People with mental illness die prematurely. Reference Harris and Barraclough1-Reference Wahlbeck, Westman, Nordentoft, Gissler and Laursen3 One reason is that their physical healthcare is on average worse than that provided to people without mental health problems. 4 For example, people with mental illness have lower rates of coronary revascularisation, hospital admission for diabetes and basic assessments such as blood pressure measurement compared with people without a mental illness. Reference Druss, Bradford, Rosenheck, Radford and Krumholz5-Reference Roberts, Roalfe, Wilson and Lester8 There is a pressing need to improve understanding of the range of factors contributing to these inequalities. A potential mechanism underlying these disparities is discrimination against people with mental illness by health professionals who share the general public's stigmatising views towards such people. Reference Lauber, Anthony, Jdacic-Gross and Rossler9,Reference Patel10 In keeping with these findings, the 2008 Stigma Shout survey of almost 4000 people using mental health services and carers conducted by the mental health charity Rethink Mental Illness identified medical professionals as one of the most important groups for Time to Change to target, 11 and the Viewpoint survey showed that health professionals are a common source of experiences of discrimination reported by people with mental illness (see also Corker et al, this supplement). Reference Henderson, Corker, Lewis-Holmes, Hamilton, Flach and Rose12,Reference Corker, Hamilton, Henderson, Weeks, Pinfold and Rose13 Rethink Mental Illness has a track record of anti-stigma work with medical and nursing students, Reference Kassam, Glozier, Leese, Henderson and Thornicroft14-Reference Clement, van Nieuwenhuizen, Kassam, Flach, Lazarus and de Castro16 and this work was continued as a component of the Time to Change programme (phase one: 2008-2011), called Education Not Discrimination (END). The aim of this study was to ascertain the effects of the training on medical students both immediately and after 6 months with respect to mental health-related knowledge, attitudes, intended behaviour and empathy. We predicted that there would be significantly greater improvement among intervention participants relative to control participants at immediate and 6-month follow-up for each of these outcomes.
Method
The END intervention for medical students was implemented between 2008 and 2011 at four medical schools in different regions of England. It was delivered as part of the medical training at the universities but participation was voluntary, as was participation in the study. The intervention had previously been delivered at one medical school and was based on previous work with police officers that combined educational and social contact elements. Reference Kassam, Glozier, Leese, Henderson and Thornicroft14,Reference Kassam, Glozier, Leese, Loughran and Thornicroft15,Reference Pinfold, Huxley, Thornicroft, Farmer, Toulmin and Graham17-Reference Thornicroft, Rose and Kassam19 It consisted of a short lecture with key facts and figures about stigma and discrimination; testimonies about the experiences of mental health problems and stigma from people with direct experience of mental health problems, either personally or as carers; and role-plays in small groups, using professional role-players to act the parts of service users and carers. Medical students volunteered to role-play themselves in a medical history-taking scenario. Fellow students and actors then provided feedback after the role-play.
Measures
We used the following measures to assess mental health-related knowledge, attitudes, intended behaviour and empathy at three time points: baseline, immediate follow-up and 6-month follow-up.
Knowledge
Mental health-related knowledge was measured with the Mental Health Knowledge Schedule (MAKS). Reference Evans-Lacko, Little, Meltzer, Rose, Rhydderch and Henderson20 This comprised six items covering stigma-related mental health knowledge areas (help-seeking, recognition, support, employment, treatment and recovery) and six items that enquired about classification of various conditions as mental illnesses. Reference Rusch, Evans-Lacko and Thornicroft21 Overall test-retest reliability of the MAKS was 0.71 and the overall internal consistency among items was 0.65. Reference Evans-Lacko, Little, Meltzer, Rose, Rhydderch and Henderson20 The total score was calculated so that higher MAKS scores indicated greater knowledge.
Attitudes
Mental health-related attitudes were measured using three items from the Community Attitudes toward the Mentally Ill (CAMI) scale: Reference Taylor and Dear22
-
(a) one of the main causes of mental illness is a lack of self-discipline and will-power;
-
(b) there is something about people with mental illness that makes it easy to tell them from normal people;
-
(c) it is frightening to think of people with mental problems living in residential neighbourhoods.
The choice of these particular items was made in cooperation with those facilitating and running the intervention so that they would specifically capture the defined attitude changes that were targeted by the intervention. On a five-point Likert scale participants were asked to indicate whether they agreed or disagreed with the three statements.
