In 1939 Penrose examined European statistics on prison and psychiatric hospital populations and introduced what is now known as the ‘hydraulic hypothesis’. This hypothesis presents the idea that the number of prisons increases as the number of psychiatric beds decreases. Reference Lamb and Weinberger1–Reference Swartz4 The idea gained prominence in the era of deinstitutionalisation, Reference Banks, Stone, Pandiani, Cox and Morschauser3,Reference Conacher5,Reference Susnick and Belcher6 and has been revisited following deinstitutionalisation in South America. Reference Lamb7,Reference Mundt, Chow, Arduino, Barrionuevo, Fritsch and Girala8 Deinstitutionalisation emerged in the 1950s and 1960s in the USA and UK and was triggered by humanitarian, economical and societal factors. Reference Lesage, Morissette, Fortier, Reinharz and Contandriopoulos9–Reference Leff, Dayson, Gooch, Thornicroft and Wills12 Subsequently this policy was pursued in Canada, Reference Sealy and Whitehead13,Reference Herman and Smith14 western Europe, Reference Novella15,Reference Pijl, Kluiter and Wiersma16 northern Europe, Reference Munk-Jorgensen17–Reference Vazquez-Barquero, Garcia and Torres-Gonzalez19 southern Europe, Reference Priebe, Badesconyi, Fioritti, Hansson, Kilian and Torres-Gonzales20,Reference Saraceno21 non-communist central European countries, Reference Haug and Rossler22 Australia, Reference Rosen23,Reference Young and Ashman24 New Zealand, Reference Joseph, Kearns and Moon25 Jamaica, Reference Whitley and Hickling26,Reference Hickling27 and in other parts of the world. In many countries it is still an ongoing process. Reference Haug and Rossler22 However, in central and eastern Europe and in east and southeast Asia, mental healthcare still relies heavily on large psychiatric hospitals and therefore deinstitutionalisation is central to mental health reforms in these areas. Reference Semrau, Barley, Law and Thornicroft28,Reference Ito, Setoya and Suzuki29
Since deinstitutionalisation began, arguments that psychiatric reforms have led to former patients entering prisons and becoming homeless have been prolifically published in the professional literature, Reference Conacher5,Reference Appleby and Desai30–Reference Wallace, Mullen and Burgess33 as well as in newspapers. Reference Winerip34 As a rule, these arguments have been based on either ecological studies or – more often – personal observations or judgements. Ecological studies are observational studies that work with aggregated rather than individual data. Such studies resulted in contradictory findings. Priebe et al, Hodgins et al, Raphael & Stoll and Kramp & Gabrielsen, for example, came to the conclusion that where there were fewer psychiatric beds there were more criminal convictions of those with mental disorders. Reference Priebe, Badesconyi, Fioritti, Hansson, Kilian and Torres-Gonzales20,Reference Hodgins, Muller-Isberner and Allaire35–Reference Kramp and Gabrielsen37 On the other hand, Wallace et al and Hartvig & Kjelsberg, for instance, came to the opposite conclusion and did not attribute increased criminal convictions to deinstitutionalisation. Reference Wallace, Mullen and Burgess33,Reference Hartvig and Kjelsberg38 No matter what the findings, ecological studies face the risk of ecological fallacy, i.e. invalid inference on causal relationship from group data to individual level.
The limitations of ecological studies might be overcome by cohort studies. Some studies approached people who were homeless or in prison and then detected a history of psychiatric treatment at the individual level: see, for instance, Bassuk & Lamb and Whitmer. Reference Bassuk and Lamb39,Reference Whitmer40 The problem with such studies is an implicit assumption that these people, usually with new and acute disorders, would not end up homeless or in prison under the old system dominated by psychiatric hospitals. It is an assumption that the old system would somehow deal better with the new societal situation.
