 | 10.3 | ||
| Work–life balance | 5.1 | 41.9 | χ2 1 = 51.87 | <0.001 |
| Training | 2 | 8.3 | χ2 1 = 4.29 | <0.05 |
| Training too long | 2 | 5.3 | ||
| Future of the specialty uncertain | 2 | 2 | ||
| Advice from others | 2 | 1.4 | ||
| Working relationships in the specialty | 2 | 5.2 | ||
| Lack of exposure and opportunities so far | 2 | 2.1 | ||
| Competition | 1 | 12.7 | χ2 1 = 12.7 | <0.001 |
| Inadequate income | 1 | 1.2 | ||
| Personal circumstances | 1 | 1.5 | ||
| Fear of litigation | 0 | 2.5 |
a. Some doctors gave more than one reason and we counted each reason.
b. Significance tests, comparing those rejecting psychiatry and those rejecting other specialties.
Choosing psychiatry, following rejection of another specialty
Of the doctors who had considered and rejected a specialty other than psychiatry, 4% then chose psychiatry. This is exactly in line with doctors' general level of choice for psychiatry (Table 1).
Discussion
Early career choices for psychiatry
In the UK, until recently, newly qualified doctors undertook a ‘house officer’ year of working in a medical post and a surgical post under supervision, and then undertook a variable number of posts (depending on the wishes of individual doctors and their success in applications) before entering training for their choice of career specialty. A new programme of postgraduate medical training was introduced in the UK in 2005 which replaced the single ‘house officer’ year with two ‘foundation years’ before specialising. Prior to 2005, doctors could make their final career choice several years after graduation. It is now expected that most doctors will choose their broad area of specialty training, such as psychiatry, in their second postgraduate year so that they can start specialty training in their third year after graduation.
One year after graduation, about 4% of doctors chose psychiatry as their first choice of eventual career, similar to the 3–4% of doctors entering psychiatry in the USA between 1992 and 2002 Reference Sierles, Yager and Weissman10 and 4% entering US psychiatry residency training in 2007. Reference Salsberg, Rockey, Rivers, Brotherton and Jackson3 In the UK, the percentage of men who chose psychiatry has been consistent over the past 25 years. Previously, a higher percentage of women than men doctors in the UK have become psychiatrists. However, there has been a decline in choices for psychiatry made by women over the past decade, with a small increase in the last two surveys. Hours of work in medicine have been falling in the UK, following the implementation of European working time regulations, and working practices are considered to have become more ‘family friendly’ – aspects of working as a psychiatrist that have made it popular for women. Reference Taylor, Lambert and Goldacre11 These changes to medicine will probably make some specialties more attractive to women doctors in the future than they have been in the past. If psychiatry loses its historical competitive edge with women, recruitment overall may worsen.
We have shown elsewhere that there is a high level of correspondence between early career choices for psychiatry and eventual destinations in the specialty. Reference Goldacre, Laxton and Lambert12 In that publication, we showed that 75% who chose psychiatry in the first year after qualification eventually practised in it, as did 93% and 97% of those who specified it as their first choice at 3 and 5 years respectively after qualification. An early career choice for psychiatry is therefore highly predictive of an eventual career in the specialty.
Influences of medical school
A recent review of the impact of undergraduate experiences on recruitment into psychiatry highlighted an enthusiasm for psychiatry in school that dissipates once the student is in medical school. Reference Eagles, Wilson, Murdoch and Brown13 These authors listed factors which may dissuade medical students from choosing psychiatry. These included insufficient exposure to psychiatry in medical school, and a lack of status for psychiatry among peers. It has been suggested that efforts to increase the number of doctors choosing psychiatry might focus on medical schools which produce a smaller than average percentage of doctors wanting to pursue psychiatry. 14 In our study, differences between medical schools were not particularly striking, although a higher percentage of doctors from medical schools in Scotland and Northern Ireland seem attracted to psychiatry. The extent to which these higher percentages reflect the characteristics of students selected at entry to medical school, and/or the influence of medical education, needs further examination. The degree to which different medical schools within other countries vary in their rates of recruitment into psychiatry is also an area for further study.