Behaviour
Behaviour was measured by the Reported and Intended Behaviour Scale (RIBS). Reference Evans-Lacko, Rose, Little, Flach, Rhydderch and Henderson23 We assessed changes in intended behaviour in four different contexts (living with, working with, living nearby and continuing a relationship with someone with a mental health problem) which were derived from the Star Social Distance Scale. Reference Phillips24,Reference Link, Yang, Phelan and Collins25 Overall test-retest reliability of the RIBS was 0.75 and its overall internal consistency was 0.85. The total intended behaviour score was calculated, with higher scores indicating more favourable intended behaviour.
Empathy
Four items from the Jefferson Scale of Physician Empathy were used. Reference Hojat, Gonnella, Nasca, Mangione, Veloksi and Magee26 These items tested awareness of the importance of the emotional status of the patients and their family; understanding the impact of emotional ties to their patient for healing; willingness to disclose mental health problems as linked to the fear of being treated differently; and feeling comfortable talking to a person with mental health problems. On a seven-point Likert scale the participants were asked to agree or disagree with empathy-related statements. In a previous psychometric study the internal consistency reliability of the Jefferson empathy scale was found to be 0.89 for medical students. Reference Hojat, Gonnella, Nasca, Mangione, Veloksi and Magee26
Timing of assessments
Immediately before the first part of the intervention (lecture and testimonies) participants completed the baseline questionnaire including all four stigma measures in addition to sociodemographic details (date of birth, gender and ethnic origin). Participants completed the first follow-up immediately after the second and last part of the intervention (the role-play). Six months later participants were asked by email to complete the online follow-up questionnaire, a link to which was provided in the email. Participants in the control group did not receive any of the END intervention and received their standard medical school curriculum.
Participants
The study inclusion criteria were being a third-year medical student enrolled at one of the four participating medical schools, providing a valid email address for the online follow-up and giving valid written consent. Potential participants were contacted by their schools in advance about the intervention and the planned study before being recruited to the study at the sites where they received teaching. The lecture and the testimony that comprised the END intervention were scheduled in the educational plan for the students but the intervention did not constitute obligatory modules of their training. Researchers (either from the Institute of Psychiatry or the Mental Health Research Network) collected data from study participants who attended the initial part of the intervention (lecture and testimony). Before the start of the lecture, an information sheet, consent form and baseline questionnaire were distributed to the participants and collected immediately after completion. Approval was obtained from the King's College London research ethics committee.
Control participants were recruited from two sites. At one university, students were randomised by the academic registry to either intervention or control group. At another, two out of six student groups based at different sites were recruited to the control group.
Statistical analysis
We calculated total scores for the MAKS, RIBS and empathy scales by adding the respective items so that a higher total score would represent less stigmatising responses. The CAMI scores were not added but were analysed at item level. Score changes were measured at two time comparison points: the change between baseline and immediate follow-up, and the change between baseline and 6-month follow-up. Separate linear regression models were used to investigate changes in knowledge, attitude, intended behaviour and empathy outcomes at both follow-up points. Covariates used in the regression model included group membership (control v. intervention), age (continuous), gender (male v. female), ethnicity (Black and minority ethnic v. others) and the respective baseline scores. We calculated the adjusted and unadjusted values (i.e. univariate and multivariate regressions).
Results
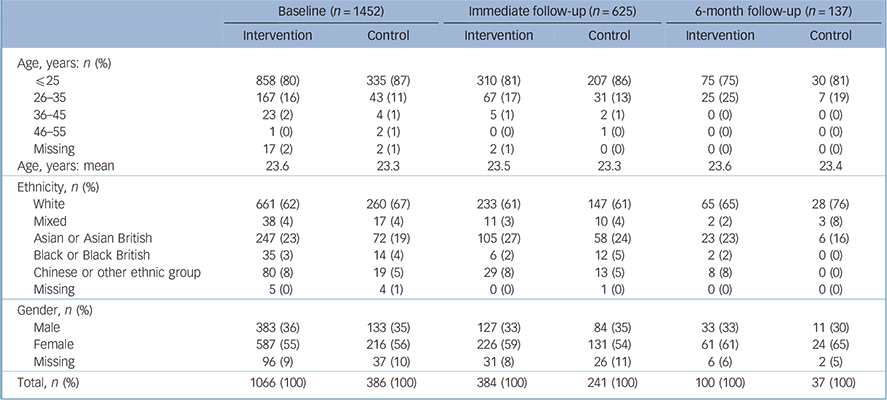
Table 1 describes the demographic characteristics of the participants. Most participants were aged 25 years or younger (mean 23.5 years), White and female. Chi-squared tests were calculated to establish whether there were any demographic differences between the intervention group and the control group. Compared with the intervention group, the control group had more people in the lower age categories: χ2(4,n = 1433) = 10.1, P = 0.04. With this exception, the demographic profiles of the control and intervention groups were similar. Chi-squared tests were also calculated to investigate whether there was systematic drop-out between baseline and follow-up for control v. intervention group. Only one of the chi squared tests was significant: Black and minority ethnic (BME) participants were more likely than White participants to take part in the immediate follow-up: χ2(1,n = 1443) = 4.1, P = 0.05. There was no other difference in drop-out rates for the immediate follow-up or the 6-month follow-up in terms of the demographic variables collected.