Maj, on behalf of the World Psychiatric Association and in concordance with the World Health Organization (WHO) and the European Commission, stated that deinstitutionalisation should be regarded as a priority worldwide. Reference Maj41–43 However, the question of homelessness and criminality among patients discharged from the institutions has not been resolved, Reference Prins44 and may become an obstacle to reform efforts. For instance, in the Czech Republic some psychiatrists and media outlets published messages predicting that mental health reform would drive people with psychosis into homelessness and imprisonment. Reference David45–49 This backlash phenomenon has been described during the early years of deinstitutionalisation in the USA and is referred to as anti-deinstitutionalisationism. Reference Christenfeld10 Cohort studies of discharged patients might help to shed light on whether or not deinstitutionalisation has led to homelessness and criminality. These studies could either use a follow-up design, assessing participants at baseline and then repeatedly for a long period, or they could follow a trace-back design in which cases of patients discharged some time ago are re-examined. We aimed to identify such cohort studies and assess homelessness and imprisonment among those with severe mental disorders who were discharged from psychiatric hospitals as a consequence of deinstitutionalisation. A further aim was to assess suicidality among these former patients as it was suggested that a reduction in psychiatric beds might increase suicide rates. 48,49 This review was conducted to bring new insights into the controversy; in other words, we hoped to replace rhetoric with evidence. This should inform decision makers, especially in countries where institutional mental healthcare predominates, and help them to pursue a good strategy for mental healthcare development. Deinstitutionalisation is the official WHO policy for Europe; however, if it leads to homelessness and criminality, the price to be paid may be perceived as too high by both policy makers and the public.
Method
A systematic literature review in compliance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines was conducted between July 2013 and February 2014. The study population was defined as people with severe mental disorders who had been resident in a psychiatric hospital for more than 1 year, whose main disability was not related to old age (dementia) or intellectual disabilities, and were 18–65 years old. If patients were older, the study could still be included if it was made clear that those with dementia were not eligible. People with dementia and those with intellectual disabilities were excluded because they do not represent typical populations of mental hospitals; rather, there are specialist institutions for both of these groups. The definition of length of stay was chosen in line with other studies that defined a long-term patient as someone treated in hospital for more than a year. Reference Leff50–Reference Jones, Robinson and Golightley53 However, some studies defined long-term patients as those with a duration of stay longer than 6 months, Reference Kunitoh54,Reference Livingston and Bryson55 and yet other studies used minimum periods of up to 2 years. Reference Gottheil, Winkelmayer, Smoyer and Exline56
Intervention was defined as a discharge of patients from psychiatric hospitals that was driven by deinstitutionalisation, defined broadly as a policy of significant reduction in the number of psychiatric beds or total closure of hospitals. The simultaneous development and functioning of community care was not necessary for a study to be included in the final analysis, although this would have had probably influenced the outcomes of interest. Only patients discharged from general as opposed to secure psychiatric hospitals were included in our review. Comparison of different groups of patients was not considered to be relevant.
Outcomes were primarily defined as criminality and homelessness among discharged patients. Criminality was expressed as the number of people who ended up in prison at some point during the follow-up period and thus was concerned mainly with serious offences. Homelessness was identified through the number of people who were known to have become homeless or had used services for homelessness at some point during the follow-up period. The rate or number of suicides was also examined.
To meet inclusion criteria studies had to have a cohort design and either follow up or trace back the discharged patients. Studies based on data gathered from registers (unless they contained individual patients' data) were excluded. Individual case reports were excluded from the final analysis, as they would introduce systematic bias. Best efforts were made to obtain grey literature with possibly relevant data; no time restraints were applied, and studies published in English, German, French or Dutch were included in the analysis.
Search strategy
Scientific databases were searched in two phases. The pilot phase took place in July 2013, and PubMed/Medline was chosen for the initial search. Nineteen potentially eligible articles were identified: eight examined homelessness and criminality among deinstitutionalised patients, two of which were concerned with the TAPS study population. These 19 articles were analysed and relevant information extracted. Reference lists were searched for additional articles, as was the review published later that year by Kunitoh. Reference Kunitoh54 The pilot demonstrated that a broad search strategy was necessary to identify all potentially eligible studies. For example, some studies did not refer to ‘deinstitutionalisation’ but rather to psychiatric or mental hospital closure, others used the term ‘transinstitutionalisation’ or ‘reinstitutionalisation’ in order to describe the process of how people ended up in other institutions, including prisons and institutions for homeless people. Some studies did not use any of these terms and spoke simply about patients discharged from psychiatric hospitals.
The second search phase took place in October, November and December 2013. The search strategy was developed, tested, adjusted and finally applied at PubMed/Medline (up to November 2013 week 2) and Web of Knowledge (including Web of Science from 1900 and Medline from 1950, both up to November 2013 week 2), and subsequently also adjusted for databases working on Ovid platform including PsycINFO, Health Management Information Consortium and Social Policy and Practice (all searched up to December 2013 week 2). A combination of truncated and asterisked words deinstitutionalisation, crime, homelessness, psychiatry, reinstitutionalisation, transinstitutionalisation, psychiatric hospital, mental hospital, discharge and closing was used to identify possibly relevant studies in peer-reviewed journals as well as grey literature (see online supplement DS1 for more details). The Cochrane Library was searched simply using ‘deinstitutionali?ation’ for title, abstracts and keywords; the last search was conducted in January 2014 week 5.
