Since the start of the military campaigns in Afghanistan and Iraq, the psychological health of deployed UK military personnel has become a high-profile political concern and is much reported in the media. In addition, various aspects of military health, such as the effects of ‘overstretch’, Reference Rona, Fear, Hull, Greenberg, Earnshaw and Hotopf1 alcohol misuse Reference Fear, Iversen, Meltzer, Workman, Greenberg and Wessely2 and gender Reference Woodhead, Wessely, Jones, Fear and Hatch3 have been explored in scientific publications. However, most of the scientific work on this topic has been conducted with personnel who are stationed in their home bases either before or after deployment where there is a variable gap between returning home and completion of the survey. Asking personnel about what happened to them on deployment is likely to be affected by memory distortion. In order to find out more about deployment mental health and its support in high-threat areas, the US forces began surveying military personnel in their deployed location in 2003; 4 in 2009 the UK began to survey deployed military personnel in Iraq. Reference Mulligan, Jones, Woodhead, Davies, Wessely and Greenberg5 The result of this study (termed the Operational Mental Health Needs Evaluation Iraq or OMHNE I) suggested that the mental health of UK armed forces on deployment was similar to that reported during surveys of home-based personnel. Reference Hotopf, Hull, Fear, Browne, Horn and Iversen6,Reference Fear, Jones, Murphy, Hull, Iversen and Coker7 The OMNHE I found that 20.5% of deployed personnel reported symptoms of probable common mental disorder and 3.4% reported probable post-traumatic stress disorder (PTSD). As OMHNE I took place during the last phase of the UK’s military operations in Iraq, during which the operational threat level was much decreased compared with prior years, this contrasted sharply with the combat intensity experienced by UK armed forces personnel deployed in Afghanistan at that time. Therefore, in order to better understand the mental health impact of prolonged operations in a high-threat area, a further survey was carried out in the winter of 2010 among 1431 personnel deployed in Afghanistan (termed OMHNE A1). In this survey we found that 2.8% of personnel were experiencing probable PTSD and 17% reported symptoms of probable common mental disorder; we found that in addition to low levels of stress back at home, Reference Mulligan, Jones, Davies, McAllister, Fear and Wessely8 good mental health on deployment was related to supportive factors such as team cohesion and leadership. Reference Jones, Seddon, Fear, McAllister, Wessely and Greenberg9 A further survey of deployed personnel was carried out in Afghanistan during July and August 2011 (termed OMHNE A2). Unlike the OMHNE A1, the A2 survey was undertaken in the summer to take account of different climactic conditions and seasonal variations in combat intensity. During OMHNE A1, we were unable to carry out as much forward sampling as we would have desired as a major offensive operation was underway and transport assets were somewhat limited; no such restrictions were present during A2. Given that being in a forward area potentially limits access to medical, welfare and family support, we sought to assess whether location and combat environment had had an impact on mental health. This paper compares the mental health of UK personnel who took part in the A1 and A2 surveys while deployed to Afghanistan and assesses the impact on mental health of predeployment psychoeducation, family, welfare and medical support while taking account of the year of deployment.
Method
The OMHNE survey methodology is described in detail in our previous publications. Reference Mulligan, Jones, Woodhead, Davies, Wessely and Greenberg5,Reference Mulligan, Jones, Davies, McAllister, Fear and Wessely8,Reference Jones, Seddon, Fear, McAllister, Wessely and Greenberg9 On each occasion, the survey teams consisted of both military mental health professionals and general military personnel. Although the sampling was broadly representative of the deployed force, a decision was taken prior to each theatre visit to oversample potentially high-risk groups such as the Counter-IED Task Force (CIED-TF) (colloquially, but not militarily, known as bomb disposal personnel). A cluster-based, purposive sampling strategy was used to capture various groups as truly random sampling was not possible. The visit plans sought to ensure that the sampled locations were representative of the deployment profile of the overall force; however, this proved difficult during the 2010 visit as a consequence of major offensive combat operations that reduced the team’s ability to move freely between locations. As a result, fewer forward locations were visited than planned, such as check points and patrol bases positioned in more austere and exposed areas. In order to maximise the forward survey focus during A2, the survey team sought to ensure that as many forward locations as possible were visited and that personnel surveyed in relatively safe main operating bases were drawn from units that undertook frequent deployments to areas outside the base area.