Table 1 Demographic data for the sample at baseline and follow-up
| Baseline (n = 1452) | Immediate follow-up (n = 625) | 6-month follow-up (n = 137) | ||||
|---|---|---|---|---|---|---|
| Intervention | Control | Intervention | Control | Intervention | Control | |
| Age, years: n (%) | ||||||
| ⩽25 | 858 (80) | 335 (87) | 310 (81) | 207 (86) | 75 (75) | 30 (81) |
| 26-35 | 167 (16) | 43 (11) | 67 (17) | 31 (13) | 25 (25) | 7 (19) |
| 36-45 | 23 (2) | 4 (1) | 5 (1) | 2 (1) | 0 (0) | 0 (0) |
| 46-55 | 1 (0) | 2 (1) | 0 (0) | 1 (0) | 0 (0) | 0 (0) |
| Missing | 17 (2) | 2 (1) | 2 (1) | 0 (0) | 0 (0) | 0 (0) |
| Age, years: mean | 23.6 | 23.3 | 23.5 | 23.3 | 23.6 | 23.4 |
| Ethnicity, n (%) | ||||||
| White | 661 (62) | 260 (67) | 233 (61) | 147 (61) | 65 (65) | 28 (76) |
| Mixed | 38 (4) | 17 (4) | 11 (3) | 10 (4) | 2 (2) | 3 (8) |
| Asian or Asian British | 247 (23) | 72 (19) | 105 (27) | 58 (24) | 23 (23) | 6 (16) |
| Black or Black British | 35 (3) | 14 (4) | 6 (2) | 12 (5) | 2 (2) | 0 (0) |
| Chinese or other ethnic group | 80 (8) | 19 (5) | 29 (8) | 13 (5) | 8 (8) | 0 (0) |
| Missing | 5 (0) | 4 (1) | 0 (0) | 1 (0) | 0 (0) | 0 (0) |
| Gender, n (%) | ||||||
| Male | 383 (36) | 133 (35) | 127 (33) | 84 (35) | 33 (33) | 11 (30) |
| Female | 587 (55) | 216 (56) | 226 (59) | 131 (54) | 61 (61) | 24 (65) |
| Missing | 96 (9) | 37 (10) | 31 (8) | 26 (11) | 6 (6) | 2 (5) |
| Total, n (%) | 1066 (100) | 386 (100) | 384 (100) | 241 (100) | 100 (100) | 37 (100) |
Knowledge
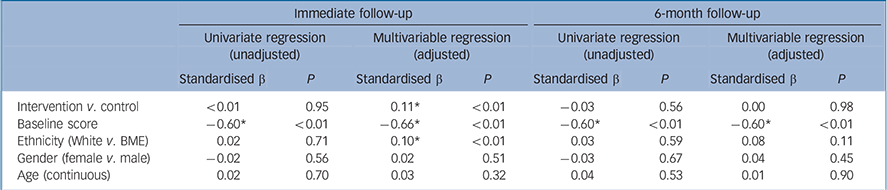
Compared with those in the control group, those in the intervention group had significantly greater improvements in mental health-related knowledge at immediate follow-up. Immediate improvement in knowledge was also associated with lower baseline score and non-BME ethnicity. Those in the intervention group did not show greater improvements in knowledge at the 6-month follow-up compared with controls. The baseline MAKS score, however, predicted the improvement, with individuals with a lower baseline MAKS score showing greater improvements (Table 2).