Results
The search strategy resulted in over 9416 unique and possibly relevant pieces of literature. Most relevant articles were identified by this strategy, although a few (n = 19) other potentially eligible articles were identified through references, authors and experts (Fig. 1).

Fig. 1 PRISMA flowchart.
Included studies
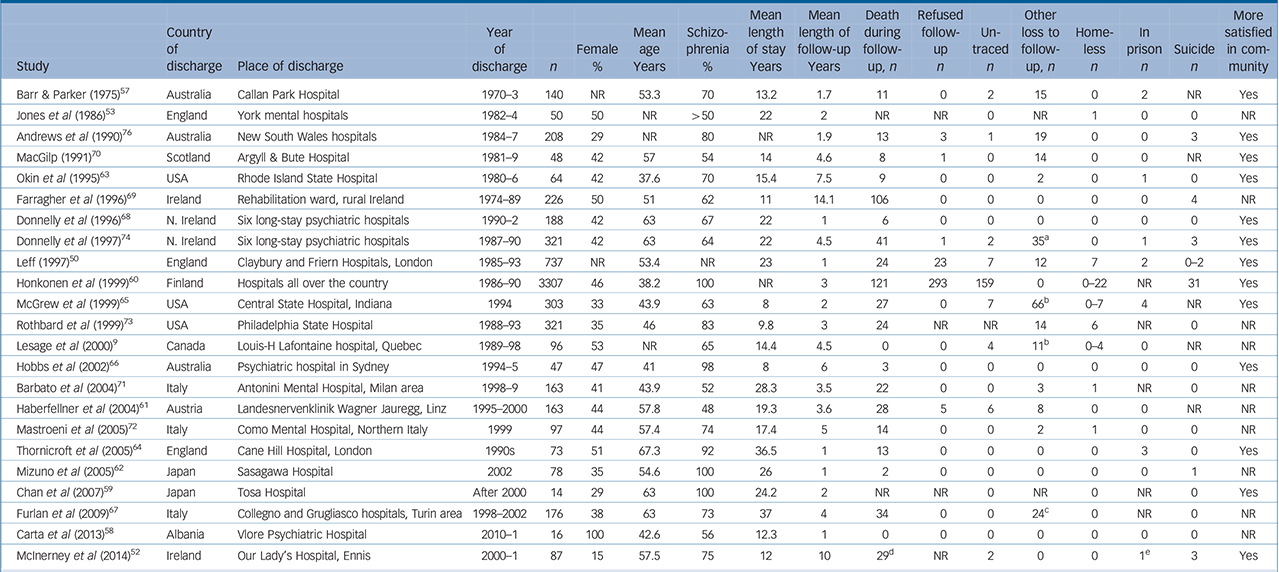
Twenty-three studies representing unique populations of deinstitutionalised patients from Albania, Australia, Austria, Canada, England, Wales, Finland, Ireland, Italy, Japan, Northern Ireland, Scotland and USA were identified and analysed (Table 1). The years of patient discharge ranged from 1970 (Australia) up to 2011 (Albania), Reference Barr and Parker57,Reference Carta, Agaj, Harapej, Lecca, Xhelili and Altoe58 which effectively means that the earliest period of deinstitutionalisation was not covered. The first studies conducted in the USA and the UK were of patients discharged between 1980 and 1986 (USA) and between 1982 and 1984 (UK). No eligible study from Latin America was found. The included studies are described in detail in online supplement DS2, and excluded studies in supplement DS3. The included studies differed in quality and ranged from local cohort studies with as few as 14 respondents, Reference Chan, Inoue, Shimodera, Fujita, Fukuzawa and Kii59 to studies conducted on a national scale with as many as 3307 respondents. Reference Honkonen, Saarinen and Salokangas60 The studies of highest quality were conducted by the TAPS team in England and by Honkonen et al in Finland. Reference Leff50,Reference Honkonen, Saarinen and Salokangas60 These were methodologically rigorous and included large cohorts of patients. However, there was a considerable loss to follow-up in the Finnish study. Reference Honkonen, Saarinen and Salokangas60 Both studies reported few adverse consequences and that patients were more satisfied in the community than in the hospital.