During both surveys, fully informed signed consent to participate was obtained from participants who were given the opportunity to complete the survey anonymously if they wanted no further contact from the survey team. The core of the survey instrument was retained between visits to ensure that a robust comparison could be undertaken. Completed surveys were scanned using proprietary software, cleaned by the survey team and analysed before the visit end using SPSS version 15 for Windows.
In both surveys, the two main mental health outcome measures used were the 12-item General Health Questionnaire (GHQ-12) Reference Goldberg and Williams10 and the Post Traumatic Stress Disorder Checklist Civilian version (PCL-C). Reference Weathers, Litz, Herman, Huska and Keane11 Scores of 4 or more indicated that the respondent was a ‘case’ of probable common mental disorder on the GHQ-12 and a score of 50 or more indicated probable PTSD on the PCL-C. A PCL-C score of 30 or more was used to provide an estimate of the proportion of personnel reporting subthreshold through to probable PTSD caseness symptoms that may have been associated with functional impairment, Reference Rona, Jones, Iversen, Hull, Greenberg and Fear12 hereafter termed subthreshold PTSD. To determine the association of a range of variables with mental health overall, we combined the categories common mental disorder and PTSD into a single variable labelled ‘any mental health problem’. Self-rated general health was assessed with one question from the 36-item Short Form Health Survey (SF-36); ‘cases’ were defined as individuals rating their health as fair or poor. Reference McHorney, Ware and Raczek13,Reference Ware and Sherbourne14 Functional impairment was assessed using a single question to indicate the level of difficulty with everyday tasks arising from reported PTSD symptoms (no difficulty, somewhat, very, extremely difficult or no problems).
For the purpose of analyses, a traumatic incident scale was computed. This was derived by summating any positive responses to the 17 items of the Operational Experiences Scale, which was modified from the Combat Experiences Scale. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman15 Tertiles were generated for this scale and the middle and lower tertiles were combined so that a comparison could be made between the highest levels of combat exposure and all others. The OMHNE survey utilised a number of scales to measure items thought to be associated with mental health, such as morale, leadership, Reference Wright, Cabrera, Bliese, Adler, Hoge and Castro16 cohesion Reference Browne, Iversen, Hull, Workman, Barker and Horn17 and stigmatising beliefs. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman15 Each scale was dealt with in a similar manner where individual scale items were first reduced to binary variables (indicating presence or absence) and then converted to count variables. For the stigma scale, cut-off points of 1 and 3 items were examined and for the cohesion, leadership and morale scales, the cut-off points were 3 out of 4 endorsements to represent high levels of each. Finally, the survey contained several groups of questions regarding predeployment preparation in the form of psychoeducation where personnel were asked ‘Did you receive a stress brief prior to this deployment?’; perceptions of family and welfare support at home, ‘Has the military provided any reassurance or support to your family (parents, siblings, partner or spouse) whilst you have been on this deployment? (e.g. phone calls or visits, arranging ‘’get-togethers” with other service families, newsletters, etc.)’; and questions about the use of deployed medical support such as primary care facilities and the field hospital.
The surveys were powered on the GHQ-12 to detect an 18-22% prevalence of common mental disorder with a confidence level of 95%. The final target sample size was approximately 15% of the deployed force. Categorical analyses were conducted using Pearson’s chi-squared test. Categorical variables were further examined using unadjusted and adjusted univariable and multivariable logistic regression, which was used to generate odds ratios (ORs) with 95% confidence intervals.
In addition to the year of deployment, predictor variables were adjusted for sociodemographic characteristics that have been shown to be important in previous UK armed forces studies including age, service background, engagement type and gender; Reference Fear, Jones, Murphy, Hull, Iversen and Coker7 where the nature of the deployment might theoretically be linked to mental health such as combat exposure, deploying without other unit members and being in a relationship (reflecting available social support); home-front concerns, Reference Mulligan, Jones, Davies, McAllister, Fear and Wessely8 such as having dependant children; time spent away from home and time spent on previous tours; Reference Rona, Fear, Hull, Greenberg, Earnshaw and Hotopf1 deployment location and shorter v. longer period in theatre, reflecting potential exposure to cumulative operational stress. Trends in the data were examined using chi-squared test for trend and significance was defined as P⩽0.05 throughout. Percentages and numbers stated throughout this paper may not add up to sample totals due to missing data.