Table 2 Predictors of mental health-related knowledge improvements at follow-up (linear regression)
| Immediate follow-up | 6-month follow-up | |||||||
|---|---|---|---|---|---|---|---|---|
| Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
|||||
| Standardised β | P | Standardised β | P | Standardised β | P | Standardised β | P | |
| Intervention v. control | <0.01 | 0.95 | 0.11Footnote * | <0.01 | –0.03 | 0.56 | 0.00 | 0.98 |
| Baseline score | –0.60Footnote * | <0.01 | –0.66Footnote * | <0.01 | –0.60Footnote * | <0.01 | –0.60Footnote * | <0.01 |
| Ethnicity (White v. BME) | 0.02 | 0.71 | 0.10Footnote * | <0.01 | 0.03 | 0.59 | 0.08 | 0.11 |
| Gender (female v. male) | –0.02 | 0.56 | 0.02 | 0.51 | –0.03 | 0.67 | 0.04 | 0.45 |
| Age (continuous) | 0.02 | 0.70 | 0.03 | 0.32 | 0.04 | 0.53 | 0.01 | 0.90 |
BME, Black and minority ethnic.
* P<0.05.
Attitude
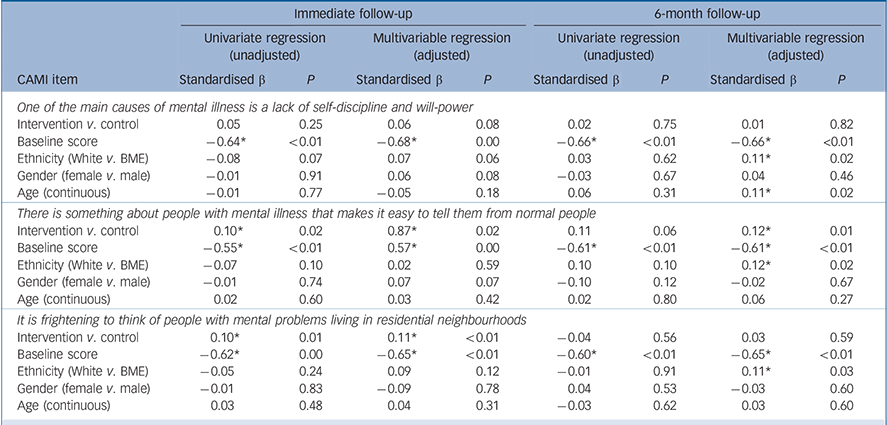
Compared with the control group, those in the intervention group had significantly greater improvements in mental health-related attitudes at immediate follow-up for two of the three CAMI items (‘There is something about people with mental illness that makes it easy to tell them from normal people’ and ‘It is frightening to think of people with mental problems living in residential neighbourhoods’). Furthermore, the baseline score predicted the short-term changes for all attitude items, with the greatest improvements occurring in the people with lower baseline scores. At 6 months' follow-up attitudinal improvement was significantly better among those in the intervention group for the second attitude item only (‘There is something about people with mental illness that makes it easy to tell them from normal people’). For all three CAMI items, White ethnicity and lower baseline CAMI score were also significant predictors of greater improvement (Table 3). Older age was associated with significantly greater improvement in the first attitude item (‘One of the main causes of mental illness is a lack of self-discipline and will-power’).