Factors influencing career choice for psychiatry
The factor cited as having a great deal of influence by the highest percentage of intending psychiatrists in year 1 was ‘What I really want to do’. This was specified by 76% of intending psychiatrists, and it was a significantly higher level of enthusiasm for their specialty than that expressed by intending doctors for general practice. Three factors had a greater influence on career choice for psychiatry than on doctors' choice for other clinical careers: the doctors' self-appraisal of their own skills, their inclinations before medical school (which is not scored highly for most specialties), and their experience of the subject as a student. These factors in combination indicate, at least for some choosing psychiatry, an early and strong interest in the specialty.
Professional bodies have suggested offering more work experience placements to secondary school students (i.e. those aged 16–18) as a way to improve recruitment into psychiatry. 14 Doctors' ‘experience of the job so far’ was less influential in year 1 for those choosing psychiatry than for those choosing other careers. The lack of work experience in the first year after medical graduation highlights the need for more doctors to spend time in a psychiatry placement in their early postgraduate years. Reference Collins15 Over the period covered by these studies, particularly in the early period, policies were implemented in the UK to emphasise community care for psychiatric patients and to reduce hospital in-patient admissions. This may have reduced the scope for junior doctors to gain experience of work in psychiatry in the hospital setting, and the change in work profile in psychiatry from in-patient to non-in-patient care may have had an impact on junior doctors' predilection for the specialty in ways that we cannot assess.
A study by Dein et al Reference Dein, Livingston and Bench16 asked consultant psychiatrists to specify the most important factors in their choice of career. The most important factors were empathy for patients, working conditions and experience of the subject as a student. However, their study included only psychiatrists and there was no element of comparison with other specialties. An Australian study of medical students found that the most important factors in career choice for psychiatry were that it was considered to be an interesting subject and intellectually challenging. Reference Malhi, Parker, Parker, Kirkby, Boyce and Yellowlees17
Factors deterring career choice for psychiatry: those who once considered it
On the one hand, it is important that medical students and junior doctors are given adequate early experience of psychiatry. On the other hand, exposure may discourage some doctors. Positive choices for psychiatry, in our study, were heavily influenced by the nature of the specialty, the doctors' experience of it, and the doctors' self-appraisal of whether psychiatry is the right specialty for them. However, a similar range of factors – job content of the specialty, experience of it, and reflection on it as a career – were also cited as negative factors that influenced some doctors who seriously considered psychiatry as a career but then decided not to pursue it. It seems likely that views about psychiatry may be more polarised than those for other specialties.
Another UK study of doctors who initially chose psychiatry but then pursued a different career found that lack of respect among peers and the public, perceived threats of violence from patients, lack of resources and low morale were dissuading factors. Reference Lambert, Turner, Fazel and Goldacre18 A survey of Australian medical students found that the least attractive aspects of psychiatry included its lack of prestige and ‘perceived absence of a scientific foundation’. Reference Malhi, Parker, Parker, Kirkby, Boyce and Yellowlees17 These negative perceptions of psychiatry have been cited elsewhere Reference Rajagopal, Rehill and Godfrey19,Reference Brown, Vassilas and Oakley20 and should be countered with real and good experiences of working in psychiatry during and after medical school. More importantly, the extent to which these factors can be altered by medical school education needs further investigation.
Future prospects
Although recruitment into psychiatry is difficult worldwide, demand for psychiatric services is increasing. Reference Katschnig21 The percentage of newly qualified doctors in the UK who choose psychiatry is below the level needed to replace the current generation of practising psychiatrists. 4,22 The number of UK applicants for training in psychiatry is lower than that for any other large specialty, Reference Fazel and Ebmeier23 and psychiatry in the UK is heavily reliant on the recruitment of international medical graduates. As in the UK, in the USA a substantial percentage of applications for psychiatry training/residency posts come from international medical graduates. Reference Salsberg, Rockey, Rivers, Brotherton and Jackson3
One of our main findings is that the proportion of medical students choosing psychiatry as a career has not changed appreciably since 1974. This is despite a decade of initiatives by the Royal College of Psychiatrists to increase recruitment into psychiatry. These initiatives, mostly targeted at medical students, have principally aimed to emphasise the biopsychosocial model in psychiatry, and have highlighted how psychiatry is one of a number of professions contributing to the care of psychiatric patients. Reference Brown, Vassilas and Oakley20 In contrast, a group of mostly academic psychiatrists Reference Craddock, Antebi, Attenburrow, Bailey, Carson and Cowen24 recently called for more emphasis on the medical model in the teaching of psychiatry, and argued that this would contribute to improving the number and quality of candidates for psychiatry training. Commentators have suggested that a lack of emphasis on medical models has fuelled perceptions that psychiatry may not have enough medical content to be attractive to many doctors. Reference Søndergård25 Although these views were not widely shared among psychiatrists, the extent to which changes to teaching and training of students and junior doctors in psychiatry alters perceptions about it, and choices for it, needs testing. Our qualitative data provide some support for the perceived lack of applicability of the medical model as a reason for rejecting psychiatry after having seriously considered it as a career option.