Results
In total, 2794 personnel took part in the surveys; refusal to participate and returning spoiled or incomplete questionnaires was minimal, resulting in a response rate of 99.6% during OMHNE A1 (n = 1431) and 95.8% during OMHNE A2 (n = 1363). During the A2 survey, 68.7% of the participants were located in forward areas (check points, patrol bases and forward operating bases rather than main operating bases) contrasting with 35.7% in forward areas during A1 (χ2 = 350.54, d.f. = 1, P⩽0.001) (online Table DS1).
The sociodemographic characteristics of the two samples differed significantly in a number of ways. The A1 sample contained greater numbers of army and Royal Marines personnel, marginally fewer Royal Air Force and fewer Royal Navy personnel. Significantly greater numbers of reserve forces took part in A1 (A1: 6.9% (n = 98) v. A2: 4.6% (n = 60), P⩽0.01). Although the age categories differed significantly, the difference in the proportions of personnel under 24 years of age, a group known to be at greater risk of mental health disorder, was not significant (A1: 42.3% v. A2 40.2%, P = 0.26). The A2 sample contained a significantly greater number of personnel with dependent children (A1: 64.2% v. A2: 69.0%, P⩽0.01), significantly fewer personnel with shorter lengths of service (A1: 42.0% v. A2: 37.1%, P = 0.01), significantly fewer individual augmentees (A1: 8.7% v. A2: 6.7%, P⩽0.05) and significantly greater numbers of operationally experienced personnel (A1: 40.0% v. A2: 50.5%, P⩽0.001). Although the proportions of the three combat role categories were significantly different in the two samples, the proportions of combat personnel (those undertaking direct combat missions and most at risk of poorer mental health) were similar (A1: 53.7% (n = 769), A2: 51.8% (n = 706), χ2 = 1.05, d.f. = 1, P = 0.30). When compared with whole service data (where it was available) 18 in both OMHNE samples, Royal Air Force and Royal Navy personnel were underrepresented as were officers, senior non-commissioned officers and reserve forces, and both samples were younger than expected. The levels of general combat exposure differed significantly between the two samples. During A1, 46.5% (n = 661) of personnel reported exposures falling within the upper tertile of combat exposure compared with 36.8% (n = 501) of A2 personnel (P⩽0.001).
Mental health outcomes between the two surveys were not significantly different; the prevalence of probable PTSD was 2.8% during A1 and 1.8% during A2 (P = 0.08). For common mental health disorders the rate was 17.0% during A1 and 16.0% during A2 (P = 0.49). A total of 94.1% of A1 personnel rated their global health as good, very good or excellent compared with 93.3% of A2 personnel (P = 0.39). The rate of reporting a PCL-C score ⩾30 was 16.5% during A1 and 14.4% during A2 (P = 0.13) and functional impairment related to PTSD symptoms was not significantly different between the two surveys (22.2% during A1 v. 20.2% during A2 (P = 0.18)). During both deployments, PCL-C ⩾30 scores were more prevalent in more austere, exposed and dangerous locations. Of the combined subthreshold and probable PTSD ‘cases’ in both samples (n = 415), 67.2% (n = 279) reported being somewhat, very much or extremely functionally impaired compared with 11.9% (n = 246) of non-cases (n = 2063) (χ2 = 632.86, d.f. = 1, P=0.001).
Around half of personnel reported three or more stigmatising beliefs about having a mental health problem (stigma) and/or barriers to care (A1: 49.4% v. A2: 47.1%, P = 0.24). Any mental health disorder caseness was significantly associated with reporting ⩾3 stigma/barriers to care at both assessment points (A1 ‘cases’: 69.5% (n = 169) v. 45.0% non-cases (n = 495), χ2 = 47.8, d.f. = 1, P⩽0.001, A2: 65.9% (n = 139) v. 43.4% (n = 460), χ2 = 35.8, d.f.= 1, P⩽0.001). The mental health outcomes are shown in Table 1.