Table 3 Predictors of mental health-related attitude improvements at follow-up (linear regression)
| Immediate follow-up | 6-month follow-up | |||||||
|---|---|---|---|---|---|---|---|---|
| Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
|||||
| CAMI item | Standardised β | P | Standardised β | P | Standardised β | P | Standardised β | P |
| One of the main causes of mental illness is a lack of self-discipline and will-power | ||||||||
| Intervention v. control | 0.05 | 0.25 | 0.06 | 0.08 | 0.02 | 0.75 | 0.01 | 0.82 |
| Baseline score | –0.64Footnote * | <0.01 | –0.68Footnote * | 0.00 | –0.66Footnote * | <0.01 | –0.66Footnote * | <0.01 |
| Ethnicity (White v. BME) | –0.08 | 0.07 | 0.07 | 0.06 | 0.03 | 0.62 | 0.11Footnote * | 0.02 |
| Gender (female v. male) | –0.01 | 0.91 | 0.06 | 0.08 | –0.03 | 0.67 | 0.04 | 0.46 |
| Age (continuous) | –0.01 | 0.77 | –0.05 | 0.18 | 0.06 | 0.31 | 0.11Footnote * | 0.02 |
| There is something about people with mental illness that makes it easy to tell them from normal people | ||||||||
| Intervention v. control | 0.10Footnote * | 0.02 | 0.87Footnote * | 0.02 | 0.11 | 0.06 | 0.12Footnote * | 0.01 |
| Baseline score | –0.55Footnote * | <0.01 | 0.57Footnote * | 0.00 | –0.61Footnote * | <0.01 | –0.61Footnote * | <0.01 |
| Ethnicity (White v. BME) | –0.07 | 0.10 | 0.02 | 0.59 | 0.10 | 0.10 | 0.12Footnote * | 0.02 |
| Gender (female v. male) | –0.01 | 0.74 | 0.07 | 0.07 | –0.10 | 0.12 | –0.02 | 0.67 |
| Age (continuous) | 0.02 | 0.60 | 0.03 | 0.42 | 0.02 | 0.80 | 0.06 | 0.27 |
| It is frightening to think of people with mental problems living in residential neighbourhoods | ||||||||
| Intervention v. control | 0.10Footnote * | 0.01 | 0.11Footnote * | <0.01 | –0.04 | 0.56 | 0.03 | 0.59 |
| Baseline score | –0.62Footnote * | 0.00 | –0.65Footnote * | <0.01 | –0.60Footnote * | <0.01 | –0.65Footnote * | <0.01 |
| Ethnicity (White v. BME) | –0.05 | 0.24 | 0.09 | 0.12 | –0.01 | 0.91 | 0.11Footnote * | 0.03 |
| Gender (female v. male) | –0.01 | 0.83 | –0.09 | 0.78 | 0.04 | 0.53 | –0.03 | 0.60 |
| Age (continuous) | 0.03 | 0.48 | 0.04 | 0.31 | –0.03 | 0.62 | 0.03 | 0.60 |
BME, Black and minority ethnic; CAMI, Community Attitudes toward the Mentally Ill.
* P<0.05
Intended behaviour
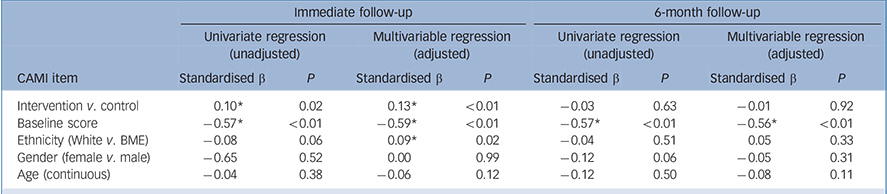
Participants in the intervention group had a significantly greater improvement in intended behaviour at immediate follow-up relative to participants in the control group. Additionally, those with a lower baseline RIBS score and White participants (compared with the BME group) had a significantly greater CAMI score at immediate follow-up. Intervention and control participants did not have significantly different long-term changes at 6-month follow-up. Only lower baseline RIBS score was associated with greater improvements in RIBS score at 6-month follow-up (Table 4).
Table 4 Predictors of mental health-related intended behaviour at follow-up (linear regression)
| Immediate follow-up | 6-month follow-up | |||||||
|---|---|---|---|---|---|---|---|---|
| Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
|||||
| CAMI item | Standardised β | P | Standardised β | P | Standardised β | P | Standardised β | P |
| Intervention v. control | 0.10Footnote * | 0.02 | 0.13Footnote * | <0.01 | –0.03 | 0.63 | –0.01 | 0.92 |
| Baseline score | –0.57Footnote * | <0.01 | –0.59Footnote * | <0.01 | –0.57Footnote * | <0.01 | –0.56Footnote * | <0.01 |
| Ethnicity (White v. BME) | –0.08 | 0.06 | 0.09Footnote * | 0.02 | –0.04 | 0.51 | 0.05 | 0.33 |
| Gender (female v. male) | –0.65 | 0.52 | 0.00 | 0.99 | –0.12 | 0.06 | –0.05 | 0.31 |
| Age (continuous) | –0.04 | 0.38 | –0.06 | 0.12 | –0.12 | 0.50 | –0.08 | 0.11 |
BME, Black and minority ethnic; CAMI, Community Attitudes toward the Mentally Ill.
* P<0.05.