Table 1 Summary of included studies
| Study | Country
of discharge |
Place of discharge | Year of discharge |
n | Female % |
Mean age Years |
Schizophrenia % |
Mean length of stay Years |
Mean length of follow-up Years |
Death during follow-up, n |
Refused follow-up n |
untraced n |
Other loss to follow-up, n |
Homeless n |
In prison n |
Suicide n |
More satisfied in community |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Barr & Parker (1975) Reference Barr and Parker57 | Australia | Callan Park Hospital | 1970–3 | 140 | NR | 53.3 | 70 | 13.2 | 1.7 | 11 | 0 | 2 | 15 | 0 | 2 | NR | Yes |
| Jones et al (1986) Reference Jones, Robinson and Golightley53 | England | York mental hospitals | 1982–4 | 50 | 50 | NR | >50 | 22 | 2 | NR | NR | 0 | NR | 1 | 0 | 0 | NR |
| Andrews et al (1990) Reference Andrews, Teesson, Stewart and Hoult76 | Australia | New South Wales hospitals | 1984–7 | 208 | 29 | NR | 80 | NR | 1.9 | 13 | 3 | 1 | 19 | 0 | 0 | 3 | Yes |
| MacGilp (1991) Reference MacGilp70 | Scotland | Argyll & Bute Hospital | 1981–9 | 48 | 42 | 57 | 54 | 14 | 4.6 | 8 | 1 | 0 | 14 | 0 | 0 | NR | Yes |
| Okin et al (1995) Reference Okin, Borus, Baer and Jones63 | USA | Rhode Island State Hospital | 1980–6 | 64 | 42 | 37.6 | 70 | 15.4 | 7.5 | 9 | 0 | 0 | 2 | 0 | 1 | 0 | Yes |
| Farragher et al (1996) Reference Farragher, Carey and Owens69 | Ireland | Rehabilitation ward, rural Ireland | 1974–89 | 226 | 50 | 51 | 62 | 11 | 14.1 | 106 | 0 | 0 | 0 | 0 | 0 | 4 | NR |
| Donnelly et al (1996) Reference Donnelly, McGilloway, Mays, Knapp, Kavanagh and Beecham68 | N. Ireland | Six long-stay psychiatric hospitals | 1990–2 | 188 | 42 | 63 | 67 | 22 | 1 | 6 | 0 | 0 | 0 | 0 | 0 | 0 | Yes |
| Donnelly et al (1997) Reference Donnelly, McGilloway, Mays, Perry and Lavery74 | N. Ireland | Six long-stay psychiatric hospitals | 1987–90 | 321 | 42 | 63 | 64 | 22 | 4.5 | 41 | 1 | 2 | 35 a | 0 | 1 | 3 | Yes |
| Leff (1997) Reference Leff50 | England | Claybury and Friern Hospitals, London | 1985–93 | 737 | NR | 53.4 | NR | 23 | 1 | 24 | 23 | 7 | 12 | 7 | 2 | 0–2 | Yes |
| Honkonen et al (1999) Reference Honkonen, Saarinen and Salokangas60 | Finland | Hospitals all over the country | 1986–90 | 3307 | 46 | 38.2 | 100 | NR | 3 | 121 | 293 | 159 | 0 | 0–22 | NR | 31 | Yes |
| McGrew et al (1999) Reference McGrew, Wright, Pescosolido and McDonel65 | USA | Central State Hospital, Indiana | 1994 | 303 | 33 | 43.9 | 63 | 8 | 2 | 27 | 0 | 7 | 66 b | 0–7 | 4 | NR | Yes |
| Rothbard et al (1999) Reference Rothbard, Kuno, Schinnar, Hadley and Turk73 | USA | Philadelphia State Hospital | 1988–93 | 321 | 35 | 46 | 83 | 9.8 | 3 | 24 | NR | NR | 14 | 6 | NR | 0 | NR |
| Lesage et al (2000) Reference Lesage, Morissette, Fortier, Reinharz and Contandriopoulos9 | Canada | Louis-H Lafontaine hospital, Quebec | 1989–98 | 96 | 53 | NR | 65 | 14.4 | 4.5 | 0 | 0 | 4 | 11 b | 0–4 | 0 | NR | NR |
| Hobbs et al (2002) Reference Hobbs, Newton, Tennant, Rosen and Tribe66 | Australia | Psychiatric hospital in Sydney | 1994–5 | 47 | 47 | 41 | 98 | 8 | 6 | 3 | 0 | 0 | 0 | 0 | 0 | 0 | Yes |
| Barbato et al (2004) Reference Barbato, D'Avanzo, Rocca, Amatulli and Lampugnani71 | Italy | Antonini Mental Hospital, Milan area | 1998–9 | 163 | 41 | 43.9 | 52 | 28.3 | 3.5 | 22 | 0 | 0 | 3 | 1 | NR | 0 | NR |
| Haberfellner et al (2004) Reference Haberfellner, Grausgruber, Grausgruber-Berner, Ortmair and Schony61 | Austria | Landesnervenklinik Wagner Jauregg, Linz | 1995–2000 | 163 | 44 | 57.8 | 48 | 19.3 | 3.6 | 28 | 5 | 6 | 8 | 0 | 0 | NR | NR |
| Mastroeni et al (2005) Reference Mastroeni, Bellotti, Pellegrini, Galletti, Lai and Falloon72 | Italy | Como Mental Hospital, Northern Italy | 1999 | 97 | 44 | 57.4 | 74 | 17.4 | 5 | 14 | 0 | 0 | 2 | 1 | 0 | 0 | NR |
| Thornicroft et al (2005) Reference Thornicroft, Bebbington and Leff64 | England | Cane Hill Hospital, London | 1990s | 73 | 51 | 67.3 | 92 | 36.5 | 1 | 13 | 0 | 0 | 0 | 0 | 3 | 0 | Yes |
| Mizuno et al (2005) Reference Mizuno, Sakuma, Ryu, Munakata, Takebayashi and Murakami62 | Japan | Sasagawa Hospital | 2002 | 78 | 35 | 54.6 | 100 | 26 | 1 | 2 | 0 | 0 | 0 | 0 | 0 | 1 | NR |
| Chan et al (2007) Reference Chan, Inoue, Shimodera, Fujita, Fukuzawa and Kii59 | Japan | Tosa Hospital | After 2000 | 14 | 29 | 63 | 100 | 24.2 | 2 | NR | NR | 0 | NR | 0 | NR | 0 | Yes |
| Furlan et al (2009) Reference Furlan, Zuffranieri, Stanga, Ostacoli, Patta and Picci67 | Italy | Collegno and Grugliasco hospitals, Turin area | 1998–2002 | 176 | 38 | 63 | 73 | 37 | 4 | 34 | 0 | 0 | 24 c | 0 | NR | 0 | NR |