Table 1 Mental health outcomes

| n (%) | ||||
|---|---|---|---|---|
| Mental health outcome | OMHNE A1 and A2, n | A1 | A2 | Adjusted ORFootnote a |
| Global health | 1.11 (0.72-1.70) | |||
| Excellent, very good or good | 2610 | 1341 (94.1) | 1269 (93.3) | |
| Poor/fair | 175 | 84 (5.9) | 91 (6.7) | |
| Common mental disorder | 0.90 (0.68-1.19) | |||
| Not a case, ⩽3 symptoms | 2320 | 1179 (83.0) | 1141 (84.0) | |
| Case, ⩾4 symptoms | 460 | 242 (17.0) | 218 (16.0) | |
| Post-traumatic stress disorder | 2.12 (0.99-4.53) | |||
| Not a case | 2713 | 1378 (97.2) | 1335 (98.2) | |
| Case | 63 | 39 (2.8) | 24 (1.8) | |
| Subthreshold post-traumatic stress disorder | 1.27 (0.94-1.70) | |||
| PCL-C cut-off ⩽30 | 2346 | 1183 (83.5) | 1163 (85.6) | |
| PCL-C cut-off ⩾31 | 430 | 234 (16.5) | 196 (14.4) | |
| Functional impairment | 1.03 (0.79-1.35) | |||
| None | 1955 | 957 (77.8) | 998 (79.8) | |
| Somewhat, very or extremely functionally impaired | 525 | 273 (22.2) | 252 (20.2) | |
| Stigmatising beliefs and barriers to care | 2620 | 1.09 (0.88-1.34) | ||
| ⩽2 item | 1354 | 681 (50.6) | 673 (52.9) | |
| ⩾3 items | 1266 | 666 (49.4) | 600 (47.1) | |
OMHNE, Operational Mental Health Needs Evaluation; A1, Afghanistan, winter 2010; A2, Afghanistan, summer 2011; OR, odds ratio; PCL-C, Post Traumatic Stress Disorder Checklist Civilian version.
a. Adjusted for 2010 v. 2011, rank, service background, engagement type, individual augmentee v. formed unit, gender, relationship status, dependent children, check point and patrol base v. forward operating base and main operating base, combat exposure, previous tours, shorter v. longer period in theatre, family support, good v. poorer leadership.
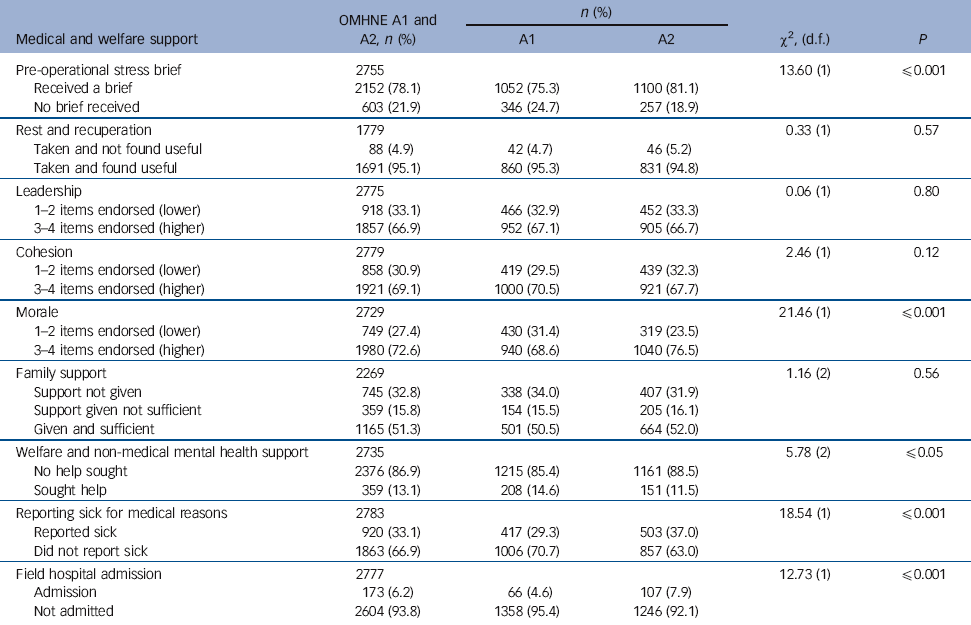
When the components of operational support were examined, the proportion of personnel who remembered receiving predeployment stress briefings rose significantly from 75.3% during A1 to 81.1% during A2 (P=0.001), although the rate of taking rest and recuperation and finding it helpful remained constant at around 95% (P = 0.57). Subjective impressions of leadership were generally high and remained fairly constant across the two surveys. A total of 67.1% of personnel endorsed ⩾3 out of 4 positive leadership statements during A1 and 66.7% during A2 (P = 0.80). For perceptions of unit cohesion, 70.5% endorsed ⩾3 out of 4 positive cohesion statements during A1 and 67.7% during A2 (P = 0.12). However, levels of morale had increased significantly from 68.6% endorsing ⩾3 out of 4 positive morale statements during A1 to 76.5% during A2 (P⩽0.001).