Empathy
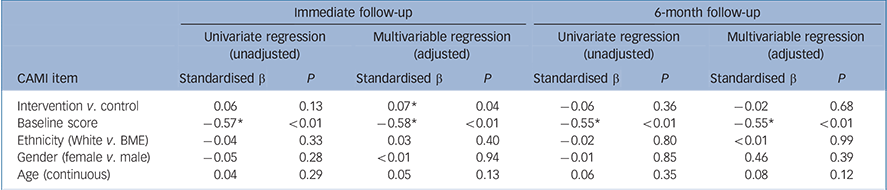
Empathy increased significantly more in people who participated in the intervention at immediate follow-up. Furthermore, lower baseline empathy score was associated with greater changes in empathy at immediate follow-up. At the 6-month follow-up, however, only lower baseline empathy score was associated with a greater improvement in empathy (Table 5).
Table 5 Predictors of physician empathy at follow-up (linear regression)
| Immediate follow-up | 6-month follow-up | |||||||
|---|---|---|---|---|---|---|---|---|
| Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
Univariate regression (unadjusted) |
Multivariable regression (adjusted) |
|||||
| CAMI item | Standardised β | P | Standardised β | P | Standardised β | P | Standardised β | P |
| Intervention v. control | 0.06 | 0.13 | 0.07Footnote * | 0.04 | –0.06 | 0.36 | –0.02 | 0.68 |
| Baseline score | –0.57Footnote * | <0.01 | –0.58Footnote * | <0.01 | –0.55Footnote * | <0.01 | –0.55Footnote * | <0.01 |
| Ethnicity (White v. BME) | –0.04 | 0.33 | 0.03 | 0.40 | –0.02 | 0.80 | <0.01 | 0.99 |
| Gender (female v. male) | –0.05 | 0.28 | <0.01 | 0.94 | –0.01 | 0.85 | 0.46 | 0.39 |
| Age (continuous) | 0.04 | 0.29 | 0.05 | 0.13 | 0.06 | 0.35 | 0.08 | 0.12 |
BME, Black and minority ethnic; CAMI, Community Attitudes toward the Mentally Ill.
* P<0.05.
Discussion
The results show significantly greater improvements at immediate follow-up for all stigma-related outcomes - mental health-related knowledge, attitudes, intended behaviour and empathy - among medical students receiving the Time to Change END intervention relative to those in the control group. However, this advantage did not persist. Six months following the intervention only one attitude item was associated with a greater improvement in the intervention group relative to the control group. This is a matter of concern which requires consideration.
One explanation for the short-term nature of its impact is that the intervention coincided with the start of the psychiatric rotation for both groups, the impact of which may have nullified any effect on the outcomes of the END training. Evaluation of previous similar interventions with medical students also showed that it was effective in improving knowledge at 1 week, Reference Kassam, Glozier, Leese, Loughran and Thornicroft15 whereas police officers reported that the intervention they received helped them improve their communication with people with mental health problems and increased their confidence to support people in mental distress. Reference Pinfold, Thornicroft, Huxley and Farmer18 However, the intervention with the police had no impact on the extent of their endorsement of the stereotype of people with mental illness as violent, suggesting that professional experience also has an influence on attitudes.
A second possible explanation for the decrease in difference at 6 months is that people in the control group might have been influenced by priming after having been prompted to answer questions on their mental health-related knowledge, attitudes, intended behaviour and empathy at baseline, resulting possibly in a short-term positive attitude shift which was diminished at the long-term follow up. Future studies might consider a Solomon group design to control for such effects. Reference Solomon27 Third, one might also consider the possibility that the training might have had a longer-lasting effect if it had been more specifically targeted towards medical students. In a qualitative assessment, medical students reported feeling somewhat patronised by the lecture's content because they felt that the factual knowledge and training on mental health problems received at their respective medical schools made this part of the intervention unnecessary. However, they felt more positive about the testimonies of people using mental health services, in that learning about the patient's perspective affected the students' attitudes and provided an insight into mental health topics that their formal education had not provided (details available from the author on request). Sadow & Ryder also found that a personal presentation from someone with experience of mental health treatment made a greater impact on attitudes of future health professionals than purely educational interventions. Reference Sadow and Ryder28 Fourth, external events such as influential news events or media stories (e.g. a reported shooting rampage by somebody who is described as having mental health problems) might have affected mental health-related stigma, potentially explaining similar changes in the intervention and control group as having influenced both groups alike. In this study, however, the observation periods for the different groups were staggered, being determined by the start of the respective psychiatric rotations for the different cohorts over 3 years.