We found that experiences of psychiatry as a student and in early medical training were important in determining choices. Student experience and experience of jobs so far seemed to be more influential for psychiatry than is the case for general practice and other specialties. This suggests that provision of more experience of psychiatry in foundation years might encourage recruitment to psychiatry. In keeping with the role of student experience, we also found potentially important differences in the proportion choosing psychiatry by medical school, but also differences in retention rates by medical school. These findings underscore the importance of student and early training experiences.
Strengths and limitations
The study has several strengths: it covers 12 cohorts of newly qualified doctors from all UK medical schools, going as far back as 1974; it has a high response rate for this type of study; it can be considered as nationally representative of the UK; and it is a prospective cohort study and therefore not subject to recall bias about early career intentions. Career intentions, as they were in years 1, 3 and 5, were provided by the doctors contemporaneously. Its longitudinal design also means that doctors' replies 1 year post-qualification can be compared with their later replies in years 3 and 5.
The study's limitations include the fact that it is restricted to UK medical graduates. There are 2 years post-graduation in which UK doctors work mostly in general medicine and surgery, and the length of this type of early training/internship differs by country. The importance of early choice is likely to be stronger in countries such as the USA where residency choice is made earlier. There are a few gaps in our data coverage: for example, the absence of year-1 data between 1983 and 1993 is because the funding body, the Department of Health, ceased funding the surveys in this period. Non-responder bias is possible, as with all surveys. We did not ask those who did not choose psychiatry whether certain factors might have made them choose it. We asked individuals about preferences, but some who choose psychiatry may not get posts in it.
Appendix 1
Method for coding reasons for rejection of a specialty by theme
-
1. Each doctor's record includes a separate field for chosen specialty, rejected specialty (if any) and text comments on reasons for rejection, as well as for many other data items.
-
2. We selected records with a free-text comment about considering but then rejecting a specialty, for all specialties (not just psychiatry); and created a separate file containing the free text (and no other information). Accordingly, we were masked, in theme-scoring the comments, to the actual chosen specialty and the rejected specialty (although, of course, the doctors' text often mentioned them by name), gender, ethnicity and other personal data.
-
3. Two people independently read all the comments without a pre-conceived list of themes or coding schemes (i.e. using ‘grounded’ theory).
-
4. The themes were then agreed as those that had emerged from the totality of reading the comments.
-
5. The comments were then read again independently by two people, and scored as fitting a theme.
-
6. The two readers then compared their scoring of themes and any differences were resolved by discussion.
-
7. The themes were coded and then the additional information – chosen specialty, rejected specialty, whether the doctor was male or female, etc. – were added to the file of comments.
-
8. The records were analysed as those from doctors who specified that they had seriously considered, but then decided against trying for a career in (a) psychiatry and (b) all other specialties.
Appendix 2
Examples of statements about psychiatry
Job content
‘Negative experience as a medical student’
‘Unrewarding – difficult to make patients better’
‘Not challenging enough – pace too slow’
‘Fail to exercise majority of skills learnt as a medical student’
‘Not enough medicine – waste of my learning’
‘Realisation that practice different to theory’
‘Psychiatry in small amounts is ok – but would probably be too much if full time’
‘Experience in psychiatry as an F1 [Foundation Year 1, the first year after medical qualification] made me realise it was quite a narrow field that was too slow moving’
‘Enjoyed the subject greatly, but had numerous bad placements that put me off’
‘Violent patients’
‘Singular dislike of personality disorders’
Self-appraisal
‘Not suited to my personality’
‘Too depressing’
‘I feel physically scared of psychiatric patients’
‘Too emotionally demanding’









eLetters
No eLetters have been published for this article.