Subjective impressions of family support remained stable with two-thirds of personnel reporting that families at home had received some level of family support at both time points (P = 0.56) and over half of all personnel felt that this support was sufficient at both survey points. Significantly more personnel (37.0%) had reported sick on at least one occasion during A2 than during A1 (29.3%) (P⩽0.001). The proportion of personnel admitted to the field hospital had also risen significantly from 4.6% during A1 to 7.9% during A2 (P⩽0.001). Among help-seekers, 85 of 3405 (2.5%) accessed medical sources (paramedical, doctor or mental health practitioner) and 625 of 3405 (18.4%) sought help from non-medical sources (friend, commander, chaplain or peer support). The support elements are detailed in Table 2.
After adjusting for year of deployment and a range of additional observed confounding variables, we found that those who did not recall receiving a predeployment stress brief (21.9%, n = 603), and those who took rest and recuperation but did not find it helpful (4.9%, n = 88 of those who took rest and recuperation) reported poorer mental health; however, the latter became borderline non-significant when adjusted for all confounding variables. Better mental health was associated with reporting the highest levels of perceived leadership. Perceived adequate support to families at home was associated with better mental health, however those who sought out support for a stressful, family or emotional problem from non-medical sources during deployment were more likely to report mental health problems as were personnel who reported sick for medical reasons and also those admitted to the field hospital. Despite the substantial differences in the levels of combat exposure and the variations in deployment location between OMHNE A1 and A2, the year of deployment had no modifying effect on any of the support variables examined. The adjusted logistic regression analyses are shown in online Table DS2.
Table 2 Operational and family welfare and medical support
| OMHNE A1
and A2, n (%) |
n (%) | ||||
|---|---|---|---|---|---|
| Medical and welfare support | A1 | A2 | χ2, (d.f.) | P | |
| Pre-operational stress brief | 2755 | 13.60 (1) | ⩽0.001 | ||
| Received a brief | 2152 (78.1) | 1052 (75.3) | 1100 (81.1) | ||
| No brief received | 603 (21.9) | 346 (24.7) | 257 (18.9) | ||
| Rest and recuperation | 1779 | 0.33 (1) | 0.57 | ||
| Taken and not found useful | 88 (4.9) | 42 (4.7) | 46 (5.2) | ||
| Taken and found useful | 1691 (95.1) | 860 (95.3) | 831 (94.8) | ||
| Leadership | 2775 | 0.06 (1) | 0.80 | ||
| 1-2 items endorsed (lower) | 918 (33.1) | 466 (32.9) | 452 (33.3) | ||
| 3-4 items endorsed (higher) | 1857 (66.9) | 952 (67.1) | 905 (66.7) | ||
| Cohesion | 2779 | 2.46 (1) | 0.12 | ||
| 1-2 items endorsed (lower) | 858 (30.9) | 419 (29.5) | 439 (32.3) | ||
| 3-4 items endorsed (higher) | 1921 (69.1) | 1000 (70.5) | 921 (67.7) | ||
| Morale | 2729 | 21.46 (1) | ⩽0.001 | ||
| 1-2 items endorsed (lower) | 749 (27.4) | 430 (31.4) | 319 (23.5) | ||
| 3-4 items endorsed (higher) | 1980 (72.6) | 940 (68.6) | 1040 (76.5) | ||
| Family support | 2269 | 1.16 (2) | 0.56 | ||
| Support not given | 745 (32.8) | 338 (34.0) | 407 (31.9) | ||
| Support given not sufficient | 359 (15.8) | 154 (15.5) | 205 (16.1) | ||
| Given and sufficient | 1165 (51.3) | 501 (50.5) | 664 (52.0) | ||
| Welfare and non-medical mental health support | 2735 | 5.78 (2) | ⩽0.05 | ||
| No help sought | 2376 (86.9) | 1215 (85.4) | 1161 (88.5) | ||
| Sought help | 359 (13.1) | 208 (14.6) | 151 (11.5) | ||
| Reporting sick for medical reasons | 2783 | 18.54 (1) | ⩽0.001 | ||
| Reported sick | 920 (33.1) | 417 (29.3) | 503 (37.0) | ||
| Did not report sick | 1863 (66.9) | 1006 (70.7) | 857 (63.0) | ||