| Carta et al (2013) Reference Carta, Agaj, Harapej, Lecca, Xhelili and Altoe58 | Albania | Vlore Psychiatric Hospital | 2010–1 | 16 | 100 | 42.6 | 56 | 12.3 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | NR |
| McInerney et al (2014) Reference McInerney, Finnerty, Avalos and Walsh52 | Ireland | Our Lady's Hospital, Ennis | 2000–1 | 87 | 15 | 57.5 | 75 | 12 | 10 | 29 d | NR | 2 | 0 | 0 | 1 e | 3 | Yes |
NR, not repotted.
a. Of these, 33 were in hospital and thus ineligible for follow-up.
b. In hospital at the time of follow-up.
c. Patients were transferred to facilities for the elderly.
d. At the 5-year follow-up.
e. At the 5-year follow-up; this man died by suicide later on.
The percentage of women respondents ranged from 15% to 100%, Reference McInerney, Finnerty, Avalos and Walsh52,Reference Carta, Agaj, Harapej, Lecca, Xhelili and Altoe58 and the proportion of those with schizophrenia ranged from 48% to 100%. Reference Chan, Inoue, Shimodera, Fujita, Fukuzawa and Kii59–Reference Mizuno, Sakuma, Ryu, Munakata, Takebayashi and Murakami62 The mean age of discharged patients varied between 37.6 years and 67.3 years. Reference Okin, Borus, Baer and Jones63,Reference Thornicroft, Bebbington and Leff64 All discharged patients had a lengthy stay in psychiatric hospital, ranging from 8 years to 37 years, Reference McGrew, Wright, Pescosolido and McDonel65–Reference Furlan, Zuffranieri, Stanga, Ostacoli, Patta and Picci67 and were followed up from 1 year to 14.1 years after discharge. Reference Donnelly, McGilloway, Mays, Knapp, Kavanagh and Beecham68,Reference Farragher, Carey and Owens69 The studies by Farragher et al, McInerney et al and Furlan et al had high rates of loss to follow-up (47%, 33% and 19% respectively) due to high death rates. Reference McInerney, Finnerty, Avalos and Walsh52,Reference Furlan, Zuffranieri, Stanga, Ostacoli, Patta and Picci67,Reference Farragher, Carey and Owens69 One study had a 22% loss to follow-up due to readmission of previously discharged patients. Reference McGrew, Wright, Pescosolido and McDonel65 Rates of refusal to participate in the follow-up were highest in the studies by Honkonen et al and Leff (9% and 3% respectively). Reference Leff50,Reference Honkonen, Saarinen and Salokangas60 Otherwise, refusals to follow-up were rare. The rate of untraced patients was under 1% in the majority of studies, but reached 5% in the study by Honkonen et al and 4% in the studies by Lesage et al and Haberfellner et al. Reference Lesage, Morissette, Fortier, Reinharz and Contandriopoulos9,Reference Honkonen, Saarinen and Salokangas60,Reference Haberfellner, Grausgruber, Grausgruber-Berner, Ortmair and Schony61
Out of 23 studies, 15 reported no case of homelessness among discharged patients. Barbato et al reported 1 case out of 163 patients (0.6%), Reference Barbato, D'Avanzo, Rocca, Amatulli and Lampugnani71 Leff reported 7 cases out of 737 patients (0.9%), Reference Leff50 Mastroeni et al reported 1 case out of 97 patients (1%), Reference Mastroeni, Bellotti, Pellegrini, Galletti, Lai and Falloon72 Rothbard et al reported 6 cases out of 321 patients (1.9%), Reference Rothbard, Kuno, Schinnar, Hadley and Turk73 and Jones et al reported 1 case out of 50 patients (2%). Reference Jones, Robinson and Golightley53 Honkonen et al, McGrew et al and Lesage et al reported 0–22 (0–0.7%), 0–4 (0–4.2%) and 0–7 (0–2.3%) possible cases of homelessness out of 3307, 96 and 303 patients respectively. Reference Lesage, Morissette, Fortier, Reinharz and Contandriopoulos9,Reference Honkonen, Saarinen and Salokangas60,Reference McGrew, Wright, Pescosolido and McDonel65 Problems with housing other than homelessness were identified in some studies (online supplement DS2).
The number of discharged patients who ended up in prison was recorded in 18 studies; of these, 11 reported that no patient was imprisoned. Donnelly et al found 1 out of 321 patients in prison (0.3%), Reference Donnelly, McGilloway, Mays, Perry and Lavery74 Leff found 2 out of 737 patients in prison (0.3%), Reference Leff50 McInerney et al found 1 out of 87 patients in prison (1.1%), Reference McInerney, Finnerty, Avalos and Walsh52 McGrew et al found 4 out of 303 patients in prison (1.3%), Reference McGrew, Wright, Pescosolido and McDonel65 Barr & Parker found 2 out of 140 patients in prison (1.4%), Reference Barr and Parker57 Okin et al reported that 1 out of 64 patients was imprisoned (1.6%), Reference Okin, Borus, Baer and Jones63 and Thornicroft et al found 3 out of 73 discharged patients (4.1%). Reference Thornicroft, Bebbington and Leff64 Misdemeanours that had not led to imprisonment occurred occasionally.