On a more positive note, lower baseline scores were consistent predictors of greater improvements in knowledge, attitudes, intended behaviour and empathy at immediate follow-up and 6 months later. These findings suggest that those with more stigmatising attitudes towards mental health benefit most from the intervention. This is similar to a finding from Galletly & Burton, who showed that students with the most negative attitudes towards people with schizophrenia benefited most from an anti-stigma intervention and displayed the greatest improvement in attitudes. Reference Galletly and Burton29 Similar findings were demonstrated by the qualitative assessment of the END training, which suggested that the impact of the training depended on the knowledge, attitude, behaviour and empathy that the participants showed before participating in the training (details available from the author on request). This underlines the importance of identifying and targeting groups with a higher need for mental health-related education. At 6-month follow-up participants' attitudes in the BME group improved more than attitudes in the White group. These findings correspond to research reported by Knifton et al, who showed that there is a variety of need in mental health education between different ethnic groups, which might influence the efficacy of anti-stigma training. Reference Knifton, Gervais, Newbigging, Mirza, Quinn and Wilson30
Limitations
Control groups were only available at two of the four participating medical schools, so our control group may have differed from the intervention group in terms of variables other than the measured demographic characteristics we controlled for. Second, for feasibility the questionnaire had to be short, thus only three items from the CAMI were included instead of either the original scale or the shortened version used in the Attitudes to Mental Illness survey. Reference Mehta, Kassam, Leese, Butler and Thornicroft31 Further, as Bargh et al showed, Reference Bargh, Chaiken, Govender and Pratto32 attitudes are not always explicitly and consciously accessible and changeable, and this applies to mental health stigma. Last, we are unable to provide evidence on whether those who received the intervention would behave differently towards people with mental health problems in their clinical practice. Mechanisms and processes of stigma and discrimination have to be better understood to improve the efficacy of anti-stigma interventions. Reference Hinshaw and Stier33
Implications
Future research needs to investigate how it can be assured that positive changes prevail over time. First, although there is good evidence that interventions in the form of personal testimonies can be effective, Reference Clement, van Nieuwenhuizen, Kassam, Flach, Lazarus and de Castro16,Reference Pinfold, Thornicroft, Huxley and Farmer18,Reference Corrigan, River, Lundin, Penn, Uphoff-Wasowski and Campion34 it may be that different types of intervention content have differential effectiveness, in line with what has been found for public education campaigns. Reference Clement, Jarrett, Henderson and Thornicroft35 In this case research is required to establish what the most effective ingredients are. Second, it may be that ‘booster’ sessions are needed to maintain gains over time and this should be investigated further. A third possibility is greater integration between anti-stigma training and the rest of medical student education. If medical students learn negative attitudes and behaviour towards people with mental health problems from their role models, this will render training such as END ineffectual beyond its immediate impact. This potential problem is significant in the context of professional training based on the apprenticeship model; on the other hand, if doctors show leadership by tackling stigma and modelling non-discriminatory practice then the impact of training such as END could be better sustained.
Funding
The study was part funded by the Big Lottery Fund, Comic Relief and Shifting Attitudes to Mental Illness (SHiFT), UK government Department of Health, through their funding of the Time to Change programme. G.T. and C.H. are funded in relation to a National Institute for Health Research (NIHR) Applied Programme grant awarded to the South London and Maudsley NHS Foundation Trust (G.T.). D.R. and G.T. are also supported in relation to the NIHR Specialist Mental Health Biomedical Research Centre at the Institute of Psychiatry, King's College London and the South London and Maudsley NHS Foundation Trust (G.T.). C.H. is also funded by a grant from Guy's and St Thomas' Charity.
Acknowledgements
We thank the Education Not Discrimination team from Rethink Mental Illness for facilitating the data collection at interventions, and Sue Baker, Maggie Gibbons and Paul Farmer (Mind) and Paul Corry and Mark Davies (Rethink Mental Illness) for their collaboration. Further, we thank the Mental Health Research Network and other helpers for their invaluable support in collecting the data. We are also pleased to thank Paul Willams for advice regarding the databases and statistical analysis.










eLetters
No eLetters have been published for this article.