| Field hospital admission | 2777 | 12.73 (1) | ⩽0.001 | ||
| Admission | 173 (6.2) | 66 (4.6) | 107 (7.9) | ||
| Not admitted | 2604 (93.8) | 1358 (95.4) | 1246 (92.1) | ||
OMHNE, Operational Mental Health Needs Evaluation; A1, Afghanistan, winter 2010; A2, Afghanistan, summer 2011.
Discussion
Main findings
This study examines data derived from two operational surveys of UK military personnel deployed to Afghanistan some 18 months apart comparing health outcomes as well as the impact of predeployment preparation, leadership, family and welfare and medical support. There were a number of key findings; despite the differences in composition of the two samples, general mental health and stigma/barriers to care were not significantly different at the two survey points, although the rates of reported combat exposure had reduced significantly during A2. In both samples, subthreshold and probable PTSD and associated functional impairment were more prevalent in forward areas. Direct operational mental health support in the form of memorable predeployment stress briefs, perceived good leadership and perceptions of good family support were associated with better mental health at both survey points, however, in both samples, those seeking help from both non-medical and medical sources were more likely to experience poorer mental health.
Our study reveals stable and relatively low levels of mental disorder in comparison with the findings of US deployed mental health surveys 19,Reference Sundin, Fear, Iversen, Rona and Wessely20 and those found in UK military population-based surveys. Reference Hotopf, Hull, Fear, Browne, Horn and Iversen6,Reference Fear, Jones, Murphy, Hull, Iversen and Coker7 Although psychological health was not significantly different between the two Afghanistan surveys, it continues the pattern of reduction from the rate reported in the first Iraq survey. The ‘healthy warrior’ effect Reference Wilson, Jones, Fear, Hull, Hotopf and Wessely21 may explain why this pattern of reducing disorder has emerged, where those who are medically unfit and those lost from service through natural attrition do not deploy. Additionally, direct operational support such as the significant increase in the numbers recalling predeployment stress briefing and continuing high levels of perceived good leadership appear to be associated with better mental health, and we note that morale had risen significantly at the second survey point.
Mental health stigmatisation
The rate of mental health stigmatisation and perceived barriers to care remained high between the two survey points despite considerable effort being made by UK armed forces to promote a positive view of mental health through a number of active strategies such as education, poster and media campaigns. This is of particular concern as the rate of mental disorder in those reporting stigmatisation is higher than in the non-stigmatised. Reference Iversen, van, Hacker, Greenberg, Hotopf and Rona22 Despite the persistence of stigma, our data reveal a mixed picture where help-seeking from welfare sources had fallen significantly but medical help-seeking had risen significantly. We have previously observed that stigmatisation is substantially higher during deployment than when it is measured immediately postdeployment Reference Osório, Jones, Fertout and Greenberg23 and have argued that, although it may influence the decision to seek help, deployment stigma may help to reinforce hardiness. Given that functional impairment arising from subthreshold and probable PTSD symptoms may act to reduce operational effectiveness, attempts to reduce stigma should continue so that those with mental health symptoms feel more able to step forward and receive help.