Suicide rates were reported in 18 studies, and of these 11 indicated that no suicide occurred. The highest rates of suicide were reported by McInerney et al, who found that 3 out of 87 patients died by suicide (3.4%) (S. J. McInerney, personal communication, 2014), Farragher et al who found that 4 out of 226 patients died by suicide (1.8%) and Andrews et al who found that 3 out of 208 patients died by suicide (1.4%). Reference McInerney, Finnerty, Avalos and Walsh52,Reference Farragher, Carey and Owens75,Reference Andrews, Teesson, Stewart and Hoult76
Discussion
Deinstitutionalisation has been criticised, mainly in the USA, where it was considered to have been poorly organised, resulting in lower levels of funding or budget cuts, and also to have been inconsistent with stated political declarations. Reference Bassuk and Lamb39,Reference Armstrong77–Reference Durham88 This has been concisely described by Dumont & Dumont, who stated that the original US plan, developed under the presidencies of John F. Kennedy and Lyndon Johnson, included an investment of $7 billion and establishment of 2000 community mental health centres across the USA; Reference Dumont and Dumont89 however, this plan was not realised as Johnson's successor, Richard Nixon, substantially restricted its funding. The appropriateness of the delivery of community care has also been criticised elsewhere, for example in Denmark and Canada. Reference Munk-Jorgensen17,Reference Knowles90
Ecological studies have been widely used to research the consequences of deinstitutionalisation, and often conclude that decreasing the number of beds in mental hospitals leads to more people with mental illness in prison or on the streets. Our review does not support this, and we think that these ecological studies might have been confounded. Rather than deinstitutionalisation, other societal factors such as rapid globalisation, increases in migration, growing individualism, less emphasis on traditional families, pressures on housing and the labour market, increased illegal drug use, growing unemployment, legal changes (e.g. those associated with the war on drugs), changes in mental healthcare funding and associated budget cuts could have all contributed to the rising number of people with mental health problems who end up in prison or homeless in the USA and in western Europe. Durham emphasised that the context of deinstitutionalisation in the USA was characterised by restrictive changes in Medicaid, social security and disability payment systems, and by the reduction in low-cost housing and other sociopolitical changes. Reference Durham88
Countries in Latin America have also undergone deep societal changes in the past 30 years. Although the overall burden of psychiatric and neurological disease has grown tremendously, investment in mental healthcare has remained low, and other societal challenges have emerged. Reference Caldas de Almeida and Horvitz-Lennon91 Again, in this context, it might be not surprising that the study by Mundt et al, which analysed data related to deinstitutionalisation in Latin America, found an association between a decreasing number of mental health beds and an increasing number of prison places. Reference Mundt, Chow, Arduino, Barrionuevo, Fritsch and Girala8 The study's authors were, however, aware of its limitations, and indicated that an increase in the number of prison places cannot be solely explained by decreases in the number of hospital beds. They suggest that more evidence is required to determine the pathways leading people with mental health problems into prison. Reference Mundt, Chow, Arduino, Barrionuevo, Fritsch and Girala8