Operational support
Our data appear to support the previous finding that recalling receiving a pre-operational stress brief is associated with better mental health. Reference Mulligan, Jones, Woodhead, Davies, Wessely and Greenberg5 The rise in the proportion of personnel remembering predeployment stress briefings may reflect the general effort that has been invested in supporting deployment mental health. The data also reveal continued high levels of perceived good leadership and it is likely that good leaders will ensure that reasonable quality predeployment stress briefs are delivered to their personnel.
Although rest and recuperation was deemed useful by the majority of personnel at both survey points and had some influence on mental health, it became borderline non-significant when all observable confounders were accounted for. It remains, however, an important component of deployment mental health support when it has perceived utility.
Perceived support for the family
We have previously reported that stress in the service person’s family is an important target for deployment mental health support and the perception that such support is in place was important at both survey points. However, given that this finding is about perceived support, we highlight the notion that family support efforts must be made visible to deployed personnel to be meaningful. When we combined the surveys, around a third of personnel reported that family support was inadequate and this rate remained constant between the two surveys; we therefore suggest that there is scope to further improve this form of support for those deployed on operations.
Help-seeking
Help-seeking on operations is associated with poorer mental health, whether it be from non-medical sources such as friends, commanders or other welfare sources, or from medical sources, including primary care facilities and the field hospital. The rates of reporting sick for medical reasons and admission to hospital both increased significantly over time, however it is notable that medical assets were the least popular sources of help for mental health support in our surveys (data available from the authors on request). Given that mental health symptoms are more prevalent among those reporting sick and our stigma findings suggest that a significant proportion of deployed personnel may be disinclined to seek help because of perceived psychological and physical barriers, we suggest that medical consultations are an important opportunity for mental ill health prevention or the detection of early symptoms. This could be achieved by asking a simple question about the person’s current mental well-being irrespective of the reason for consultation. The same could be said for those seeking help from non-medical sources for what might appear to be general personnel issues.
Combat exposure
The first survey, OMHNE A1, was conducted during intense offensive combat operations, whereas the A2 survey took place in a marginally more benign and static operational area as evidenced by the significant reduction in reported combat exposure, although this remained substantial. However, the current survey sampled a greater number of austere forward locations and we expected this to have had a substantial influence on mental health, Reference Shigemura and Nomura24 which it did not.
Strengths and weaknesses
The major strength of this study was that it sampled deployed personnel in their place of duty, and not just in the relatively safe large centres such as main bases. We are therefore confident that this study reflects a robust view of deployment mental health. Most studies that purport to examine deployment mental health do so by asking for retrospective accounts, which introduces the possibility of memory distortion. Furthermore, the surveys that have been undertaken have rarely discriminated between personnel deployed in extreme or remote locations and those in safer areas. Overall, the demographic profile of the two samples differed significantly on a number of key factors and, although we attempted to control for confounders in the multivariable analyses, it is possible that unobserved confounders or those not selected for inclusion a priori may have influenced the results. As with any cross-sectional data, it is not possible to establish the direction of cause and we acknowledge that the outcomes are associative rather than directional. Finally, the sampling strategy used in this study was not random, however we preselected visit locations based on the requirement to include sufficient numbers of forward locations and representative personnel. Although we oversampled potentially at-risk groups, there were sufficient numbers of personnel in the general survey to satisfy correct subgroup proportionality and the power requirements of the study.
Implications
We conclude that at both survey points there were relatively low levels of mental health disorders among UK armed forces personnel deployed in arduous conditions in Afghanistan and that the rates remained stable over time. In both samples, forward deployment was associated with subthreshold and probable PTSD symptoms that were linked to functional impairment. Mental health stigmatisation and barriers to care remained high in both surveys and appear to require further efforts to reduce them as they were associated with symptoms of mental disorder. Irrespective of the year of deployment, direct operational support, including perceived good leadership and satisfactory family support to those at home, appeared to be important associates of good mental health. Finally, the proportion of personnel seeking medical consultations and general welfare support interventions rose between the two surveys and they may be important occasions for detecting mental ill health in deployed personnel.







eLetters
No eLetters have been published for this article.