The evidence presented here comes from cohort studies of long-term psychiatric patients discharged into the community. These studies might be more helpful than ecological studies in determining direct causality between deinstitutionalisation and homelessness and criminality. Reference Dickey, Gudeman, Hellman, Donatelle and Grinspoon92 Our review shows that such studies were conducted on different cohorts of patients and in a number of different countries. Analysis of these studies demonstrates that homelessness and criminality among discharged patients occurred sporadically, and suggests that even patients who were discharged after many years in hospital did well in the community. This is in line with the evidence presented by Kunitoh, Reference Kunitoh54 who conducted a systematic review and concluded that deinstitutionalisation was generally beneficial for the majority of discharged patients in terms of both social functioning and quality of life. It also supports findings made by Rothbard & Kuno, who analysed four cases of deinstitutionalisation in Europe and suggested that discharging long-stay patients to the community might be easier than is usually assumed. Reference Rothbard and Kuno93 Our study reveals little evidence of negative consequences of deinstitutionalisation globally.
Limitations
Patients from the studies analysed here are not representative of all deinstitutionalised patients. Untraced and unreported patients could have biased the results, although it would be far from appropriate to conclude that untraced patients were either in prison or homeless. Analyses of withdrawal, which were conducted in some studies (for example those by Honkonen et al and Gardos et al), Reference Honkonen, Saarinen and Salokangas60,Reference Gardos, Cole and LaBrie94 showed that these patients did better at baseline, and therefore might have had improved health during the follow-up and as a consequence deliberately lost contact with mental health services. In addition, there might have been some unreported negative outcomes in primary studies, for instance those that occurred among patients who were already dead by the time of the follow-up. Differences in length of stay, age, gender distribution, place and means of discharge, availability of community services and year of discharge were detected in included studies and make direct comparisons more difficult. Furthermore, mean values might be unrepresentative because outliers could skew the distribution. This was probably the case for many studies analysed here, but this influenced only the sociodemographic profile of patients and not the outcomes of interest – homelessness, imprisonment, suicidality – as these have a binary form (yes or no). There were considerable differences in the follow-up periods, which ranged from 1 year to 25 years. Studies with longer follow-up are expected to have higher drop-out rates and also a greater chance that some of the respondents would become homeless, commit a serious offence or die by suicide. Differences in the health status and history of psychiatric treatment of the population in the studies may be attributed to differences in diagnostic profiles. In some cases, for example in the study by Furlan et al, Reference Furlan, Zuffranieri, Stanga, Ostacoli, Patta and Picci67 the mean age of patients was close to 65 years; thus, some might have had age-related disorders such as dementia, which could slightly bias the results. In many studies there were some patients with personality disorders and drug misuse, and it is not entirely clear whether these were the patients who eventually became homeless or were imprisoned.
A further limitation relates to the place of stay after discharge from hospital. Some of the patients were discharged to nursing homes, and it is questionable whether these can be considered to be proper community facilities. The same applies to the Sasagawa project. Reference Mizuno, Sakuma, Ryu, Munakata, Takebayashi and Murakami62 The Sasagawa hospital was converted into a facility with traditional living accommodation and it is arguable whether this represents ‘regular’ deinstitutionalisation. Additionally, the definition of homelessness was not addressed in the majority of studies. For instance, in the study by Rothbard et al, everyone who had ever been admitted to a homeless shelter was considered to be homeless, no matter how long this period had lasted. Reference Rothbard, Kuno, Schinnar, Hadley and Turk73 On the other hand, Double & Wong found two former patients in a Sheffield hostel for homeless men, but did not record them as homeless. Reference Double and Wong95 The problem of definition also applies to criminality. There are a number of ways to measure criminality, such as self-reports, police reports, number of trials and records from country-specific registers. Our review focused on serious offences only and reported the number of those who ended up in prison after being discharged from psychiatric hospitals. Less serious offences, as well as other relevant details from primary studies, are reported in online supplement DS2.
New cohorts and short-term patients
Despite its limitations, our review suggests that deinstitutionalisation has not resulted in substantial homelessness and imprisonment among discharged long-term patients. It may be, however, postulated that deinstitutionalisation has had a negative effect on new cohorts of patients without access to a psychiatric hospital. This hypothesis is difficult to test. A randomised controlled trial and 5-year follow-up of newly admitted patients with schizophrenia spectrum disorder in Denmark did not find evidence to justify hospital-based treatment, Reference Nordentoft, Ohlenschlaeger, Thorup, Petersen, Jeppesen and Bertelsen96 and a study by Wahlbeck suggested that deinstitutionalisation in Nordic countries, where appropriate community services were available, might have contributed to a reduction in the life expectancy gap between those with mental health problems and general population, Reference Wahlbeck, Westman, Nordentoft, Gissler and Laursen97 but still it is difficult to entirely rule out the aforementioned hypothesis.
It may be also argued that recipients of long-term hospital care have stabilised disorders and are thus at a lower risk of unwanted outcomes than those in their first year of severe mental illness. This argument, however, is not against deinstitutionalisation. It stresses the need for availability of mental health services and mental health beds, but does not imply that these have to be located in large psychiatric institutions. On the contrary, Housing First and assertive community treatment are both community-based services that have been shown to be effective in working with homeless people with mental health problems. Reference Coldwell and Bender98–Reference Somers, Rezansoff, Moniruzzaman, Palepu and Petterson100 Although it might be more expensive to provide such comprehensive care in the community, this does not make it less cost-effective, and it is a human right to live independently and to be included in the community. 101
Implications
The perfect methodological approach that would allow a clear conclusion on the association between deinstitutionalisation, homelessness and imprisonment is unclear. This systematic review, however, demonstrates that the number of former long-stay patients who became homeless or imprisoned after discharge was not excessive, contrary to popular argument. The findings suggest that some of the ecological studies may have been confounded. Cohort studies that followed up or traced back people discharged from long-term psychiatric care show that these patients benefited from the transfer to the community and that serious behavioural problems such as homelessness, imprisonment or suicide did not occur frequently. However, this might have been different with patients with intellectual disabilities or those who were discharged from secure wards. The review has implications for forthcoming psychiatric reforms in eastern Europe and elsewhere. It will help decision makers to tackle the argument that deinstitutionalisation will lead to homelessness and criminality among those with mental health problems, and it will also help stakeholders to justify reforms and advocate increased investment in mental health budgets.
Future research
The findings presented here suggest that Penrose's hydraulic hypothesis might need to be reconsidered. In Penrose's time de facto all public mental healthcare investment went into psychiatric hospitals. Decreasing the number of psychiatric beds signified decreasing investment in mental healthcare. This has, however, changed with the discovery of effective psychopharmaceuticals and with the introduction of new forms of care, both of which emerged roughly in the mid-20th century. Now, a decrease in the number of psychiatric beds no longer necessarily means a decreasing investment in mental healthcare. Instead, as a consequence of the increasing burden of mental disorders and more pressure on the availability of good-quality care in the community, investments into mental health might be rising, whereas the number of beds in mental hospitals might be simultaneously decreasing. Deinstitutionalisation has been criticised and its association with homelessness and criminality among those with mental disorders has been suggested mainly in locations where there have also been deep societal changes, mental health budget cuts and insufficient investment into the development of appropriate multilayered care in the community. Together, these factors suggest that Penrose's hydraulic hypothesis could be stated more precisely as the idea that criminality and homelessness increase as efficacious public investment into mental health decreases. Further research is needed to examine this refined hypothesis.
Funding
This work was supported by the Czech National Institute of Mental Health grant CZ.1.05/2.1.00/03.0078 and by the European Regional Development Fund. The funding source had no role in study design, data collection and analysis, interpretation of the results, writing the report or the decision to submit the paper for publication.
Acknowledgements
We acknowledge the excellent support from the King's College London library team.







eLetters
No eLetters have been published for this article.